Public Meeting of the Board of Directors – Thursday 31 July 2025
Public Meeting of the Board of Directors will be held at 9.30am on Thursday 31 July 2025 in the Inspire@ room at Horizon Leeds, 3rd Floor, 2 Brewery Wharf, Kendall Street, Leeds, LS10 1JR.
Agenda
Opening proceedings
| Item | Item title | Lead | Time |
| 1 | Apologies for absence (verbal) | Merran McRae | 9.30am |
| 2 | Sharing stories (verbal) | Older People’s Service | 9.35am |
| 3 | Declarations of interests and any declarations of conflicts of interest in any agenda item (enclosure) | Merran McRae | No time specified |
| 4 | Minutes of the meeting held on 29 May 2025 (enclosure) | Merran McRae | No time specified |
| 5 | Matters arising (verbal) | Merran McRae | No time specified |
| 6 | Actions outstanding from the public meetings of the Board of Directors (enclosure) | Merran McRae | 10.05am |
| 6.1 | Action 29 supporting information – Musculoskeletal (MSK) Data (enclosure) | Darren Skinner | No time specified |
Use of resources
| Item | Item title | Lead | Time |
| 7 | Annual Responsible Officer and Medical Revalidation Report (enclosure) | Wendy Neil | 10.10am |
| 8 | Chief Executive’s report (enclosure) | Dr Sara Munro | 10.20am |
| 9 | Report from the Chair of the Finance and Performance Committee for the meetings held on 28 July 2025 (to follow) | Cleveland Henry | 10.30am |
| 10 | Report from the Chief Financial Officer (enclosure) | Dawn Hanwell | 10.35am |
| 11 | 2025 – 2026 Organisational Priorities Quarter 1 Progress Report (enclosure) | Dawn Hanwell | 10.45am |
| 12 | Approval of the Data Security and Protection Toolkit (self-certification) (enclosure) | Dawn Hanwell | 10.55am |
| 13 | Health and Safety Annual Report (enclosure) | Dawn Hanwell | 11.00am |
| Not applicable | Break | Not applicable | 11.15am |
| 14 | Report of the Chief Operating Officer (enclosure) | Joanna Forster Adams | 11.25am |
| 15 | EPRR | Joanna Forster Adams | 11.35am |
| 15.1 | EPRR Assurance Standards (enclosure) | Joanna Forster Adams | No time specified |
| 15.2 | EPRR Annual Report (enclosure) | Joanna Forster Adams | No time specified |
Patient centred care
| Item | Item title | Lead | Time |
| 16 | Report from the Chair of the Quality Committee for the meetings held on 12 June and 10 July 2025 (enclosure) | Dr Frances Healey | 11.40am |
| 17 | Safer Staffing Report (enclosure) | Nichola Sanderson | 11.45am |
| 18 | Report from the Medical Director (enclosure) | Dr Chris Hosker | 11.50am |
| 19 | Guardian of Safe-working Hours Q4 and Annual Report (enclosure) | Dr Chris Hosker | 11.55am |
Workforce
| Item | Item title | Lead | Time |
| 20 | Report from the Chair of the Workforce Committee for the meeting held on 5 June 2025 (enclosure) | Zoe Burns-Shore | 12.05pm |
| 21 | Report from the Director of People and Organisational Development (enclosure) | Darren Skinner | 12.10pm |
Governance
| Item | Item title | Lead | Time |
| 22 | Report from the Chair of the Audit Committee for the meetings held on 17 June and 15 July 2025 (enclosure) | Martin Wright | 12.20pm |
| 23 | Board Assurance Framework (enclosure) | Dr Sara Munro | 12.25pm |
| 23.1 | Risk Appetite Statement (enclosure) | Dr Sara Munro | No time specified |
| 24 | Report from the Committees in Common held on 23 July 2025 (enclosure) | Merran McRae | 12.30pm |
| 25 | Use of Trust Seal (verbal) | Merran McRae | No time specified |
| 26 | Any other business | Merran McRae | 12.35pm |
The next meeting of the Board will be held on Thursday 25 September 2025 at 9.30am in the Inspire@2 room at Horizon Leeds, 3rd Floor, 2 Brewery Wharf, Kendall Street, Leeds, LS10 1JR.
Declaration of Interests for members of the Board of Directors
Executive Directors
| Name | Directorships, including Non-executive Directorships, held in private companies or PLCs (with the exception of those of dormant companies). | Ownership, or part-ownership, of private companies, businesses or consultancies likely or possibly seeking to do business with the NHS. | Majority or controlling shareholdings in organisations likely or possibly seeking to do business with the NHS. | A position of authority in a charity or voluntary organisation in the field of health and social care. | Any connection with a voluntary or other organisation contracting for NHS services. | Any substantial or influential connection with an organisation, entity or company considering entering into or having entered into a financial arrangement with the Trust, including but not limited to lenders or banks. | Any other commercial or other interests you wish to declare. This should include political or ministerial appointments (where this is information is already in the public domain – this does not include personal or private information such as membership of political parties or voting preferences) | Declarations made in respect of spouse or co-habiting partner |
| Sara Munro Chief Executive |
None. | None. | None. | Trustee Workforce Development Trust |
None. | None. | None. | None. |
| Dawn Hanwell Chief Financial Officer and Deputy Chief Executive |
None. | None. | None. | None. | None. | None. | None. | None. |
| Chris Hosker Medical Director |
Director Trusted Opinion Ltd. |
None. | Director Lilac Tree Clinic Ltd. |
None. | Director Lilac Tree Clinic Ltd. |
None. | None. | Partner: Director Trusted Opinion Ltd. |
| Joanna Forster Adams Chief Operating Officer |
None. | None. | None. | None. | None. | None. | None. | Partner: Director of Public Health Middlesbrough Council and Redcar and Cleveland Borough CouncilPartner: Chair The Junction Charity |
| Nichola Sanderson Director of Nursing and Professions |
None. | None. | None. | None. | None. | None. | None. | None. |
| Darren Skinner Director of People and Organisational Development |
Director Skinner Consulting Ltd. |
None. | None. | None. | None. | None. | None. | None. |
Non-Executive Directors
| Name | Directorships, including Non-executive Directorships, held in private companies or PLCs (with the exception of those of dormant companies). | Ownership, or part-ownership, of private companies, businesses or consultancies likely or possibly seeking to do business with the NHS. | Majority or controlling shareholdings in organisations likely or possibly seeking to do business with the NHS. | A position of authority in a charity or voluntary organisation in the field of health and social care. | Any connection with a voluntary or other organisation contracting for NHS services. | Any substantial or influential connection with an organisation, entity or company considering entering into or having entered into a financial arrangement with the Trust, including but not limited to lenders or banks. | Any other commercial or other interests you wish to declare. This should include political or ministerial appointments (where this is information is already in the public domain – this does not include personal or private information such as membership of political parties or voting preferences) | Declarations made in respect of spouse or co-habiting partner |
| Merran McRae Chair |
Director Finnbo Ltd |
None. | None. | None. | None. | None. | None. | Partner: Director Finnbo Ltd |
| Zoe Burns-Shore Non-executive Director |
Executive Director for Customer Delivery Money and Pensions Service |
None. | None. | None. | None. | None. | None. | None. |
| Frances Healey Non-executive Director |
None. | None. | None. | Trustee The National Confidential Enquiry into Patient Outcome and Death (NCEPOD) |
None. | None. | Visiting Professor University of LeedsAdvisory Role and Peer Reviewer Research studies and potential research studies related to patient safety |
None. |
| Cleveland Henry Non-executive Director |
Director 63 Argyle Road Ltd. |
None. | None. | Chair of the Board of Trustees Community Foundations for Leeds |
None. | None. | Director of Group Delivery & Deployment Optum (UK) (Digital Health sector) |
Partner: Lead Cancer Nurse Leeds Teaching Hospitals NHS Trust |
| Kaneez Khan Non-executive Director |
Director Primrose Consultancy Yorkshire |
None. | None. | None. | None. | None. | None. | None. |
| Katy Wilburn Non-executive Director |
None. | None. | None. | None. | None. | None. | None. | None. |
| Martin Wright Non-executive Director |
None. | None. | None. | Trustee Roger’s Almshouses (Harrogate) |
None. | None. | None. | Partner: Trustee Roger’s Almshouses (Harrogate) |
Declarations pertaining to directors being a Fit and Proper Person under the CQC Regulation 5 and meeting all the criteria in the Provider Licence and the Trust’s Constitution to be and continue to be a director
Each director has been checked in accordance with the criteria for fit and proper persons and have completed the necessary self-declaration forms to show that they do not fit within any definition of an “unfit person” as set out in the provider licence, the Health and Social Care Act 2008 (Regulated Activities) Regulations 2008 or the Trust’s constitution; that they meet all the criteria for being a fit and proper person as defined in the Social Care Act 2008 (Regulated Activities) Regulations 2008; and that there are no other grounds under which I would be ineligible to continue in post.
Executive Directors
| Criteria | Dr Sara Munro | Nichola Sanderson | Dawn Hanwell | Dr Christian Hosker | Joanna Forster Adams | Darren Skinner |
| a) Are they a person who has been adjudged bankrupt or whose estate has been sequestrated and (in either case) have not been discharged? | No | No | No | No | No | No |
| b) Are they a person who has made a composition or arrangement with, or granted a trust deed for, any creditors and not been discharged in respect of it? | No | No | No | No | No | No |
| c) Are they a person who within the preceding five years has been convicted of any offence if a sentence of imprisonment (whether suspended or not) for a period of not less than three months (without the option of a fine) being imposed on you? | No | No | No | No | No | No |
| d) Are they subject to an unexpired disqualification order made under the Company Directors’ Disqualification Act 1986? | No | No | No | No | No | No |
| e) Do they meet all the criteria for being a fit and proper person as defined in the Social Care Act 2008 (Regulated Activities) Regulations 2008. | Yes | Yes | Yes | Yes | Yes | Yes |
Non-executive Directors
| Criteria | Merran McRae | Zoe Burns-Shore | Kaneez Khan MBE | Dr Frances Healey | Cleveland Henry | Martin Wright | Katy Wilburn |
| a) Are they a person who has been adjudged bankrupt or whose estate has been sequestrated and (in either case) have not been discharged? | No | No | No | No | No | No | No |
| b) Are they a person who has made a composition or arrangement with, or granted a trust deed for, any creditors and not been discharged in respect of it? | No | No | No | No | No | No | No |
| c) Are they a person who within the preceding five years has been convicted of any offence if a sentence of imprisonment (whether suspended or not) for a period of not less than three months (without the option of a fine) being imposed on you? | No | No | No | No | No | No | No |
| d) Are they subject to an unexpired disqualification order made under the Company Directors’ Disqualification Act 1986? | No | No | No | No | No | No | No |
| e) Do they meet all the criteria for being a fit and proper person as defined in the Social Care Act 2008 (Regulated Activities) Regulations 2008. | Yes | Yes | Yes | Yes | Yes | Yes | Yes |
Minutes for the Public Board of Directors Thursday 29 May 2025 at 9:30am
Held in the in Inspire@ room at Horizon Leeds, 3rd Floor, 2 Brewery Wharf, Kendall Street, Leeds, LS10 1JR.
Attendance
Board members
| Name | Role | Apologies |
| Mrs M McRae | Chair of the Trust | Attended |
| Mrs Z Burns Shore | Non-Executive Director | Attended |
| Mrs J Forster Adams | Chief Operating Officer | Attended |
| Mrs D Hanwell | Chief Financial Officer and Deputy Chief Executive | Attended |
| Mr C Henry | Non-Executive Director (Senior Independent Director) | Attended |
| Dr F Healey | Non-Executive Director | Attended |
| Dr C Hosker | Medical Director | Attended |
| Ms K Khan MBE | Non-Executive Director | Attended |
| Dr S Munro | Chief Executive | Attended |
| Mr D Skinner | Director of People and Organisational Development | Attended |
| Miss N Sanderson | Director of Nursing and Professions | Attended |
| Miss K Wilburn | Non-Executive Director | Sent apologies |
| Mr M Wright | Non-Executive Director (Deputy Chair of the Trust) | Attended |
All members of the Board have full voting rights.
Also in attendance
- Mrs C Edwards – Associate Director of Corporate Governance / Trust Board Secretary
- Mr K Betts – Corporate Governance Officer
- Mr Peter Johnstone – Head of Operations (for minute 25/052)
- Mrs Shereen Robinson – Freedom to Speak Up Guardian (for minute 25/068)
- One member of the public attended the meeting
Minutes
Mrs McRae opened the public meeting at 09:30 and welcomed everyone.
25/051 – Apologies for absence (agenda item 1)
Apologies were received from Miss Katy Wilburn, Non-Executive Director. The meeting was quorate.
25/052 – Sharing stories – Learning Disabilities Service (agenda item 2)
Sharing stories – Learning Disabilities Service (agenda item 2)
Mrs McRae welcomed Mr Peter Johnstone to the meeting who introduced himself to the Board, noting that he would be sharing details of a project in the Learning Disability Service involving videos co-produced with service users about the Specialised Supported Living Service. He noted that the service had been in a challenging position 12 months ago with ten tenancy vacancies, however the vacancies had reduced over the last year. As the service was not suitable for prospective clients to undertake home visits, videos were developed to support those moving into the service.
Mr Johnstone shared two videos with the Board which were stories of those already within the service to show the tenant and family experience of moving into the service, and an overview of the facilities and rooms. They were shown to prospective clients but also used by social workers to promote and share the service. He added that the videos were shared with consent and could only be accessed via a link shared by the service. Both videos had been useful and supported discussions with potential tenants and families. The overall aim was to develop a film for each of the 16 houses with a need to consider how to ensure service user engagement was undertaken appropriately to develop a library of resources to share and utilise.
Mrs Forster Adams thanked Mr Johnstone and noted that the Board had heard about the financial challenges of the service but understood the effort and work to fill vacancies. She queried the timeframe for planning and familiarising tenants with the houses before moving in. Mr Johnstone responded that the service was working with partners to develop a reasonable timescale to support the moving in process, noting that there was a need to allow a respectful period for staff and tenants before new tenants arrived. The aim was to get to a 4-week period from nomination of tenancy to visits and overnight stays, with moving in to take place within 8 weeks in total.
Mr Henry thanked Mr Johnstone for bringing the service to life and showing the important role of families in supporting tenants to move into houses which was demonstrated through the videos. Ms Khan acknowledged the cultural perspective for families who take on caring roles which was important to show through the videos, and the positive element of showing tenants gaining more independence was important.
Mrs McRae queried the requirement for a review of learning disability services across Leeds, and Mrs Forster Adams, noted the difficulty was it had only recently been agreed that a multi-agency group would come together to review services across Leeds and the requirements moving forward. Mr Johnstone added that there was a need for an independent review of the learning disability landscape to review what was needed over future years. Dr Munro noted that this was not an area being considered nationally despite significant shifts in life expectancy and the services required over recent years. She acknowledged that guidance and toolkits were being developed to review provision at a local level, but a national widescale review was not in place, therefore there was an opportunity to drive this forward in Leeds. Mrs Hanwell added that there was a need to consider the health component of service user needs, and this should be considered in the strategy and multi-agency complexity requirements for service provision, including housing and funding arrangements.
Mrs McRae thanked Mr Johnstone for attending the meeting and encouraged service visits.
The Board of Directors thanked Mr Johnstone for attending the meeting and sharing the engagement work within the Learning Disability Service.
25/053 – Declaration of interests for directors and any declared conflicts of interest in respect of the agenda items (agenda item 3)
The Board of Directors noted that there had been no changes in the declarations of interest.
25/054 – Minutes of the previous meeting held on 27 March 2025 (agenda item 4)
The minutes of the meeting held on 27 March 2025 were received and agreed as an accurate record.
25/055 – Matters arising (agenda item 5)
Matters arising (agenda item 5)
Mr Wright requested an update regarding the recognition of carer experience as a protected characteristic. Mrs Burns Shore noted that it had been discussed at Workforce Committee, but more work was needed. There was a belief that support for colleagues was in place for care leavers, but there was a service design element to be considered. Mr Skinner confirmed that the Equality Act defined the protected characteristics, therefore making it a protected characteristic had legal requirements. Mrs McRae noted that the original ask was to treat it as equal to a protected characteristic to which Mr Skinner noted that what was currently done by the Trust was probably equal, but review was needed. Dr Munro noted that the Trust had signed up to the NHS England Carers Charter and the challenge was about constitution and employment procedures to take it a step further which the City Council were looking to implement. She added that conversations were ongoing in the Council with a long programme of work with incremental steps planned due to the consequences from a liability perspective.
Ms Khan noted that the protected element of characteristics was invaluable and important to consider, and that there was a need to consider whether those with lived experience felt that the Trust were meeting the requirement. Mrs McRae added that when the update was provided to the Council of Governors it would be helpful to be clear on the work the Trust was already doing and the adherence to supporting charters.
The Board of Directors noted that there were no matters arising.
25/056 – Actions outstanding from the public meeting of the Board of Directors (agenda item 6)
Mrs McRae presented the action log which showed those actions previously agreed by the Board in relation to the public meetings, those that were completed and those that were still outstanding. It was noted that there were a number coming back to Board in September 2025, and all others were noted to have updates provided or be completed.
In relation to action 27 regarding intention planning, Dr Munro noted that this had been discussed, and intention planning was not going to be mandated as the focus would remain on civility and respect with a programme of work in place. If it became mandated the level of resource required to monitor it would be unmanageable. She added that there were several programmes around bank staff therefore the Executive Directors were content this was in an appropriate process through the Workforce Committee. Dr Healey noted that within the staff survey, local results showed levels of variations therefore next year it would be helpful to look at those areas where results were not optimum to consider whether they were universal or locality specific issues. The action was agreed as completed.
In relation to action 23 which was noted as complete, Dr Munro confirmed that the internal audit relating to appraisals would be reviewed by the Workforce Committee as required.
The Board received the cumulative action log, agreed to close the actions that had been completed and noted the updates provided for ongoing actions.
25/057 – Report from the Chief Executive (agenda item 7)
Dr Munro presented the Chief Executive’s report, taking the content as read, and acknowledging the paper on priorities to follow later in the agenda.
She highlighted the engagement events underway which closed off the Well Led Review action regarding sharing the Trust priorities, and a Frequently Asked Questions pack from the sessions would be shared with the wider organisation. In relation to industrial action, she noted the ballot underway for Resident Doctors.
She informed the Board that the Leeds System Review launch event would take place the following day, with the Value Circle the chosen provider for the review. The launch event was the start of the process for a broad set of stakeholders to have an opportunity to shape the programme of work to ensure appropriate involvement, with the initial report expected by the end of September 2025. In addition, the leadership arrangements for LCH were noted, and the Chair for Leeds Teaching Hospitals would be announced in due course.
Dr Munro noted that the ICB draft structures were due to be submitted to NHS England regional teams with follow up responses by mid-June for any proposed iterations. The staff consultation would commence in July 2025 for 45 days, with a 45% reduction in headcount for West Yorkshire ICB. No changes would be made to the footprint of the ICB. There was a high-level proposal for a smaller Place based team with alignment of ICB functions and provider partnership arrangements being key in arrangements. There was uncertainty regarding the changes for the ICB as there was no agreement of funding for redundancies and national agreements for processes were not yet agreed. She noted that the blueprint for the role and structure of regional teams to undertake provider assurance for performance and quality was expected.
The Provider Assurance Framework was noted to be out for consultation with Trusts segmented; the Trust were in segment 2 primarily due to out of area placement, and the proposed new framework would include an indication of Trust positions.
Dr Munro noted it was as important as ever to include the Reasons to be Proud given all the changes underway, and it was important to recognise staff continuing to deliver the day job.
Mrs McRae noted that the Non-Executive Directors had requested an update on the blanket vacancy freeze and assurance on whether not filling vacancies posed any safety or quality risks. Dr Munro noted that that whilst a full freeze was in place, any exceptional requests would be reviewed by the Executive Directors weekly and approved if appropriate. The scale of the financial challenge meant that until teams had the opportunity to review working within a smaller budget the Trust was at risk of recruiting to posts that would not exist in the future. The freeze was in place for a 4-week period whilst a high-level request was underway to consider the financial gap and team structures required to deliver this. She confirmed that teams were aware of the route for exceptional requests. She added that this process released staff involved in the Vacancy Management Panel to support staff to consider the changes needed within teams to meet the financial challenge.
Dr Munro noted that as the scale of redundancies across organisations became known, opportunities for the use of vacancies to support movement across jobs would be in place. Mr Skinner noted that there was a Memorandum of Understanding in place from previous working arrangements that would be used for this. Mrs McRae acknowledged it was helpful to understand the nuance and processes underneath the blanket decision.
Mrs Burns Shore queried how the cost per head of population had been reached, and Dr Munro responded it was a weighted average approach that NHS England implemented nationally for ICBs. In relation to the risk to the Trust regarding the 45% reduction at ICB level, Dr Munro confirmed that this was not known yet as decisions had not been made in relation to where functions would ultimately sit. A Transition Group had been established for accountable officers to oversee the changes which would allow for a wider review of functions and roles. Mrs Hanwell added that legal changes would be required to implement the blueprint which would need to be factored into the process including times and finance for statutory and legal changes.
Mrs McRae thanked Dr Munro for the report.
The Board received the report from the Chief Executive and noted the content.
25/058 – Report from the Chair of the Finance and Performance Committee for the meetings held on 22 April and 27 May 2025 (agenda item 8)
Mr Henry presented the Chair’s report from the Finance and Performance Committee meetings on 22 April and 27 May 2025, and acknowledged that the reports from the Chief Operating Officer and Chief Financial Officer would cover some of the updates.
He noted the focus at the April 2025 committee on the month 12 financial performance, budget versus run rate, and system position. He noted the update regarding the corporate growth reduction and agency trajectories. The committee reviewed the Digital Plan and innovation within capital constraints acknowledging the focus on driving forward with the right technology. The committee received assurance from the EPRR annual report and PAM report.
The May 2025 committee meeting focused on the month 1 financial position, discussion regarding the growth reduction challenge and the work underway regarding the benchmarking process. He noted the Chief Operating Officer report content and the review of the organisational priorities for 2024/25 and proposed priorities for 2025/26. The Information Governance Annual Report was received for assurance purposes.
Mrs Forster Adams clarified that the EPRR Annual Report would be presented to the Board in July 2025 alongside the Assurance Report. She added that the Section 136 detentions would no longer be reported at Board level but would be reviewed at the Mental Health Legislation Committee.
Mr Wright acknowledged the stress put on teams for understandable reasons related to the use of bank staff, targets for financial delivery, and the vacancy freeze, and that the pressure and scrutiny staff were under should be recognised. Mr Henry acknowledged that the detail seen at Finance and Performance Committee demonstrated the work underway and the data supported the changes implemented but it was important to be mindful of the impact on staff.
The Board of Directors received the Chair’s reports from the Finance and Performance Committee and noted the matters reported on.
25/059 – Report from the Chief Financial Officer (agenda item 9)
Mrs Hanwell presented her Chief Financial Officer’s report, noting the discussion at Finance and Performance Committee regarding the month 12 position to confirm the Trust had delivered all requirements.
She noted that month 1 was challenging to give an indication of the position, which was broadly on plan currently, however it was important to note the scrutiny in place regarding the £18.5 million gap at a local and system level with a fortnightly review in place. She added that the capital plan was agreed for 2025/26 as shown in the report, and opportunities and risks would continue to be reviewed as they arose.
The corporate benchmarking return was to be completed by Friday 30 May 2025 and a ‘comply or explain’ approach would be reported via the Finance and Performance Committee, with further efficiencies for corporate services to be reviewed as part of the work within the Trust.
She noted that the new scorecard and metrics for segmentation had a clear link in the domains to the national priorities which was reflected within the Trust priorities for 2025/26.
In relation to the corporate benchmarking, Mr Wright noted it was challenging to undertake it across organisations and compare and queried whether further work was underway to look at nearest comparators to understand potential areas of focus. Mrs Hanwell responded that there were opportunities for collaborative working which was underway led by Directors of Finance and Executive Directors to consider further areas for review, which may also be driven forward by the Leeds System Review.
Mrs Burns Shore queried whether the budget review could likely mean redundancies, and Mrs Hanwell responded that the substantive pay budget was underspent in the full year and the run rate was due to overspends and bank or agency use, therefore the vacancy freeze allowed alignment with staffing structures to avoid redundancy scenarios. She added that the ‘comply or explain’ approach for corporate benchmarking covered some of the growth reasons and from month 2 would have additional elements in for monitoring corporate growth.
Mrs McRae thanked Mrs Hanwell for the report.
The Board received the Chief Financial Officer’s report and noted the content.
25/060 – 2024 – 2025 Organisational Priorities Quarter 4 Progress Report & 2025 – 2026 New Organisational Priorities (agenda item 10)
Mrs Hanwell presented the report noting the detail closing the 2024/25 position, highlighting the completion of 5 priorities with the others being continued and carried forward into 2025/26. She noted the rigorous process to develop the 2025/26 organisational priorities, grouping them into three distinct areas, with the link to national mandates and performance monitoring processes.
Dr Healey acknowledged the achievements within 2024/25 and the complexity of the work. She queried when the quality dashboard would be available at Trust level, which may link to financial and workforce metrics in integrated reporting, but was needed for broader quality metrics which were important to give oversight at a Trust level. Dr Hosker responded noting the rigour behind the metrics had moved towards a focus on quality and culture, and the aligned metrics would include mandated metrics supported by local level metrics. He added that if the Quality Committee needed a specific data set that could be worked into the alignment process. Dr Healey noted that the metrics were needed for the Board and Quality Committee, for committee and board level assurance. She noted that the Board needed to understand the timescales and deliverables. Dr Hosker noted that the Quality Dashboard was available on Echo with multiple metrics, but it needed further development to narrow it down to key oversight needs. Dr Munro added that there was lots of data available, and the challenge was how to covert this into intelligence for assurance or indicator purposes at Committee and Board level to support improvements in performance.
Dr Munro informed the Board that the Board Development Session in June 2025 would focus on improvement and efficiencies, and an update regarding the dashboard would be brought to that session. She noted it would need to move to implementation with the acknowledgement that it may not be perfect and would be worked through. Mrs McRae commented that there was a need to consider how to align the data to committees and Board and the requirement for the content of the Quality & Culture Dashboard at assurance level, with the proposal to be shared at the June 2025 Board session.
Discussion took place regarding the support required from Non-Executive Directors regarding the priorities, and it was noted that committees could support the creative thinking process around how to do this. Dr Munro added that the use of private and other Board time would be key to the delivery of the priorities, such as discussions around corporate functions and how this would work across organisations, the integration of pathways led by Mrs Forster Adams, and the Leeds system review implications including future organisational direction. She noted it would be important to use time to debate the ideas and shape decisions and the operational priorities would help the Trust to support the system review and partnership working arrangements.
Mrs McRae thanked Mrs Hanwell for the report.
The Board of Directors received the 2024 – 2025 Organisational Priorities Quarter 4 Progress Report, and the 2025 – 2026 New Organisational Priorities and noted the content.
25/061 – Report of the Chief Operating Officer (agenda item 11)
Mrs Forster Adams presented her report, noting the depth of the discussion at Finance and Performance Committee. She noted that the report demonstrated how alignment of work was underway and how it would be implemented through different approaches. The report started to introduce detail on priority areas of work which would be transformational.
She highlighted the focus on Emergency Department (ED) performance and the collective work needed to reduce the waits in ED for mental health admissions and support. She noted that the Trust was not yet able to systematically report on ED waits, however work continued regarding electronic systems to provide this, however there was no timeline as yet.
She noted the ongoing discussions regarding contract agreements and the optimisation of community MH transformation to support this. She highlighted the temporary closure of Oasis Crisis House and that the Trust had worked with colleagues to optimise the model which had improved, however estates work meant this would be closed for 10 weeks. She acknowledged the high-risk nature of this closure for short term support provision and the improving patient flow programme and consideration of mitigation and different operating models for that period of time was underway.
She highlighted the improvement in crisis responsiveness due to a change in the operating model to have a locality focus which had led to an improvement in the recruitment of staff into services to support resilience.
She informed the Board of four programmes of work that would include and engage all in Care Services:
- Optimise community mental health transformation in LYPFT which was being scoped currently.
- Inpatient quality transformation programme which incorporated the improving patient flow programme of work and provided a broader focus.
- Reducing Waits in ED as referred to previously which balanced clinical risk with community requirements.
- Transformation of children and young people’s mental health services which would include transition between services and would be an area of focus at the Board Strategic Discussion Day in June 2025
Ms Khan noted the issues regarding the safeguarding supervision target and staff burnout due to stress which was acknowledged at Workforce Committee. Miss Sanderson responded that there were a broad range of strategies in place regarding supervision, and practitioners were working with teams including enhanced services to support the staff in those areas. She noted that the recording of supervision had been challenging when determining what should be included.
In relation to Aspire, Ms Khan queried the confidence regarding progress being seen, and Mrs Forster Adams responded that she was confident that collaborative work on a recovery plan was underway and would be monitored for effectiveness. She added that the review of pathways and community optimisation would support this in the longer term. In relation to the email threat referred to in the report, she noted that this had been sent to each provider in the country and was hostile, rather than a threat, about the Supreme Court ruling.
Dr Healey noted that the Board needed to support transformational change through innovative solutions as despite partnership working and best efforts on aspects within our control, substantial challenges remain. Mrs Forster Adams acknowledged that the programmes of work planned would give the Board opportunity to review progress and provide an additional level of challenge for approaches taken.
Mrs McRae queried whether hubs would support the ED work programme, and Mrs Forster Adams noted that they would be supportive for improvements.
Mrs McRae thanked Mrs Forster Adams for her report.
The Board received the Chief Operating Officer report and discussed the content.
25/062 – EPRR (agenda item 12) and EPRR & Business Continuity Policy (agenda item 12.1)
Mrs Forster Adams took the policy as read and noted it was at the Board for approval in line with EPRR standards.
Mrs McRae noted it was disappointing that there was low up take for strategic commander training therefore there was a need to have executive oversight of the processes.
The Board approved the EPRR and Business Continuity Policy and Mrs McRae thanked Mrs Forster Adams for her report.
The Board received the EPRR and Business Continuity policy and approved the content.
25/063 – Report from the Chair of the Quality Committee for the meetings held on 10 April and 8 May 2025 (agenda item 13)
Dr Healey presented the Chair’s Reports from the Quality Committee meetings held on 10 April and 8 May 2025, taking them as read.
She highlighted the focus on actions taken in response to incidents, complaints, etc. as key to assurance, and the current pause on one regular report to review the content and requirements moving forward.
She made a clarification regarding the referral to the Audit Committee noting that this related to First Aid Training as part of Health and Safety legislation; the referral had been completed.
She confirmed that appropriate action had been agreed regarding clarifying oversight of investigations of incidents in the spot purchased beds.
Mrs McRae thanked Dr Healey for the reports.
The Board of Directors received the Chair’s reports from the Quality Committee and noted the matters reported on.
25/064 – Report from the Director of Nursing and Professions (agenda item 14)
Miss Sanderson presented the report taking it as read by the Board, highlighting the Task and Finish groups established to progress the programmes of work to improve the quality of care and improve efficiencies. She noted that CPD funding was available for 2025/26 and would be used appropriately in areas that had not previously benefited from it. She highlighted the work of Amy Pratt, staff governor, as part of national guidance for catering in mental health settings.
She also noted the significant piece of work that had been undertaken regarding early warning score approaches across all services and the documentation of mental health assessments.
Mrs McRae thanked Miss Sanderson for the report acknowledging the content within the report, including the CPD funding. In relation to the Patient Safety Partners recruitment delay, Mrs McRae asked if this would be reported through the Quality Committee, and Miss Sanderson confirmed it would.
The Board of Directors received the Report of the Director of Nursing and Professions and noted the content.
25/065 – Review of the Independent Investigation into the Care and Treatment provided to VC (agenda item 14.1)
Miss Sanderson presented the report taking it as read by the Board. She noted it was important to reflect on the recommendations that provider Trusts were responsible for ensuring were in completed and added that the current position provided assurance that these were underway and linked into existing work streams. She noted that attention would not be solely on these recommendations, as there would also be a review of internal areas of priority following investigations and patient safety related issues internally.
Mrs McRae thanked Miss Sanderson for the report noting the positive responses to the recommendations from work underway already. She queried whether there was a tracking system given the number of recommendations from a variety of sources, and Miss Sanderson confirmed that this was in place and linked to the priorities. She also noted that the amended approach to reporting was being worked through to provide assurance whilst not reverting to lengthy reports as per previous processes.
The Board of Directors received the review of the Independent Investigation into the Care and Treatment provided to VC and noted the content.
25/066 – Report from the Chair of the Workforce Committee for the meeting held on 30 April 2025 (agenda item 15)
Mrs Burns Shore presented the Chair’s report, highlighting the review of the People Plan and core priorities identified. She noted the issue regarding the alignment of training and sickness information regarding stress and MSK absence, therefore the focus was on mandatory training compliance. She noted the discussion regarding the bank forum and the desire to choose bank work over substantive roles, however there was a successful conversion from bank to substantive roles and work with the bank would continue.
Discussion took place regarding the data for MSK and stress training and absence, and Mr Skinner agreed to provide the detail on numbers of staff affected to understand the scale of the issue.
Mr Henry noted the link between bank staff who do not want to take on substantive roles and the drive to reduce bank use, and Mr Skinner noted that this was a national pressure to balance as all organisations were to deliver the reduction in bank use.
Mrs McRae thanked Mrs Burns Shore for the report.
The Board of Directors received the Report from the Chair of the Workforce Committee and noted the content.
25/067 – Workforce Committee Terms of Reference (agenda item 15.1)
The Board of Directors received and approved the Workforce Committee Terms of Reference.
25/068 – Freedom to Speak Up Guardian Annual Report (agenda item 16)
Mrs Robinson presented the report taking it as read noting the slight increase in number of concerns in comparison to the previous year. She noted the recent internal Audit had provided high assurance however work was taking place on the recommendations including barriers to speaking up. This included work with the Guardian of Safe Working to promote the service with medical staff, but with the acknowledgement that they had other routes to raise concerns. She informed the Board that recruitment for ambassadors had been paused at the current time, and the evaluation forms had been updated to measure success of communication from the service.
Due to the number of perceived unfair work practice or process concerns, work was underway regarding reminders of the policies in place. She noted that further review of neurodiversity related concerns would take place to understand if additional manager support was needed for this.
In relation to learning, Mrs Robinson informed the Board that the Trust was taking on board the National Guardian Office learning and that the policy was to be amended to make it clear that the service did not undertake investigations on concerns. She noted the awareness of national changes such as sexual harassment including the Trust sign up to the Sexual Safety Charter. She added that there was cultural awareness training underway for international nurses following national learning.
She noted that at the Board Strategic Discussion Day in October 2025 there would be a focus on the Freedom to Speak Up Annual Return and the role of the Board for leadership and role modelling.
Mr Henry commented that as the Non-Executive Director with a lead for Freedom to Speak Up, the communication plan was positive in relation to awareness of the service across the Trust services and the importance of the right routes of signposting of concerns. He noted that there may be an increase in concerns regarding the financial and workforce decisions to be made moving forward, demonstrating the importance of communication as this progresses.
Mr Wright thanked Mrs Robinson for the report, acknowledging the internal audit report finding. He added that the staff survey results would indicate there should perhaps be more referrals to the service using the role of the ambassador to bridge the gap and queried if there was more to be done. Mrs Robinson responded that the use of the ambassador network was reflected in the staff survey results and it was important to note that there were multiple ways to raise a concern so they may not all come through the service. Mr Skinner confirmed that triangulation of all data sources took place to review data as a whole.
Dr Healey queried the process for patient safety or quality related issues, and Mrs Robinson confirmed that they were flagged through the Chief Executive and Medical Director to escalate or ask for support. Dr Healey acknowledged the process for individual incidents had been previously explained to board, but that the themes and patterns of quality-related issues raised through this route were also useful information for Quality Committee. Ms Sanderson suggested this might be part of the review of regular reports of themes and actions taken in response from various data sources provided to Quality Committee and Mrs Robinson and Ms Sanderson agreed to discuss this.
Mrs McRae thanked Mrs Robinson for the report.
The Board received the Freedom to Speak Up Guardian report and discussed the content.
25/069 – Report from the Chair of the Mental Health Legislation Committee for the meeting held on 15 May 2025 (agenda item 17)
Ms Khan presented the Chair’s report, taking it as read by the Board, highlighting the discussion regarding the Section 136 mandated target which had led to a review of how the Trust benchmarked with other organisations.
The reduction in mental health legislation training required a manual check for performance detail therefore was to be referred to the Workforce Committee. Mrs Burns Shore noted that it would be more appropriate for this to be managed via the People and Organisational Development Governance Group with escalation to the Committee if needed.
Mrs McRae queried whether the 0% recording for Section 136 data was noted by the Committee, and Dr Hosker noted that this had been an ongoing issue in relation to the reporting of reviews and when the time frame relates to multiple professionals. Ms Khan noted that this was the reason for the benchmarking review to potentially provide different ways of recording and learning opportunities.
The Board received and noted the content of the Report from the Chair of the Mental Health Legislation Committee.
25/070 – Report from the Chair of the Audit Committee for the meeting held on 8 April 2025 (agenda item 18)
Mr Wright presented the Chair’s report, taking it as read, noting the internal audits received and varying levels of assurance provided. The committee had reviewed all the reports and were content with the recommendations in place. He noted that the Head of Internal Audit opinion was indicative of a positive result which was welcomed. He thanked all committees for reviewing the internal audit plan for 2025/26 which had now been agreed.
He noted that the committee continued to work on Health and Safety, and the distinction between health and safety and patient safety, and the appropriate definitions and parameters for review.
The Board received and noted the content of the Report from the Chair of the Audit Committee.
25/071 – Board Assurance Framework (agenda item 19)
Dr Munro presented the updated version of the Board Assurance Framework, and specifically noted the upgraded risk rating for Strategic Risk 4 to a level 15 due to the financial pressures as noted and discussed during the meeting. She added that the action deadline dates would continue to be reviewed as part of the review process.
Mr Wright noted that he had attended the Audit Committee for Leeds Teaching Hospitals and noted their different approach to risk management and risk register reporting process at Committee level due to the complexity of the acute organisation. He felt that this provided assurance for our approach within the Trust. Dr Munro added that the risk register was reviewed via the Executive Risk Management Group which provided an escalation route for this rather than in depth reviews of each directorate risk register.
Mrs McRae thanked Dr Munro for the report.
The Board received the Board Assurance Framework and noted the content.
25/072 – Fit and Proper Person Declaration (agenda item 20)
Mrs McRae referred to the report, taking it as read by the Board, thanking all for their contributions. The Board noted the compliance with the Fit and Proper Person declaration.
The Board received and noted the Fit and Proper Person Declaration for 2024/25.
25/073 – Self-certification against condition CoS7 of the provider licence (agenda item 21)
Dr Munro presented the report, taking it as read by the Board, noting the legal requirement of the position and review by the Audit Committee.
The Board noted agreement with the compliance certification.
The Board received and noted the Self-certification against condition CoS7 of the provider licence report.
25/048 – Use of Trust Seal (agenda item 22)
The Board noted that the Trust Seal had not been used since the previous meeting.
25/049 – Any other business (agenda item 23)
Mr Henry commented that the workforce and agency trajectory plan and digitalisation of admin tasks linked to some discussions in the meeting and the use of advances in technology to support processes and improve reporting opportunities and compliance was important to consider and keep at the fore of discussions.
Mrs McRae noted that the link to the report to be completed for the Freedom to Speak Up section of the Board Strategic Development Day in October would be shared ahead of the session for review.
The Board noted the additional item of business raised.
25/050 – Resolution to move to a private meeting of the Board of Directors
At the conclusion of business, the Chair closed the public meeting of the Board of Directors at 12:30 and thanked members of the Board and members of the public for attending.
The Chair then resolved that members of the public would be excluded from the meeting having regard to the confidential nature of the business transacted, publicity on which would be prejudicial to the public interest.
Return to agenda
Actions outstanding from the public meetings of the Board of Directors
Open Actions
| Log number | Action (including the title of the paper that generated the action) | Person who will complete the action | Meeting to be brought back to / date to be completed by | Update report – comments |
| 24 | Sharing stories – Supporting carers to care with confidence (minute 25/025 – agenda item 2 – March 2025)
It was agreed that a response on updates to the asks for support would be provided to the Board in six months’ time, with Miss Sanderson taking the lead on the action. |
Nichola Sanderson | September 2025 | Ongoing |
| 25 | Report from the Chief Financial Officer (minute 25/040 – agenda item 16 – March 2025)
It was agreed that an update regarding the run rate and justification for staffing levels work would be brought back to the Board in six months time. |
Nichola Sanderson | September 2025 | Ongoing |
| 28 | 2024 – 2025 Organisational Priorities Quarter 4 Progress Report & 2025 – 2026 New Organisational Priorities (minute 25/060 – agenda item 10 – May 2025)
Mrs McRae commented that there was a need to consider how to align the data to committees and Board and the requirement for the content of the Quality & Culture Dashboard at assurance level, with the proposal to be shared at the June 2025 Board session. |
Chris Hosker | June 2025 (Board Strategic Development Day) | New Complete This was discussed at the Board Strategic Discussion day in June 2025. |
| 29 | Report from the Chair of the Workforce Committee for the meeting held on 30 April 2025 (minute 25/066 – agenda item 15 – May 2025)
Discussion took place regarding the data for MSK and stress training and absence, and Mr Skinner agreed to provide the detail on numbers of staff affected to understand the scale of the issue. |
Darren Skinner | Management action | New Complete Data has been provided by Mr Skinner (document circulated – item 6.1). |
Closed actions
| Log number | Action (Including the title of the paper that generated the action) | Person who will complete the action | Meeting to be brought back to / date to be completed by | Update report – comments |
| 19 | Report from the Chief Financial Officer (minute 25/010 – agenda item 10 – Jan 2025)
Ms Burns-Shore queried whether NHS organisations could be expected to share services going forward. Mrs McRae noted that this would be discussed further at the April 2025 strategic board development day and asked Mrs Hanwell to provide information ahead of this session on what shared services the Trust had. |
Dawn Hanwell | April 2025 | Complete This was included in the Board Strategic Development Day in April 2025. |
| 26 | Staff Survey Results (minute 25/043 – agenda item 18 – March 2025)
It was agreed that the Workforce Committee would review the bank staff results in more detail. |
Workforce Committee | Management action | Complete This has been included on the Workforce Committee forward plan for agenda items |
| 27 | Staff Survey Results (minute 25/043 – agenda item 18 – March 2025)
It was agreed that the Executive Management Team would consider whether intention planning should be mandated and how to address bank and substantive staff result differences through committee or board, or other ongoing workstreams. |
Executive Management Team | Management action | Complete It was noted that intention planning was not being mandated as there were existing programmes in place to support the required workstreams for civility and respect. |
Actions from Committees for the Board of Directors
None.
Return to agenda

Bar chart comparing the percentage of total musculoskeletal problems, S12 (Other musculoskeletal problems) and S11 (Back Problems), across various NHS regions and trusts. The x-axis shows percentages from 0.00% to 12.00%. The y-axis lists the following regions and trusts, along with their approximate values: Tees, Esk and Wear Valleys NHS Foundation Trust – S12: 8%, S11: 3%, South West Yorkshire Partnership NHS Foundation Trust – S12: 8%, S11: 5%, Rotherham, Doncaster and South Humber NHS Foundation Trust – S12: over 10%, S11: over 4%, Leeds Teaching Hospitals NHS Trust – S12: 9%, S11: over 4%, Leeds Community Healthcare NHS Trust – S12: over 7%, S11:over 3%, Leeds and York Partnership NHS Foundation Trust – S12: 9%, S11:3%, Bradford District Care NHS Foundation Trust – S12: over 7%, S11: over 4%. Each region displays two bars representing the two categories of musculoskeletal problems.
Cover sheet for Responsible Officer Annual report 1 April 2024 – 31 March 2025
- Paper title: Responsible Officer Annual report 1 April 2024 – 31 March 2025
- Date of meeting: 31 July 2025
- Presented by: Wendy Neil, Responsible Officer
- Prepared by: Wendy Neil, Responsible Officer
This paper supports the Trust’s strategic objective/s (SO):
- SO1 – We deliver great care that is high quality and improves lives.
- SO2 – We provide a rewarding and supportive place to work.
- SO3 – We use our resources to deliver effective and sustainable services.
This paper relates to the Trust’s strategic risks (SR):
- SR1 – Quality including safety assurance processes
- SR2 – Delivery of the Quality Strategic Plan
- SR3 – Culture and environment for the wellbeing of staff
- SR5 – Adequate working and care environments
Executive summary
This report has been produced using the template provided by NHS England, setting out the information and metrics that a designated body is expected to report upwards, to assure their compliance with the regulations and commitment to continual quality improvement in the delivery of professional standards.
The report is in four parts:
Section 1 – Qualitative/narrative
Section 2 – Metrics
Section 3 – Summary and conclusion
Section 4 – Statement of compliance
Do the recommendations in this paper have any impact upon the requirements of the protected groups identified by the Equality Act? No
Recommendation
The Board is asked to:
- read and agree that this report provides assurance that the key requirements for compliance with regulations and key national guidance required of LYPFT as a designated body are met.
The Chair is asked to:
- sign the statement of compliance on p18 to enable the completed report to be submitted to NHS England.
Designated Body Annual Board Report and Statement of Compliance
This template sets out the information and metrics that a designated body is expected to report upwards, to assure their compliance with the regulations and commitment to continual quality improvement in the delivery of professional standards.
Section 1 Qualitative/narrative
1A – General
The board/executive management team of Leeds and York Partnership NHS Foundation Trust can confirm that:
1A(i) An appropriately trained licensed medical practitioner is nominated or appointed as a responsible officer.
| Action from last year: | Maintain the current Responsible Officer arrangements |
| Comments: | Nil |
| Action for next year: | Maintain |
1A(ii) Our organisation provides sufficient funds, capacity and other resources for the responsible officer to carry out the responsibilities of the role.
| Yes / No: | Yes |
| Action from last year: | To undertake a mapping exercise to identify any future investment needs to enable the Responsible Officer to fulfil their role, noting in particular the requirements of Good Medical Practice 2024 and the needs of the LYPFT medical workforce. |
| Comments: | The mapping exercise revealed an increase in the number of doctors with a prescribed connection to LYPFT for the past 5 consecutive years (from 112 in 2020/21 to 139 in 2024/25) with further increases projected as a result of reduction in agency locum usage and expansion of the medical workforce in reconfigured services.
A separate exercise confirmed a 4-fold increase in the number of doctors working into LYPFT who have their prescribed connection elsewhere (e.g. doctors who provide clinical sessions into LYPFT as part of a Service Level Agreement) (from 3 in 2020/21 to 12 in 2024/25) with further increases in the number of these doctors also projected. In addition, a benchmarking exercise identified that LYPFT provided less support for the necessary functions of a RO compared with similar Trusts (e.g. with respect to the amount and seniority of administrative support). In an attempt to mitigate against the increase in workload that this increase in doctors has generated for the Responsible Officer and the Medical Directorate team and compounded by the relative lack of resource, various actions have been undertaken in 2024/25 to improve the efficiency of systems and processes used to oversee medical professional standards (e.g. by streamlining the process for review of medical appraisals and by updating the ‘Managing Concerns about Medical Staff’ policy to avoid unnecessary escalation of cases). There remains a risk however that resources provided are not sufficient to enable necessary functions to be undertaken in the forthcoming years and changes and enhancements to the team structure are therefore planned for 2025/26. |
| Action for next year: | To gain approval for, and implement, changes and enhancements to the team structure within the Medical Directorate to ensure sufficient capacity for the Responsible Officer to carry out the responsibilities of the role. |
1A(iii)An accurate record of all licensed medical practitioners with a prescribed connection to our responsible officer is always maintained.
| Action from last year: | Maintain |
| Comments: | A ‘Starters and Leavers’ report is presented at each meeting of the Good Medical Practice Assurance Group (chaired by the RO). The report is generated by cross-referencing data on GMC Connect with data held by the People and Organisational Development Team and in so doing provides assurance that all medical practitioners are connected to the correct designated body.
Additional checks are made around the time of Resident Doctor rotation to ensure the doctor’s prescribed connection is correct. |
| Action for next year: | Maintain |
1A(iv) All policies in place to support medical revalidation are actively monitored and regularly reviewed.
| Action from last year: | A review of the Trust’s Medical Appraisal procedure will take place in 2024/25 to enable consultation, ratification, and dissemination to key stakeholders by October 2025. |
| Comments: | The Trust’s Medical Appraisal Procedure has been reviewed and updated and is on target for ratification by October 2025.
An internal audit conducted by Audit Yorkshire in 2024/25 reviewed the appraisal process for all LYPFT staff. No major issues were identified with the Medical Appraisal process and only 2x minor areas of weakness were identified. These were i) the process of notifications being sent to the Trust’s Learning Management Systems team following a Medical Appraisal and ii) documenting within the Medical Appraisal procedure the requirement to prompt staff to hold a six-month review of the PDP. Both of these areas have since been addressed. |
| Action for next year: | To disseminate and embed into practice the updated Medical Appraisal procedure once ratified. |
1A(v) A peer review has been undertaken (where possible) of our organisation’s appraisal and revalidation processes.
| Action from last year: | To develop and deliver a programme of refresher training for existing appraisers
Next peer review due 2027 unless a sooner date is felt necessary. |
| Comments: | The programme of training for appraisers has been reviewed and was updated in 2024/25.
Appraiser Development forums (ADFs) continue to take place quarterly, with one meeting now combined with the annual training day for new appraisers. This day provides specific training for new appraisers in the morning and joint sessions with new and existing appraisers in the afternoon with the emphasis of this session being on benchmarking and experiential learning. All appraisers continue to have a yearly assurance review when their development needs are discussed and suggestions received for further training. The latter are then incorporated into future ADFs. |
| Action for next year: | Maintain |
1A(vi) A process is in place to ensure locum or short-term placement doctors working in our organisation, including those with a prescribed connection to another organisation, are supported in their induction, continuing professional development, appraisal, revalidation, and governance.
| Action from last year: | Maintain |
| Comments: | Trust employed locum and short-term placement doctors working in LYPFT continue to be managed the same as substantive doctors. They receive tailored local induction and are supported in CPD, appraisal, revalidation and governance.
A Medical In-Post Review Framework was developed in 2024/25 for doctors with a prescribed connection not with LYPFT (e.g. doctors who provide clinical sessions into LYPFT as part of a Service Level Agreement). The Framework has been shared with the relevant doctors and their medical line managers have received training with respect to its completion. Use of the Framework will go live in Q1 2025/26. Its impact and the outputs will be monitored by the Medical Directorate team. |
| Action for next year: | To review the impact and outputs of the new Medical In-Post Review Framework |
1B – Appraisal
1B(i) Doctors in our organisation have an annual appraisal that covers a doctor’s whole practice for which they require a GMC licence to practise, which takes account of all relevant information relating to the doctor’s fitness to practice (for their work carried out in the organisation and for work carried out for any other body in the appraisal period), including information about complaints, significant events and outlying clinical outcomes.
| Action from last year: | To continue to work with the Trust’s risk department to explore ways to improve the accuracy and accessibility of SUI/coroners information and complaints/compliments.
To continue to oversee the provision of a Casenote audit, review the results and develop action plans as appropriate. |
| Comments: | The RO and Head of Medical Development and Operations are now proactively involved in the process of allocation, investigation and oversight of complaints relating to doctors and in ensuring that doctors are provided with appropriate support during this process.
The second annual Trustwide Casenote Audit has been completed and the results discussed at Good Medical Practice Assurance Group. It revealed improved compliance with agreed standards, with the report and individualised results to be uploaded onto doctor’s files on L2P to enable reflection at appraisal. |
| Action for next year: | To continue to oversee the provision of a Casenote audit, review the results and develop action plans as appropriate. |
1B(ii) Where in Question 1B(i) this does not occur, there is full understanding of the reasons why and suitable action is taken.
| Action from last year: | Complete a review, and implement the use, of a new data proforma to provide more detailed and accurate information regarding complaints and significant events |
| Comments: | The Head of Medical Development and Operations and Medical Directorate Administrator have been working with colleagues in the Risk Management Team to improve information specific to complaints and significant events.
This work has led to a review of the Trust’s DATIX reporting system in enabling specific information which supports medical appraisal to be provided at the time of completing a DATIX which then generates reports for doctors’ supporting information for appraisal. |
| Action for next year: | To embed a process within the Medical Directorate to access DATIX and provide doctors with meaningful data for their supporting information. |
1B(iii) There is a medical appraisal policy in place that is compliant with national policy and has received the Board’s approval (or by an equivalent governance or executive group).
| Action from last year: | A review of the Trust’s Medical Appraisal procedure will begin 2024/25 to enable consultation, ratification, and dissemination to key stakeholders in good time for renewal due October 2025. |
| Comments: | The Trust’s Medical Appraisal Procedure has been reviewed and has been submitted to the relevant Trust governance processes. It is on target for ratification by October 2025. |
| Action for next year: | To disseminate and embed into practice the updated Medical Appraisal procedure once ratified. |
1B(iv) Our organisation has the necessary number of trained appraisers to carry out timely annual medical appraisals for all its licensed medical practitioners. While there is no regulatory stipulation on appraiser/doctor ratios, a useful working benchmark is that an appraiser will undertake between 5 and 20 appraisals per year. This strikes a sensible balance between doing sufficient to maintain proficiency and not doing so many as to unbalance the appraiser’s scope of work.
| Action from last year: | To review the content of the appraiser training to ensure that it remains relevant and in keeping with Good Medical Practice 2024 and other local and national standards.
Continue to monitor the number of medical appraisers and, if required, complete further rounds of recruitment. |
| Comments: | The format and content of appraiser training has been reviewed and now includes information on Good Medical Practice 2024 and the locally developed Minimum Dataset for supporting information. LYPFT currently have 25 trained appraisers (16 consultants, 9 SAS doctors). Recruitment continues to take place annually to ensure there remains this necessary number of appraisers to carry out timely medical appraisals. |
| Action for next year: | To continue to review and develop appraiser teaching and training materials to ensure this is relevant to local and national standards.
To continue to monitor the number of medical appraisers and complete further rounds of recruitment as required. |
1B(v) Medical appraisers participate in ongoing performance review and training/ development activities, to include attendance at appraisal network/development events, peer review and calibration of professional judgements (Quality Assurance of Medical Appraisers or equivalent).
| Action from last year: | Obtain and evaluate feedback from the Appraisal Development Forums and implement any developments as appropriate to their future structure and content. |
| Comments: | Appraisal Development Forums (ADFs) are now CPD approved.
Feedback is routinely sought after each ADF from all the participants and used to develop future sessions. Appraisers participate in an annual Appraiser Assurance Review meeting with the Director/Associate Director of Medical Professional Standards where further exploration of development needs and feedback is obtained. Themes are collated and inform topics to be covered in ADFs. The RO and Medical Appraisal and Revalidation leads continue to be actively involved in NHSE and Mental Health Appraisal networks. |
| Action for next year: | To continue to obtain feedback through ADFs and annual Appraiser Assurance reviews to inform topics for future ADFs and training.
To encourage appraiser participation at regional network events. RO to take on the role of chair of the regional Mental Health network and develop a programme of education and development for group members. |
| Action from last year: | Obtain and evaluate feedback from the Appraisal Development Forums and implement any developments as appropriate to their future structure and content. |
| Comments: | Appraisal Development Forums (ADFs) are now CPD approved.
Feedback is routinely sought after each ADF from all the participants and used to develop future sessions. Appraisers participate in an annual Appraiser Assurance Review meeting with the Director/Associate Director of Medical Professional Standards where further exploration of development needs and feedback is obtained. Themes are collated and inform topics to be covered in ADFs. The RO and Medical Appraisal and Revalidation leads continue to be actively involved in NHSE and Mental Health Appraisal networks. |
| Action for next year: | To continue to obtain feedback through ADFs and annual Appraiser Assurance reviews to inform topics for future ADFs and training.
To encourage appraiser participation at regional network events. RO to take on the role of chair of the regional Mental Health network and develop a programme of education and development for group members. |
1B(vi) The appraisal system in place for the doctors in our organisation is subject to a quality assurance process and the findings are reported to the Board or equivalent governance group.
| Action from last year: | Continue to work with L2P to ensure the appraisal documentation is compliant with the requirements of Good Medical Practice 2024.
Review the impact of the Appraiser Assurance Review document and revise/update as appropriate. |
| Comments: | Revised/updated version of L2P now includes all GMP 2024 domains.
Data regarding the quality of the appraisal continues to be reviewed as part of the appraiser’s annual Appraiser Assurance Review meeting in advance of their appraisal. The review documentation has been updated in 2024/25 to improve clarity and consistency. For doctors with additional specific roles in Medical Education a new process to quality assure their work and identify any training and development needs (mirroring the Medical In-Post reviews) has been developed. This will then form part of their annual appraisal and will go live in Q1 2025/26. |
| Action for next year: | To embed the process of quality-assuring Medical Education-related work undertaken by doctors and include this in the supporting information for discussion and reflection at appraisal. |
1C – Recommendations to the GMC
1C(i) Recommendations are made to the GMC about the fitness to practise of all doctors with a prescribed connection to our responsible officer, in accordance with the GMC requirements and responsible officer protocol, within the expected timescales, or where this does not occur, the reasons are recorded and understood.
| Action from last year: | Maintain |
| Comments: | The Good Medical Practice Assurance Group meets bi-monthly to review the progress of all doctors under notice for revalidation. Recommendations regarding fitness to practice are considered at each meeting and where recommendations are agreed, these are submitted to the GMC within two working days of the meeting.
In 2024/25 all recommendations about the fitness to practice of doctors were made to the GMC within the expected timescales with no exceptions. |
| Action for next year: | Maintain |
1C(ii) Revalidation recommendations made to the GMC are confirmed promptly to the doctor and the reasons for the recommendations, particularly if the recommendation is one of deferral or non-engagement, are discussed with the doctor before the recommendation is submitted, or where this does not happen, the reasons are recorded and understood.
| Action from last year: | Maintain |
| Comments: | The Good Medical Practice Assurance Group proactively reviews data obtained from GMC connect about all doctors under notice, including progress regarding MSF and any issues or matters of potential concern.
Should any issues be identified which may possibly result in deferral or non-engagement then the doctor is contacted after the meeting to explore those issues further and provide support for the issues to be addressed. This and any subsequent contacts are documented and shared with the doctor for their information and reflection. As a result of this proactive approach there were 0 deferrals or cases of non-engagement in 2024/25. When a revalidation recommendation is made to the GMC the doctor is informed of this in writing by the RO on the day the recommendation has been approved. |
| Action for next year: | Maintain |
1D – Medical governance
1D(i) Our organisation creates an environment which delivers effective clinical governance for doctors.
| Action from last year: | Maintain |
| Comments: | The Professional Lead for Psychiatry continues to be a member of Trust-wide Clinical Governance and the Good Medical Practice Assurance Group, enabling effective sharing of relevant information between the two groups.
All medical line managers receive annual training regarding their roles and responsibilities including with respect to clinical governance processes. They also receive training as Case Investigators and as such are able to investigate and support doctors should concerns be raised regarding their conduct and/or performance. |
| Action for next year: | Maintain |
1D(ii) Effective systems are in place for monitoring the conduct and performance of all doctors working in our organisation.
| Action from last year: | To develop, implement and evaluate a robust process to ensure that actions arising as a result of investigations into the conduct and performance of doctors are completed and reflected on by the doctor at their appraisal. |
| Comments: | A tracked spreadsheet is kept by the RO of all actions recommended following investigations into the conduct and/or performance of doctors. This is reviewed on a regular basis and the doctor’s details remain on the agenda of the Good Medical Practice Assurance Group until such time as all actions have been signed off as satisfactorily completed.
The incorporation from 1 April 2025 of a new system of Medical In-Post Reviews of doctors with a prescribed connection not with LYPFT (including agency locum doctors and doctors who provide clinical sessions into LYPFT as part of a Service Level Agreement) will ensure improved monitoring of the conduct and performance of these doctors who work in LYPFT but who have their prescribed connection elsewhere. |
| Action for next year: | To review the impact and outputs of the new Medical In-Post Review Framework |
1D(iii) All relevant information is provided for doctors in a convenient format to include at their appraisal.
| Action from last year: | Covered under section 1B (ii) |
| Comments: | Not applicable |
| Action for next year: | Not applicable |
1D(iv) There is a process established for responding to concerns about a medical practitioner’s fitness to practise, which is supported by an approved responding to concerns policy that includes arrangements for investigation and intervention for capability, conduct, health and fitness to practise concerns.
| Action from last year: | For the Trust’s Managing Concerns with Medical Colleagues (MHPS) policy to be ratified and embedded into practice.
To work with the Trust’s Freedom to Speak Up Guardian to ensure that staff feel enabled to raise concerns about medical staff should this be necessary and assured that their concerns will be responded to appropriately. To deliver, in conjunction with NHS Resolution, Case Investigator training for relevant medical and workforce staff within LYPFT and the wider region. |
| Comments: | Managing Concerns with Medical Colleagues (MHPS) policy has been ratified and is embedded into practice.
Trust Freedom to Speak Up Guardian attended meeting of Good Medical Practice Assurance Group and separate 1:1 meetings with RO to ensure a shared understanding of appropriate process for responding to concerns about medical staff. LYPFT now has a full complement of trained Case Investigators (n=28) following a successful training event in 2024. Update/refresher training is scheduled for 2025. |
| Action for next year: | To deliver and evaluate Case Investigator Training |
1D(v) The system for responding to concerns about a doctor in our organisation is subject to a quality assurance process and the findings are reported to the Board or equivalent governance group. Analysis includes numbers, type and outcome of concerns, as well as aspects such as consideration of protected characteristics of the doctors and country of primary medical qualification.
| Action from last year | Annual Equality Impact Assessment (EIA) to be undertaken in conjunction with the MWRES lead to review compliance against MWRES indicators regarding investigations into concerns regarding doctors. |
| Comments | EIA undertaken and results discussed at Good Medical Practice Assurance group. It confirmed that there were 11 cases when concerns were recorded about the conduct and/or behaviour of a doctor in the Trust. This was in keeping with previous years.
The ethnicity of the doctors about whom concerns were raised, and the ethnicity of the Case Investigators was proportionate to the medical workforce. |
| Action for next year | To continue to work with the Medical Workforce Race Equality Standard (MWRES) lead to ensure the Trust responds fairly and appropriately when concerns are raised about doctors.
To undertake an annual Equality Impact Assessment (EIA) in conjunction with the MWRES lead to review compliance against MWRES indicators regarding investigations into concerns regarding doctors. |
1D(vi) There is a process for transferring information and concerns quickly and effectively between the responsible officer in our organisation and other responsible officers (or persons with appropriate governance responsibility) about a) doctors connected to our organisation and who also work in other places, and b) doctors connected elsewhere but who also work in our organisation.
| Action from last year | To embed the process by which MPIT forms are requested within other pre-employment checks undertaken for doctors joining the Trust. |
| Comments | MPIT forms are now requested as standard once notification has been received of a doctor’s recruitment to a role within LYPFT. These are reviewed by the RO.
The RO has regular meetings with the ELA and other ROs to enable benchmarking of practice regarding when and how to escalate concerns. In cases where concerns have arisen, the RO has liaised with the appropriate individuals. |
| Action for next year | Maintain |
1D(vii) Safeguards are in place to ensure clinical governance arrangements for doctors including processes for responding to concerns about a doctor’s practice, are fair and free from bias and discrimination (Ref GMC governance handbook).
| Action from last year | To evaluate the role of the Cultural Inclusion Ambassadors in the Decision-Making Groups. |
| Comments | Evaluation of the role of the Cultural Inclusion Ambassadors in the Decision-Making Groups (now termed ‘Responding to Concerns Advisory Groups’) is underway and due for completion Q1 2025. |
| Action for next year | To complete evaluation of the role of the Cultural Inclusion Ambassadors in the Responding to Concerns Advisory Groups and develop an action plan depending on findings. |
1D(viii) Systems are in place to capture development requirements and opportunities in relation to governance from the wider system, e.g. from national reviews, reports and enquiries, and integrate these into the organisation’s policies, procedures and culture. (Give example(s) where possible.)
| Action from last year | Maintain |
| Comments | The Good Medical Practice Assurance Group continues to include within its agenda a standing item wrt relevant CPD which is then shared with doctors as appropriate. It also includes a ‘topic discussion’ section where external speakers are invited and topics can be debated at greater length. |
| Action for next year | Maintain |
1D(ix) Systems are in place to review professional standards arrangements for all healthcare professionals with actions to make these as consistent as possible (Ref Messenger review).
| Action from last year | Maintain |
| Comments | The RO is a member of the Practitioner Performance Advice (PPA) Service Reference Group whose remit is to work with PPA to design services and develop and benchmark approaches to managing issues relating to medical professional standards. |
| Action for next year | RO to continue to input into PPA Service Reference Group and incorporate relevant learning into LYPFT ways of working. |
1E – Employment Checks
1E(i) A system is in place to ensure the appropriate pre-employment background checks are undertaken to confirm all doctors, including locum and short-term doctors, have qualifications and are suitably skilled and knowledgeable to undertake their professional duties.
| Action from last year | To work with colleagues in Recruitment to ensure Trust readiness for implementation of the NHS Digital Staff Passport (NHS DSP) for doctors joining the organisation (current expected go live date Q2 2025) |
| Comments | The recruitment manager has continued to be actively involved in discussions re the NHS Digital Staff Passport. It has been agreed that LYPFT will wait until the beta phase is complete before implementing it and remains committed to the long-term plan for all NHS staff groups to be able to use Digital Staff Passport.
Annual audit confirmed that there was 100% compliance with all domains with respect to necessary pre-employment checks for agency locums employed 2024/25 and 100% compliance with 6 of 8 domains for substantive medical staff, with 80% compliance in the other domains in 2024/25. |
| Action for next year | To continue to undertake annual audits of pre-employment background checks for doctors. |
1F – Organisational Culture
1F(i) A system is in place to ensure that professional standards activities support an appropriate organisational culture, generating an environment in which excellence in clinical care will flourish, and be continually enhanced.
| Action from last year | Maintain |
| Comments | The Trust’s ‘People Plan 2024-2027’ outlines the Trust’s ambitions for its staff to enable them to provide high-quality healthcare services. These ambitions are i) looking after our people ii) belonging in the NHS iii) new ways of working and delivering care and iv) growing for the future, and are accompanied by a Road map which sets out key actions and milestones. |
| Action for next year | To work with colleagues in the Trust to implement the ambitions of the ‘People Plan’. |
1F(ii) A system is in place to ensure compassion, fairness, respect, diversity and inclusivity are proactively promoted within the organisation at all levels.
| Action from last year | To build on relationships between the Responsible Officer and the Trust’s Freedom to Speak Up Guardian and Medical Workforce Race Equality Standards lead and explore opportunities for future collaborative projects. |
| Comments | The Trust’s Freedom to Speak Up Guardian and Medical Workforce Race Equality Standards leads have both attended the Good Medical Practice Assurance Group to ensure shared understanding of roles and responsibilities and adherence to Trust values.
Mandatory training for all doctors includes the requirement to undertake regular diversity and inclusion training. Compliance with this is monitored. |
| Action for next year | Maintain |
1F(iii) A system is in place to ensure that the values and behaviours around openness, transparency, freedom to speak up (including safeguarding of whistleblowers) and a learning culture exist and are continually enhanced within the organisation at all levels.
| Action from last year | To reflect on and implement actions following review of medical leadership within the organisation. |
| Comments | Work reviewing medical leadership reflected on as main agenda item during the 2024 Medical Leadership Day attended by consultants and SAS doctors from the Trust. |
| Action for next year | To continue to pursue opportunities for doctors to contribute to work within the organisation to embody the Trust values. |
1F(iv) Mechanisms exist that support feedback about the organisation’ professional standards processes by its connected doctors (including the existence of a formal complaints procedure).
| Action from last year | To continue to review the outputs of medical exit interviews and develop action plans to address any areas of concern. |
| Comments | Exit interviews have continued to be conducted as standard with doctors who leave the organisation and the results collated. To date no consistent themes have been highlighted.
The RO and Head of Medical Development and Operations have been working closely with colleagues in the complaints team to develop a more robust process for the investigation of complaints about doctors and ensure that those doctors receive appropriate support through the process. This information is recorded for consideration by the Good Medical Practice Assurance Group to enable triangulation with other data pertaining to doctor’s professional standards. |
| Action for next year | To continue to work with colleagues in the complaints team to ensure complaints about doctors are managed fairly and appropriately. |
1F(v) Our organisation assesses the level of parity between doctors involved in concerns and disciplinary processes in terms of country of primary medical qualification and protected characteristics as defined by the Equality Act.
| Action from last year | Annual Equality Impact Assessment (EIA) of concerns and disciplinary processes regarding doctors to continue to be undertaken in conjunction with the MWRES lead. |
| Comments | Results from 2024/25 EIA discussed at Good Medical Practice Assurance group.
It revealed 63% of doctors involved in disciplinary processes obtained their primary medical qualification (PMQ) outside the UK. A ‘Fair Experience For All’ checklist was completed for all investigated cases and revealed no evidence that PMQ or any other protected characteristics had contributed to the concerns or the outcome for the doctor following the investigation. |
| Action for next year | To continue to undertake an annual Equality Impact Assessment (EIA) in conjunction with the MWRES lead and reflect on the findings. |
1G – Calibration and networking
1G(i) The designated body takes steps to ensure its professional standards processes are consistent with other organisations through means such as, but not restricted to, attending network meetings, engaging with higher-level responsible officer quality review processes, engaging with peer review programmes.
| Action from last year | Next peer review due 2027 unless a sooner date is felt necessary. |
| Comments | The RO, Director and Associate Directors of Medical Professional Standards and the Head of Medical Development and Operations continue to regularly attend regional and mental-health-specific network meetings. |
| Action for next year | RO to take on the role of chair of the regional network meetings and develop a programme of education and development for group members. |
Section 2 – metrics
Year covered by this report and statement: 1 April 2024 – 31 March 2025.
.
All data points are in reference to this period unless stated otherwise.
2A General
The number of doctors with a prescribed connection to the designated body on the last day of the year under review. This figure provides the denominator for the subsequent data points in this report.
| Total number of doctors with a prescribed connection on 31 March | 139 |
2B – Appraisal
The numbers of appraisals undertaken, not undertaken and the total number of agreed exceptions is as recorded in the table below.
| Total number of appraisals completed | 138 |
| Total number of appraisals approved missed | 1 |
| Total number of unapproved missed | 0 |
2C – Recommendations
Number of recommendations and deferrals in the reporting period.
| Total number of recommendations made | 26 |
| Total number of late recommendations | 0 |
| Total number of positive recommendations | 24 |
| Total number of deferrals made | 2 |
| Total number of non-engagement referrals | 0 |
| Total number of doctors who did not revalidate | 0 |
2D – Governance
| Total number of trained case investigators | 27 |
| Total number of trained case managers | 4 |
| Total number of new concerns registered | 4 |
| Total number of concerns processes completed | 4 |
| Longest duration of concerns process of those open on 31 March | 67 days |
| Median duration of concerns processes closed | 91 days |
| Total number of doctors excluded/suspended | 0 |
| Total number of doctors referred to GMC | 0 |
2E – Employment checks
Number of new doctors employed by the organisation and the number whose employment checks are completed before commencement of employment.
| Total number of new doctors joining the organisation | 21 |
| Number of new employment checks completed before commencement of employment | 21 |
2F Organisational culture
| Total number of claims made to employment tribunals by doctors | 0 |
| Number of these claims upheld | N/A |
| Total number of appeals against the designated body’s professional standards processes made by doctors | 0 |
| Number of these appeals upheld | N/A |
Section 3 – Summary and overall commentary
This comments box can be used to provide detail on the headings listed and/or any other detail not included elsewhere in this report.
General review of actions since last Board report
21 of the 22 actions identified in the 2023/24 report have been completed and LYPFT remains compliant with the Medical Profession (Responsible Officers) (Amendment) Regulations 2023.
Actions still outstanding
To complete evaluation of the role of the Cultural Inclusion Ambassadors in the Responding to Concerns Advisory Groups and develop an action plan depending on findings.
Current issues
Nil.
Actions for next year (replicate list of ‘Actions for next year’ identified in Section 1):
-
- To gain approval for, and implement, changes and enhancements to the team structure within the Medical Directorate to ensure sufficient capacity for the Responsible Officer to carry out the responsibilities of the role.
- To disseminate and embed into practice the updated Trust’s Medical Appraisal procedure once ratified.
- To review the impact and outputs of the new Medical In-Post Review Framework
- To continue to oversee the provision of a Casenote audit, review the results and develop action plans as appropriate.
- To embed a process within the Medical Directorate to access DATIX and provide doctors with meaningful data for their supporting information.
- To disseminate and embed into practice the updated Trust’s Medical Appraisal procedure once ratified.
- To continue to review and develop appraiser teaching and training materials to ensure this is relevant to local and national standards.
- To continue to monitor the number of medical appraisers and complete further rounds of recruitment as required.
- To continue to obtain feedback through ADFs, and annual Appraiser Assurance reviews to inform topics for future ADFs and training.
- To encourage appraiser participation at regional network events
- RO to take on the role of chair of the regional Mental Health network and develop a programme of education and development for group members.
- To embed the process of quality-assuring Medical Education-related work undertaken by doctors and include this in the supporting information for discussion and reflection at appraisal.
- To deliver and evaluate Case Investigator Training
- To continue to work with the Medical Workforce Race Equality Standard (MWRES) lead to ensure the Trust responds fairly and appropriately when concerns are raised about doctors.
- To undertake an annual Equality Impact Assessment (EIA) in conjunction with the MWRES lead to review compliance against MWRES indicators regarding investigations into concerns regarding doctors.
- To complete evaluation of the role of the Cultural Inclusion Ambassadors in the Responding to Concerns Advisory Groups and develop an action plan depending on findings.
- To continue to undertake annual audits of pre-employment background checks for doctors
- RO to continue to input into PPA Service Reference Group and incorporate relevant learning into LYPFT ways of working
- To work with colleagues in the Trust to implement the ambitions of the ‘People Plan’.
- To continue to pursue opportunities for doctors to contribute to work within the organisation to embody the Trust values
- To continue to work with colleagues in the complaints team to ensure complaints about doctors are managed fairly and appropriately.
- To continue to undertake an annual Equality Impact Assessment (EIA) in conjunction with the MWRES lead and reflect on the findings.
- To work with colleagues in the Trust to implement the ambitions of the ‘People Plan’.
- To continue to pursue opportunities for doctors to contribute to work within the organisation to embody the Trust values
- To continue to work with colleagues in the complaints team to ensure complaints about doctors are managed fairly and appropriately.
- To continue to undertake an annual Equality Impact Assessment (EIA) in conjunction with the MWRES lead and reflect on the findings.
Overall concluding comments (consider setting these out in the context of the organisation’s achievements, challenges and aspirations for the coming year):
The annual increase in the numbers of doctors with a prescribed connection to LYPFT over the past 5 consecutive years is a positive example of the impact of recruitment and retention initiatives and should be welcomed. Likewise is the increase in the number of doctors working into LYPFT who have their prescribed connection elsewhere such as doctors who provide clinical sessions into LYPFT as part of a Service Level Agreement.
A stable medical workforce positively impacts on patient care and organisational outcomes by improving efficiency, reducing costs and enhancing quality of care. Overseeing the professional standards of these doctors however requires time and adequate resources and a mapping exercise has confirmed that there is risk that continued expansion of the medical workforce without proportionate investment in the supporting infrastructure risks the Trust becoming non-compliant with the statutory Medical Profession (Responsible Officers) (Amendment) Regulations 2023.
For those doctors with a prescribed connection to LYPFT there were no unapproved missed appraisals in 2024/25 and 100% of the recommendations for revalidation made to the GMC were positive and submitted on time. For those doctors working into LYPFT who have their prescribed connection elsewhere a new system of Medical In-Post Reviews will be introduced in Q1 2025/26 to provide assurance to LYPFT of the doctor’s ongoing fitness to undertake the role and assurance to the doctor’s RO at the time of their annual medical appraisal of the scope of their work in LYPFT in accordance with NHSE recommendations.
When concerns are raised about a doctor these will continue to be managed in accordance with the Trust’s policy (updated 2024) and, following a further round of training to be delivered in conjunction with NHSE in Q1 2025/26, all medical line managers will have received training in conducting investigations into a doctor’s practice. The presence of Cultural Inclusion Ambassadors in Responding to Concerns Advisory Groups, something which is unique to LYPFT, is currently being evaluated and the results should be available by Q2 2025/26. Also planned for 2025/26 are continued improvements to the way that complaints about doctors are allocated, investigated and overseen and that doctors are provided with appropriate support during this process.
External to LYPFT the RO and members of the Medical Directorate team will continue in 2025/26 to be actively involved in regional and national networks and reference groups, pursuing opportunities for shared learning and development for the benefit of all.
Section 4 – Statement of Compliance
The Board/executive management team have reviewed the content of this report and can confirm the organisation is compliant with The Medical Profession (Responsible Officers) Regulations 2010 (as amended in 2013).
Signed on behalf of the designated body
[(Chief executive or chairman (or executive if no board exists)]
- Official name of the designated body: Leeds and York Partnership NHS Foundation Trust
- Name: Merran McRae
- Role: Chair
- Signed:
- Date:
Cover sheet for Chief Executive’s report – Leeds Provider Partnership Review
- Paper title: Chief Executive’s report – Leeds Provider Partnership Review
- Date of meeting: 31 July 2025
- Presented by: Dr Sara Munro, Chief Executive Officer
- Prepared by: Dr Sara Munro, Chief Executive Officer
This paper supports the Trust’s strategic objective/s (SO):
- SO1 – We deliver great care that is high quality and improves lives.
- SO2 – We provide a rewarding and supportive place to work.
- SO3 – We use our resources to deliver effective and sustainable services.
This paper relates to the Trust’s strategic risks (SR):
- SR1 – Quality including safety assurance processes
- SR2 – Delivery of the Quality Strategic Plan
- SR3 – Culture and environment for the wellbeing of staff
- SR4 – Financial sustainability
- SR5 – Adequate working and care environments
- SR6 – Digital technologies
- SR7 – Plan and deliver services that meet the health needs of the population we serve.
Executive summary
The purpose of this paper is to share with board the specification for the Leeds Provider Partnership Review.
Recommendation
The Board is asked to note the content of the report and specification.
Chief Executive’s report – Leeds Provider Partnership Review
The purpose of this report is to update and inform the Board of key activities and issues from the Chief Executive.
1. Our services and our people
Trust Priorities
All the Executive Director appraisals have now been completed and the Trust priorities reflected in annual objectives for the coming year.
The roadshow of Executive led presentations to teams and departments across the Trust concludes at the end of July. Feedback has been very positive from all involved and we have decided to run similar sessions later in the year to be able to share progress and update teams on what is happening in and around the Trust that is of relevance.
I wanted to take the opportunity to highlight the significant progress made in our procurement team – Led by Nicky Woodhead. I had the pleasure of visiting them as part of the executive presentation and was given a tour and update on the improvement work Nicky and the team had led over the past 12 months. The impact is now very noticeable in improved responsiveness and performance of the department.
Thrive and Shine
Our creative staff engagement and well-being team are well underway with the Thrive and Shine roadshows which are taking place over the summer period. The road shows have been developed based on some of the feedback from the last staff survey and they have several aims:
- celebrate staff contributions with fun, engaging activities.
- Focus on wellbeing through interactive stalls, gratitude walls, and practical support.
- Runs July–September, visiting key sites and offering virtual stops for remote staff.
- Activities include prize draws, wellbeing resources, inspiring stories, and a chance to share feedback.
NHSE Chair Penny Dash visit to Leeds and Becklin
The chair of NHSE Penny Dash visited Leeds on the 8th of July 2025. Following a tour at Leeds General Infirmary a small group of representatives from health and care in the city joined Penny for lunch to discuss the 10-year plan and the work underway in the city. Following this we were delighted to host Penny at the Becklin Centre – she visited Ward 1, spoke with ward staff and the senior leadership Team.
Industrial Action
At the time of writing this paper we are preparing for Resident doctors taking strike action from 7am Friday 25 July to 7am Wednesday 30 July, unless a pay deal is reached. 90% of BMA members voted in favour of taking industrial action on a 55% turnout. The mandate lasts until January 2026, and the dispute is with the government on pay and conditions. The Trust has reconvened its Industrial Action Strategic Coordination Group to safeguard patient safety and minimise disruption and NHSE have issued explicit guidance on the approach to be taken to determine services that should be maintained and are therefore classed as exempt from action. Further updates will be provided at the Board meeting.
2. Leeds System Update
The Leeds Provider Partnership Review is now underway following the launch event held after the last board meeting on the 30th of May at St Georges Church Leeds. The event was very well attended from partners across the city including colleagues from the Trust. The review has been commissioned by NHS providers, Leeds City Council, and the ICB. The first phase has focused on reviewing key documentation, including organizational strategies and interviews with a range of stakeholders including the biggest meeting of primary care practices at the annual GP assembly.
The outputs from this first phase will be discussed with the CEOs and the operational steering group to then agree to the next area of focus. Now the 10-year plan for health has been published this will be explicitly considered in the blueprint we want to create for the city and what the roadmap should look like to achieve this – including a view on organizational readiness and risks and issues that will need to be addressed. We have also asked that learning from work underway in other systems is included. The aim is still to have a draft report in September.
Professor Pil Wood – CEO at Leeds Teaching Hospitals NHS Trust has just announced his intention to retire at the end of this year. Phil will remain committed to the Leeds Provider Partnership development during this time, and this will be one of the priority areas of work for his future successor.
3. Regional and national updates
The most notable update since our last board is the publication of the 10-year plan for health, coinciding with the NHS 77th Birthday. The board has been sent links to the plan separately and the public facing presentation from DHSC shared with the council of governors.
The plan sets out a future model of provision which has shifted significantly in the use of AI and technology to enable care delivery, service delivery, support staff etc.
Some key updates to note;
- Further guidance on the implementation of the 10-year plan is being developed over the summer.
- The foundation trust model will be relaunched, and mature systems will be able to develop as an integrated health organisation where population budgets are collectively managed.
- Move to medium term financial planning and capital planning is welcomed.
- Anticipate further changes to the funding and payment mechanisms for providers.
- The development of a blueprint for NHSE regional teams has still not been published.
- The timescale for changes to ICBs is still to be confirmed.
- The progress of the new MHA to receive royal assent is expected to now take place in the autumn.
- A new workforce strategy is expected in the autumn.
- Development of modern service frameworks will begin later in the year to set out more detailed strategy on service areas including mental health.
NHS CEOs were asked to volunteer to help with the development of detailed implementation guidance over the next few months and the following work streams are being established:
- Neighbourhood health
- NHS App and single patient record
- Oversight model, foundation trust and model integrated health organisation
- Financial foundations and medium-term planning
- Quality
- Workforce
Having volunteered for several of these I have now been asked to join the workforce workstream.
The second phase of the review by Penny Dash into the quality and safety regulatory landscape for health and care was also published in July. Key headlines include abolition of Health Watch and the National Guardians office. The FTSUG role will however remain at provider level. Consolidation of different safety regulatory functions is recommended e.g. HSSIB to be incorporated into CQC. There will be a relaunch of the national quality board and publication of a new national quality strategy for the NHS.
National Oversight Framework (NOF)
NHSE consulted on the development of a new NOF for providers and ICBs earlier this year. It is also being referred to as the Provider assessment framework/score (PAF/PAS). The consultation has concluded, and all NHS providers will be assessed under the new framework and scored in segments from 1-4. The level a Trust is in determines the level of oversight/intervention that will be provided by NHSE regional teams. One is the highest/best segment – 4 is the lowest.
For Trusts in segment 4 should they be deemed not to have capacity to improve they can be placed in a new segment of 5. Trusts currently in special measures will be placed in segment 5. Any Trust in receipt of deficit support financially cannot be higher than segment 3.
NHSE is compiling these new segments, and this will be discussed further at finance and performance committee and in the private board. We were expecting the outcomes to be made public this month but have been advised this has been deferred until later in the summer.
4. Reasons to be proud
Baton of Hope tour will highlight suicide prevention in Leeds
 The Baton of Hope will come to visit Leeds on 10 September – World Suicide Prevent Day – as part of a special UK-wide tour promoting suicide prevention.
The Baton of Hope will come to visit Leeds on 10 September – World Suicide Prevent Day – as part of a special UK-wide tour promoting suicide prevention.- People affected by suicide will carry the Baton on a relay route through Leeds.
- Planning an event at the Becklin Centre to mark the occasion – we hope the event will include food, drinks, and art.
- Contribute to the Tree of Hope: Write a message of hope to be included in a collaborative art installation at the Becklin Centre.
Shine and Thrive summer roadshow in York
 A fantastic start to our summer roadshow at our sites in York as Sarah, Tracey, Amy, Victoria and Judith head out on the road.
A fantastic start to our summer roadshow at our sites in York as Sarah, Tracey, Amy, Victoria and Judith head out on the road.- Staff from Clifton House and Mill Lodge had fun in the “sun”. Playing games, adding to the gratitude wall and taking time for their own wellbeing.
Positive Practice in Mental Health Awards 2025

- The Pathway Development Service were highly commended in the Complex Needs category for their innovative video triage and consultation initiative.
- Principal Clinical Psychologist Laura Eggleton described it as “a fantastic acknowledgment given there were over 500 nominations across the awards.”
Trust’s first Supported Interns
 Congratulations to Danny, Antonio and Preston who have now reached the end of their programmes.
Congratulations to Danny, Antonio and Preston who have now reached the end of their programmes.- Thank you to Estates, LD Admin, Red Kite View admin and NDS Admin team for supporting young people with special educational needs to gain experience of the workplace and enhance their employability.
- Danny and Antonio will stay with LYPFT as a volunteer, and apprentice Maintenance Technician respectively. Preston has secured an admin role at LTHT.
- We will be welcoming 3 new interns to the Trust in October 2025.
Nia Trafford, Senior Healthcare Support Worker, Skylark Ward – Red Kite View
 Nia was the winner of two awards ‘Innovative Practice’ and ‘Calm in a Crisis’ the team feel Nia deserves further recognition at a Trust level not just internally at RKV. The quotes are from Nia’s colleagues at Red Kite View from this year’s Red Kite Awards:
Nia was the winner of two awards ‘Innovative Practice’ and ‘Calm in a Crisis’ the team feel Nia deserves further recognition at a Trust level not just internally at RKV. The quotes are from Nia’s colleagues at Red Kite View from this year’s Red Kite Awards:
“Nia always treats every young person as an individual and develops really creative and flexible approaches to working with them and developing positive therapeutic relationships. They have been integral in embedding AMBIT values and practices onto Skylark.”
“Nia always looks at things from a fresh perspective and reminds us of what may be going on for the Young People.”
“Very calm, well organised, very experienced and shows such patience while on shift. They are amazing!”
July’s Research Hero – Dr Mutza
 We are delighted to acknowledge Dr. Mo Murtza as Research Hero of the Month for July 2025. His exceptional dedication in identifying participants for the DIAMONDS study and collaborating with IT to search for diabetes cases has been invaluable. As Co-Principal Investigator, Mo addressed risk and safety concerns and stepped in as a ‘blind rater’ when needed. His efforts to make research inclusive, such as assisting a participant in Urdu, are truly commendable. Although moving to a different trust, Mo will continue his research with us on a new commercial trial this autumn. We are incredibly grateful for his contributions and look forward to his continued impact.
We are delighted to acknowledge Dr. Mo Murtza as Research Hero of the Month for July 2025. His exceptional dedication in identifying participants for the DIAMONDS study and collaborating with IT to search for diabetes cases has been invaluable. As Co-Principal Investigator, Mo addressed risk and safety concerns and stepped in as a ‘blind rater’ when needed. His efforts to make research inclusive, such as assisting a participant in Urdu, are truly commendable. Although moving to a different trust, Mo will continue his research with us on a new commercial trial this autumn. We are incredibly grateful for his contributions and look forward to his continued impact.
Mo says “Research excites me because it gives clinicians a voice in shaping the future of our patient’s care. Working with the R&D team on the DIAMONDS trial reminded me how vital evidence-based practice is in shaping better outcomes for our patients. I felt proud to contribute alongside such a dedicated and forward-thinking team!”
Dr Sara Munro
Chief Executive Officer
24 July 2025
Cover sheet for Chief Financial Officer (CFO) Finance Report
- Paper title: CFO Finance Report
- Date of meeting: 31 July 2025
- Presented by: Dawn Hanwell, Chief Financial Officer and Deputy Chief Executive
- Prepared by: Jonathan Saxton, Deputy Director of Finance
This paper supports the Trust’s strategic objective/s (SO):
- SO3 – We use our resources to deliver effective and sustainable services.
This paper relates to the Trust’s strategic risks (SR):
- SR4 – Financial sustainability
Executive summary
The Trust is on plan in month 3 but only due to one off non-recurrent means, this demonstrates the importance of the expedient delivering of the efficiency programme. The capital plan is currently behind plan budget expected to achieve plan by the year end.
Due to the system submitting a plan with a £33.2m improvement target, the Trust have agreed to target a £0.9m non recurrent surplus stretch against the break-even plan, this will be documented in future returns to NHSE.
NHS England has developed an updated Assessment Framework which will replace the current Oversight Framework. Formal publications of segmentation is scheduled for August for quarter 1. At this stage we have no concerns on the finance domain.
Do the recommendations in this paper have any impact upon the requirements of the protected groups identified by the Equality Act? No
Recommendation
The Board is asked to:
- Note the Trust revenue and capital positions for 2025/26.
- Note the system position, the devolvement of the £33.2m Improvement and implication for the Trust.
- Note the new National Oversight Framework metrics for 2025/26.
CFO Finance Report
1 – Introduction
This report provides an overview of the financial position at the end of month 3, 2025/26 financial year. It also includes some other relevant updates and information.
2 – Income and Expenditure Performance 2025/26
The overall summary reported position to NHSE against the Trust plan is shown in table below. This reflects a position broadly on plan overall (surplus of only £10k).
Income and expenditure plan position for month 3
| Category | Plan Annual (£’000) | Plan YTD (£’000) | Actual YTD (£’000) | Variance YTD (£’000) |
| Patient Care Income | 235,819 | 59,854 | 59,947 | 93 |
| Other Income | 37,634 | 8,709 | 8,889 | 180 |
| Total Income | 273,453 | 68,563 | 68,836 | 272 |
| Pay Expenditure | (200,366) | (50,369) | (49,469) | 899 |
| Non Pay Expenditure | (68,406) | (16,811) | (18,054) | (1,243) |
| Total Expenditure | (268,772) | (67,180) | (67,523) | (344) |
| Surplus / Deficit | 4,681 | 1,384 | 1,312 | (72) |
| Adjustments for NHSE Reporting | (4,681) | (1,384) | (1,302) | 82 |
| Adjusted Position | 0 | 0 | 10 | 10 |
The key items of note overall in the position are:
- Bank expenditure remains at an average of £1.5m per month and is £398k above plan year to date. This is largely driven by increased evening and weekend usage of bank working.
- Agency expenditure has reduced in year and is £607k under plan year to date. The majority (89%) of agency is related to medical staff.
- Substantive pay expenditure is also £669k under plan, largely attributable to management of recruitment , linked to assessing recurrent cost savings.
- Against the in year trajectory Out of area placement (OAP) spend is £800k cumulatively overspend year to date. This is concerning given the reducing trajectory for the year.
- Overall corporate departments, doctors in training and pharmacy have broadly started the year along the same pattern as they exited the prior year, with significant vacancies and underspend.
- Non-recurrent benefits such as technical flexibilities, interest Receivable above plan and the delay in recruiting to the additional Perinatal ward are supporting the position, this is in the region of £2.3m.
3 – Efficiency Programme
3.1 – Run Rate efficiency
The efficiency programme target is to deliver in year run-rate savings of £18.5m. This is based on our system plan, which reflects run rate movements year on year (not recurrent internal budget).
The workstreams that will deliver the required run-rate reduction will have oversight through the workforce and agency project board, the inpatient flow programme and the procurement steering group, with assurance though the Finance and Planning Group (FPG) to the Executive team, providing the enhanced rigour and oversight.
The table below is the M3 progress of the run-rate reductions.
| Programme / Scheme Name | Apr Plan | May Plan | Jun Plan | YTD Plan | Apr Actual | May Actual | Jun Actual | YTD Actual | YTD Variance |
| Inpatient Flow | 170 | 236 | 297 | 703 | (100) | (65) | 53 | (112) | (815) |
| Reduce external room hire | 0 | 0 | 0 | 0 | 10 | 25 | 2 | 37 | 37 |
| Reduce our warehousing provision | 0 | 0 | 0 | 0 | 0 | 0 | 17 | 17 | 17 |
| Reducing use of taxi’s | 0 | 0 | 0 | 0 | 4 | 3 | 0 | 7 | 7 |
| CPC additional £500k | 42 | 42 | 42 | 126 | 42 | 41 | 42 | 125 | (1) |
| Interest Receivable | 313 | 313 | 313 | 939 | 447 | 431 | 416 | 1,294 | 355 |
| Unidentified efficiency target | 250 | 250 | 250 | 750 | 0 | 0 | 0 | 0 | (750) |
| Overtime Reduction | 0 | 0 | 0 | 0 | 23 | 39 | 45 | 107 | 107 |
| Reducing Agency Spend | 33 | 67 | 100 | 200 | 225 | 225 | 353 | 803 | 603 |
| Reduce Bank Expenditure | 20 | 40 | 60 | 120 | (280) | 28 | (30) | (282) | (402) |
| Technical Flex | 297 | 255 | 232 | 784 | 682 | 335 | 180 | 1,197 | 413 |
| Non-Pay Savings / Procurement | 83 | 83 | 83 | 249 | 0 | 0 | 0 | 0 | (249) |
| Wagestream | 0 | 0 | 0 | 0 | 2 | 2 | 2 | 5 | 5 |
| Total | 1,208 | 1,286 | 1,377 | 3,871 | 1,055 | 1,064 | 1,079 | 3,198 | (673) |
As shown above at M3 the Trust is £673k behind plan, year to date. The inpatient flow programme is currently £815k behind plan due to increased OAPs activity in April and May. The unidentified efficiency target remains behind plan, however will be offset by new schemes identified during year, or further slippage and flexibility non recurrently. The agency reduction and Interest receivable schemes are currently £603k and £355k better than planned respectively. Technical flex is also ahead of plan by £413k. Actions are being taken to recover this position later in the year.
3.2 – Budget efficiency
The Trust’s recurrent internal budgets identified a recurrent £14.5m budget saving programme (recurrent CIP). This is based on allocated budgets not run rate profiles. It is a target figure to balance budgets. assuming every service and department is operating from their opening base budget position, not what is being spent (run rate).
| Div/Dept | Target (£000) | Schemes Agreed (£000) | Remaining (£000) |
| CFO | 2,000 | 1,664 | (336) |
| POD | 650 | 62 | (588) |
| Nursing | 600 | 367 | (233) |
| Care Services | 9,009 | 3,571 | (5,438) |
| Medical | 850 | 136 | (714) |
| CEO | 200 | 133 | (67) |
| COO | 50 | 50 | 0 |
| Reserves | 450 | 1,310 | 860 |
| SSL Contract | 691 | 341 | (350) |
| Total | 14,500 | 7,634 | (6,516) |
In May indicative targets were given to services and departments with the expectation that they begin to design structures/services that are recurrently affordable within the overall budget.
In July £7.6m of recurrent budget CIP schemes were presented to the Extended Executive Management Team (EEMT) and deemed to be either low or medium risk. These schemes will be put forward to the Quality Impact Assessment (QIA) meeting scheduled for August for approval. Executives have been asked to identify further schemes to close the gap or explain what the impact would be to achieve the full CIP by department/division, so that the EEMT can agree next steps.
4 – Trust Capital Plan 2025/26
4.1 – Capital Planning
The capital planning process for 2025/26 has increased in complexity with the addition of specific purpose allocations such as for constitutional standards and critical backlog maintenance, at system level. In addition, these specific allocations are essentially Public Dividend Capital (PDC) as cash will be provided to organisations who are provided with these allocations. These specific purpose allocations have been allocated to systems to determine prioritisation as well as the core capital cover allocation for 2025-26.
We anticipate changes to these allocations are likely in year and have recently been notified that the Trust will receive £823k of PDC for the roof scheme at St Mary’s House, however, this is not additive and a reduction in our operational envelope for 2025-26 will offset this. The Trust will therefore have a cash benefit in this instance.
4.2 – Capital Expenditure
The capital position is detailed in Appendix A. Cumulative year to date capital expenditure is £2.0m at M3 against a plan of £3.6m. The YTD plan includes £2.5m of PDC capital expenditure for Parkside Lodge (actual £618k at M3), which is now forecast later this financial year. Expenditure includes network infrastructure £0.24m phased later in year in the plan.
Providers plan for capital expenditure at 105% of capital allocations, with an acknowledgement that they must operate within the allocation (100%) in year. In order to facilitate this, LYPFT’s 2025/26 capital plan includes £2m (phased later in year) on behalf of all providers within the ICS.
5 – Underlying Position
At month 3 we have submitted a re-assessment of the Trust underlying position to NHSE. This will form part of the Trust and system medium term planning that will be developed over the next few months. As with planning, the underlying run-rate or planned position is different to the Trust internal budget underlying position, as shown below. As NHSE hold Trusts to account for their run-rate, the planned position was submitted to NHSE. At this stage have estimated that the underlying position is £9.9m.
6 – System Financial Position
6.1 – System M3 Revenue Position
The month 3 year-to-date position for the ICS was an actual £23.7m deficit against a planned £19.7m deficit; a shortfall/adverse variance against plan of £4.0m. The full-year plan for the ICS is a break-even plan after receipt of £49.2m deficit support funding. Reported forecasts (to NHSE) for all ten NHS provider organisations and ICB remain at planned levels, break-even.
6.2 – The £33.2m System Improvement Target
As previously noted, for the system to submit an overall balanced plan, the ICB submitted a plan with a £33.2m system improvement target within it, with the agreement that in year this target would be split between organisations. The Leeds Place took a £5.2m share of this target and it has been agreed that LYPFT’s share of this is £0.9m. This means that the trust will have a target to achieve a £0.9m surplus in 25/26 against our break-even plan.
6.3 – The System M3 Capital Position
Year to date there is a £16m underspend against the system operational and IFRS16 capital plans and a £11.4m underspend against the National Capital plans. It is expected that all capital plans are delivered by the end of the financial year.
7 – The NHS National Oversight Framework for 2025/26
As noted in the May committee paper, there is a new Oversight Framework for 25/26.The domains and metrics that are being used to calculate Trust and organisations scores have now been released.
The Finance and Productivity domain with metrics that are relevant for Mental Health Providers is shown below:
| Domain | Metric |
| 5. Finance and Productivity | • Planned surplus/deficit, • Variance year-to-date vs. financial plan, • Relative difference in costs (specific productivity measure for MH) |
In the Quarter 1 segment scores are based on only 2 of the 3 metrics, Variance year to date has not been used at this stage, but it is expected to be used at quarter 2.
It should be noted that the degree of emphasis on financial balance is such that any reported deficit will generate an automatic override which will place an organisation on segment 3, irrespective of performance in other domains.
8 – Conclusion
The Trust is on plan in month 3 but only due to one off non-recurrent means, this demonstrates the importance of the expedient delivering of the efficiency programme. The capital plan is currently behind plan budget expected to achieve plan by the year end.
Due to the system submitting a plan with a £33.2m improvement target, the Trust have agreed to target a £0.9m non recurrent surplus stretch against the break-even plan, this will be documented in future returns to NHSE.
NHS England has developed an updated Assessment Framework which will replace the current Oversight Framework. Formal publications of segmentation is scheduled for August for quarter 1. At this stage we have no concerns on the finance domain.
9 – Recommendation
The Board is asked to:
- Note the Trust revenue and capital positions for 2025/26.
- Note the system position, the devolvement of the £33.2m Improvement and implication for the Trust
- Note the new National Oversight Framework metrics for 2025/26
Jonathan Saxton
Deputy Director of Finance
24 July 2025
Appendix A – Capital Plan
Capital Programme – at 30 June 2025 – Year to date
ICS Operational Capital
Estates Operational
| Category / Project | Annual Plan (£’000) | YTD Plan (£’000) | Actual Spend (£’000) | YTD Variance (£’000) |
| Health and Safety / Fire / Accessibility / Backlog | 750 | 0 | 68 | (68) |
| Security Review | 150 | 0 | 3 | (3) |
| Sub-Total | 900 | 0 | 72 | (72) |
IT/Telecoms Operational
| Category / Project | Annual Plan (£’000) | YTD Plan (£’000) | Actual Spend (£’000) | YTD Variance (£’000) |
| IT Network Infrastructure | 250 | 0 | (240) | (240) |
| Server/Storage | 30 | 0 | None. | (0) |
| PC Replacement EUL | 360 | 0 | 8 | (8) |
| Cyber Security | 170 | 0 | None. | (0) |
| Sub-Total | 810 | 0 | 248 | (248) |
Estates Strategic Developments
| Category / Project | Annual Plan (£’000) | YTD Plan (£’000) | Actual Spend (£’000) | YTD Variance (£’000) |
| Lifecycle Contribution | 100 | 0 | 36 | (36) |
| St Mary’s House, North/South Wing/ Estate Strategy | 375 | 0 | None. | 0 |
| Aire Court | 350 | 0 | None. | 0 |
| Sustainability and Green Plan | 250 | 0 | 68 | (68) |
| Completion of Minor Schemes | 228 | 40 | 94 | (54) |
| Woodlands Generator | 50 | 0 | None. | 0 |
| Water Main Upgrade [Lead] SMH/SMHosp | 115 | 0 | None. | 0 |
| The Mount Perinatal | 5,000 | 1,000 | 894 | 106 |
| Acoustics – Improvement | 150 | 0 | None. | 0 |
| Security-Critical System Replacement | 300 | 0 | None. | 0 |
| Sub-Total | 6,918 | 1,040 | 1,093 | (53) |
IT Strategic Developments
| Category / Project | Annual Plan (£’000) | YTD Plan (£’000) | Actual Spend (£’000) | YTD Variance (£’000) |
| Data Centre and Adjustments [ICB] | 2,036 | 0 | None. | 0 |
| Sub-Total | 2,036 | 0 | 0 | 0 |
Disposals
| Category / Project | Annual Plan (£’000) | YTD Plan (£’000) | Actual Spend (£’000) | YTD Variance (£’000) |
| ICS | 0 | 0 | (8) | (8) |
| Sub-Total | 0 | 0 | (8) | (8) |
Total ICS Operational Capital
| Category / Project | Annual Plan (£’000) | YTD Plan (£’000) | Actual Spend (£’000) | YTD Variance (£’000) |
| Total ICS Operational Capital | 10,664 | 1,040 | 1,404 | (364) |
PDC Funded Schemes
| Category / Project | Annual Plan (£’000) | YTD Plan (£’000) | Actual Spend (£’000) | YTD Variance (£’000) |
| EPR Developments | 2,500 | 0 | None. | 0 |
| Complex Rehab | 5,600 | 2,500 | 618 | 1,882 |
| Total PDC Funded Schemes | 8,100 | 2,500 | 618 | 1,882 |
IFRS16 Leased Assets
| Category / Project | Annual Plan (£’000) | YTD Plan (£’000) | Actual Spend (£’000) | YTD Variance (£’000) |
| Leased Buildings | 0 | 0 | None. | 0 |
| Lease Cars | 150 | 30 | 16 | 14 |
| Sub-Total | 160 | 30 | 16 | 14 |
Disposals
| Category / Project | Annual Plan (£’000) | YTD Plan (£’000) | Actual Spend (£’000) | YTD Variance (£’000) |
| Leased | 0 | 0 | (4) | 4 |
| Sub-Total | 0 | 0 | (4) | 4 |
Total IFRS16 Leased Assets
| Category / Project | Annual Plan (£’000) | YTD Plan (£’000) | Actual Spend (£’000) | YTD Variance (£’000) |
| Total IFRS16 Leased Assets | 150 | 30 | 11 | 19 |
Total Capital Spend
| Category / Project | Annual Plan (£’000) | YTD Plan (£’000) | Actual Spend (£’000) | YTD Variance (£’000) |
| Total Capital Spend | 18,914 | 3,750 | 2,033 | 1,537 |
Cover sheet for 2025 – 2026 Organisational Priorities Quarter 1 Progress Report
- Paper title: 2025 – 2026 Organisational Priorities Quarter 1 Progress Report
- Date of meeting: 31 July 2025
- Presented by: Dawn Hanwell, Chief Financial Officer and Deputy Chief Executive
- Prepared by: Amanda Burgess, Head of the Programme Management Office
This paper supports the Trust’s strategic objective/s (SO):
- SO1 – We deliver great care that is high quality and improves lives.
- SO2 – We provide a rewarding and supportive place to work.
- SO3 – We use our resources to deliver effective and sustainable services.
This paper relates to the Trust’s strategic risks (SR):
- SR1 – Quality including safety assurance processes
- SR2 – Delivery of the Quality Strategic Plan
- SR3 – Culture and environment for the wellbeing of staff
- SR4 – Financial sustainability
- SR5 – Adequate working and care environments
- SR6 – Digital technologies
- SR7 – Plan and deliver services that meet the health needs of the population we serve.
Executive summary
This report provides a summary of the Trust’s progress against our 2025 – 2026 organisational priorities. This is the first report of 2025 – 2026 setting out how we are initiating our 14 priorities each with an identified lead executive. Our quarterly report is in place to demonstrate the progress made on each priority specifically, identify where a priority may require attention or further action to ensure its intended outcomes are achieved.
Each slide provides a summary of a priority and details how we are delivering against each of the high-level milestones. We have adopted the ‘alert, advise, assure’ approach to provide the key messages on whether the defined milestones are being met, alert where matters require escalation or give assurance that a priority is on track.
In total we have 105 high-level milestones for delivery. At the end of quarter one we have:
- 2 milestones are marked as ‘alert’
- 11 milestones are marked as ‘advise’
- 92 milestones are marked as ‘assure’
All our organisational priorities are governed through the executive-led portfolio specific governance groups to ensure monthly oversight and monitoring is achieved. Any escalations are reporting through to the monthly Extended Executive Management Team meetings.
Do the recommendations in this paper have any impact upon the requirements of the protected groups identified by the Equality Act? No
Recommendation
The Board of Directors is asked to:
- Consider our position against our 2025/26 organisational priorities at the end of quarter 1.
- Be assured as to the systems and processes in place for monitoring and supporting the delivery of each priorities high-level milestones and underpinning tasks.
2025 – 2026 Organisational Priorities Quarter 1 Progress Report
Overview and key messages
This is the first progress report for 2025 – 2026 and provides a summary of the Trust’s progress against our 14 organisational priorities.
The reporting format demonstrates at a high level how we are progressing against the key milestones for each priority. Using the ‘alert, advise, assure’ approach to provide clarity on where we might be going off track, what measures we are putting in place to ensure we deliver the priority and where we are making good progress.
We govern and have oversight of the progress we are making against our priorities through the monthly Extended Executive Management Team meetings. On a quarterly basis assurance is provided through the Finance & Performance Committee and Board of Directors meetings.
At the end of quarter 1 2025 – 2026 the following priorities are reporting as red (alert):
- People Plan metrics: this is our performance against the BAME staff entering a disciplinary process.
The following priorities are reporting as amber (advise):
- Efficiency and Productivity Programme: this is our performance against our budget and run-rate savings targets.
- Workforce efficiencies: this is our performance against the target for reducing bank expenditure by 10%.
- People Plan metrics: this is our performance against sickness absence, stress and anxiety, MSK and compliance with clinical supervision.
- Delivering an expanded perinatal inpatient service: although good progress has been made, we have not fully established a Co-Production Working Group.
- Clinical outcome measures: although significant progress has been made, we have not managed to deploy the new patient portal application as intended.
2025 – 2026 organisational priorities quarter 1 progress summary
| Priority Area | Lead | Exc Owner | Scheme status | Alert | Advise | Assure |
| Delivery of our Efficiency and Productivity Programme (total efficiency programme) | J. Saxton | D. Hanwell | Live | None | 2 | None |
| Delivery of our workforce efficiency programme | J. Saxton | D. Skinner | Live | None | 1 | 2 |
| Delivery of our Inpatient Quality Transformation Programme | L. McDonagh | J. Forster Adams | Live | None | None | 3 |
| Reducing mental health ED attendances and delays Project | E. Townsley | J. Forster Adams | Live | None | None | 4 |
| Delivering a Redesigned Community Mental Health Service Programme | R. Carroll | J. Forster Adams | Live | None | None | 2 |
| CYPMH Transformation Programme (inc redesign of Tier 3.5/4 models of care) | T. Richardson | J. Forster Adams | Live | None | None | 6 |
| Delivering an expanded perinatal inpatient service and provider collaborative | R. Mumby | C. Hosker | Live | None | 1 | 23 |
| Implementation of ReSPECT (Recommended Summary Plan for Emergency Care and Treatment) to replace the DNARCPR (Do Not Attempt Cardiopulmonary Resuscitation) document across the organisation | M.C. Trevett | C. Hosker | Live | None | None | 9 |
| Delivering Improving Health Equity strategic priorities | S. Valinakis | J. Forster Adams | Live | None | None | 3 |
| Create clinical outcome reporting systems enabling the implementation of outcome measures across all our care services | E. Joubert, I. Hogan | C. Hosker | Live | None | 3 | 5 |
| Development and implementation of Quality and Culture dashboards for revision in selective services | R. Wylde, A. McNichol | C. Hosker, D. Skinner | Live | None | None | 16 |
| Develop and agree our future FM model across our PFI sites | W. Duffy | D. Hanwell | Live | None | None | 4 |
| Conclude the EPR procurement process and develop/ratify the business case for the preferred EPR. In parallel explore and develop options for adding to the existing EPR platform. | I. Hogan | D. Hanwell | Live | None | None | 2 |
| Delivery of key People Plan priority metrics | H. Tetley, A. McNichol | D. Skinner | Live | 2 | 4 | 13 |
Delivery of our Efficiency and Productivity Programme
Our performance at the end of quarter 1
| Savings Type | Annual Target | YTD Target | YTD Actual | Status |
| Budget | £14,500,000 | £3,625,000 | £0 | Advise |
| Run Rate | £18,500,000 | £3,871,000 | £3,278,125 | Advise |
Alert, Advise, Assure
Advise:
We have reviewed our efficiency and productivity programme for 2025/26. Against the budget saving target, we are behind plan. Our Equality and Quality Impact Assessment process is scheduled to take place in August where a number of schemes will be considered. Subject to approval the schemes can be formally transacted.
At the end of quarter 1, our run-rate savings target is slightly behind
plan but progressing well to date.
Delivery of our Workforce Efficiency Programme
Our performance at the end of quarter 1
| Savings Type | Type | YTD Target | YTD Actual | Status |
| Efficiency Workstream – Overtime Reduction | Run-Rate | £247,947 | £107,209 | Assure |
| Reducing Agency Spend | Run-Rate | £200,000 | £803,128 | Assure |
| Reduce Bank Expenditure | Run-Rate | £120,000 | -£281,583 | Advise |
Alert, Advise, Assure
Advise:
We have reviewed our Workforce Efficiency Programme for 2025/26 and continuing with the exec-led governance in place. In 2024/25 we initiated key strands of work to address reducing bank expenditure by 10%. For 2025/26 bank expenditure is overseen by our Director of Nursing and Professions with a focus on understanding the cross- cutting issues and the interdependency with agency and overtime expenditure.
Assure:
At the end of quarter one we are making good progress and below target with both the reducing agency spend by 30% and overtime expenditure.
Reducing mental health ED attendances and delays project
Our performance at the end of quarter 1
| Objective or Milestone | Start | Finish | Progress | Status |
| Baseline Audit of activity against the ED Action Cards | May-25 | Apr-26 | 5% | Assure |
| Full Review of ALPS System, processes, reporting and partnership working | Jun-25 | Dec-25 | 7% | Assure |
| Pilot improvements that will have the biggest impact on winter 2025 | Oct-25 | Apr-26 | 0% | Assure |
Alert, Advise, Assure
Assure:
We have established a new project to develop, implement and monitor the progress we are making across four workstreams. Ahead of winter the intention is to complete a full review of our Acute Liaison Psychiatry (ALPS) systems and processes and pilot the improvements we believe will have the biggest impact. All activities will be tracked against the two National Oversight Framework metrics.
In addition, working with our partners at LTHT we are exploring how we might be able to create a mental health crisis facility on the acute Trust site.
Delivery of our Inpatient Quality Transformation Programme
Our performance at the end of quarter 1
| Objective or Milestone | Start | Finish | Progress | Status |
| Improving Flow Programme | Sep-24 | Mar-26 | 49% | Assure |
| Culture of Care | Mar-25 | Jan-26 | 22% | Assure |
| Adult Acute Care Pathway | Apr-25 | Jan-27 | 10% | Assure |
Alert, Advise, Assure
Assure:
Improving Flow: Our programme of work to improve flow continues into 2025/26 and we continue to remain on track with key milestones being met. Despite the ongoing work out of area placements remain a challenge and at the end of quarter one we are behind trajectory. This position continues to be actively monitored. Moreover, our length of stay position has reduced in line with the planned trajectory.
Culture of Care: Four wards across Care Services are testing new ways of working based on the Culture of Care standards. At this point work is on track to achieve the pilot milestones.
Adult Acute Care Pathway: At the end of quarter 1 we have initiated a project to review our adult acute care pathway, with scoping/benchmarking against other mental health providers underway.
Delivering a Redesigned Community Mental Health Service Programme
Our performance at the end of quarter 1
| Objective or Milestone | Start | Finish | Progress | Status |
| Implementation of the complex psychosis Pathway Project Group | Mar-25 | Apr-26 | 41% | Assure |
| Optimising LYPFT community services with integrated models of care | Jun-25 | Nov-26 | 2% | Assure |
Alert, Advise, Assure
Assure:
We have initiated a new internal programme of work to develop and implement new community service models of care, with the aim of delivering integration, having fewer teams and improved clinical pathways. Programme governance arrangements have been initiated, with the first meeting held on 3 July 2025. The scope of work currently includes adults, older adults, complex psychosis and adult eating disorders. Other specialist community services are also being considered.
The complex psychosis pathway review now has a signed off model, following stakeholder engagement. A workforce consultation document is in the final stages of development to enable staff engagement to commence during quarter two.
Children and young people transformation programme
Our performance at the end of quarter 1
| Objective or Milestone | Start | Finish | Progress | Status |
| Revise PC Board governance structure including ensuring the PC Development Session includes all nominated place-based leads | Oct-24 | Oct-25 | 30% | Assure |
| Working with place-based providers develop a Standard Operating Procedure that meets the PC aim | Jun-25 | Oct-25 | 30% | Assure |
| Develop a PID documenting the aim/objectives for the PC in 2025/26 | Sep-25 | Sep-25 | 0% | Assure |
| Working with place-based providers develop a Standard Operating Procedure that meets the PC aim | Jun-25 | Oct-25 | 30% | Assure |
| Understanding, identify and address the variation in each place-based pathways | Apr-25 | Dec-25 | 65% | Assure |
| Scoping what an inpatient outreach team, day provision and crisis offer might look like linked with each place-based pathway | Jan-26 | Mar-26 | 30% | Assure |
Alert, Advise, Assure
Assure:
We have initiated a key programme of work both as a CYP provider collaborative partner and internally to improve the overall offer for young people presenting mental health need across the CYP mental health system. Red Kite View is integral to the review, with hospital avoidance being a core principle of quality care and treatment of CYP.
During quarter one we have begun the review of the provider collaborative governance arrangements, with a development session scheduled to take place during quarter two.
Delivering an expanded perinatal inpatient service and provider collaborative
Our performance at the end of quarter 1
| Objective or Milestone | Start | Finish | Progress | Status |
| Perinatal Programme – Ward Build Programme | Sep-25 | Feb-26 | 0% | Assure |
| Phased Start | Feb-26 | May-26 | 0% | Assure |
| Organise workshop for stakeholders | May-25 | May-25 | 100% | Assure |
| Collate and write report on outputs from workshop with recommendations and present at CRG/Assurance Board | Jun-25 | Jun-25 | 100% | Assure |
| Agree and prioritise recommendations | Jul-25 | Aug-25 | 20% | Assure |
| Form working groups / develop project initiation docs for sign off | Sep-25 | Sep-25 | 0% | Assure |
| Stand up working group to analyse current pathway and agree on local additions | May-25 | May-25 | 100% | Assure |
| Document and agree pathway with wider collaborative groups with local protocols added | Jun-25 | Aug-25 | 100% | Assure |
| Organise and deliver a session with other PNPC to deepen understanding of existing inclusion/exclusion criteria | Jul-25 | Sep-25 | 0% | Assure |
| Work closely with Referral Management Service to develop collective understanding of agreed pathway | Jun-25 | Feb-26 | 10% | Assure |
| Design information/education sessions in relation to pathway | Aug-25 | Nov-25 | 0% | Assure |
| Develop TOR and seek opinion from CRG | Sep-25 | Oct-25 | 0% | Assure |
| Set up working group | May-25 | May-25 | 100% | Assure |
| Develop Project Brief/action plan for sign off | Jul-25 | Jul-25 | 50% | Assure |
| Set up working group through Co-Production Group | Jun-25 | Jul-25 | 20% | Advise |
| Develop project brief/action plan for sign off | Jul-25 | Aug-25 | 50% | Assure |
| Link community workforce with MBU so induction/experience/insight into MBU operations can be gained by community staff | Sep-25 | Mar-25 | 0% | Assure |
| Collect data from community partners for WTE/demand/activity | Apr-25 | Mar-26 | 25% | Assure |
| Analysis of demographics at place level across the system | Jul-25 | Sep-25 | 0% | Assure |
| Analysis of demographic demand at community level | Aug-25 | Oct-25 | 0% | Assure |
| Analysis of demographic demand at MBU level | Oct-25 | Nov-25 | 0% | Assure |
| Propose targeted interventions to address inequities | Dec-25 | Jan-26 | 0% | Assure |
| Twice yearly healthcare inequality session at CRG | Apr-25 | Mar-26 | 28% | Assure |
| Agree and disseminate post go live evaluation of PC in first year (in addition to RC survey) | Jan-26 | Feb-26 | 0% | Assure |
Alert, Advise, Assure
Advise:
The Perinatal Provider Collaborative (PC) was formally initiated during 2024/25. Largely the work is on track, however we are slightly behind with fully establishing a Co-Production Working Group. It is expected that this will get underway during quarter two.
Assure:
Aligned with the opening of the expanded perinatal inpatient ward, work is underway with PC stakeholders to facilitate how the beds will be utilised/accessed.
Delivering Improving Health Equity Strategic Priorities
Our performance at the end of quarter 1
| Objective or Milestone | Start | Finish | Progress | Status |
| Increased coordination of LYPFTs existing programmes, projects and initiatives focused on improving equity to amplify the impact and efficiency of existing initiatives. | Apr-25 | Mar-26 | 80% | Assure |
| Ensure we are meeting our statutory obligations relating to equity, maximising opportunities to broaden this work and embed within the broader strategic plan. This includes Equality Act, Public Sector Equity Duty, EDS 22, PCREF and the Health Inequalities Duties under Health and Care Act. | Apr-25 | Mar-26 | 80% | Assure |
| Strengthen our foundations: a focus on our patient, carer, staff and community engagement. | Apr-25 | Mar-26 | 80% | Assure |
Alert, Advise, Assure
Assure:
At the end of quarter one our Institute for Health Equity (IHE) action plan has been approved with a new IHE team established to support its delivery. New governance arrangements have been initiated to have oversight of the plan progress.
We have made fantastic progress against all three objectives. For the ‘strengthen our foundation’ objective which has a focus on patients, carers and staff, we have successfully engaged with the Racial Equity in Health and Social Care (FRESH) and agreed the objectives and recruited lived experience partners.
Create clinical outcome reporting systems enabling the implementation of outcome measures across all our care services
Our performance at the end of quarter 1
| Objective or Milestone | Start | Finish | Progress | Status |
| Establish ePROMs (electronic Patient Reported Outcome Measures) Project governance arrangements, including the development of a PID and Project Timeline | Jun-25 | Aug-25 | 5% | Advise |
| Develop understanding of the use of ePROMs across all service areas | Jun-25 | Oct-25 | 5% | Assure |
| Pilot and evaluate ePROMs questionnaires through Patient Portal Questionnaire/Survey Module for the Gambling Service | Oct-25 | Dec-25 | 0% | Assure |
| Pilot and evaluate ePROMs questionnaires and deployment approach through Patient Portal Questionnaire/Survey Module within two CMHT services | Jan-26 | Mar-26 | 0% | Assure |
| Deploy ePROMS across all in-scope services across the Trust. Deployment phased by readiness/infrastructure | Apr-26 | Dec-26 | 0% | Assure |
| Design, build and test the Patient Portal | Jan-25 | Jun-25 | 65% | Advise |
| Expression of interest submitted to integrate the Patient Portal with the NHS App | Jun-25 | Jun-25 | 100% | Assure |
| Compliance, testing and training for Patient Portal including the creation and approval of the Digital Clinical Safety Case and training materials for all staff using Patient Portal | Jul-25 | Sep-25 | 5% | Advise |
| Onboard with the NHS App MH Wayfinder Programme in readiness for the Trust endorsing the use of the Patient Portal Appointments Module | Jul-26 | Dec-26 | 0% | Assure |
Alert, Advise, Assure
Advise:
We have reviewed the delivery objectives for this priority in 2025/26. This is to link the Patient Reported Outcome Measure (PROM) usage with the Patient Portal App. We are seeking additional resources to help in working with each in-scope service, in order to understand the PROMs in use, how the information is gathered and how the Patient Portal App can be used as the vehicle for service users completing their PROM questionnaire.
At the end of quarter one we have not managed to deploy the new patient portal application as intended. The SMS connectivity has now been resolved enabling the building and testing of the patient portal to progress. We are however awaiting confirmation of email connectivity, which we are working to address during quarter 2.
Assure:
During quarter one we have submitted an expression of interest for integrating the Patient Portal with the NHS App.
Development and implementation of Quality and Culture dashboards for revision in selective services
Our performance at the end of quarter 1
| Objective or Milestone | Start | Finish | Progress | Status |
| Engage clinical leaders: Hold workshops with Clinical Team Managers and professional leads to introduce STEEEP and daily management systems | Apr-25 | Jun-25 | 100% | Assure |
| Baseline understanding: Assess current knowledge and define local meaning for each STEEEP domain (starting with Safe). | Apr-25 | Jun-25 | 100% | Assure |
| Strengthen governance links: Advance the alignment of metrics across team, service line, and beyond for better visibility and assurance | Oct-25 | Dec-25 | 0% | Assure |
| Continue dashboard iteration: Develop or enhance dashboards based on evolving requirements and feedback | Oct-25 | Dec-25 | 0% | Assure |
| Consolidate learning: Use findings from Safe and Effective trials to develop an action plan for rolling out all six STEEEP domains. | Jan-26 | Mar-26 | 0% | Assure |
| Service-wide integration: Finalise dashboard prototype and ensure it supports aligned reporting across teams, services, and board. | Jan-26 | Mar-26 | 0% | Assure |
| Plan for full rollout: Agree next steps for full implementation. | Jan-26 | Mar-26 | 0% | Assure |
Alert, Advise, Assure
Assure:
Quality dashboard: At the end of quarter one we have held a series of workshops with Clinical Team Managers and Professional Leads to introduce STEEEP. The aim of the workshops has been to identify key metrics and consider how they would provide assurance at a team and service level. During quarter two the intent is to finalise the metrics and refine the dashboard design.
Culture dashboard: The objectives and milestones are currently in development for the culture dashboard, with the aim of having these ready for the quarter two report.
Develop and agree our future facilities management model across our PFI sites
Our performance at the end of quarter 1
| Objective or Milestone | Start | Finish | Progress | Status |
| Facilities management long list of delivery model options considered through PFI programme governance | Jul-25 | Jul-25 | 75% | Assure |
| Meeting with NHS England to consider the Trust’s preferred option(s) for soft/hard facilities management | Jul-25 | Aug-25 | 0% | Assure |
| Facilities management short list of delivery model options with a preferred option considered through PFI programme governance | Sep-25 | Sep-25 | 0% | Assure |
| Development and approval of an Outline Business Case for facilities management considered through PFI programme governance and ratified by the Board of Directors | Sep-25 | Nov-25 | 0% | Assure |
Alert, Advise, Assure
Assure:
At the end of quarter one we have completed an analysis of our future facilities management options. This generated a long list that we could risk assess with involvement from key stakeholders across the organisation. The outcome of this exercise will be considered at the next PFI Programme Steering Group meeting scheduled to take place in July 2025.
Conclude the EPR procurement process and develop/ratify the business case for the preferred EPR. In parallel explore and develop options for adding to the existing EPR platform
Our performance at the end of quarter 1
| Objective or Milestone | Start | Finish | Progress | Status |
| Options and OBC Development | Mar-25 | Jul-25 | 100% | Assure |
| OBC Approval | Jul-25 | Jul-25 | 33% | Assure |
| Procurement Preparation | Aug-25 | Nov-25 | 0% | Assure |
| Final Procurement pre approval | Nov-25 | Dec-25 | 0% | Assure |
| Procurement | Jan-26 | Jun-26 | 0% | Assure |
Alert, Advise, Assure
Assure:
At the end of quarter one we have completed the EPR Outline Business Case (OBC) which has been endorsed by the EPR Programme Board. During quarter two the OBC will be considered through other internal governance groups, before final endorsement by the Board of Directors.
Delivery of our People Plan metrics
Our performance at the end of quarter 1
| Ambition | KPI | YTD Target | YTD Actual | Q1 | Latest | Status |
| Looking After Our People | People Promise 4 theme score – We are safe and healthy. | 6.00% | 6.50% | Green | Green | Assure |
| Looking After Our People | Improve staff sickness levels (0.2% reduction year-on-year to 4%) | 5.00% | 6.02% | Amber | Amber | Advise |
| Looking After Our People | Stress and Anxiety | 30.00% | 39.60% | Amber | Amber | Advise |
| Looking After Our People | MSK | 10.00% | 12.70% | Amber | Amber | Advise |
| Looking After Our People | Compulsory Training | 85.00% | 88.00% | Green | Green | Assure |
| Looking After Our People | Wellbeing Assessments | 85.00% | 85.00% | Green | Green | Assure |
| Belonging in the NHS | People Promise 3 theme score – We each have a voice that counts | 7.10% | 7.00% | Green | Green | Assure |
| Belonging in the NHS | Performance Development Review (PDR) Compliance | 85.00% | 83.00% | Green | Green | Assure |
| Belonging in the NHS | Percentage of BAME Colleagues entering Disciplinary Process (WRES)* | 1.25% | 2.37% | Red | Red | Alert |
| Belonging in the NHS | Bullying and Harassment (>70%) | 70.00% | 66.20% | Green | Green | Assure |
| Belonging in the NHS | Percentage of Disabled Staff (staff survey) sharing disability status in ESR | 18.00% | 12.18% | Green | Green | Assure |
| New ways of working and delivering care | Staff Survey Increase the number of staff reporting positive opportunities for flexible working (75% 2 year progressive Target) | 75.00% | 73.00% | Green | Green | Assure |
| New ways of working and delivering care | Clinical Supervision | 85.00% | 74.00% | Amber | Amber | Advise |
| Growing for the future | Vacancies | 5.00% | 12.03% | Red | Red | Alert |
| Growing for the future | Turnover (8-10%) | 10.00% | 7.74% | Green | Green | Assure |
| Growing for the future | Apprenticeships | 80.00% | 74.00% | Green | Green | Assure |
| Growing for the future | Decrease the Internal Bank workforce | 536 | 560 | Green | Green | Assure |
| Growing for the future | Monthly Fill Rates – RN | 80.00% | 84.00% | Green | Green | Assure |
| Growing for the future | Monthly Fill Rates – HCA | 80.00% | 89.00% | Green | Green | Assure |
Alert, Advise, Assure
Alert:
WRES: Although we have seen a reduction in the number of staff entering formal disciplinary processes to such a degree that the WRES metric now reflects a distorted position when viewed in isolation. In 2023/24 we had 25 cases of which 13 colleagues were from an ethnically diverse background. We have seen a positive decrease in case numbers with 13 in total and of those 7 colleagues were from an ethnically diverse background for 2024/25. The Trust has a clear WRES action plan to do more to address this continued disparity.
Advise:
Sickness: At the end of June our sickness rate is at 6.02%. We are however continuing to see an increase in absence related to stress, anxiety and MSK. Absence reasons are being scrutinised as part of the wider workforce efficiency measures.
Clinical supervision: At the end of quarter 1 we are behind the target for clinical supervision.
Assure:
Overall, at the end of quarter 1 we continue to make good progress with our metrics.
Cover sheet for Data Security and Protection Toolkit
- Paper title: Data Security and Protection Toolkit
- Date of meeting: 31 July 2025
- Presented by: Dawn Hanwell, Chief Financial Officer and Deputy Chief Executive
- Prepared by: Carl Starbuck, Head of Information Governance
This paper supports the Trust’s strategic objective/s (SO):
- SO1 – We deliver great care that is high quality and improves lives.
- SO3 – We use our resources to deliver effective and sustainable services.
This paper relates to the Trust’s strategic risks (SR):
- SR1 – Quality including safety assurance processes
- SR6 – Digital technologies
Executive summary
Presenting the final scoring of this year’s NHS England Data Security & Protection Toolkit return. This is the 7th return against the DSP Toolkit and the first against the new Cyber Assessment Framework (CAF) aligned Toolkit, which has seen wholesale revisions of the Toolkit’s content and approach for the 2024/2025 reporting year.
Internal Audit carried out an appraisal of a subset of Outcomes aligned to the national Audit Framework mandated by NHS England.
- Due to Audit opinion being that 1 requirement did not fully meet standards, the audit returned the following result:
- Overall risk determined for the 12 outcomes included in our testing sample:- Medium
- Overall confidence level of Independent Assessment:- Medium
- On the basis of the Audit, the Trust initially returned a ‘Standards Not Met’ result on the Toolkit, with an Improvement Plan drafted to cover the actions agreed with the Auditors, which then gave us an ‘Approaching Standards’ result once the Improvement Plan was approved by NHS England.
- The response to the recommendations must be approved by Dawn Hanwell, CFO (as SIRO). The response to the recommendations will then form our Improvement Plan.
Do the recommendations in this paper have any impact upon the requirements of the protected groups identified by the Equality Act? No
Recommendation
The Board of Directors is asked to:
- Accept the assurance provided by this report, noting that this is already our final position.
- The Improvement Plan will be tracked to completion by IGG in the months ahead.
Data Security and Protection Toolkit
Executive summary
Presenting the final scoring of this year’s NHS England Data Security & Protection Toolkit return. This is the 7th return against the DSP Toolkit and the first against the new Cyber Assessment Framework (CAF) aligned Toolkit, which has seen wholesale revisions of the Toolkit’s content and approach for the 2024/2025 reporting year.
Internal Audit carried out an appraisal of a subset of Outcomes aligned to the national Audit Framework mandated by NHS England.
- Due to Audit opinion being that 1 requirement did not fully meet standards, the audit returned the following result:
- Overall risk determined for the 12 outcomes included in our testing sample:- Medium
- Overall confidence level of Independent Assessment:- Medium
- On the basis of the Audit, the Trust initially returned a ‘Standards Not Met’ result on the Toolkit, with an Improvement Plan drafted to cover the actions agreed with the Auditors, which then gave us an ‘Approaching Standards’ result once the Improvement Plan was approved by NHS England.
- The response to the recommendations must be approved by Dawn Hanwell, CFO (as SIRO). The response to the recommendations will then form our Improvement Plan.
Data Security and Protection Toolkit v7 – 2024-2025
The DSP Toolkit v7 consists of 47 Outcomes broken down into the following 5 domains:-
A – Managing risk (7)
B – Protecting against cyber attack and data breaches (20)
C – Detecting cyber security events (7)
D – Minimising the impact of incidents (5)
E – Using and sharing information appropriately (8)
Figures in brackets denote the number of Outcomes per domain.
Each of the 47 Outcomes breaks down into multiple evidential requirements, with each Outcome having 3 possible results:-
- Not Achieved
- Partially Achieved
- Fully Achieved
Some Outcomes are simplified to just Not Achieved / Fully Achieved.
The vision for the new CAF-aligned Toolkit is to build and strengthen the Outcomes each year over a 5-year planning horizon, such that the Outcomes expected to be Not Achieved or Partially Achieved in the first year are gradually raised to Partially or Fully Achieved, ultimately strengthening the assurance requirement with all Outcomes to be Fully Achieved in year 5.
Each of the Outcomes was passed to an appropriate subject matter expert (mainly in Cyber Security, ICT and Information Governance, but also with some Procurement and HR input), to have them assemble an evidence base against each Outcome and then document our compliance on the DSP Toolkit website. All evidence items must be complete to mark the Outcome as Partially or Fully Achieved.
At the close of the Toolkit in June, and based on the Audit report, the Trust stated that all but 1 Outcome had been met, with the reporting graphically represented per domain as follows:-
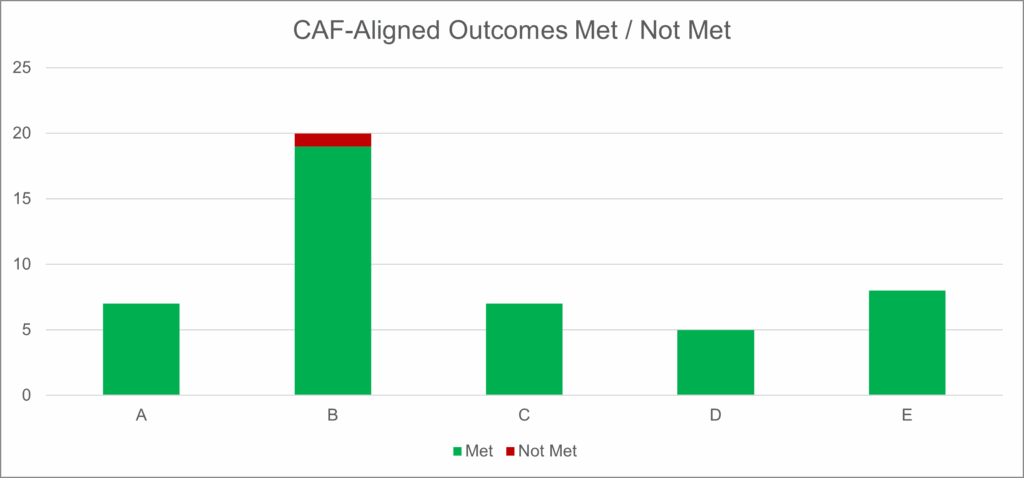
A – Managing risk
B – Protecting against cyber attack and data breaches
C – Detecting cyber security events
D – Minimising the impact of incidents
E – Using and sharing information appropriately
Internal Audit’s appraisal was reported to the Information Governance Group (26th June 2025), however an error was identified in the report (a discrepancy in the reporting, as only 1, not, 2, Outcomes were agreed to be ‘Overstated’). The (final draft) Internal Audit report is attached as Appendix A, which shows the recommendations arising out of the Audit, and the management response to these recommendations.
NHS England has stated that due to reports of large numbers of organisations not achieving ‘Standards Met’, there has been a decision to leave the Toolkit unaltered for the 2nd iteration in 2025-2026, which should then allow us to meet all Outcomes at the next reporting round once the Improvement Plan has been delivered.
Conclusion
This concludes the presentation of the Data Security and Protection Toolkit outcome report for 2024 / 2025.
Recommendation
The Board of Directors is asked to:
- Accept the assurance provided by this report, noting that this is already our final position.
- The Improvement Plan will be tracked to completion by IGG in the months ahead.
Carl Starbuck
Head of Information Governance / Data Protection Officer
24/07/2025
Audit Yorkshire – LY 17/2025 Data Security and Protection Toolkit
Leeds and York Partnership NHS Foundation Trust
27 June 2025
Final Report
Internal audit contacts:
Helen Higgs, Managing Director and Head of Internal Audit
- Email Helen Higgs
- 07931 224784
Jonathan Hodgson, Internal Audit Manager
Will Ellis, Trainee Senior Internal Auditor
- Email Helen Higgs
- 07931 224784
Contents
1. Introduction
2. Executive Summary
3. Key Findings
4. Appendices
Appendix A: Understanding your report ratings
Appendix B: Summary of work undertaken, and risks reviewed
Appendix C: Summary of work undertaken, and risks reviewed – additional outcomes
Appendix D: Audit Brief
Report Distribution
Executive sign-off:
- Dawn Hanwell, Chief Financial Officer and Deputy Chief Executive
Distribution:
- Carl Starbuck, Head of Information Governance
- Ian Hogan, Chief Digital Information Officer
- Hergy Galsinh, Head of Cyber Security
- Andy Gleadall , Head of Network Operations
- Aaron Hull, Cyber Security Specialist
Section 1: Introduction
Why security and governance of information issues in the Health and Social Care sector require attention from independent assessors
Data and information are critical business assets that are fundamental to the continued delivery and operation of health and care services across the UK. The Health and Social Care sector must have confidence in the confidentiality, integrity and availability of their information assets and must ensure that any personal data collected, stored and processed by public bodies are aligned to specific legal and regulatory requirements.
The need to demonstrate an ability to defend against, block and withstand cyber-attacks and data breaches has been amplified by the introduction of the Network and Information Systems (NIS) Regulations and the UK General Data Protection Regulation (GDPR). As such, it is essential that Health and Social Care sector organisations that are impacted by those regulations take proactive measures to defend themselves from cyber- attacks and data breaches and evidence their ability to do so in line with regulatory and legal requirements.
The Cyber Assessment Framework (CAF) aligned Data Security and Protection Toolkit (DSPT) is one of several mechanisms in place to support Health and Social Care organisations in their ongoing journey to manage cyber security and information governance risk.
The CAF-aligned DSPT allows organisations that have access to NHS patient data and systems to measure their performance against the five objectives of the CAF-aligned DSPT, providing valuable insight into the technical and operational security and governance of information control environment and relative strengths and weaknesses of those controls. Another mechanism is to independently assess the security and governance of information control environments of Health and Social Care organisations. Independent assessment providers help to strengthen the trust placed on the CAF-aligned DSPT submissions by Health and Social Care organisations’ boards, Department of Health and Social Care and NHS England by assessing the effectiveness of the organisation’s security and governance of information controls. This approach ensures that the controls in place are effective in securing patient data throughout the organisation’s estate, including staff handling of data and safe storage on the organisation’s systems.
The role independent assessment providers play in helping to strengthen the reliance placed on the CAF-aligned DSPT submissions by Health and Social Care Organisations’ boards, Department of Health and Social Care and NHS England is summarised in the National Data Guardian report, ‘Review of Data Security, Consent and Opt-Outs and the Care Quality Commission report, Safe data, safe care’. Both reports include the following recommendation: ‘Arrangements for internal data security audit and external validation should be reviewed and strengthened to a level similar to those assuring financial integrity and accountability’ (NDG 6, CQC 6 Table of recommendations). Therefore, it is essential that independent assessment providers, including internal auditors, focus on the assessment of the effectiveness of health and social organisations’ security and governance of information controls, as opposed to simply focusing on the veracity of their CAF-aligned DSPT submissions.
Reporting period: 01 July 2024 to 30 June 2025.
Scope and Objectives
This independent assessment provides the following:
- An assessment of the overall risk associated with Leeds and York Partnership NHS Foundation Trust’s (LYPFT) security and governance of information control environment. For example, the level of risk associated with weak or failing controls and security and governance of information objectives not being achieved
- An assessment as to the veracity of LYPFT’s self-assessment / DSPT submission and the Independent Assessor’s level of confidence that the submission aligns to their assessment of the risk and controls. The objective of this independent assessment from Audit Yorkshire’s perspective is to understand and help address security and governance of information risk and identify opportunities for improvement; whilst also satisfying the annual requirement for an independent assessment of the DSPT submission.
Scope of the review
The scope of the review included consideration of processes supporting the DSPT self-assessment process, including:
- The process for compiling and reviewing the toolkit (including approval within the governance structure); and
- The availability of evidence supporting in-scope outcomes and validation of that evidence by the DSPT Coordinator.
Our approach
Our work has involved the following activities:
- Meetings with key staff involved in the process
- Walkthroughs of key processes relevant to the completion of the DSPT
- Desktop review of documentation supporting the DSPT
- Sample testing where appropriate.
In cases where we note controls do not exist, we have raised this as a finding.
Out of Scope
- Our work is limited to assessment of the evidence to support the 12 outcomes required to be assessed for this review (as detailed in Appendix A and B) therefore, the review will not provide assurance that the entire DSPT return is accurate and complete.
- Our work will not include detailed testing of information technology (IT) systems and will not cover the submission of the DSPT.
- Further limitations of scope identified during our work will be included within the final report.
Section 2: Executive Summary
CAF-aligned DSPT Independent Assessment Report Outputs
Our review followed the CAF-aligned DSPT Independent Assessment Framework and Guidance published by NHS England. We have reviewed 12 outcomes across the five objectives in the Cyber Assessment Framework. NHS England have mandated eight outcomes to be audited for 2024/2025, together with a further four outcomes to be audited which have been approved by the LYPFT Board.
We produced this report as an output of this review. As a result of our evidence assessment and interviews with key stakeholders, we have delivered five findings in total. All findings and associated management actions have been discussed and accepted by Dawn Hanwell, Chief Financial Officer and Deputy Chief Executive, on behalf of the Trust.
Overall Risk Assurance Rating
| Overall risk determined for the 12 outcomes included in our testing sample, across all five CAF objectives | Medium |
| This is a measurement of how many outcomes have been assessed as not meeting the minimum standard as prescribed by NHS England. | Medium |
| Overall confidence level of Independent Assessment | Medium |
| This is a measurement of whether the evidence provided by the Trust meets their own self-assessment of outcome achievement levels. | Medium |
The tables below summarises our independent assessment of each outcome in our testing sample. The overall risk rating has been derived from an evaluation of the impact and likelihood of each in-scope outcome, to derive an overall assessment conclusion based on NHS England guidance. The risk scoring is based on our assessment that no more than one outcome is rated as not meeting minimum achievement levels required.
The overall confidence level denotes the organisation’s self-assessment against the Toolkit deviates slightly from our Independent Assessment.
Overall Risk Assurance Rating
The tables below summarises our independent assessment of each outcome in our testing sample. The overall risk rating has been derived from an evaluation of the impact and likelihood of each in-scope outcome, from which we have assigned a point scoring to derive an overall assessment conclusion based on NHS England guidance. The risk scoring is based on our assessment that the Trust is not meeting the minimum achievement level for two mandatory outcomes and one additional outcome.
| Objective | Outcome | Minimum achievement level set by NHSE (as per the profile set for 24/25) | Trust assessed achievement level | IA assessed achievement level | High | Medium | Low | Minimum Level Met | Minimum achievement level met? |
| A | A2.a | Partially Achieved | Partially Achieved | Partially Achieved | None | None | None | PA#1- PA#7 | Yes |
| A | A4.a | Partially Achieved | Partially Achieved | Partially Achieved | None | None | None | PA#1 – PA#7 | Yes |
| B | B2.a | Partially Achieved | Not Achieved | Not Achieved | None | PA#3, PA#6 | PA#4 | PA#1 – PA#3, PA#5, PA#7 | No |
| B | B4.d | Partially Achieved | Partially Achieved | Partially Achieved | None | None | PA#1 | PA#1 – PA#5 | Yes |
| C | C1.a | Partially Achieved | Partially Achieved | Partially Achieved | None | None | None | PA#1 – PA#3 | Yes |
| D | D1.a | Partially Achieved | Partially Achieved | Partially Achieved | None | PA#3 | None | PA#1 – PA#6 | Yes |
| E | E2.b | Achieved | Achieved | Achieved | None | None | A#3 | A#1 – A#3 | Yes |
| E | E3.a | Achieved | Achieved | Achieved | None | None | None | A#1 – A#6 | Yes |
| A | A1.a | Achieved | Achieved | Achieved | None | None | None | A#1 – A#4 | Yes |
| A | A2.b | Achieved | Achieved | Achieved | None | None | A#5 | A#1 – A#5 | Yes |
| B | B3.c | Partially Achieved | Partially Achieved | Partially Achieved | None | None | None | PA#1 – PA#4 | Yes |
| B | B3.e | Partially Achieved | Partially Achieved | Partially Achieved | None | None | None | PA#1 | Yes |
We have determined overall risk rating of the organisation’s data security and protection control environment, for the in-scope assessments as Medium. Our assessment is based on NHS England guidance. The NHS England definitions in Appendix A were used for aiding the decision of calculating the overall risk assessment for Leeds and York Partnership Foundation Trust.
Areas of good practice
- The Trust has a number of policies in place to support the management of risks relating to Information Security and Governance
- Processes are in place to identify analyse and prioritize risks.
- Confidence in the effectiveness of the Trust’s IT security comes from a number of different sources.
- The Trust has included Data Protection and Cyber Security Clauses within contracts with suppliers.
- The Trust has a procedure in place to manage remote access to the network.
- Systems are in place to help ensure backups of critical data.
- Devices containing data important to the Trust’s operation are disposed of by an appropriately qualified and accredited company.
- Announced vulnerabilities are tracked and prioritized.
- Monitoring is in place to highlight cases of suspicious or undesirable behaviour.
- The Trust has a Cyber Incident Response Plan and an ICT Networks Disaster Recovery Plan.
- Data Security Awareness training is mandatory for all staff.
- An escalation route to the Information Governance lead is in place to respond to staff queries regarding data sharing.
Summary of key findings
| Criteria | Findings |
| A2.b – Risk Management | 3.1 • The Trust reviews existing methods of gaining IT Security assurance but have not formally documented this process. Risk: The methods used for assurance may not remain the most appropriate if not reviewed. |
| B2.a – Identity verification, authentication and authorisation | 3.2 • The systems which support the essential functions across the Trust have not been identified and do not have supporting documented procedures for system onboarding, offboarding and access recertification. Risk: User accounts could gain or retain inappropriate access to sensitive information which could result in a data breach. |
| B4.d – Vulnerability Management | 3.3 • The Trust has processes and systems in place to manage vulnerabilities and create backups of critical data but have not formally documented these. Risk: Announced vulnerabilities for software packages, network and information systems may not be addressed in the absence of key staff members. |
| D1.a – Response plan | 3.4 • The Trust has a Cyber Incident Response Plan alongside its Business Continuity Plans and Emergency Incident Response Plan. However, the most recent Cyber Incident scenario test took place in 2023. It is recommended that the Trust completes a test of its Cyber Incident Response procedures to help prepare staff to respond should the Trust be impacted by a Cyber Incident. Risk: Staff may not be adequately prepared to respond to a Cyber Incident. |
| E2.b – Consent | 3.5 • The Trust shares information regarding its use of information with the public via its website, but some links on the website were found to be broken. Risk: Information provided to patients and service users about the use and sharing of information may not be clear. |
Section 3: Key Findings
3.1 A2.b Risk Management – Low Risk
For Outcome A2.b Risk Management, we noted opportunities to strengthen the process used to review existing assurance methods, which is required as per the national guidance for the following indicator of good practice:
- A#5 The methods used for assurance are reviewed to ensure they are working as intended and remain the most appropriate method to use.
As per the CAF requirements of A#5 the risk management process should demonstrate that the organisation has a scheduled or efficiently reactive process for reviewing its assurance methods which ensures that they remain appropriate. Whilst procedures for carrying out vulnerability identification are well established within the team and discussions to review services provided by external assurance providers take place as and when reports are commissioned, there is currently no documented procedure to support the reviewing of existing assurance methods to ensure they are still fit for purpose. For example, an IT Health Check was commissioned by an external organisation for the Trust, but a timetable and procedure to commission future reports and to review internal processes used to gain assurance are not documented. This is assessed as low risk due to the established processes within the team, however it is recommended that the procedure is documented to help ensure assurance methods are reviewed regularly and that this review can be completed in the absence of key staff members.
Risk
Low – The Methods used for assurance may not remain the most appropriate if not reviewed regularly.
Recommendation
1. The Trust should document process used to review assurance methods to ensure this is completed and recorded on an annual basis.
Management Response
| Recommendation | Management Response | Target Date |
| 1. The Cyber Security team will conduct an annual appraisal of the multiple assurance methods used to make sure they remain fit for purpose when considered against the current threat landscape, based on intelligence received from appropriate sources (e.g., NHS England, National CSOC Weekly Cyber Alert Bulletin, NIST, Wildfire, MDE and RSS Feeds), and will present these findings to the Information Governance Group / Digital Steering Group for ratification of an approved and robust approach to Cyber Security assurance. | Hergy Galsinh, Head of Cyber Security (Deputising Officer – Aaron Hull, Cyber Security Specialist) |
31/12/2025 |
Evidence to confirm implementation
1. Papers presented to the Information Governance Group / Digital Steering Group and minutes documenting approval or further recommendations of the committee members.
3.2 B2.a Identity verification, authentication and authorisation – Low / Medium Risk
For Outcome B2.a Identity verification, authentication and authorisation, we noted further action is required to meet the following indicators of good practice, and therefore to meet the required standards for this overall outcome:
- PA#3 All authorised users and systems with access to information, systems and networks on which your essential function(s) depends are individually identified and authenticated.
- PA#6 The list of users and systems with access to information, systems and networks supporting and delivering the essential function(s) is reviewed on a regular basis, at least annually.
CAF requirements of PA#3 and PA#6, are dependent on the Trust identifying the systems it has in place that support its essential functions and having processes in place to grant and remove access, perform access recertification annually. Whilst the Trust shared a list of systems which are in use, it has not identified which systems are specifically required for the Trust to provide its essential functions and processes for the creation and removal of user accounts and for employee transfers do not take these systems into account. Additionally, PA#6 includes a requirement to recertify access to essential systems on a yearly basis and this is not currently taking place. This is assessed as medium risk due to the possibility of users gaining or retaining access to inappropriate sensitive data
For the below indicator of good practice we noted opportunities to strengthen the processes around the use of MFA at the Trust.
- PA#4 You use additional authentication mechanisms, such as multi-factor authentication (MFA), for privileged access to all network and information systems that operate or support your essential function(s).
The Trust has implemented MFA for its privileged access to IT systems and it is recommended to further develop this by documenting, risk-assessing, and internally approving cases where MFA has not been implemented for systems that support the Trust’s essential functions.
Risk
Medium Risk – User accounts could gain or retain inappropriate access to sensitive information which could result in a data breach.
Recommendation
2. The Trust should identify which applications are used to support its essential functions, ensure processes are in place to manage the granting and removal of access within these systems and ensure an annual recertification of access within these systems is completed.
Management Response
| Recommendation | Management Response | Target Date |
| 2. To address the recommendation effectively, a phased approach will be adopted as outlined below:Phase 1: Identification of Essential Applications
An initial review will be conducted to identify all applications that underpin the Trust’s essential business and clinical functions. This will be led by myself assisted by DDaT colleagues, in collaboration with application leads, to ensure comprehensive coverage and accurate classification of systems. Phase 2: Access Management Process Review and Implementation Following identification, there will be a review of existing processes related to user access provisioning and deprovisioning. Where gaps are identified, standardised procedures will be developed and implemented to ensure that access rights are granted based on role-based requirements and promptly revoked upon changes in employment status or responsibilities. This will include clear lines of accountability and documentation of access approvals. Phase 3: Annual Access Recertification. The application lead will undertake an annual recertification exercise which challenges and corroborates all currently open access for the application under their lead and create a written report of findings to support future audit. |
Andy Gleadall, Head of Network Operations l | 31/12/2025 |
Evidence to confirm implementation
2. Essential Application Register
Associated Procedural Documents per essential application
Recertification reports (where available)
3.3 B4.d Vulnerability Management – Low Risk
For outcome B4.d Vulnerability Management we noted opportunities to strengthen the process used to Monitor and Manage vulnerabilities, which is required as per the national guidance for the following indicators of good practice:
- PA#1 Your response plan covers your essential function(s).
As per the CAF requirements of PA#5 the Trust must receive, track and analyse announced vulnerabilities, prioritise the vulnerabilities based on risk and mitigate externally exposed vulnerabilities within a defined timeframe. Discussions with key contacts confirmed that whilst these processes are taking place and are embedded within the team as day-to-day activities, they are not supported by procedural documentation which could result in the Trust being unable to manage its vulnerabilities in the absence of key staff members. This is assessed as low risk due to the demonstration of established processes which already in place.
Risk
Low Risk – Announced vulnerabilities for software packages, network and information systems may not be addressed in the absence of key staff members
Recommendation
3. The Trust should document the procedures used to identify indicators of compromise, manage and apply patches to known vulnerabilities and to perform data backups.
Management Response
| Recommendation | Management Response | Target Date |
| 3. The procedures for identifying IOCs, patching vulnerabilities and applying backups will be documented to ensure that in the absence of key staff members, the process of these foundational processes can continue.
The creation of the document will have a phased approach: Phase1: Define the purpose and scope of the document, and identify roles and responsibilities of key staff members and their delegates where required. This will ensure that the processes may resume even in the absence of key staff members. It also ensures that there are clear boundaries and responsibilities to ensure these processes are being adhered to. Phase2: Identify and document existing procedures of IOC Detection, Patch Management and Backup/Recovery. This section will define the definition and purpose of each of the processes discussed, including the validity of each. Phase3: Create a review and audit schedule of the document and processes contained within; ensuring it is referenced against the relevant standards and frameworks. The document should be reviewed by DSG to ensure alignment with strategy. |
Hergy Galsinh, Head of Cyber Security
(Deputising Officer – Aaron Hull, Cyber Security Specialist) |
31/12/2025 |
Evidence to confirm implementation
3. Papers presented to IGG / DSG and minutes documenting approval or further recommendations of the committee members.
3.4 D1.a Response plan – Medium Risk
For outcome D1.a Response Plan we noted opportunities to strengthen the Trust’s Cyber Incident Response Plan, which is required as per the national guidance in relation to the following indicator of good practice:
- PA#3 Your response plan is understood by all staff who are involved with your organisation’s response function.
As per the CAF requirements for D1.a the Cyber Incident Response Plan should identify and document: scenarios for known attacks and incidents; assigned roles and responsibilities of staff within the response function; the obligations of the organisation as controller or processor of personal data for the reporting of incidents; existing system partners with key contacts for each to enable notification. Our review found that at the time of the audit, these elements were not specifically identified within the Trust’s Cyber Incident Response Plan, however this has been addressed with documentation updated and approved by the relevant committee.
This outcome has been assessed as medium risk as whilst supporting documentation is now in place to satisfy the Cyber Incident Response Plan requirements within the DSPT, the most recent Cyber Incident Response scenario testing was carried out in 2023. It has therefore been recommended that the Trust carry out regular Response Plan testing to help prepare staff to respond should the Trust be impacted by a Cyber Incident.
Risk
Medium Risk – Cyber Incident Response Team members may not be able to deploy their capabilities to minimise the adverse impact of an incident on the operation of essential functions, including the restoration of those functions.
Recommendation
4. The Trust should complete a regular Cyber Incident Response scenario test to ensure all team members are familiar with their roles and responsibilities should the Trust be impacted by a Cyber Incident.
Management Response
| Recommendation | Management Response | Target Date |
| 4.
The Responsible Officer will liaise with the EPRR lead to establish when the next Trustwide exercise will take place, and its proposed theme.
The Responsible Officer will ensure that appropriate DDaT personnel have reserved time to participate and will seek Executive Officer participation. |
Ian Hogan, Chief Digital Information Officer | 31/12/2025 |
Evidence to confirm implementation
4. Exercise will be documented as previously, with any DDaT outcomes used to formulate an improvement plan, with actions tracked to completion.
3.5 E2.b Consent – Low Risk
For outcome E2.b consent we noted opportunities to strengthen the information provided to patients and service users about the use and sharing of information and consent, which is required as per the national guidance for the following indicators of good practice:
- A#3 Information provided to patients and service users about the use and sharing of information and consent is appropriate and clear
As per the CAF requirements of A#3 the Trust must provide transparency materials and exemplar communications with the public relating to consent for information sharing. Our review found that the Trust provides public facing information regarding consent and detailing processes for the sharing and use of information though its website, however some of the links on the website, such as the link to the Information Governance Policy or the Leeds City-wide Information Sharing Protocol, were not working at the time of the audit. This is assessed as low risk as the materials are already in existence and the finding can be addressed through a minor update to the Trust’s website.
Risk
Low Risk – Information provided to patients and service users about the use and sharing of information may not be clear.
Recommendation
5. The Trust should perform a review of the “How we use information about you” section of its website to ensure all links are working correctly.
Management Response
| Recommendation | Management Response | Target Date |
| 5. Review of relevant Trust website pages to ensure all content is current and up-to-date and all hyperlinks are live. Upon initial examination it appeared that some document links had been broken during work on the Trust’s public facing website for Accessibility compliance and in reforming the approach to our FoIA Publication Scheme.
Hyperlinks to contact e-mail addresses have also been checked and updated where required. Change document submitted to and actioned by the Trust Communications Team. |
Carl Starbuck, Head of Information Governance | Completed |
Evidence to confirm implementation
5. Copy of change documented and evidence of updates to website.
Appendix A: Understanding your report ratings
Overall Risk Assurance Rating
The table on the next slide shows the ‘Overall Risk Assurance Across all five CAF objectives’ as well as the ‘Confidence level of the Independent Assessor in the veracity of the self-assessment’. It includes the calculation of each risk assurance rating by detailing the scores obtained at each outcome level with respect to their category (Low, Medium, High and Critical). To better understand the ‘scoring methodology’ please see the worked example in Appendix C.
We assessed the overall risk across all five objectives as Medium and the confidence level of the Independent Assessor in the veracity of the self-assessment as Medium.
The overall Risk Rating for the Trust is Medium.
The rating is based on a risk assurance rating score at the CAF-aligned DSPT level. Scores have been calculated using tables 4 and 5 (see section 2.4, Task Three – Deliver CAF-aligned DSPT Independent Assessment of the independent assessment Guidance document and the Executive Summary
Understanding your report ratings – Assurance Level
The assurance level for the Trust (based on the overall risk across all five objectives) is Medium
The rating is based on a risk assurance rating score at the CAF-aligned DSPT level. Scores have been calculated using tables 4 and 5 (see section 2.4, Task Three – Deliver CAF-aligned DSPT Independent Assessment of the independent assessment Guidance document and Appendix C within this report).
- Overall risk determined for the 12 outcomes included in our testing sample, across all five CAF objectives: Medium
- Overall confidence level of Independent Assessment: Medium
Veracity of your DSPT self-assessment
We have assessed 12 outcomes, and found that, for all 12 outcomes, our rating aligned with the organisation’s self-assessment. However, we noted that, for one outcome, there were findings identified during the course of the audit that impacted the overall achievement level, resulting in a Medium level of deviation between the independent and self-assessment. The confidence level in the veracity of the DSP Toolkit self-assessment is therefore ‘Medium’.
Independent assessment Outputs
- Overall risk determined for the 12 outcomes included in our testing sample, across all five CAF objectives: Medium
- Overall confidence level of Independent Assessment: Medium
How to determine the indicator of good practice achievement level
The CAF-aligned DSPT Independent Assessor must assess the achievement level for each in-scope DSPT indicator of good practice assessed as part of their DSPT review. The Independent Assessor leverages knowledge and subject matter expertise alongside observations made during the assessment to evaluate each indicator of good practice against the Not Achieved, Partially Achieved or Achieved statements of the Cyber Assessment Framework. These statements are used to assign an achievement level to each indicator of good practice.
This achievement level reflects the maturity of the organisation in being able to meet the expected outcomes through implementation of controls and processes.
How to determine the outcome level achievement level
The DSPT Independent Assessor must then follow the CAF requirements to assign an achievement level at the outcome level. The CAF states that an outcome will be rated as Achieved if every underlying indicator of good practice is rated as Achieved. An outcome with be rated as Not Achieved if one or more underlying indicator of good practice is rated as Not Achieved. Finally, an outcome will be rated as Partially Achieved if no indicator of good practice is rated as Not Achieved, but not all indicators of good practice are rated as Achieved.
How to determine the overall risk rating for the organisation
The DSPT Independent Assessor then uses the table below to assign an overall risk rating to the organisation.
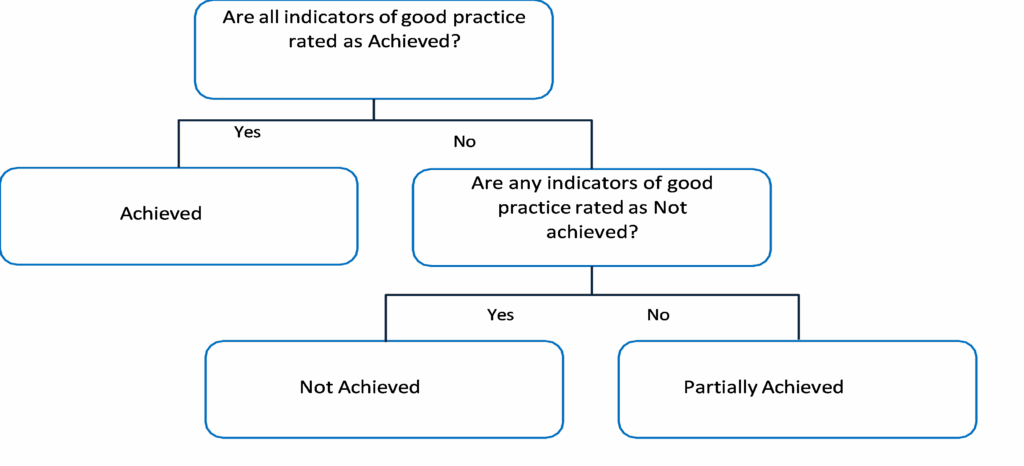
Overall Risk Rating across all tested outcomes
- Very High: More than four outcomes are rated as not meeting minimum achievement levels required and/or the organisation cannot comply with mandatory policy requirements.
- High: Between two and four outcomes are rated as not meeting minimum achievement levels required.
- Moderate: No more than one outcome is rated as not meeting minimum achievement levels required.
- Low: All minimum achievement levels have been met.
- Very Low: All minimum achievement levels have been met and achievement levels have been exceeded for at least one outcome.
Overall Confidence and Risk Levels
The confidence-level in the veracity of the Trust’s DSPT self-assessment submission has been determined by comparing our assessment findings against the self-assessment made by the Trust. The following NHS England definitions were used for aiding the decision of applying a confidence-level.
| Level of deviation between self and independent assessment | Confidence level |
| High level of deviation – the organisation’s self-assessment against the Toolkit differs significantly from the Independent Assessment. For example, the organisation has declared as “Standards Met” (meeting the expected achievement levels across all outcomes) but the independent assessment has found multiple outcomes as not meeting minimum levels of achievement. |
Low |
| Medium level of deviation – the organisation’s self-assessment against the Toolkit differs somewhat from the Independent Assessment. For example, the Independent Assessor has exercised professional judgement in comparing the self-assessment to their independent assessment and there is a non-trivial deviation or discord between the two. |
Medium |
| Low level or no deviation – the organisation’s self-assessment against the Toolkit does not differ / deviates only minimally from the Independent Assessment. | High |
Appendix B: Summary of work undertaken, and risks reviewed – Mandatory outcomes
Below we set out our assessment of the organisations’ current scores for the CAF outcomes reviewed under the scope of this assessment.
We have based our assessment on the requirements set out within the NHS England Independent Assurance Framework, and indicated whether not, in our opinion, Leeds and York Partnership Foundation Trust have met the in-scope outcomes.
| Assessment Category | Definition |
| Agree | From the evidence available we are able to agree with the organisation’s self-assessment as a reasonable assessment of current performance. |
| Understated | From the evidence provided it is our assessment that the organisation is performing at a level higher than recorded. |
| Overstated | From the evidence available we are not able to agree the self-assessment as a reasonable assessment of current performance. |
| Agree but insufficient | From the evidence provided it is our opinion the organisation has been accurate with its self-assessment, but it has not currently completed the mandatory outcomes as required by NHSE. |
A2.a
Your organisation has effective internal processes for managing risks to the security and governance of information, systems and networks related to the operation of your essential function(s) and communicating associated activities. This includes a process for data protection impact assessments (DPIAs).
| IGP# | Trust/ICB Assessment | Internal Audit Assessment | Comment | Overall Assessment |
| PA#1 | Partially Achieved | Agree | The organization has processes in place to identify, analyse and prioritize risk. Risk assessments support data protection by design. | Agree |
| PA#2 | Partially Achieved | Agree | Risk assessments are informed by an understanding of system vulnerabilities. | Agree |
| PA#3 | Partially Achieved | Agree | Risk management processes have clear outputs and are aligned with the Trust’s overall strategic goals. | Agree |
| PA#4 | Partially Achieved | Agree | Governance Groups are in place to support the discussion and communication of updates of Risks to key stakeholders. | Agree |
| PA#5 | Partially Achieved | Agree | Evidence was shared with us demonstrating processes for assessing risk. | Agree |
| PA#6 | Partially Achieved | Agree | The Trust performs threat analysis based on internal and external intelligence. | Agree |
| PA#7 | Partially Achieved | Agree | Trust policies and procedures show that legislation such as UK-GDPR is considered. | Agree |
A4.a
The organisation understands and manages security and IG risks to information, systems and networks supporting the operation of essential functions that arise as a result of dependencies on external suppliers. This includes ensuring that appropriate measures are employed where third party services are used.
| IGP# | Trust/ICB Assessment | Internal Audit Assessment | Comment | Overall Assessment |
| PA#1 | Partially Achieved | Agree | The Trust has a Supplier Business Continuity Assurance Procedure | Agree |
| PA#2 | Partially Achieved | Agree | The Trust maintains a list of all contracts with its suppliers | Agree |
| PA#3 | Partially Achieved | Agree | A sample of supplier contracts were found to include Cyber Security and Data Protection obligations. | Agree |
| PA#4 | Partially Achieved | Agree | The Trust’s ICT Disaster Recovery Plan lists external parts with connections at the Trust. | Agree |
| PA#5 | Partially Achieved | Agree | Supplier contracts include obligations regarding scheduled and unscheduled downtime | Agree |
| PA#6 | Partially Achieved | Agree | Data Protection Impact Assessments for two sampled suppliers showed that the Trust has performed an assessment with information shared with suppliers. | Agree |
| PA#7 | Partially Achieved | Agree | Data is not transferred internationally | Agree |
B2.a
You robustly verify, authenticate and authorise access to the information, systems and networks supporting your essential function(s).
| IGP# | Trust/ICB Assessment | Internal Audit Assessment | Comment | Overall Assessment |
| PA#1 | Partially Achieved | Agree | Agree – pending confirmation that temporary staff members are verified. | Agree but insufficient |
| PA#2 | Partially Achieved | Agree | The Trust has a policy in place to demonstrate the process to authenticate users accessing the network. | Agree but insufficient |
| PA#3 | Partially Achieved | Agree but insufficient | The Trust should identify its essential applications and ensure documented processes are in place for granting and removing access. | Agree but insufficient |
| PA#4 | Partially Achieved | Agree | The Trust should ensure it is documenting, risk-assessing, and internally approving cases where MFA has not been implemented. | Agree but insufficient |
| PA#5 | Partially Achieved | Agree | A procedure is in place to manage remote access to the network. | Agree but insufficient |
| PA#6 | Partially Achieved | Agree but insufficient | The Trust should identify its essential applications and ensure an annual recertification of existing access is carried out. | Agree but insufficient |
| PA#7 | Partially Achieved | Agree | The Trust’s password policy is aligned with industry best practice. | Agree but insufficient |
B4.d
You robustly verify, authenticate and authorise access to the information, systems and networks supporting your essential function(s).
| IGP# | Trust/ICB Assessment | Internal Audit Assessment | Comment | Overall Assessment |
| PA#1 | Partially Achieved | Agree | Threat Intelligence is gathered from a number of sources. Supporting documentation should be created to ensure this can be completed in the absence of key staff. | Agree |
| PA#2 | Partially Achieved | Agree | Announced vulnerabilities are tracked and prioritized. However, this is not managed using a documented process. | Agree |
| PA#3 | Partially Achieved | Agree | The Trust has identified and documented some vulnerabilities that have temporary mitigations. | Agree |
| PA#4 | Partially Achieved | Agree | Monitoring is in place to scan for unsupported systems. Unsupported systems are logged, and risk assessed. | Agree |
| PA#5 | Partially Achieved | Agree | Regular vulnerability testing takes place. | Agree |
C1.a
You robustly verify, authenticate and authorise access to the information, systems and networks supporting your essential function(s).
| IGP# | Trust/ICB Assessment | Internal Audit Assessment | Comment | Overall Assessment |
| PA#1 | Partially Achieved | Agree | Evidence provided shows that data relating security of IT Functions is collected by the Trust. | Agree |
| PA#2 | Partially Achieved | Agree | Technical solutions are in place to detect indicators of compromise however procedures are not formally documented. | Agree |
| PA#3 | Partially Achieved | Agree | Security monitoring is done which highlights cases of suspicious or undesirable behavior. | Agree |
| PA#4 | Partially Achieved | Agree | Processes to monitor traffic are in place however procedures are not formally documented. | Agree |
D1.a
You have an up-to-date incident response plan that is grounded in a thorough risk assessment that takes account of your essential function(s) and covers a range of incident scenarios.
| IGP# | Trust/ICB Assessment | Internal Audit Assessment | Comment | Overall Assessment |
| PA#1 | Partially Achieved | Agree | The Trust has a documented Cyber Incident Response Plan | Agree |
| PA#2 | Partially Achieved | Agree | The Incident Response Playbook covers specific scenarios or threats that may impact the Trust | Agree |
| PA#3 | Partially Achieved | Agree | Incident Response Scenario Testing is carried out, but the most recent testing did not involve all current members of the Incident Response Team. | Agree |
| PA#4 | Partially Achieved | Agree | The Incident Response Plan was shared with the EPPR steering Group | Agree |
| PA#5 | Partially Achieved | Agree | The Trust’s Incident Response documents contains sections on the obligations as a controller or processor of data | Agree |
| PA#6 | Partially Achieved | Agree | The Trust’s Incident Response Plan includes a list of system partners and their key contacts. | Agree |
E2.b
You have a good understanding of requirements around consent and privacy, including the common law duty of confidentiality, and use these to manage consent.
| IGP# | Trust/ICB Assessment | Internal Audit Assessment | Comment | Overall Assessment |
| A#1 | Achieved | Agree | Training is mandatory for all staff to ensure familiarity with Data Security requirements. | Agree |
| A#2 | Achieved | Agree | Policies and procedures are in place to support staff to manage consent appropriately. | Agree |
| A#3 | Achieved | Agree | Information provided to patients is clear and is shared with the public via the Trust’s website. However, some links on the website were found to be broken. | Agree |
E3.a
You lawfully and appropriately use and share information for direct care.
| IGP# | Trust/ICB Assessment | Internal Audit Assessment | Comment | Overall Assessment |
| A#1 | Achieved | Agree | Data Security Awareness – Level 1 is mandatory for all staff | Agree |
| A#2 | Achieved | Agree | Training is in place to support staff to understand what direct care is and when they should use or share information to facilitate it. | Agree |
| A#3 | Achieved | Agree | The Trust’s Confidentiality Code of Conduct Policy gives information on the sharing of data for direct care purposes. | Agree |
| A#4 | Achieved | Agree | The Trust’s data sharing policy and training is aligned with Caldicott Principle 7. | Agree |
| A#5 | Achieved | Agree | Escalation to the Information Governance Lead enables the facilitation of ad hoc data sharing. | Agree |
| A#6 | Achieved | Agree | Arrangements for the sharing of healthcare related information is documented and available to the public. | Agree |
Appendix C: Summary of work undertaken and risks reviewed – Additional outcomes
A1.a
You have effective organisational information assurance management led at board level and articulated clearly in corresponding policies.
| IGP# | Trust/ICB Assessment | Internal Audit Assessment | Comment | Overall Assessment |
| A#1 | Achieved | Agree | Policies and Procedures are owned by groups with delegated authority from Executive Management | Agree |
| A#2 | Achieved | Agree | Regular updates are provided to and discussed by the Board of Directors on Information and Security governance. | Agree |
| A#3 | Achieved | Agree | Board level individuals attend groups with accountability for Security and Governance of information | Agree |
| A#4 | Achieved | Agree | None. | Agree |
A2.b
You have gained confidence in the effectiveness of the security and governance of your technology, people, and processes relevant to your essential function(s).
| IGP# | Trust/ICB Assessment | Internal Audit Assessment | Comment | Overall Assessment |
| A#1 | Achieved | Agree | Confidence in the effectiveness of the Trust’s IT security comes from a number of different sources. | Agree |
| A#2 | Achieved | Agree | The Trust has chosen appropriate methods to gain assurance in its IT Security processes. | Agree |
| A#3 | Achieved | Agree | Independent assurance is provided through an Internal Audit program and through external organizations providing vulnerability assessments. | Agree |
| A#4 | Achieved | Agree | Deficiencies are identified through assurance activities and owned by named responsible officers | Agree |
| A#5 | Achieved | Agree | Assurance is reviewed regularly with external providers and further advice is sought from external groups such as NCSC | Agree |
B3.c
You have protected stored soft and hard copy data important to the operation of your essential function(s).
| IGP# | Trust/ICB Assessment | Internal Audit Assessment | Comment | Overall Assessment |
| PA#1 | Partially Achieved | Agree | The Trust do not transfer data to less secure systems. | Agree |
| PA#2 | Partially Achieved | Agree | Systems are in place to ensure backups and encryption protocols are in place to protect data. | Agree |
| PA#3 | Partially Achieved | Agree | Cryptographic protections, such as the use of Bitlocker are in place | Agree |
| PA#4 | Partially Achieved | Agree | Systems are in place to ensure backups of critical data. | Agree |
B3.e
Before reuse and / or disposal you appropriately sanitise devices, equipment and removable media holding data important to the operation of your essential function(s).
| IGP# | Trust/ICB Assessment | Internal Audit Assessment | Comment | Overall Assessment |
| PA#1 | Partially Achieved | Agree | Devices are disposed of by an appropriately qualified and accredited company. | Agree |
Appendix D: Audit Brief
Internal Audit Brief – Data Security and Protection Toolkit – February 2025
| Audit Objective | The objective of the review is twofold: a) to satisfy the annual requirement for an independent assessment of the Trust’s DSP Toolkit submission b) to understand and help address data security and data protection risk and identify opportunities for improvement. |
| Audit Background and Scope | Department of Health policy requires that all organisations which process NHS patient information, for whatever purpose, should provide assurance via the Data Security and Protection (DSP) Toolkit. The DSP Toolkit is an online tool that enables organisations to measure their performance against national data security and information governance standards, and to evidence this by the publication of annual self-assessments.
NHS Trusts and Integrated Care Boards, as Category 1 organisations, are subject to mandatory audit and must upload a completed audit report as part of their annual Toolkit submission. The proposed Internal Audit review will add value by providing independent assurance to the Trust Board that the organisation’s DSP Toolkit assessment is supported by sufficient evidence of compliance, and that effective controls are in place for managing data security and protection risk. The DSPT changed in September 2024 for NHS Trusts (Acute, Foundation, Ambulance and Mental Health), Integrated Care Boards, Commissioning Support Units and DHSC Arm’s Length Bodies to align with the National Cyber Security Centre’s (NCSC) Cyber Assessment Framework CAF. The review will be conducted in accordance with the national DSP audit framework, Strengthening Assurance, as updated for 2024-25. The prescribed sample of assertions for audit is published on the NHS England website at Audit News. The Reporting period is 01 July 2024 to 30 June 2025. |
| Key Risks and Counter Fraud Risks | The audit will address risks in relation to the following mandatory outcomes prescribed for the 2024-25 audit: A2.a Risk management process A4.a Supply chain B2.a Identity verification, authentication and authorisation B4.d Vulnerability management C1.a Monitoring coverage D1.a Response plan E2.b Consent E3.a Using and sharing information for direct careThe audit will also address risks in relation to the following locally selected outcomes: A1.a Board Direction A2.b Assurance B3.c Stored Data B3.e Media/equipment sanitisation |
| Methodology | Audit fieldwork will consist of: • Obtaining access to your organisation’s DSP Toolkit self-assessment • Reviewing the mandatory evidence texts that will be assessed for your organisation • Requesting and reviewing the documentation provided in relation to in-scope evidence texts • Interviewing the stakeholders who are responsible for each of the in-scope self-assessment responses • Using professional judgement and knowledge of the organisation, reviewing the operation of key technical controls using the DSP Toolkit Independent Assessment Framework. |
| Client Contacts | Carl Starbuck, Head of Information Governance Hergy Galsinh, Head of Cyber Security Andy Gleadall, Head of Network Operations Aaron Hull, Cyber Security Specialist |
| Internal Audit Contacts | Helen Higgs, Managing Director and Head of Internal Audit Jonathan Hodgson, Associate Director Bryony Harris, Senior Auditor |
| Executive Sign Off | Dawn Hanwell, Chief Financial Officer and Deputy Chief Executive |
| Committee Reporting | Audit Committee (July 2025 Committee expected) |
| Timing | Start date of fieldwork: April 2025 End date of fieldwork: May 2025 Draft report date: 15 working days from fieldwork end date Management responses: 15 working days after the draft report is issued Final report date: 5 working days from receipt of management responses |
[Data Protection: Access to and use of personal data, as required for this audit, will be managed in accordance with the Internal Audit Charter and Data Protection legislation.]
Cover sheet for Annual Health and Safety Report
- Paper title: Annual Health and Safety Report
- Date of meeting: 31 July 2025
- Presented by: Dawn Hanwell, Chief Financial Officer and Deputy Chief Executive
- Prepared by: Warren Duffy, Deputy Director of Estates and Facilities and Roland Webb, Head of Health and Safety
This paper supports the Trust’s strategic objective/s (SO):
- SO3 – We use our resources to deliver effective and sustainable services.
This paper relates to the Trust’s strategic risks (SR):
- SR5 – Adequate working and care environments
Executive summary
This annual report provides an overview to the Board of Directors of the Health and Safety position within the Trust for 2024/25. The report includes annual statistics relating to violence and aggression, RIDDORS, incidents and highlights our position on Health and Safety related training. The report provides a final position on our 24/25 Health and Safety Workplan and introduces our 25/26 Health and Safety Workplan.
Do the recommendations in this paper have any impact upon the requirements of the protected groups identified by the Equality Act? No
Recommendation
The Board of Directors are asked to accept this annual report and support the Health and Safety 2025/26 Workplan.
Health and Safety Annual Report (April 2024 – March 2025)
Contents
- 1 – Executive Summary
- 2 – Introduction
- 3 – Health and Safety Governance
- 4 – Health and Safety 2024-2025 Annual Workplan
- 5 – Health And Safety 2025 – 26 Workplan
- 6 – Violence and Aggression
- 7 – Health and Safety Incidents
- 8 – Reporting of Injuries, Diseases and Dangerous Occurrences Regulations (RIDDOR)
- 9 – Health and Safety Training Review
- 10 – Trust Risk Register
- 11 – Health and Safety Policies
- 12 – Health and Safety Audits and Inspections
- 13 – Security Management
- 14 – Fire Safety
- 15 – Other Areas of Note Relatable to Health and Safety
- 16 – Conclusion
- 17 – Recommendation
- 18 – Appendix 1 – 7 Day absences including Non RIDDOR
- 19 – Appendix 2 – Trust wide Health and Safety Incident Data 2024/25
1 – Executive Summary
This Health and Safety Annual Report will provide the Trust Board with oversight regarding the Health and Safety performance from April 2024 to March 2025. The Trust Board will also be provided with updates with the aim of providing assurance in relation to the actions that are associated with the ongoing improvement measures that are required to ensure the Trust further improves its Health and Safety position. The following points are covered within the report:
- Update progress on the 24/25 work plan and introduce the 25/26 work plan
- Trust wide Health and Safety data (Violence and Aggression, RIDDOR, Datix etc.)
- Update on our current position regarding Health and Safety Audit Programme
- Update on our current position with regards to Health and Safety compliance and training
- Provide oversight on adjacent workstreams such as Security and Fire Safety
A key point to note is that there was no follow up or new enforcement upon the Trust within the reporting period from any enforcement agency in relation to Trust Health and Safety Business.
The Health and Safety Team were appointed into post during the reporting period, and a new Estates and Facilities management team established in 2024/25 and as such it is evident that results and improvements became evident towards the Q4 period of 24/25. The team, and wider Trust, have adopted electronic systems in Contractor Management, COSHH Management and Lone Working as we look to shift towards a more effective and efficient method of working as well as developing our accessibility and evidence base for Health and Safety.
2 – Introduction
Our method of assurance and reporting has been maintained in 2024/25 in that the Health and Safey Team report primarily into the Health and Safety Committee and then into the Audit Committee, on a quarterly basis against the 2025/26 workplan.
A Quarterly Report is taken to the Health and Safety Committee and Audit Committee for review and comment. This also allows the committee authority to provide a re-focus or for the Health and Safety Team to adopt new actions or priorities to support the Trust on its corporate objectives. At the end of the year, quarterly reports will form the basis for the annual report.
Furthermore, the Health and Safety Team work across committees and groups to appraise on health and safety issues to share and adapt to learning. Groups and Committees include;
- Workforce Committee – in relation to staff Health and Safety issues and data
- Quality Committee – in relation to service user Health and Safety issues and data
- Care Services Delivery and Development Group – to support and update on service development items such as lone working
- Clinical Environments Group – to provide support and advice on a variety of environmental issues.
- Fire Safety Group – to support broader Health and Safety items where fire safety is the direct or indirect risk
This report provides an update on the current provision of Health and Safety management within Leeds and York Partnership NHS Foundation Trust (hereinafter called the Trust) including an overview of achievements and work over the April 2024 – March 2025 period and introduces the work programme for 2025/2026.
3 – Health and Safety Governance
In line with its statutory responsibilities, the Trust has a Health and Safety Committee. This committee currently meets quarterly and reports to the Audit Committee.
The Health and Safety Committee is currently joint chaired by the Deputy Chief Executive / Chief Financial Officer and Trust Staff Side; and its members include the Health and Safety Team, clinical leads and accredited Health and Safety staff side representatives. The Director of Finance / Deputy Chief Executive is the accountable officer for Health and Safety, which has been delegated by the Chief Executive. Day to day responsibility for the Health and Safety programme is delegated to the Deputy Director of Estates and Facilities in conjunction with the Health and Safety team.
The Health and Safety Committee receives several reports throughout the year on key Health and Safety risks including RIDDOR, Manual Handling, Fire, Security and Violence and Aggression. These reports are scrutinised by the committee to identify any trends that are developing and action plans put in place for improvements.
The Deputy Chief Executive / Chief Finance Officer and the Deputy Director of Estates and Facilities are also members of the Audit Committee thereby ensuring that Health and Safety risks are considered as appropriate in the wider risk mix, and that risks identified in the wider organisational risk assessment processes are formally and quickly brought within the Health and Safety remit.
The Health and Safety Team will continue to play a key role in ensuring management systems are reviewed and all activities are managed appropriately to ensure compliance, but this does not mean Health and Safety is directly their responsibility within the organisation. All members of trust staff within the organisation need to continue playing their part in ensuring Health and Safety is key in all areas of work activity.
4 – Health and Safety 2024-2025 Annual Workplan
The Health and Safety Team were fully established into post by Q2 of 2024/25 after the previous team had left the Trust. The new team had inherited the workplan in-year and prioritised to close out the actions that had been set by the previous team. The Health and Safety Team, working closely with multiple stakeholders, had a successful Q3 to Q4 in stabilising the work plan and getting some of the key items progressed.
Table 1 24/25 Health and Safety Annual Plan progress
| Item | Owner | Q2 Status | Q3 Status | Q4 Status |
| A further review of the Health and Safety Committee Terms of Reference, standing agenda, frequency of papers and workstreams. | RW | Green | Green | Green |
| Continuing the role out of the SYPOL COSHH system, which is a fully integrated management system for compliance with COSHH Regulations | RW | Amber | Amber | Green |
| Reporting of Injuries, Diseases and Dangerous Occurrences Regulations (2013); updating the process of reporting notifiable incidents to ensure concise and relevant detail is provided to the HSE within legislative time limits. Reviewing current risk assessment templates available Trust wide; this was a priority in 2024/25. For example, support the clinical services for with violence and aggression risk assessments. | RW | Amber | Amber | Amber |
| Develop Partnership working with statutory bodies, primarily with the Health and Safety Executive to demonstrate the Trust’s commitment to Health and Safety and to learn and understand from the HSE’s perspective measures expected to keep stakeholders as safe as reasonably practicable | RW | Green | Green | Green |
| Develop Trust Liaison with Regional Trusts; to enable the sharing of best practice, learning from incidents and to ensure LYPFT matches, if not exceeds the regional approach to Health and Safety issues | RW | Green | Green | Green |
| Improve membership attendance at the quarterly Health and Safety Committee – there were 4 successful meetings in 2023/24 but it was identified that the committee would benefit from regular attendance of specialists with a pivotal role in supporting the Trust’s Health and Safety Agenda | RW | Amber | Green | Green |
| Ensure all policies and procedures are comprehensively reviewed and updated accordingly and in a timely manner | RW | Amber | Green | Green |
| Ensure the Health and Safety audit schedule is reviewed, amended accordingly, and completed by the end of 24/25 | RW | Amber | Amber | Green |
| Provide comprehensive assessment of the Workplace Standards and if this is to be replaced, identify suitable robust assurance mechanism for Health and Safety | RW | Red | Amber | Amber |
| Review current risk assessment templates available Trust wide; this was a priority in 2024/25. For example, supporting clinical services with violence and aggression risk assessments | RW | Amber | Amber | Green |
Below is supporting narrative around the progress against the actions on our 24/25 annual plan included:
- The review of the Health and Safety Committee Terms of Reference, standing agenda, frequency of papers and workstreams were presented at the October Health and Safety Committee meeting and finally adopted in January 2025
- Continuing the SYPOL COSHH system rollout. This is a fully integrated management system for compliance with COSHH Regulations. The Trust quickly superseded the initial allocation of 50 assessments during Q4 of 2024/25 and an updated order submitted to support further development
- Progress on updating the process of Reporting of Injuries, Diseases and Dangerous Occurrences Regulations (2013) continued to ensure concise and relevant detail is provided to the HSE within legislative time limits will be achieved moving forward. The refreshed procedure was widely sent for comment in Q4 2024/25, with the aim of being approved in Q1 25/26
- The Health and Safety audit schedule was reviewed and amended accordingly.
- Health and Safety Audits – 46 sites were audited with monitoring and reporting established
- Internal Partnership working with the Professional Lead Nurse, Infection Prevention and Control and Procurement to improve procedures on supply and use of syringes and needles to reflect our legal obligations under The Health and Safety (Sharp Instruments in Healthcare) Regulations 2013, enforced by the Health and Safety Executive.
- External Partnership working with Spectrum Healthcare CiC; The Trust Health and Safety Team have also entered a prestigious commercial partnership with Spectrum Healthcare CiC to provide Health, Safety and Environmental support to the company, this partnership providing a modest revenue stream to the Trust
5 – Health And Safety 2025 – 26 Workplan
A Health and Safety workplan has been devised for 2025/26, designed to ensure this builds further on the existing systems and processes in place currently and continuing residual actions from the the 24/25 Annual Work Plan. This includes developing and building upon links with directorate leads, strengthening links with other services, such as Occupational Health, Sexual Safety, Violence and Aggression and Operational Managers. Our workplan in 2025/26 is derived from audit findings, themes raised at various meetings, areas where we have identified where improved efficiencies can result in improved health and safety outcomes, and ensuring we are demonstrating our continued efforts to comply with UK Legislation and emerging themes from the Health and Safety Executive. The 2025/26 workplan is shown below in Table 2.
Table 2 25/26 Health and Safety Annual Work Plan
| Priority Area | How will we do this | Action Owner |
| Health and Safety Committee | Refinement of the Health and Safety Committee Terms of Reference, standing agenda, frequency of papers and workstreams and undertake an effectiveness review. | Head of Health and Safety |
| Health and Safety Software (COSHH, Lone Working and CDM Regulations) | Continue role out of the Sypol COSHH system, which is a full management system for compliance with COSHH Regulations (as referred to in the 2024-25 programme). Further develop the Lone Worker System working with clinical staff across the trust to ensure we offer an improved personal safety function. Develop the “RESET” control of contractor solution to fulfil duties under CDM2015 and our wider control of contractor responsibilities. | Head of Health and Safety |
| RIDDOR Reporting | Reporting of Injuries, Diseases and Dangerous Occurrences Regulations (2013); update the Policy to assist with the reporting of notifiable incidents to ensure concise and relevant detail is provided to the HSE within legislative time limits and improves Trust data. | Head of Health and Safety |
| Risk Assessments | Review current risk assessment templates available Trust wide; this will be a priority in 2025/26. For example, support the clinical services for with violence and aggression risk assessments. | Head of Health and Safety |
| Trust Risk Register | Ensure that any items that are of risk are suitably recorded on the Trust risk register and provide supporting mitigation for assurance as per the Trusts Risk management Procedure | Head of Health and Safety |
| Collaboration and Partnership working | Develop Partnership working with statutory bodies, primarily with the Health and Safety Executive to demonstrate the Trust’s commitment to Health and Safety and to learn and understand from the HSE’s perspective measures expected to keep stakeholders as safe as reasonably practicable. Develop Trust liaison with Regional Trusts; to enable the sharing of best practice, learning from incidents and to ensure LYPFT matches, if not exceeds the Regional approach to Health and Safety issues | Head of Health and Safety |
| Health and Safety Compliance and Mandatory Training | Work with relevant service leads and provide more regular (quarterly) on progress and use governance framework to suitably escalate where required. Continue to support all services with Health and Safety related training. | Head of Health and Safety |
| Policies and Procedures | Ensure that all Health and Safety relevant Policies and Procedures and reviewed and managed accordingly within the next reporting period | Head of Health and Safety |
| Trust Wide Reporting (Health and Safety Incident Data) | Work with relevant senior leads to ensure our Audit, Quality and Workforce Committees are suitably appraised with clear, timely, and accurate data – where each committee is presented with data that is applicable to its terms of reference and ensure the data is supported by definitions and supporting narrative and reasons. | Head of Health and Safety |
As in 2024/25 we will report progress on a quarterly basis to the Audit Committee and Health and Safety Committee respectively.
6 – Violence and Aggression
The Trust carries out its duties for Violence and Aggression in accordance with directives from the Health and Safety Executive as well as UK legislation. NHS Employers have a duty to protect the health, safety and welfare of staff under the 1974 Health and Safety at Work Act. This includes assessing the risk of violence and taking steps to reduce it as required under the Management of Health and Safety at Work Regulations 1999.
The Health and Safety Executive (HSE) defines violence at work as:
“Any incident in which an employee is abused, threatened or assaulted in circumstances relating to their work”. This covers the serious or persistent use of verbal abuse, which the HSE say, “can add to stress or anxiety, thereby damaging an employee’s health”.
It also covers our people assaulted or abused outside their place of work, for example, while working in the community, when the incident relates to their work. It is these directives and definitions that help the Trust in constructing its strategic aims in relation to Violence and Aggression.
6.1 – Violence and Aggression LYPFT Strategic Aims
In considering the vision and the above HSE definition, our Trust objectives for Violence Prevention and Reduction are as follows:
- To create a safer working environment and ensure good practice is replicated Trust wide.
- To encourage the reporting of incidents, by achieving a consistent process so that our colleagues feel that reporting is worthwhile.
- Reduce the number, severity and occasions of incidents of violence and incidents of hate in the Trust.
- Reduce colleague on colleague violence and incidents of hate and strive to become an “anti-hate” organisation.
- Actively work to eradicate any unwanted, inappropriate and/or harmful sexual behaviours towards our people.
- Reduce colleague time lost and absences resulting from violent incidents, incidents of hate and unwanted, inappropriate and/or harmful sexual behaviours.
- Ensuring an effective, proactive and supportive wellbeing and critical incident support pathway following violence and incidents of hate and unwanted, inappropriate and/or harmful sexual behaviours
- Ensure adequate support for those engaging with the criminal justice system.
- Develop and embed an engagement, awareness and communication programme alongside these objectives.
Progress with the Strategic Aims will also include measurement against the National Staff Survey results. The Staff Survey is a critical piece of research into how employees feel about working at LYPFT, including safety and shall continue to be monitored through the Violence Prevention Group.
6.2 – Violence and Aggression incidents involving staff
Leeds and York Partnership Foundation Trust is committed to reducing violence towards our staff, as identified within Our People Plan, under the strategic priority of “Belonging in the NHS”. This supports the overall NHS People Plan promise to prevent violence, so that “staff should never be fearful or apprehensive about coming to work”. This demonstrates our commitment to the health and wellbeing of colleagues, as well as recognising the negative impact that poor health and wellbeing can have on service user care.
During the reporting period, 3421 reports of violence and aggression, threats and abuse during 24/25 that staff were exposed to. Whilst this years figure is 4.5% lower based on the three-year average, this masks Violence/assault (Staff) analysis indicating a stubborn, high rate of incidents.
Table 3. 2024/25 Staff only Violence and Aggression total data
| Violence and Aggression Category Summary | Totals (2024/25) | (2023/24) | (2022/23) | Three Year Average |
| Violence/assault | 1381 | 1513 | 1587 | 1494 |
| Violence (Staff) | 1171 | 1114 | 1322 | 1202 |
| Verbal/written abuse (staff) | 539 | 491 | 657 | 562 |
| Verbal Abuse | 236 | 239 | 240 | 238 |
| Violence (Public) | 69 | 73 | 58 | 67 |
| Verbal abuse (Public) | 25 | 13 | 14 | 17 |
| Total | 3421 | 3443 | 3878 | 3581 |
Incidents of violence and aggression, threats and abuse are wide ranging in nature from perceived low-level threats to serious assaults. Incidents affect not only immediate staff, but the wider services and can have cumulative as well long-term impacts on staff. Even when incidents do not result in staff absences from physical injuries or trauma, the safety team are cognisant of the impact and a valuable resource in supporting services dealing with the issue.
The Safety Team advocate reporting of most incidents to the police. The Deputy Director of Estates and Facilities and Head of Health and Safety now regularly attend Workforce and Quality Committees to support separate work stream improvements addressing causes, impacts and aims to reduce incidences of Violence and Aggression affecting both staff and service users.
The national Violence Prevention and Reduction (VPR) standard complements existing health and safety legislation and is a data-driven method focusing on colleague health and wellbeing, in a way that is reflective, proactive, preventative, responsible and accountable. All NHS-funded services operating under the NHS standard contract are required to review and self-assess their status against the VPR standard twice a year and provide Board assurance. Performance is to be measured against the standard, as well as the Trust’s overall VPR Strategy.
The VPR Strategy was approved by the Board in January 2024, as well as our self-assessment against the VPR standard. The VPR Strategy outlines our vision, intent, objectives and organisational functions and responsibilities in delivering the VPR standard and is supported by a policy which was also approved by the Policies and procedures group in March 2024. Both the Strategy and the Policy has been written collaboratively and incorporate recent Trust workforce priorities on incidents of hate and domestic violence and sexual safety. It also details the wellbeing support and the established critical incident support, which is provided following any violent incidents. The implementation of the VPR Strategy and Policy will be led and monitored from within the Violence and Reduction Steering Group, but receive input from other groups, as detailed in the Strategy. The delivery and impact of this Strategy will be monitored and part of achieving the standard requires reporting to the Board twice a year, and delivered through the Quality Committee.
6.3 Violence and Aggression incidents involving service users
The NHS defines violence and aggression in the context of service user and visitor behaviour towards staff using two main categories:
- Physical Assault as “Any act where a person intentionally or recklessly causes another to suffer or apprehend immediate unlawful violence”. and includes hitting, kicking, biting, or any other form of physical attack.
- Non-Physical Assault that refers to “verbal abuse, threats, or other intimidating behaviour causing someone to fear for their safety or well-being, even where no physical contact occurs
These definitions are aligned with legal standards such as the Criminal Justice Act 1988 and are used across the NHS to guide policies and procedures for managing and preventing such incidents.
Service user on service user violence and aggression within the Trust is measured where one service user exhibits physically or verbally aggressive behaviour towards another service user.
NHS guidance categorises physical assault as an “Any act where a service user intentionally or recklessly causes another service user to suffer physical harm or fear of harm.”
Non-Physical Assault: Includes verbal abuse, threats, intimidation, or harassment that causes distress or fear.
These incidents are managed under the NHS Violence Prevention and Reduction Standard (VPRR), which provides a risk-based framework to ensure safety for all individuals in NHS care settings, including service users that the Trust is embracing. The Trust maintains committed to ensuring processes are in place to ensure that we are demonstrating as much as is reasonably practicable to minimise violence and aggression incidents. During 2024/2025, a total of 1621 incidents were reported on the DATIX reporting system, with 85% (1384) attributed to violence/assault and of those, 93.78% (1298) reported in four Care Groups;
Table 4. 24/25 Service User Violence and Aggression total data
| Patient Reported Violence and aggression | Verbal Abuse | Violence/assault | Total |
| Adult Acute Services | 68 | 524 | 592 |
| Older Peoples Services | 42 | 437 | 479 |
| Children and Young People Services | 38 | 204 | 242 |
| Forensic Services | 44 | 133 | 177 |
| Learning Disability Services | 13 | 31 | 44 |
| Eating Disorders and Rehabilitation Services | 24 | 19 | 43 |
| Community and Wellbeing Services | 3 | 21 | 24 |
| Regional and Specialist Services | 5 | 9 | 14 |
| Liaison and Perinatal Services | 0 | 6 | 6 |
| Total | 237 | 1384 | 1621 |
This data will be primarily managed at the Violence and Aggression Group where plans will be put in place to further review detail and trends. The data is 24/25 is coherent with data in previous years where Adult Acute services remaining an area of highest incidents. Data will inform the workplans of other groups and Health and Safety Team (and supported by the Security Manager) will continue to offer support with the Violence and Reduction lead in the Trust.
The work at this group will report into the respective Audit, Quality and Workforce Committees.
7 – Health and Safety Incidents
In 2024/25 there was a total of 6086 incidents attributable to ‘Health and Safety’ reported via Datix. We introduced this level of reporting into our quarterly reports in 2024/25 and these incident numbers capture the following categories;
- Incidents affecting patients – 3141 incidents
- Incident affecting staff – 1987 incidents
- Incident affecting organisation – 851 incidents
- Incident affecting visitor / contractor / member of the public – 107 incidents
N.B Some of the data cross references against the Violence and Aggression Data
The areas across the Estate that carry most of the incidents continue to be Adult Acute, Older Persons Service and Forensic Services but are closely followed by Children and Young Persons.
The three-year review of data for Health and Safety Incident Data is shown as;
Table 5. 3-year review of Health and Safety Incident Data
| 2022/23 | 2023/24 | 2024/25 | Three Year Average |
| 6498 | 6004 | 6086 | 6196 |
2024/25 total incident numbers show that we had 82 more incidents than the previous year, but we are under the three-year average for total number of incidents. The information we do have, especially regarding ‘Health and Safety/ and ‘Slips Trips and Falls’ will also dictate some of our Audit Programme in that we will inspect regularly until assured that measures are in place to control incident occurrences.
Data quality and data definition need to improve. A priority item for the 2025/26 workplan is to provide improved reporting across committees to be clear on data and to be indicative of where the problematic areas currently reside and to provide services leads relevant, accurate information to be able to make Health and Safety (and adjoining workstream), improvements. The Health and Safety Team will work with clinical, and workforce leads and report back to the Audit Committee throughout 2025/26 to ensure that we provide the information that will provide the most assurance, accompanied by workplans. Appendix 2 provides a table for the Trust wide Health and Safety Incident Data 2024/25.
8 – Reporting of Injuries, Diseases and Dangerous Occurrences Regulations (RIDDOR)
The Trust accepts that the Reporting of Injuries, Diseases and Dangerous Occurrences Regulations 2013 places a duty on it as an employer to ensure compliance with legislation and to ensure the health and safety of our employees, service users, clients, residents and visitors who may come into contact with our services. Reporting of Injuries, Diseases and Dangerous Occurrences Regulations 2013 (RIDDOR), is enforced by the Health and Safety Executive (HSE), who also share intelligence of reports with the CQC.
During the reporting period the Trust was required to report 9 incidents to the Health and Safety Executive under the provision of RIDDOR (Reporting of Injuries, Diseases and Dangerous Occurrences 2013). Overall, there has been a slight decrease in the number of RIDDOR incidents reported to the HSE over the previous year (10 in the previous year);
Table 6. Three Year RIDDOR Notifications in LYPFT
| 22/23 RIDDORS | 23/24 RIDDORS | 24/25 RIDDORS |
| 24 | 10 | 9 |
There have been no incident investigations by the Health and Safety Executive or Care Quality Commission in relation to these incidents.
All incidents are reported through the online Datix incident management system and are investigated by the Line Manager concerned and appropriate action taken to reduce the risk of re-occurrence. This data and the insight into where, will allow The Health and Safety Team to carry out a deeper diver and work with the services accordingly, as well as work with other key stakeholders such as Violence and Aggression Leads and The PFI Special Purpose Vehicle. The Health and Safety Team automatically receive all copies of staff accident and incidents that are reported and depending on the severity of the accident/incident will undertake a full investigation in conjunction with the manager concerned.
Appendix 1 highlights the areas of the incidents and also includes over 7 day absences where RIDDORS are not required.
9 – Health and Safety Training Review
Overall, training compliance has improved from 23/24 with an increase of 5% to 87% compliant, combined across all areas.
Wherever compliance appears to be sub-optimal, the Health and Safety Team will work and support colleagues with individual responsibilities to ensure that the Trust continues to strengthen the “Safe People, Safe Place” agenda.
Health and Safety training has been refreshed and reviewed over the year to ensure it is up to date, meets statutory compliance and is accessible to all staff groups. Health and Safety training is mandatory every 3 years, and the Trust remains aligned to the National e-learning programme for this training.
In terms of overall compliance, the Learning Management Team have advised that significant consideration should still be given concerning ripple effects from the pandemic (e.g. extended periods of social distancing that affected class sizes) and the measures taken by senior staff (i.e. extending refresher periods of training by 6 months). These have taken considerable time to reverse but progress is actively being monitored.
There are still some areas that need improving and we continue to develop links across the Trust to support accordingly. Our 24/25 position is shown in Table 7;
Table 7 2024/25 Overall Training Compliance for Health and Safety
| Requirement | Number compliant | Number non-compliant | Total Headcount | Compliance status | 23/24 |
| Low Level Physical Interventions with PSTS and Breakaway Skills | 65 | 48 | 113 | 58% | 72% |
| Moving and Handling Advanced (LD) | 116 | 74 | 190 | 61% | 55% |
| Food Safety Level 2 | 508 | 204 | 712 | 71% | 71% |
| Moving and Handling Advanced (OPS) | 178 | 68 | 246 | 72% | 63% |
| Intermediate Level Physical Interventions with PSTS and Breakaway Skills | 148 | 36 | 184 | 80% | 73% |
| Personal Safety with Breakaway Skills | 1116 | 239 | 1355 | 82% | 78% |
| Food Safety Level 1 | 278 | 51 | 329 | 84% | 88% |
| High Level Physical Interventions with PSTS and Breakaway Skills | 470 | 86 | 556 | 85% | 85% |
| Personal Safety Theory | 615 | 105 | 720 | 85% | 92% |
| Display Screen Equipment | 1814 | 282 | 2096 | 87% | 85% |
| Moving and Handling Essentials | 610 | 95 | 705 | 87% | 79% |
| Moving and Handling Principles | 1795 | 164 | 1959 | 92% | 89% |
| Health and Safety | 2976 | 133 | 3109 | 96% | 95% |
| Overall: | 10689 | 1585 | 12274 | 87% | 82% |
Training will be monitored further at the Health and Safety Committee. During 2024/25, the Health and Safety Team have developed relationships to help teams improve their compliance levels and have had sessions with the Compulsory Training Team to build up the compliance with their support.
10 – Trust Risk Register
Any Health and Safety risks are added to the Trust Risk Register on Datix. Future work is required to ensure that all Health and Safety risks are captured including at a local level. The position continues to improve but further work is required to fully embed this – we will embed this into the Audit Programme to ensure areas assessed or deemed high risk from a Health and Safety Perspective, have suitable risk/governance arrangements in place and mitigating actions.
11 – Health and Safety Policies
Health and Safety policies have been developed or reviewed over the reporting period. As with all Health and Safety policies and associated procedures, these are considered live documents, so that even when review dates are published, these may be subject to an earlier review when this is necessary.
Policies and Procedures due for developing and for review or update during 25/26 will include:-
Table 8 Health and Safety Policies to be reviewed and updated during 25/26
| Policy/Procedure | Status |
| Trust Health and Safety Policy | Policy/procedure to be reviewed |
| RIDDOR Notifications | New policy/procedure |
| DSE Policy | Policy/procedure to be reviewed |
| Contractors Health and Safety Procedure | Policy/procedure to be reviewed |
| Permit to Work Procedure | Policy/procedure to be reviewed |
| Review of Third Party Risk Assessments | Policy/procedure to be reviewed |
| Safe Systems of Work Procedure | Policy/procedure to be reviewed |
| Health and Safety Inspections and Audits Procedure | Policy/procedure to be reviewed |
The Trust Health and Safety Policy and RIDDOR policy have been progressed in 2024/25 and Q1-Q2 of 25/26 will see these policies updated and signed off accordingly.
12 – Health and Safety Audits and Inspections
46 Health and Safety Audits were completed during the reporting period, which is in keeping with previous reporting periods. Our audits provided findings that have created actions for us to record and monitor accordingly, with a view to closing out and improve our health and safety provision on the estate.
Table 9. Year-end position for outstanding actions from the Health and Safety Audits programme
Health and Safety audit actions – Outstanding Actions
| Month and year | Apr-24 | May-24 | Jun-24 | Jul-24 | Aug-24 | Sep-24 | Oct-24 | Nov-24 | Dec-24 | Jan-25 | Feb-25 | Mar-25 |
| Total | 55 | 45 | 45 | 33 | 28 | 30 | 30 | 30 | 30 | 34 | 34 | 37 |
The trends through the year and year end position would suggest that the following areas are mainly picked up during audits;
- DSE Self-assessments by clinical staff – this will be further supported with a revised, updated policy in 25/26
- Control of Substances Hazardous to Health (COSHH) assessments – this will be further developed and supported with the further role out of the Trusts Sypol system
- First Aid – an improvement will be needed in areas for identifying responsible persons and implementing local procedures
A review of the inspection and audit process had been proposed to ensure that staff within clinical/non-clinical areas undertake the responsibility for completing these audits themselves as even with the current resource this is a huge undertaking for these audits to be completed by the Health and Safety team on an annual basis. This approach is in line with generally expected legal requirements for managers and supervisors.
The Trust approach to audits and inspections will be reviewed further during 25/26 to ensure that these remain to be proactive and fit for purpose. From this proposal a key area of work is to undertake central validation work to check and verify the reported compliance. This will involve a member of the Health and Safety team going into areas to check that the reported evidence is in place including examination of management systems, risk assessments and delivery of any mitigating action plans.
Audit issues are addressed structurally for assurance through Site meetings and various groups, i.e. Clinical Environment Group, Estates Steering Group and Health and Safety Committee.
Health and Safety issues that cannot be resolved immediately will be risk assessed and as appropriate put onto the trust risk register.
13 – Security Management
13.1 – General Healthcare Security update
LYPFT engage with multiple organisations to ensure knowledge is shared and best practice adopted in relation to ongoing security matters across the country.
The Trust Security Manager is an active member of NAHS (National association for Healthcare Security) and attends the National performance advisory group where such best practices are shared and debated.
The Terrorism (Protection of Premises) Act 2025, also known as Martyn’s Law, received Royal Assent on Thursday 3 April 2025. This Act delivers the Government’s manifesto commitment to strengthen the security of public premises and events.
The Government intends for there to be an implementation period of at least 24 months before the Act comes into force. This will allow the SIA’s new function to be established, whilst ensuring those responsible for premises and events in scope have sufficient time to understand their new obligations. This will enable them to plan and prepare appropriately
13.1 – Security Review
A previous Security review was carried out in the Trust and there are 2 outstanding actions and one that is partially complete.
Table 10 25/26 Security Objective Year 3 Summary (2024/2025)
| Objective Year 2 (2023/2024) | Target Date | Status |
| Provide feedback to the Exec lead for which security staffing option is the preferred outcome | July 2025 | Ongoing |
| Review contract arrangements with Mitie Security | July 2025 | Ongoing |
| Complete 1/3 of security upgrades (approximately 5 sites) | April 2025 (Phase 1) | Partially complete |
| Complete redevelopment of security control room | February 2025 | Complete |
In 25/26 Q1 the ‘ongoing’ actions will be further developed, and an option appraisal will be explored further to establish our preferred operating model moving forwards. It is anticipated this will be resolved in Q2-3 of 25/26. These actions were also captured as part of the Audit Yorkshire report – and as such, we will monitor progress of these actions through that mechanism to avoid duplication.
We have significantly invested in our Security Infrastructure (CCTV, Access Control, Control Room) and we have developed plans to roll out our next phases – this will however be subject to capital availability and Trust processes for business case approval.
13.2 – Audit Yorkshire Internal Review / HSE recommendations.
Security Management was audited in 2023/24 and gave an overall opinion of Low Assurance on the Trust’s arrangements for managing Security.
Extensive work was put in place and a re-audit has provided an appraisal of Significant Assurance has been provided on the implementation of recommendations made in the previous Security Management internal audit report.
The previous audit raised 27 recommendations, of which 15 have been assessed as fully implemented. The remaining have been replaced by eight further recommendations. Although there is ongoing action to address identified gaps, evidence was available that all actions have been concluded, and the Trust is now moving to embed the outcomes from the initial response to the Security Management audit.
Of the outstanding actions in Table 11, one is linked to our staffing model moving forwards as highlighted in multiple reports;
Table 11 25/26 Security Audit Yorkshire Internal Review / HSE recommendations
| Action | Owner | Audit Yorkshire score | Proposed completion date |
| The Trust should complete the current review of security management, and confirm if additional resource needs to be requested, in a timely manner. | Security Manager | Moderate | 30/09/2025 |
| External Partnerships; The Trust should document when and how it will engage with external partners for security matters, including who should be involved and how the Trust’s involvement will be recorded. | Security Manager | Moderate | 01/06/2025 |
13.3 – Policy and Procedure update
This section will provide assurance in that policies are being regularly reviewed at and that there is a pro-active culture towards Policies and Procedures for Security Management. The Policies and Procedures that are applicable to Estates and Facilities Security Management is as followed.
Table 12 25/26 Security Related Policy and Procedure Reviews
| Document Number | Title | Owner | In Date? | Expires on |
| FE-0018 | Security Management Policy | Security Manager | Yes | 19/03/2026 |
| FE-0021 | Access Control Procedure | Security Manager | Yes | 28/10/2026 |
| FE-0025 | CCTV operating procedure | Security Manager | Yes | 28/10/2026 |
| FE-0019 | Lone working procedure | Operations Manager | Yes | 25/06/2026 |
| FE-0020 | Lockdown procedure | Security Manager | Yes | 31/07/2025 |
| None | Responsible Car Parking Policy | Security Manager | None | None |
Plans are already in place for FE-0020 – Lockdown Procedure, with a collaborative approach being undertaken by Estates and Facilities, Operations and Emergency Planning Teams.
13.4 – Security Risk Assessment Schedule
These risk assessments focus on the environmental and security infrastructure on sites. Further assessments are required on clinical/departmental basis to provide a more wholistic view of security arrangements Trust-wide. The following table highlights the risk assessment work schedule which is currently 94% compliant which is a 29% improvement. Risk assessment actions are now being worked through and a recurring plan devised to repeat on a 2 yearly basis or following significant incident/cause for review. Parkside Lodge remains the only primary assessment left for completion. This will be done following the planned works at this site.
Security Risk Assessments will generally be done two yearly – or more frequently subject to findings. 2025/26 will see the start of the Clinical Security Risk Assessment work and program so we can assess beyond our infrastructure.
13.5 Risk Assessment actions and KPIs
All actions from Risk Assessments will be monitored at the Site Meetings in the first instance. Common themes across sites will be grouped together with a costed action plan and assessed for capital funding if required.
KPIs are to be reported through the site meetings, into Clinical Environment Group with monthly reviews taking place to progress actions.
Actions that have been identified from the Security Risk Assessments are shown in a high-level basis and are shown in Table 13;
Table13 24/25 Security Related Risk Assessment Security Risk Assessment Actions – Outstanding Actions
| Date and Year | Jul-24 | Aug-24 | Sep-24 | Oct-24 | Nov-24 | Dec-24 | Jan-25 | Feb-25 | Mar-25 |
| Total across sites | 28 | 149 | 216 | 258 | 240 | 261 | 261 | 239 | 239 |
Common themes identified across the 2024/25 Security Risk Assessments are;
- Access control system management and audit
- Site Alarms – no alarms in place for community / outpatient sites
- Staff awareness of lockdown procedures
- Key Management arrangements on site
These themes and findings are currently ongoing with a view to being resolved or further scrutinized through Q1-Q2 and remain part of the regular update to the Estates Steering Group and Health and Safety Committee.
13.6 – Trust-Wide Car parking
Car parking remains problematic, especially at sites such as Becklin Centre and Newsam Centre.
There are options available to the Trust for improved solutions across all sites, but these come with cost and resource requirements, as well as a significant shift in how we manage car parks and will need a top-down support function to deliver. There are identified co-benefits with one of the Security Management model options and this is to be explored further in 2025/26.
The Trust does have a Responsible Car Parking Policy which has not been developed since COVID – this shall also be a priority in 2025/26 as to provide guidance and instruction for improved car parking across the estate.
13.7 – Key Management
The completed risk assessments consistently indicate that key management is a risk across our sites. Currently, there is no standardised process for issuing and recording physical keys for staff and contractors. Additionally, there are inconsistent asset registers, and sites are unaware of the number of keys they possess, should possess, or their current locations. Key cabinets have been found left open and unattended, or closed with the key still in the lock, allowing easy access. To address this issue, a key management procedure with site-specific instructions is necessary.
Each site must compile an asset list documenting the keys they hold and their usage. This list will be paired with a uniform sign-in/sign-out sheet, which must be countersigned by authorised individuals when issuing and returning the keys. Further audits will be required, and this implementation will require operational security staff.
A proposed solution will be communicated and published through site team meetings and taken to ESG for approval in 2025, detailing the associated risk implications and a timescale for resolution.
14 – Fire Safety
Our Fire Safety provision continues to be provided by Leeds Teaching Hospital Trust under an SLA which is managed by the Estates and Facilities Department. The Fire Safety Team continue to provide services in-line with legislation and guidance for Fire Safety as outlined in HTM05 : Fire code. The Fire Safety workplan encompasses these main items;
- Fire Risk Assessments
- Fire Risk Assessment findings and actions
- Fire Safety Training
- Fire Safety Drills
- Fire Evacuation Plans
- Support on the closure of the Independent Authorising Engineer Fire Audit
- Fire Safety Group (providing the monthly fire safety report)
- Collaborate and maintain relationships with the West Yorkshire Fire Service
- Contributing to NHS Estates statutory returns such as Premises Assurance Model (PAM) and Estates Return Information Collection (ERIC)
- Development of the Trust Fire Safety Policy and associated procedures
In the previous reporting period of the Premises Assurance Model (September 2024), Fire Safety was the strongest performer in Estates and Facilities based on the evidence and review of its offering, with minimal actions needs to be able to score ourselves an ‘Outstanding’ score.
The Trusts Fire Safety Group convenes monthly and receives assurance and provides instruction for any actions that are required. This group is overseen by the Trusts Health and Safety Committee where the Trust Fire Engineer or Fire Officer provides a quarterly report based on all activities as prescribed under the Service Level Agreement. We currently score ‘good’ for Fire Safety.
14.1 – Fire Safety Successes and Challenges
Key successes of note for Fire Safety in LYPFT in 2024/25 include;
- 100% Completion of Fire Risk Assessments where LYPFT are responsible to complete the task
- Transformation of mandatory training from online to face to face – ward specific training and development of a streamlined, less complex training package
- Development of Protocols to reflect recent challenges and how, as a trust we can manage fire safety better (i.e use of air fryers, vaping challenges, e-bike / e-scooter usage)
Key challenges of note for Fire Safety in LYPFT in 2024/25 include;
- There are 752 actions for fire safety that have been identified in Fire Risk Assessments
- Smoking challenges – there has been multiple issues, incidents and ongoing risks which is addressed further in 13.2 Ongoing Fire Safety Risks
- PFI Fire Safety
14.2 – Ongoing Fire Safety Risks
As reported, a challenge that have further developed in the Trust in 24/25 has been the increase in incidents in relation to smoking / vaping, especially within in-patient areas. It is acknowledged that smoking / vaping in hospitals is a complex challenge from multiple perspectives, and we also understand that there are links between smoking, fires and violence and aggression.
Figure A. Fire activations in 24/25 – cause of activations
Figure 1 highlights the number of activations in 24/25 which stands at 111 across the Estate. 43 or 39% of these activations are smoking related. In 24/25 we had 19 fires of which none of these caused significant damage or harm. We also had 19 alarm activations that were caused without reason by service users and / or members of the public.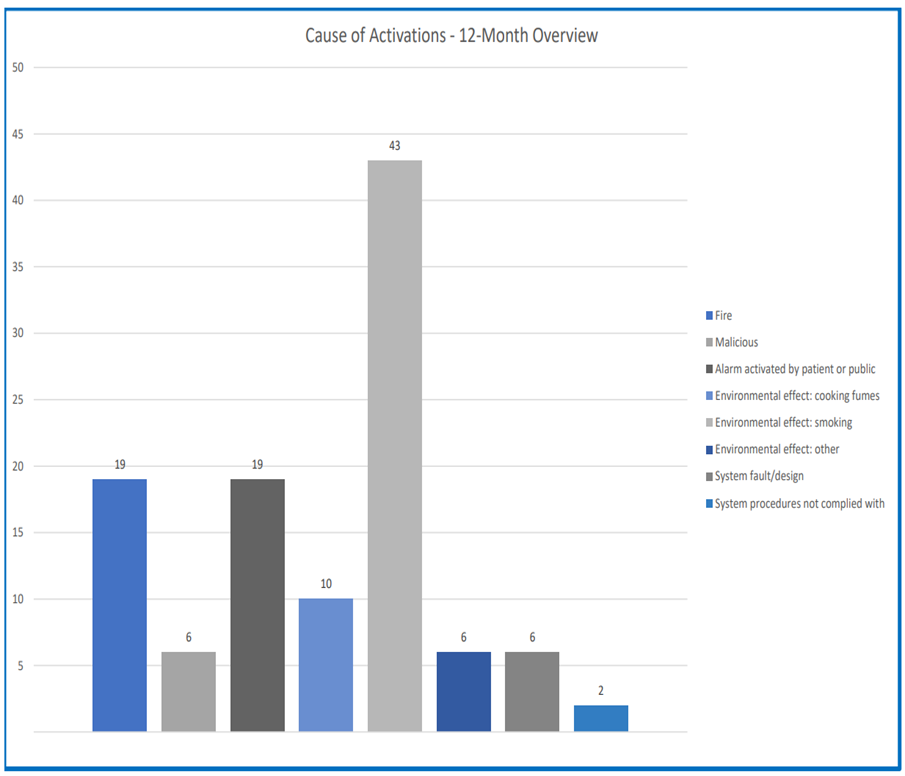
For context, each alarm activation typically automatically alerts the West Yorkshire Fire Service who dispatch a fire response team, unless advised otherwise. Each response from the fire service can be costed by the fire service and the Trust can be invoiced c.£600.00 per attendance. Further, we should always remain cognisant of the disruption these scenario’s cause, service user distress, clinical resource requirements and additional cost and resource impact of Estates and Facilities having to attend to reset fire and engineering systems. Avoiding a large financial penalty in 24/25 was only achieved due to the ongoing strong relationships between the Fire Safety Team and the West Yorkshire Fire Service, although this should not be relied upon in future.
The data, provided via Datix, shows that Newsam Centre remains a key area for concern.
Figure B. Location of Fire Alarm Activations across the Estate
2 shows the areas of high concern for where there are high volume of activations. The Becklin Centre and the Newsam Centre respectively contribute significantly to Fire Alarm activations, these sites are closely followed by Asket Croft.

A further analysis of the data has shown that in this reporting period the theme around smoking and the challenge of managing smoking is further exacerbated by the data shown in Figure 3, highlighting the number of incidents caused by smoking.
One of our major challenges is in relation to smoking. In 24/25 we had 320 reported incidents in relation to smoking. However, based on findings from risk assessments and other data and intelligence, we suspect that this is under reported. Asket Croft and the Newsam Centre were our highest number of offending areas where an incident occurred because of smoking.
Figure C. Smoking Incidents across the Trust Estate in 24/25

In 25/26, Estates and Facilities will utilise Trust Governance and seek support from Clinical and Operational colleagues to identify solutions and other risk mitigation requirements to ensure that we improve our fire safety position. On the advice of the Fire Safety Team, smoking is the biggest fire safety concern in the Trust.
14.4 – Fire Safety Training
Fire Safety Training is undergoing changes both from a system perspective and a delivery perspective. Training shall become more broader and the Fire Level 3 training will be phased out – and this is reflected in the scoring of 68%. Focus is now on Level 1-2 and compliance up to March 31st 2025 is shown below;
Table 14. Fire Safety Training levels 2024/25
| Requirement | Number Compliant | Number non-compliant | Total headcount | Compliance Status |
| Fire Level 1 | 687 | 63 | 750 | 92% |
| Fire Level 2 | 1253 | 318 | 1571 | 80% |
| Fire Level 3 | 536 | 249 | 785 | 68% |
| Total | 2476 | 630 | 3160 | 80% |
Since the Covid-19 pandemic, training was being delivered online and in 2024/25 we started to move training to face to face to enable the benefits this could bring. We have noticed that;
- Staff feel more engaged when training is on their ward / in their areas as it makes the training more specific and effective in a practical sense
- We can capture more ward staff by doing the training in a team format oppose to relying on individuals picking up this up online
- We can assist with any further fire related issues and provide advice and support for any outstanding fire risk assessment issues, especially where clinical services have been allocated actions
This approach shall be further developed in 2025/26.
15 – Other Areas of Note Relatable to Health and Safety
Other areas of note to assure the Trust Board that the Health and Safety Team are covering vast areas of Health and Safety include;
Lone working – the Trust went live on 1st December 2024 with its Lone Working App system. There have been teething issues which has resulted in the re-formation of the Task and Finish Group and it is expected based on initial meetings that this group will collaboratively resolve issues. Of the 1000 licenses purchased, there has been an uptake of over 750 staff by the end of Q4 who have signed or been signed up to the App, a figure that is likely to grow throughout 25/26.
NHS Sexual Safety Charter – from 26th October 2024, a new legal duty on employers to take reasonable steps to prevent sexual harassment under the new Worker Protection (Amendment of Equality Act 2010) Act 2023 came into force. This is coupled to the launch of the national NHS Sexual Safety Charter. The Health and Safety Team are supporting a Trust Workforce Sexual Safety task and finish group established to ensure compliance with the new employers’ duty (Workers Protection) to take reasonable steps to prevent sexual harassment.
Occupational Health – we continue to procure this service in a collaborative partnership with South West Yorkshire Partnership FT. Unfortunately, data had been impacted through the reporting period as Occupational Health were in the process of implementing a new system that was planned to go live in January 2025, albeit not fully functional. The old system was no longer supported so was switched off in December so Occupational Health staff worked manually which inevitably caused delays and a back log.
16 – Conclusion
The work plan within the reporting period has been affected by the Health and Safety Team not being fully staffed until late Q1. However, it should be noted that primary statutory requirements have been adhered to as well as identifying solutions to issues throughout the year. There is evidence of progress in some areas, and other areas where there may be a decline in performance. It must be noted that we have introduced systems and processes to cover more legislative requirements whilst maintaining the same staffing numbers – working collaboratively and effectively should allow some efficiencies so our process and systems are optimised and should not demand additional resources.
The Trust continues to ensure that the Health, Safety and welfare of all stakeholders, including service users, staff and visitors remains a high priority and a core consideration during service development and delivery.
The Health and Safety Team will prioritise improved collaboration and governance in 25/26 given that Health and Safety will only be robustly managed in the Trust when if becomes ‘everyone’s business’.
Audits, inspections and reviews of policies and procedures were all undertaken during 2024/2025. Training was refreshed and reviewed over the year to ensure it remains up to date, meeting statutory compliance and accessible to all staff groups.
17 – Recommendation
The Audit Committee are asked to accept this annual report.
18 – Appendix 1 – 7 Day absences including Non RIDDOR
Not all over say absences result in a requirement to submit an HSE RIDDOR notification, i.e. seizure, faint, stress trauma or road traffic accident.
| Location | Aggressive or hostile behaviour | Assault by patient on staff | Collision with person/object | Road traffic accident | Seizure or faint | Staff injured during restraint of pt | Loss of balance | Fall on steps/stairs | Other type of accident | Totals |
| CAMHS – Red Kite View (PICU) | 2 | 0 | 0 | 0 | 0 | 0 | 0 | 0 | 0 | 2 |
| Newsam – Ward 1 – PICU | 0 | 2 | 0 | 0 | 0 | 0 | 0 | 0 | 0 | 2 |
| 136 Suite – Adult | 0 | 0 | 0 | 0 | 0 | 0 | 0 | 0 | 1 | 1 |
| 156 Austhorpe Road | 0 | 0 | 0 | 0 | 1 | 0 | 0 | 0 | 0 | 1 |
| 34 Stainbeck Road | 0 | 0 | 0 | 0 | 0 | 1 | 0 | 0 | 0 | 1 |
| Asket Croft – Rehab and Recovery | 0 | 0 | 0 | 1 | 0 | 0 | 0 | 0 | 0 | 1 |
| Becklin – Ward 1 | 0 | 0 | 1 | 0 | 0 | 0 | 0 | 0 | 0 | 1 |
| Bluebell | 0 | 0 | 0 | 0 | 0 | 0 | 0 | 0 | 1 | 1 |
| CAMHS – Red Kite View (General Adolescent Unit) | 1 | 0 | 0 | 0 | 0 | 0 | 0 | 0 | 0 | 1 |
| Domestic Department | 0 | 0 | 0 | 0 | 0 | 0 | 0 | 1 | 0 | 1 |
| HMHT – LGI | 0 | 0 | 0 | 0 | 0 | 0 | 0 | 0 | 1 | 1 |
| Newsam – Ward 2 A and T | 0 | 1 | 0 | 0 | 0 | 0 | 0 | 0 | 0 | 1 |
| Newsam – Ward 2 W | 0 | 0 | 0 | 0 | 0 | 1 | 0 | 0 | 0 | 1 |
| Newsam – Ward 5 Rehab | 0 | 1 | 0 | 0 | 0 | 0 | 0 | 0 | 0 | 1 |
| SSE CMHT OPS | 0 | 0 | 0 | 0 | 0 | 0 | 0 | 0 | 1 | 1 |
| Yorks Centre for Eating Disorders – YCED Ward 6 NC | 0 | 0 | 0 | 0 | 0 | 0 | 1 | 0 | 0 | 1 |
| Totals | 3 | 4 | 1 | 1 | 1 | 2 | 1 | 1 | 4 | 18 |
| 23/24 Totals (12) 22/23 Totals (30) |
3 | 4 | 1 | 1 | 1 | 2 | 1 | 1 | 4 | 18 |
19 – Appendix 2 – Trust wide Health and Safety Incident Data 2024/25
The below table highlights the areas where incidents have occurred, and what group of people have been affected by the incident.
| Service | Incident affecting Patient | Incident affecting Staff | Incident affecting Organisation | Incident affecting Visitor / Contractor or Member of the Public | Total |
| Adult Acute Services | 953 | 548 | 218 | 11 | 1730 |
| Older Peoples Services | 882 | 315 | 59 | 15 | 1271 |
| Forensic Services | 380 | 438 | 209 | 6 | 1033 |
| Children and Young People Services | 450 | 352 | 136 | 34 | 972 |
| Eating Disorders and Rehabilitation Services | 275 | 130 | 158 | 2 | 565 |
| Learning Disability Services | 122 | 111 | 12 | 4 | 249 |
| Community and Wellbeing Services | 34 | 34 | 27 | 19 | 114 |
| Liaison and Perinatal Services | 30 | 26 | 16 | 9 | 81 |
| Regional and Specialist Services | 15 | 21 | 4 | 6 | 46 |
| Medical | 0 | 3 | 7 | 0 | 10 |
| Finance Services | 0 | 3 | 5 | 0 | 8 |
| Workforce Development | 0 | 2 | 0 | 1 | 3 |
| Corporate Services Directorate | 0 | 2 | 0 | 0 | 2 |
| Professions and Quality – Corporate | 0 | 2 | 0 | 0 | 2 |
| All Services | 3141 | 1987 | 851 | 107 | 6086 |
Cover sheet for Report of the Chief Operating Officer
- Paper title: Report of the Chief Operating Officer
- Date of meeting: 31 July 2025
- Presented by: Joanna Forster Adams, Chief Operating Officer
- Prepared by: Members of the Care Services’ Senior Operational Leadership Team
This paper supports the Trust’s strategic objective/s (SO):
- SO1 – We deliver great care that is high quality and improves lives.
- SO2 – We provide a rewarding and supportive place to work.
- SO3 – We use our resources to deliver effective and sustainable services.
This paper relates to the Trust’s strategic risks (SR):
- SR1 – Quality including safety assurance processes
- SR2 – Delivery of the Quality Strategic Plan
- SR4 – Financial sustainability
- SR5 – Adequate working and care environments
- SR7 – Plan and deliver services that meet the health needs of the population we serve.
Executive summary
This report is presented to the July Board of Directors’ meeting to set out the key management, development, and delivery issues across LYPFT Care Services and to highlight any potential impact for the population we serve. It is derived from work with operational, clinical and quality colleagues, where information and intelligence is used alongside experience, to establish where we should prioritise our efforts for improvement (and recovery where necessary). Our established arrangements for operational and clinical governance enable us to highlight key areas for the attention of the Board. This report has been presented and discussed in the Finance and Performance Committee.
Do the recommendations in this paper have any impact upon the requirements of the protected groups identified by the Equality Act? No
Recommendation
The Board of Directors is asked to be assured of the work being undertaken to deliver our care services and to manage the range of challenges and issues outlined in this report.
Report of the Chief Operating Officer
1 – Introduction
This report sets out the key management, development, and delivery issues across LYPFT Care Services. It aims to summarise and highlight the most significant service delivery issues we are facing.
Primarily the main areas of concern are set out in the “Alert” section of the Service Delivery and Key Performance section of this report (Section 2.1 below). However, as a very high-level summary the most concerning issues include:
- Acute flow and out of area placements (including an update on the temporary closure of Oasis House; crisis house provision in Leeds, which is a key alternative to admission to inpatient services)
- Enteral feeding supply disruption and resultant incident response/management
- Industrial Action.
Focus on our responsiveness (timely quality domain) continues so that we can ensure that we maintain and improve our response and access. Consequentially, the advisory section of this report includes updates on:
- Adult Acute: Crisis Resolution assessments within 4 hours
- Service users seen / visited at least 5 times in first week of Crisis contact
- Emergency Department (ED) waits for mental health assessment
- Aspire Provision of Early Intervention in Psychosis Services.
This month, we have introduced an “in focus” section which summarises the performance and service delivery improvements overseen in the Care Services Delivery and Development Group. These primarily relate to services where we have had performance and quality concerns and have been operationally and clinically led.
2 – Service Delivery and Key Performance Escalations
2.1 Alert
This section sets out the key areas of concern for care services that have been identified through our governance arrangements. These updates relate to the areas where services face most challenge and where risks are highest.
2.1.1 – Acute Flow and Out of Area Placements
The Out of Area (OOA) position remains significantly above projected levels, reflecting sustained system pressures. Monthly referral volumes generally ranged between 55 and 65, with notable peaks observed in February and June 2025, reflecting periods of heightened demand for inpatient mental health services.
Graph 1

Our programme of work has previously focused on alternative to hospital and purposeful admissions as the key change required to affect demand. However, work has been broadened so that we influence clinical practice in community and crisis services.
2.1.1.1 – Delays in discharging patients Clinically Ready for Discharge (CRFD)
While there has been a reduction in delayed bed days overall, delays persist for individuals who are Clinically Ready for Discharge (CRFD). These delays are predominantly due to the limited availability of appropriate accommodation, particularly supported housing that is suitably equipped to meet the needs of our service users.
Graph 2
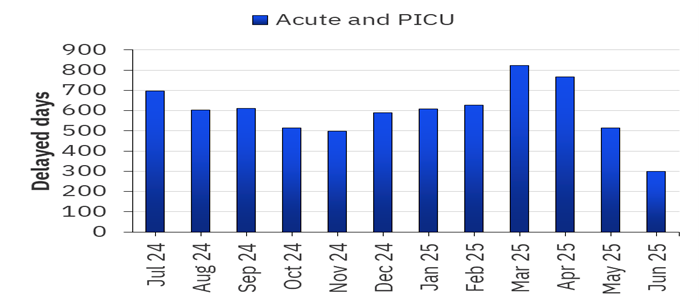
Despite the discharge workstream of our programme making progress in 2024/25, we need to double down our efforts at a system level to address the ongoing issues. Of note is that accommodation has been available with voids in some services which would be suitable for discharge from our services. This has been addressed in the immediacy, but systemic issues and lengthy processes need to be tackled. Colleagues at a system level have been helpful but this needs to be sustained. The Programme Lead, Laura McDonagh, is considering leadership of this element of the work and this may be best sought from a senior officer from the ICB or Leeds City Council. This has been effective in other programmes of work in the Health and Care sector.
We also continue to contribute to wider system initiatives, with senior-level representation in the Leeds Marmot Mental Health and Housing Task and Finish Group. This group is focused on addressing the accommodation needs of individuals with complex and enduring mental health problems, aligning closely with our discharge priorities.
In parallel, we are progressing a clinically led initiative aimed at ensuring full utilisation of all inpatient capacity. This includes introducing greater flexibility in admission criteria during periods of heightened pressure, allowing for the identification of alternative, needs-based provision. The overarching goal is to reduce reliance on out-of-area placements and improve timely access to care. This approach is being formalised through the development of a Dynamic Bed Management Process.
2.1.1.2 – Crisis House Closure
Pressures are further compounded by the temporary closure of the Oasis Crisis House, which has removed a critical community-based alternative to admission. This closure took place on 7 July and is likely to be for 8-10 weeks. Although mitigations have been put in place, these have been limited to a 5-hour day provision supporting people in crisis. We are involved in overseeing the progress on the estates work so that we can restart as soon as possible, maximising capacity for winter.
The absence of Oasis House has reduced system flexibility, increased reliance on inpatient beds, and contributed to higher admission numbers. At the date of this report there have been approximately 7 admissions to our inpatient services which would ordinarily have been routed to Oasis. We are also actively monitoring the impact of Oasis closure on CRISS and will report on this in due course.
2.1.1.3 – Complex Care and Clinical Review
In addition, complex case mix within acute wards, including patients with multiple comorbidities, safeguarding concerns, and intricate discharge planning needs continues to constrain flow and extend lengths of stay. We are unable to quantify this and will address this as part of our clinical review of the service which is a fundamental part of the 2025/26 programme of work.
To summarise, managing the current situation/pressure our immediate response and mitigation plan includes actions over and above programme activity. They include:
- Working with Adult Social Care and Third Sector Providers to reduce the voids in the Transitional Housing Units and supported accommodation
- Working with community teams to support and facilitate early discharge from hospital
- Increased frequency of Complex Case meetings to identify and resolve discharge barriers
- Recruitment of Housing Officers to work directly with our clinical teams in identifying housing barriers and supporting discharges.
2.1.1.4 – Current performance
At the date of this report, 36 individuals were receiving Out of Area care, significantly exceeding the planned trajectory of 13. This variance reflects sustained pressure on local capacity and reinforces the urgency of implementing sustainable, system-wide solutions.
Of particular concern is the spike in referrals observed in June 2025, which further increased demand for inpatient beds and placed additional strain on system flexibility. This trend will require close monitoring in the coming months, especially considering the closure of Oasis crisis beds, which plays a key role in providing an alternative to hospital admission.
Graph 3

At Month 2, the Acute service line is reporting an overspend, with £580k directly attributed to OOA placements. This reflects the ongoing demand, and discharge challenges and underscores the urgency of delivering the strategic interventions outlined above.
2.1.2 – Enteral Feed and Oral Nutrition Support (ONS) Supply Issue
In May 2025, issues escalated significantly, resulting in nationally reported shortages of several core Nutricia products, most notably Nutrison Energy Multifibre, the primary feed used by LYPFT’s Learning Disability (LD) services. The existing contract for enteral feeds, oral nutritional supplements (ONS), and associated feeding equipment has been in place for three years. It is a joint agreement between the LYPFT, Leeds Teaching Hospitals and Leeds Community Healthcare Trusts and the supplier Nutricia.
We have seen persistent challenges that have affected all three Trusts throughout the contract term, including:
- Recurring shortages of both nutritional products and feeding equipment
- Inconsistent customer service
- System-related disruptions.
Despite two formal contract breach notifications being issued, there is currently no viable option to exit the agreement due to capacity constraints across alternative suppliers. Nutricia currently supplies approximately 55% of all NHS nutritional products which limits any procurement flexibility.
The services with LYPFT that are currently affected by the supply issues are our Community Learning Disabilities Team (CLDT) and our Children and Young People’s Tier 4 service at Red Kite View. In addition, we have a number of services at high risk of disruption: Ward 6 Newsam; our Adult Eating Disorder ward; Children and Young People’s Tier 4 Service in York, Mill Lodge; our Acute Inpatient wards; and our Older People’s Services.
CLDT is most heavily affected, with around 80 service users reliant on PEG feeds using Nutrison Energy Multifibre. The CLDT Dietetics Team has had to divert clinical resources and reduce routine service delivery to prioritise continuity of care for this cohort.
The key risks associated with the supply issues are:
- Service users (community and inpatient) may run out of essential nutritional products or equipment
- A shift to alternative products may be required however, another supplier cannot provide like for like
- Risk to patient safety due to the unavailability of essential products included in the refeeding syndrome SOP, where failure to treat constitutes a medical emergency
- Financial pressure from switching to higher-cost alternative products.
The key risks for our service users are:
- Increased risk of constipation, malnutrition, and dehydration in the LD population
- Negative effects from switching feeds, especially for patients with sensory sensitivities or established, personalised prescriptions
- Potential for life-threatening complications if refeeding protocols are not followed.
We have a number of mitigating factors in place whereby most services, including those managing refeeding syndrome, can adopt alternative products with minimal disruption. However, CLDT cannot switch products safely due to:
- Clinical intolerance and harm among patients with learning disabilities
- Extended periods required to stabilise patients on new feeds
- Resource-intensive effort to switch, and eventually reverse, over 80 feeding plans.
The CLDT Dietetics Team has implemented the following measures:
- Prioritisation of caseload and reduction of non-urgent work
- Duty rota to manage out-of-stock issues
- Use of generic service emails to distribute communication load
- Daily team check-ins for coordination
- Recording clinical risks via Datix
- Maintenance of an active Nutricia issues log
- Escalation within both clinical service and AHP leadership
- Suspension of non-critical meetings
- A Band 7 locum dietician is to be recruited to provide capacity to ensure the team can make detailed reports of issues to Nutricia, DATIX and NHSE while disruption to supplies continues.
To manage and support services through this period of national and global supply issues we have established a Tactical Command Group with weekly meetings involving operational, risk, and clinical stakeholders who have defined clear reporting and escalation pathways. This group will also strengthen local and national partnerships, ensuring that LYPFT has robust representation at strategic meetings across Leeds and with NHSE. The group has ensured this risk is formally recorded on the Risk Register, with a corresponding action plan being in place.
2.1.3 – Industrial Action
The Board is advised that industrial action was called by the BMA affecting Resident Doctors between Friday 25 July 07:00 to 07:00 Wednesday 30 July. As a result, the Trust activated its planning arrangements with Strategic and Tactical Planning Groups led by the Chief Operating Officer. The purpose of the arrangements was to understand and mitigate any risks including the changeover of doctors in training in August 2025. As of 22 July, 49 out of 50 shifts affected during the strike period have been covered. In addition, 19 Memory Service outpatient appointments are to be re-scheduled as soon as possible. During the strike period the Trust has response arrangements in place to gather situation reports, understand any risks and report as required.
2.2 – Advise
2.2.1 – Adult Acute: Crisis Resolution assessments within 4 hours
The 4-hour Crisis Response service is showing signs of gradual recovery, with the team actively working to maintain performance and meet the target. Although we have seen a slight downward trend across two localities, overall, we have improved or remained at our previous position, see table 1 below. Efforts are being made to strengthen operational consistency, and there is a clear commitment to improvement. In parallel, collaboration with digital change and informatics teams is underway to enhance data quality and reporting capabilities, which will support more accurate monitoring and drive informed decision-making going forward.
We are currently advertising and recruiting to our vacancies across the three localities, and we have seen an improvement in staff absences. The leadership team continues to monitor the response rates closely and we are now able to report regularly the numbers of service users who are waiting more than 4 hours and how long this is, see table 2. What is evident is that very few service users are waiting more than 8 hrs for an assessment.
Table 1
| Locality | Very urgent 4hr Response | Urgent 24hr response |
| South CRISS | 72% (down) | 71% (down) |
| West CRISS | 75% (down) | 80% (down) |
| East CRISS | 69% (up) | 75% (up) |
| Overall | 72% (up) | 75% (equal) |
Table 2
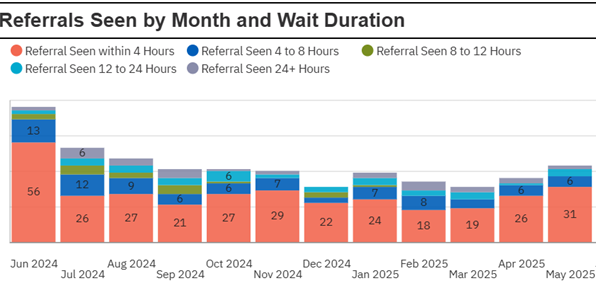
2.2.2 – Service users seen / visited at least 5 times in first week of Crisis contact
We have seen a reduction in performance relating to service users being seen at least 5 times within the first week of receiving Crisis support (33.6% against a target of 50%) due to a number of reasons. These include the length of time a person has been on caseload being less than a week, with factors such as 72 hour extended assessments from A&E not resulting in an extended stay on the caseload; shared care on the wards to facilitate leave in preparation for discharge; and also working in line with core fidelity and becoming more aligned to trauma informed care keeping a consistent team supporting service users whilst also managing acute risks. The teams are monitoring this in weekly team performance meetings and are also reviewing the MDT board daily.
2.2.3 – Emergency Department (ED) waits for mental health assessment
The ALPS 1 hour response rate had slightly deteriorated in May with an improved position to 72% at the end of June, see the graph below. The number of referrals has remained high at around 270 per month, but we saw an increase of around 40 referrals during May which accounts for the slight deterioration in the response rate. The Operational and Team Manager for ALPS have developed a detailed action plan outlining targeted improvement measures, along with a defined trajectory for progress. Implementation will be closely monitored to ensure sustained improvement and a clearer understanding of the barriers to progress.
We still expect the response rate to improve with the planned move to the LTHT site, and the team had been in the process of moving back to the identified office space in St James’ Hospital. However, some issues about where the accommodation was and the access to it have been identified. The team are working with colleagues within LTHT to try to resolve these issues so the move back to the LTHT site can resume a soon as practicable.
In addition, the team has been operating below full capacity following the departure of two staff members. These positions have now been substantively filled, with confirmed start dates and comprehensive induction plans in place for the incoming staff.
Graph 4

The reducing ED waiting times work has started, with the Terms of Reference being shared at an initial meeting of the project group and the Project Initiation Document (PID) nearing completion. The service is also gathering information about differing models of provision nationally to better inform future delivery and options that may be available to us.
2.2.4 – Aspire Provision of Early Intervention in Psychosis Services
As previously reported, the Head of Operations for our Community and Wellbeing service line has been working with colleagues in Aspire to support improvements against the physical health checks and treatment commencement targets.
We have seen an improvement in the response rate for referrals commencing a NICE recommended package of care, with two weeks achieving 57% against a target of 60% as detailed in graph 5 below. This will be monitored closely to ensure the improvement is sustained. Work continues with the team to improve the rate of completion of the Cardiometabolic assessment, with a slight improvement in May, as detailed in graph 6.
Graph 5
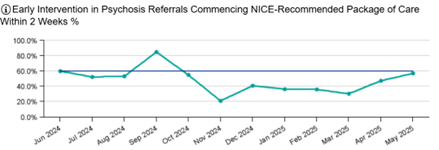
Graph 6
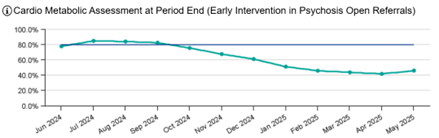
2.2.5 – Waiting List Management
An internal project has commenced which will ensure services have effective systems in place for waiting list management, and to ensure they are operating in line with national guidance and best practice. As part of the project the team will ensure that where possible systems are automated and make maximum use of the Trust’s patient record system and teams have up-to-date information on waiting times and are able to maximise the use of clinical capacity through effective demand and capacity management which will also allow services to forecast this.
The project will review Standard Operating Procedures and current processes for managing waiting lists and review capacity and demand within teams with the aim of effectively matching capacity to demand. The first three services to be reviewed will be Perinatal Community Services, the Memory Service and Deaf CAMHS. If successful, the review will be rolled on to further services.
2.2.6 – Community Services across Leeds: GP Collective Action
The Heads of Operations for both Community & Wellbeing and Forensic Services meet with ICB representatives each week to review ongoing developments. At this stage the collective action is not predicted to be resolved in the foreseeable future. The work has been transferred to the Primary Care Principles Interface workstream. This is because the ongoing approach to working with our GP colleagues is to explore where the barriers currently are within that framework and complete target work to support progress.
Care Services in LYPFT have felt minimal impact up to this point, possibly as a result of fewer pathways that lead back to the GPs compared to other Secondary Care providers. However, We have had one case within a CMHT where a GP practice refused to prescribe a change to an anti-depressant (despite being a green drug), quoting the ongoing GP Collective Action. This was escalated to the ICB and was followed up clinically by the CMHT. Ongoing discussions are being overseen by the LYPFT Pharmacy Team around a depot medication administration pilot within a GP surgery, whereby a practice nursing staff would deliver the intervention.
We have also established a group specifically to look at LYPFT service users accessing the Community Diagnostic Centres (CDCs) for blood tests and ECGs. Group leads have met with the ICB and LTHT, however, it is not currently an option for LYPFT services to request tests directly into the CDCs as it requires the use of the Integrated Clinical Environment (ICE); an electronic system used for requesting pathology tests, including blood tests, in healthcare settings. Our Clinical Systems Team, working alongside our CONNECT service, is working on the potential to access ICE safely via an online platform.
In addition to requests for tests, we are establishing two further groups, with one focused on implementing our Trust procedure around issuing fit notes, and another focused on care services referring onto departments outside of LYPFT (e.g. cardiology).
2.2.7 – Single Homelessness Accommodation Project (SHAP)
The objective of SHAP is to increase the supply of high-quality accommodation with accompanying support to address gaps in homelessness pathway provision. SHAP will be targeted at two groups: those with the longest histories of rough sleeping or the most complex needs, to help them recover from rough sleeping and its associated traumas; and vulnerable young people (age 18-25) at risk of / or experiencing homelessness or rough sleeping.
It is expected that local councils will be key to developing local strategies and providing funding to deliver those strategies. Leeds City Council have now provided a final draft of the contract to LYPFT, this is under review with procurement, delivery team and the Head of Operations for Community & Wellbeing to ensure accuracy. Once agreed this will move forward for final signing in line with the Trust’s governance procedures. In the interim the Rough Sleepers Team has been working alongside the SHAP Team and preparing the necessary clinical models, operational processes and considering challenges/issues to support with the service being implemented. The next steps will be to formalise the contract and then proceed to the recruitment of the required posts.
2.2.8 – CONNECT Community: Referral to Assessment Times
As of May 2025, the referral to assessment time (RTA) is 18 weeks. This has gradually increased from 14 weeks since October 2024. Whereas the referral to treatment times (RTTs) are currently at 22 weeks, depending on the specialty. This in the main, is due to increased sickness absence. These delays have been added to the service risk register with mitigations and recovery plans in place. This is the 3rd time psychological therapy staffing has been reported as an issue and recorded on the risk register within 2 years, highlighting an underlying issue with the staffing model. This will be addressed via a service model review to ensure there is resilience to maintain service delivery.
Waiting times are also being impacted by under activity and inefficient processes within the community team. A process mapping exercise is underway to review the current referral to assessment and treatment process, replacing this with a process that is lean and able to meet the required 4-week standard. In addition, expected activity levels are being set within 1:1 job planning and will then be monitored monthly with individual staff. This process is being written into a caseload management Standard Operating Procedure; however, we have seen that reported activity (clinical contacts) has increased since March due to improved recording, with the 3-month average of 668 compared to an average of 504 for the previous 8 months.
2.2.9 – Deaf CAMHS Access to Assessment
There is a significantly deteriorating position in Deaf CAMHS access which requires exploration, understanding and resolving. Deaf CAMHS operates in a significantly different way to ‘hearing’ CAMHS services. This is because there is an inherent complexity in working with children, young people (CYP) and families who are deaf and have mental health issues which demands a range of skills that are seldom located in single individuals. For most deaf CYP, communication is a major barrier to accessing effective care and treatment. It is imperative that we make improvements in order to respond effectively and in a timely way on a sustained basis.
In response, our Deputy Director of CYPMH Services, Tim Richardson, alongside the Head of Operations, Kay Lawn, and the Clinical Lead, Hannah George, are in the process of a comprehensive diagnostic that enables us to build on the actions already being put in place by the team and an update of this will be reported in the autumn.
2.2.10 – Assessment and Diagnostic Key Performance Metrics (KPI’s) for the Memory Assessment Service
Recent discussions with teams have identified contributing factors impacting a deterioration in both Assessment (within 8 weeks) and Diagnostic (within 12 weeks) KPIs.
This is a small function providing a vital and expert service and we have had vacancies which have now been recruited to, so we are factoring in the increased capacity into our recovery plans. Additionally, there has been some reduced medical capacity as a result of training and examinations, so we have learnt to plan more effectively in future for how this impacts on our capacity.
We have a number of mitigation and response actions in place which include:
- Clinical Team Managers (CTMs) working with the wider MDT to explore all available options and ensure full use of existing capacity
- Medics introducing additional appointments specifically for the assessment and diagnosis of medic-only patients
- Further evaluation of capacity planning to minimize impact during future medic changeovers.
Although recent operational challenges have temporarily affected KPI performance, proactive mitigation actions are showing positive early results. Continued monitoring and adaptive planning will be critical to sustaining and improving performance going forward.
Assessment (within 8 weeks)
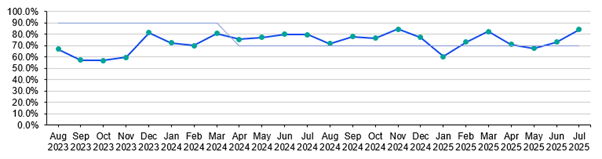
Diagnosis (within 12 weeks)
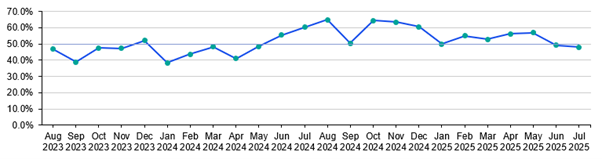
2.3 – Assure
2.3.1 – Complex Rehabilitation Service
Following approval of the Complex Psychosis Pathway business case, the service expects to begin formal consultation from 1 August 2025 followed by a mobilisation phase. This work has been incorporated into the Community Mental Health Redesign Programme. The workforce principles established from this programme of work will be applied to the Complex Psychosis Pathway.
2.3.2 – Leeds Forensic In-Patient Service
The new seclusion suite at the Newsam Centre, which is within the Forensic Service, was used for the first time recently. Initially there had been concerns about the quality of the finish of the building work, however during its recent use the suite stood up well to the use. The ward team has been praised by colleagues within the LTHT Emergency Department, as a brief transfer was required for a service user following self-injury. Despite the challenges faced with this case, there was a good response from Yorkshire Ambulance Service, West Yorkshire Police and LTHT staff, demonstrating the positive collaborative approach to meet the needs of the service user who presented as extremely unwell at the time.
3 – In focus
The purpose of this new section of the COO report is to summarise progress of improvement and recovery work in services that are overseen by the Care Services Delivery and Development Group. This month this section includes the Older Adults Services, where there have been significant challenges following the Covid pandemic, which had the highest impact on the population served by this service. This section also draws together the work of the Children and Young People’s leadership team focused on Red Kite View and summarises the update provided at a Board Development session in June 2025.
3.1 – Older People’s Mental Health Services
The Older People’s Mental Health Service within LYPFT is composed of three core components:
- Inpatient Services
- Community Services
- Intensive Services.
Each area has continued to strive for improvement and development despite the challenges faced. The following ‘In-focus’ report outlines recent developments, initiatives, and ongoing work within each of the above service areas, with a particular focus on leadership, culture, service changes, and operational delivery.
3.1.1 – Foundations: Culture and Leadership Development
In early 2024, the Service embarked on a strategic initiative to re-establish leadership, clarify direction, and embed shared values and behaviours. This work, conducted in collaboration with HR, Organisational Development (OD), and the Service Improvement Team, placed a renewed focus on cultivating a positive and sustainable culture.
The programme aimed to:
- Strengthen the Older People’s Services Senior Leadership Team (OPS SLT), its working practices, shared values, and ability to cascade these across the service
- Transition the OPS culture toward a collective leadership approach grounded in learning, psychological safety
- Promote civility and respect in the workplace, with specific emphasis on inpatient services
- Increase readiness for ongoing and future service changes.
We have seen positive indicators of progress including the development of a Leadership Charter, which outlines agreed behaviours and commitments of the OPS SLT. This has helped develop the influence of the SLT, which has positively impacted broader service development.
- Inpatient Services
The Service maintains a commitment to smaller, safer wards, supporting patient wellbeing and staff sustainability. Strategic emphasis is placed on improving flow and strengthening out-of-hospital care.
Key Developments for our in-patient service are:
- Alternatives to Admission: Development of purposeful admission criteria as part of the Trust-wide Improving Patient Flow programme
- Length of Stay Reduction: Embedding “Clinically Ready for Discharge” governance structures across wards
- Integrated IHTT Input: Establishing in-reach from the Intensive Home Treatment Team (IHTT) to enhance flow
- Interface with Adult Social Care: Strengthening escalation pathways and collaboration
- Geriatrician Support: Enhanced input from LTHT geriatricians at The Mount, improving the quality of the physical care provided
- Ward 2 Planning: Collaborative work with Liaison and Perinatal Services to align plans for the expansion of the Mother and Baby Unit (MBU), ensuring Ward 2 services were improved and appropriately supported.
In 2024/25 a £521,000 reduction in bank and agency staffing spend was achieved in compared to the previous year. However, this brings some challenges including the following:
- Maintaining safe staffing levels
- Sustaining patient flow
- Reducing operational run rates.
3.1.3 – Community Services
The Care Homes Team is currently being co-located with existing OPS Community Mental Health Teams to streamline operations with a view to improving clinical outcomes for older people living in care homes across Leeds.
Community Transformation continues to develop an integrated care model; the Older People’s Service is engaging with partners involved in this work to ensure continuity and quality in care delivery whilst retaining its specialised focus.
The Memory Assessment Service has a formal service evaluation underway to assess effectiveness and inform potential improvements.
We also continue to face challenges within the delivery of our community services which include identifying sustainable funding to support additional community-based roles.
3.1.4 – Intensive Services
Intensive Home Treatment Team (IHTT) quality improvement initiatives are ongoing to sustain high standards of care while enhancing patient flow across the care pathway.
The Intensive Care Homes Team is being integrated under a single management structure with the IHTT. This change aims to enhance collaboration and improve service quality metrics.
3.1.5 – Complex Dementia Wraparound Team
Engagement with Leeds City Council (LCC) and Leeds Community Healthcare (LCH) continues. This is to develop a future model of care for a Dementia Hub which can provide short-term, recovery-focused care for people living with dementia and associated psychological and behavioural needs. We are close to agreeing an adapted clinical model so our care homes teams can work more efficiently and effectively within the wider system.
3.1.6 – Summary
The Older People’s Mental Health Service has made significant strides in reshaping its culture, enhancing leadership, and improving clinical and operational delivery across inpatient, community, and intensive services. While challenges remain, the foundational work completed in 2024 positions the service for sustained improvement, innovation, and more integrated working with partners across the system.
3.2 – Improvements at Red Kite View
In Spring 2024, the number of concerns raised at, and with respect to Red Kite View (RKV) reached a level that prompted high-level intervention to provide support to the RKV team and to better understand what had prompted that volume of concerns.
This ‘In-focus’ section outlines in brief the interventions and the current position in terms of the Dynamic Improvement Plan.
3.2.1 – Progress update report
In May 2024, the Trust became aware of a range of concerns about Red Kite View (RKV) raised via several routes including through the CQC, the CEO office and by external professionals. Issues raised included poor supervision of young people, poor concern for staff welfare and well-being, not fully addressing staff concerns with respect to CYP safety, inadequate leadership, poor communication and staff behaviour.
The issues raised were almost exclusively about the running of the GAU (Skylark), rather than the PICU (Lapwing). The primary consideration was to ensure the unit was operating safely for young people. The safety of RKV was quickly established and it was agreed that a cessation of activity would not be necessary. All concerns have been responded to following due process.
The Provider Collaborative (PC) Lead offered to be more closely involved, and this involvement culminated in a report for EMT which set out the issues with several recommendations. Although the early intervention had established the service was not inherently unsafe, there were areas which needed a high level of focus. These areas for improvement included: systems and processes, communications, care pathways, clinical practice, incident learning and management, staffing, leadership, and culture.
Additional layers of scrutiny were applied via the West Yorkshire Collaborative Hub (WYCH), the Quality and Commissioning arm of the West Yorkshire Provider Collaborative, through a Service Development and Improvement Plan (SDIP), which in turn prompted the enactment of a Rapid Quality Review (RQR) from NHS England.
The externally monitored SDIP and RQR were closed in December 2024 and February 2025 respectively, having received evidence to provide assurance of appropriate responses to the issues raised. Any outstanding items from the SDIP and RQR were incorporated, where appropriate, along with the findings from the senior nursing team and the Provider Collaborative Lead Report into an over-arching Dynamic Improvement Plan for RKV.
The Dynamic Improvement Plan (DIP) amalgamated the concerns from the various sources into categories reflecting the different areas for improvement, i.e. systems and processes, communications, care pathways, clinical practice, incident learning and management, staffing, leadership, and culture.
The guiding principles behind improvements focus on the quality of care and treatment of young people, and positive experience for families and carers with a child in RKV. To achieve these goals, the staff providing the service need to be (and feel) well supported, understood and valued. Well valued staff invest in their own development, know when and how to seek support and provide a better service to young people and families.
Some of the things we have done in response to the concerns raised are:
- Installed a CYPS experienced Deputy Director to provide dedicated senior leadership
- Commissioned the Organisational Development Team to provide objective expert input
- Commissioned Legacy Mentors to support staff, with particular involvement to support nursing colleagues
- Introduced a Modern Matron
- Appointed a new Head of Operations (CYPS experienced)
- Established an Executive Oversight Group to monitor the Dynamic Improvement Plan.
As a result of some of the changes we have made at Red Kite View, we are seeing an improvement in the qualitative measures which show how we have improved the services we provide to children and young people. These include:
- Increased capacity and flow which has impacted positively on CYP Out of Area Placements (OAPs) – a 55% decrease overall in placements, with PICU and Low Secure admissions (at the time of writing) being eliminated. This reduction in OAPs means fewer young people are having to be treated far from home
- A reduction in the number of complaints received over the last 6 months – down by 10%
- An increase in bed usage at Red Kite View; this is a dynamic measure which is currently fluctuating between 25% and 30% increase.
In regard to the staffing position on the unit, this has improved as follows:
- Between June 2024 and June 2025, we had 6 leavers and 16 starters
- PICU nursing vacancy was at 48% in June 2024; and in June 2025 35%
- GAU nursing vacancy was at 60% in June 2024; and in June 2025 39%.
Having a more stable workforce helps provide quality care, team cohesion and supports staff well-being.
Whilst we have made significant progress with the actions we identified, there are still some areas we are working on. These include:
- Systems and processes – We undertook a full review of systems and processes. This led to some additions to the governance structure to improve internal communication within the team and the wider Trust. We will continue to work on improving communication with families and external colleagues.
- Care Pathways – We are seeking to develop innovative ways of working which will ultimately see fewer young people requiring less time in hospital. These include plans for Day Provision, a Crisis Bed model and an Outreach team to support young people in the community.
3.2.2 – Summary
Red Kite View was subject to a significant volume of concerns and the Trust responded at pace to determine the reason for these. The intensive intervention established that RKV was safe but required improvements. Recommendations came from a variety of sources and were amalgamated into one Dynamic Improvement Plan with a focus on quality of care for young people.
RKV is essential to the success of the Provider Collaborative and the wider system. Recent improvements have seen a 33% increase in bed use, leading to a 55% reduction in the use of out of area beds, meaning that more of our West Yorkshire young people are receiving the care and treatment they require closer to home. In the Provider Collaborative, with RKV at its core, use of out of area PICU and Low Secure Units has been reduced to zero at the time of writing.
4 – Service Developments
4.1 – Temporary Changes to Oasis
The crisis house, run by Leeds Survivor-Led Crisis Service (LSLCS) in partnership with LYPFT, offers an alternative to hospital admission for people who do not require a bed on an acute ward and may benefit more from a homely environment. This service will temporarily close for a period of 10 weeks to allow improvement work to take place in order to make the building more accessible.
The planned improvements are:
- Bed capacity will increase from five to six rooms
- Additional space will be created for staff use
- A fully accessible bedroom will be added
- A new summerhouse will be built in the Oasis garden to serve as a private space for confidential conversations
- One-to-one support space will also be improved.
Due to the late notice of these works commencing, it has not been possible to find alternative premises to relocate the service. LYPFT has worked with LSLCS to identify solutions for the short term. These include:
- A day service operating from DIAL House in Halton, supported by LSLCS, from 10 am to 3 pm, seven days a week, offering one-to-one support
- After 3 pm, service users will return to their home addresses and LYPFT staff will provide daily home visits between 3 pm and 8 pm
- If support is required during the night, this will be available from DIAL House
- A referral pathway has been agreed so that individuals supported by CRISS or IHTT do not need to self-refer; home teams can refer directly
- If someone accessing DIAL House needs further support, DIAL House staff will contact the crisis team to arrange a home visit.
A weekly monitoring group has been established to monitor the impact on system performance and to identify mitigating actions where necessary. Membership of this group is from LSLCS, LYPFT (CRISS, OPS and Liaison) and the West Yorkshire ICB. It is also the intention to undertake a more in-depth review at the end of the closure to determine if there has been any impact on the wider system.
4.2 – Complex Dementia Services
Leeds City Council along with Leeds Community Healthcare and LYPFT have been reviewing the provision of Complex Dementia Care across the city. A proposal for the future of Dolphin Manor at Rothwell to become a ‘Dementia Hub’ has been developed providing short-term, recovery-focused care for people living with dementia and associated psychological and behavioural needs. It brings together two separate bed bases (The Willows and The Oaks) into one and enables the ten beds used for The Willows to return to Community Care Bed use. The Integrated Commissioning Executive supported these plans. There will be an impact on the services provided by the older people’s service line, with the implications for LYPFT and other providers being worked through and a more detailed proposal monitored through our internal governance system.
5 – Improving Health Equity
The Trust’s Improving Health Equity mission is to enable equity at the heart of everything we do and maximise the Trust’s contribution to improving health equity in the populations we serve. Progress is being made in all IHE Strategic Plan areas.
This strategic plan largely focuses on improving equity in access, experience and outcomes within healthcare. We are particularly concentrating on the following groups:
- The systematic, unfair and avoidable differences in health between those with learning disability, neurodiversity, severe and enduring mental illness, and those without
- Tackling racial health inequity within mental health services which are evidenced to be extensive and persistent
- Intersectionality: People at exceptionally high risk of poor health outcomes because they are a member of multiple groups and experience compounding disadvantage, for example those with a severe mental illness and from a racialised community and who also live in a deprived community
- Our service users who experience deprivation, with a particular focus on our service users living in the 10% most deprived communities nationally.
Our year one Improving Health Equity (IHE) Action Plan focuses on three project objectives:
- Increased coordination of LYPFT’s existing programmes, projects and initiatives focused on improving equity to amplify the impact and efficiency of existing initiatives.
Progress: Year One IHE action plan agreed by the Quality Committee and has now moved to implementation. New IHE Team established to support delivery of the IHE Strategic Plan. New workplans created aligning to IHE Strategic objectives. Progressing various workstreams linking work across the Trust. These include:
- Culture of Care and PCREF Action Plan
- Equality Delivery System and service line equity focused work via cultural inclusion coordinators
- PCREF Action Plan and Advanced Choice Documents pilot
- Scoping LGBTQI+ projects across the Trust via cultural inclusion coordinators.
- Ensure we are meeting our statutory obligations relating to equity, maximising opportunities to broaden this work and embed within the broader strategic plan. This includes Equality Act, Public Sector Equity Duty, EDS 22, PCREF and the Health Inequalities Duties under Health and Care Act.
Progress: We have identified an IHE Steering Group chair and membership with Terms of Reference (ToR) established for the first meeting in July. We have a PCREF chair, ToRs, working group established first meeting in July. Presented at national PCREF Early Implementor Showcase event to share best practice and PCREF work plan so far. Wrote and coordinated WYICB PCREF paper on responding to MH Bill reforms to include PCREF. Finalising the EHIA policy, guidance and template. Team aligned to EDS delivery and assessment requirements with a focus on long-term conditions agreed across the West Yorkshire ICB.
- Strengthen our foundations: a focus on our patient, carer, staff and community engagement.
Progress: Engagement with Forum for Racial Equity in Health and Social care started. Next feedback session due end of July. Developing objectives with FRESH to establish a new PCREF Partnership Group, scoping the interest in supporting a systemwide ‘Advanced Choice Documents’ (ACD) pilot alongside Health, Council, Police, VCSE partners. We are part of the ACD national best practice implementation group and vision for ACD to be mandatory in the new mental health act reforms currently going through parliament. Scoping interest in holding future FRESH PCREF events specifically focussing on CYP, and perinatal. Four lived experience partners recruited.
6 – Emergency Preparedness Resilience and Response
6.1 – Heatwave Response
The Trust responded to the heatwave from 19 to 23 June, with tactical level planning arrangements being in place since May. Prior to the heatwave, teams were asked to fill in a survey to highlight any heatwave related needs and this helped identify areas where portable air conditioning units were required. Measures to mitigate risks of the heatwave were put in place and staff awareness was raised via the Communications Team. Additional spend has been made to purchase portable air conditioning units to ensure sufficient stock is in place to mitigate the risk in the summer period.
Summary and recommendation
The Board is asked to be assured of the work being undertaken to deliver our care services and to manage the range of challenges and issues outlined in this report.
Joanna Forster Adams
Chief Operating Officer
July 2025
Contributions from members of the Care Services’ Senior Operational Leadership Team.
Service Performance Report June 2025
Please download the Service Performance Report June 2025. This PDF is not accessible to some users, please see below plain text summaries of the document.
Access and Responsiveness: Our Response in a Crisis
- ALPS referrals responded to within 1 hour improved to 72.5% in June.
- No S136 detentions exceeded 24 hours.
- Crisis referrals seen face-to-face within 4 hours dropped to 69.7%, below the 90% target.
- 92.7% of CRISS caseloads were under 6 weeks, exceeding the 70% target.
- Only 33.6% of CRISS users were seen 5+ times in the first week, below the 50% target.
- Referrals from acute inpatients to CRISS increased to 7.5%.
Access and Responsiveness to Learning Disabilities, Regional and Specialist Services
- Gender Identity Service waiting list rose to 6,756.
- Deaf CAMHS average wait increased to 189 days.
- Community LD referrals seen within 4 weeks dropped to 64.5%, below the 75% target.
- LADS diagnostic decisions within 26 weeks were at 64.7%.
- LADS assessments started within 13 weeks were low at 14.5%.
- CAMHS inpatient assessments within 7 days reached 81.2%, below the 100% target.
- Perinatal urgent contacts within 48 hours were at 75%.
- Routine perinatal assessments within 2 weeks exceeded target at 87.5%.
- 936 distinct women were seen in the Perinatal service (target: 950).
- Perinatal DNA rate was 8.5%.
Our Acute Patient Journey
- No under-16s were admitted to adult facilities.
- CAU bed occupancy decreased to 73.3%.
- CAU average length of stay was 17.75 days.
- Liaison In-Reach assessments within 24 hours were at 82%, below the 90% target.
- Adult acute bed occupancy exceeded 100%.
- Older adult bed occupancy declined to 85.9%.
- 34.5% of occupied bed days were clinically ready for discharge.
- Out of area placements increased to 36, with 763 bed days.
- PICU placements and bed days rose significantly.
- Cardiometabolic assessments for inpatients were 56.5%, below the 80% target.
Our Community Care
- 83.7% of inpatients were followed up within 3 days (Trust-wide), above the 80% target.
- HCP services follow-up within 3 days was 85.7%.
- Community mental health caseload rose to 3,526.
- Memory service referrals seen within 8 weeks met the 70% target.
- Memory service diagnoses within 12 weeks were 55.6%, above the 50% target.
- EIP/ARMS treatment within 2 weeks was 50%, below the 60% target.
- 67.2% of EIP discharges were to primary care.
- EIP cardiometabolic assessments were 54.3%, below the 80% target.
Clinical Record Keeping
- NHS number recorded for 99.7% of service users.
- Ethnicity recorded for 81.0%.
- Sexual orientation recorded for 46.1%.
- DQMI score remained at 91.3%, below the 95% target.
Cover sheet for Emergency Preparedness, Resilience and Response (EPRR) Board statement of assurance
- Paper title: Emergency Preparedness, Resilience and Response (EPRR) Board statement of assurance
- Date of meeting: 31 July 2025
- Presented by: Joanna Forster Adams – Chief Operating Officer and Accountable Emergency Officer (AEO)
- Prepared by: Sam Grundy – Head of EPRR
This paper supports the Trust’s strategic objective/s (SO):
- SO1 – We deliver great care that is high quality and improves lives.
This paper relates to the Trust’s strategic risks (SR):
- SR1 – Quality including safety assurance processes
- SR4 – Financial sustainability
- SR5 – Adequate working and care environments
- SR6 – Digital technologies
- SR7 – Plan and deliver services that meet the health needs of the population we serve.
Executive summary
The attached document meets the requirement of NHS England EPRR standard 5: “the Board / Governing Body is satisfied that the organisation has sufficient and appropriate resource to ensure it can fully discharge its EPRR duties”.
The Head of EPRR has prepared the attached statement showing the resource allocation to EPRR, the staff directly and indirectly deployed and the arrangements that show that EPRR has the organisational status to undertake its work.
The Accountable Emergency Officer has used this information and other sources of assurance to prepare their statement of assurance to the Board.
With the current level of vacancy and absence; the Trust has insufficient dedicated expert resource to conduct all of the duties required to maintain its current EPRR core standards level of compliance (74%). As AEO I will prioritise our available resource to maintain the statutory essential duties to risk assess, plan, respond and communicate to maintain services safely and respond to incidents – overseen by the Executive Management Team. We aim to mitigate the reduced capacity with the support of colleagues from across the Trust undertaking more direct EPRR work which would ordinarily be undertaken by the EPRR team.
Do the recommendations in this paper have any impact upon the requirements of the protected groups identified by the Equality Act? No
Recommendation
The Board of Directors is asked to approve the statement of assurance.
The Accountable Emergency Officer’s – Board Statement of Emergency Preparedness, Resilience and Response (EPRR) Assurance 2025
1 – Responsibility
As Accountable Emergency Officer (AEO) under the terms of section 46 of the Health and Social Care Act 2012 I have the responsibility for:
- securing that the Trust is properly prepared for dealing with a relevant emergency,
- securing that the Trust complies with any requirements mentioned in this section (of the Act),
- providing the Board with such information as it may require for the purpose of discharging its functions under this section (of the Act).
I am also responsible under NHS England Mandatory Standards (Standard 1) for directing the EPRR portfolio.
2 – The purpose of EPRR
As an NHS funded organisation, the Trust needs to be able to plan for and respond to a wide range of incidents that could threaten health of the community or patient care. The Trust needs to also ensure statutory and regulatory requirements and expectations are discharged as part of its arrangement for managing responses and maintaining resilience.
This work is referred to in the health service as Emergency Preparedness, Resilience, and Response or EPRR. EPRR as defined by NHS England’s Core standards covers the following domains of activity:
- Governance
- Duty to risk assess
- Duty to maintain plans
- Command and control
- Training and exercising
- Response
- Warning and informing
- Co-operation
- Business continuity
- Chemical, biological, radiological, nuclear (CBRN) and hazardous material (HAZMAT).
This statement has been prepared to assure the Board of Directors that EPRR resources and arrangements are adequate to cover the responsibilities mandated under NHS England requirements as required by NHS England EPRR core standard 5.
3 – Statement of resources allocated to EPRR.
3.1 – Direct resources
The Trust’s EPRR complement is:
| Role | Grade | Full/Part time or hours |
| Head of EPRR | 8b | Full time |
| EPRR Manager (post currently vacant) | 7 | Full Time |
| EPRR Officer (part year statutory leave with partial cover in the interim) | 5 | Full Time |
This staffing resource, which was increased in January 2024 with the recruitment of the EPRR manager post, was a significant investment in EPRR and mirrors provision in Bradford District Care NHS Foundation Trust and is similar to Humber Teaching NHS Foundation Trust. This level of provision stands favourably compared with some other mental health and community providers.
The EPRR team has a small administrative budget to cover training materials and courses, stationery, and equipment. Additional resources are made available from the Chief Operating Officer’s budget for larger items of expenditure.
In terms of resources to respond to or manage the consequences of a disruptive event, the EPRR team has agreed a process of allocation of funds and recording expenditure in conjunction with the Deputy Director of Finance. This is:
- One of the EPRR incident team to contact the Deputy Director of Finance or the Associate Director of Finance with details of the incident
- Finance will then release a budget code to the EPRR team
- The EPRR team will use the budget code to incur expenditure
- The Finance team will send weekly financial reports to the EPRR team to advise the total to spend
- Reports on the expenditure will be reported through the Financial Planning Group to the Finance and Performance Committee.
3.2 – Indirect resources
The Trust operates a process of specified business continuity leads for all services. These are nominated by respective directors and cover clinical as well as corporate services. The role of the business continuity lead is to:
- Attend and represent their service at the Trust’s Emergency Preparedness, Resilience and Response Group
- Be a point of contact for those responsible for developing business continuity plans in their respective services
- Encourage the completion of business continuity planning, exercising and review within their services and ensure at least quarterly reporting of progress with business continuity plans at appropriate service governance fora.
A memorandum of understanding for mutual aid was drafted in 2024 to facilitate support to any signatory trust that requires additional trained EPRR staff to support an incident response or to offer advice to any signatory where their EPRR lead is unavailable.
4 – Organisational Status of EPRR at the Trust
The EPRR team requires adequate organisational status to conduct its work and to be able to escalate risk and issues to appropriate tiers of management. The following describes how the Trust has secured the organisational status of the EPRR team:
- The Head of EPRR reports directly to the Chief Operating Officer/ Accountable Emergency Officer. The Head of EPRR also attends the Care Services Delivery and Development Group as part of the care services senior team
- The Head of EPRR attends the Executive Management Team periodically to update the Executive Directors on significant issues regarding EPRR. Additionally, the Head of EPRR will attend the Executive Risk Management Group annually for a formal review of EPRR risks
- The governance group charged with coordinating EPRR work is chaired by the Accountable Emergency Officer and attended by the entire EPRR team
- The Trust has a non-executive EPRR champion. In 2025 this is the Trust’s Chair. The EPRR champion receives copies of all EPRR group papers and meets quarterly with the Head of EPRR. They are also invited to an EPRR group meeting annually.
5 – Capacity and capabilities of the EPRR team
5.1 – The role of the EPRR team
The role of the EPRR team is covered in detail in the Trust’s Business Continuity and EPRR Policy. However, in summary, the main responsibilities of the EPRR team are to:
- Develop plans and procedures with colleagues and with other agencies to respond to disruptive risks
- Train staff in their roles as part of an incident response team
- Facilitate the creation of business continuity plans by all relevant services,
- Advise management prior to, during and after a disruption
- Consult with stakeholders and partners to plan and prepare for disruptions.
5.2 – Relevant Qualifications
The Head of EPRR holds the required Diploma in Health Emergency Planning. The EPRR Officer has completed the award in Health Emergency Planning. If filled, the position of EPRR Manager would require the candidate to hold the required Diploma in Health Emergency Planning or equivalent qualification.
The Head of EPRR and EPRR Officer hold the Level 3 Award in Education and Training (AET) required to be able to train any aspect of EPRR to staff. If filled, the position of EPRR Manager would require the candidate to hold or undertake the Level 3 Award in Education and Training (AET).
5.3 – Capacity to meet EPRR requirements.
Table 1 below represents total available days per the EPRR team staffing complement.
Note: This table shows the capacity of the EPRR Team with the EPRR Manager vacancy held for the full year. It also assumes part cover of the EPRR Officer. This means that total capacity this year is – 443 – this represents a reduction of 215 days against a total capacity of 658 in 2024/25. The current pause on recruitment (except in exceptional circumstances) means that the EPRR team has been operating at this level of resource since 1 April 2025.
Currently it is envisaged that the work undertaken by other colleagues across LYPFT may mitigate some of the impact of this position. Additionally, as work progresses over the summer on the health and care provider alliance review, this may highlight opportunities to work more collaboratively on EPRR across organisations. EPRR specific capacity across LYPFT and LCH is currently at a level below that of similar organisations in the region.
Table 1 – Total available days per current EPRR team staffing complement:
| Staff | Total days | AL | B Hol | available |
| Head of EPRR | 261 | 35 | 8 | 218 |
| EPRR Officer/Maternity Cover | 261 | 28 | 8 | 225 |
Total available: 443.
| Plan areas | Days | Percent |
| Office admin/sickness/leave/bank holiday/vacancy filling/mandatory training | 85 | 19% |
| Contingency/ incident response | 45 | 10% |
| 1. Governance | 33 | 7% |
| 2. duty to risk assess | 12 | 3% |
| 3. duty to maintain plans | 38 | 9% |
| 4. command and control | 5 | 1% |
| 5. training and exercising | 40 | 9% |
| 6. response | 15 | 3% |
| 7. warning and informing | 5 | 1% |
| 8. co-operation | 20 | 5% |
| 9. business continuity | 120 | 27% |
| 10. chemical biological radiological nuclear (CBRN) and hazardous material (HAZMAT) | 25 | 6% |
| Total: | 443 | 100.00% |
The planned days for EPRR cover all required areas of activity with the area of business continuity given highest priority. In 2024/25 the EPRR team recorded how resource was spent against an estimated allocation. The reduction in the size of the team while the EPRR Manager post is unfilled means that time available is reduced across all domains in comparison with 2024/25. The level of reduction for each domain has been made on the basis of risk. Where risks to the Trust’s resilience are identified these will be escalated via the process identified in the EPRR Risk management procedure EP-0014.
A time allowance has been included which is given to contingency/incident response which will represent response to disruptions such as potential business continuity or critical incidents and industrial action.
These time allocations have been reflected in the 2025/26 annual plan against specific topics, plans, and exercises. This plan was presented to the EPRR Group in July 2025.
5.4 – Accountable Emergency Officer statement of assurance
In making the statement I have considered the following:
- The description of resources and plan allocation above
- The significant assurance given by an Internal Audit review in February 2025 about the Business Continuity Management System
- The temporary reduction in EPRR staffing numbers from 1 April 2025 (subject to periodic review by EMT)
- Overview and scrutiny of all EPRR activity via the EPRR Group.
I consider that with the current level of vacancy and absence, the Trust has insufficient dedicated expert resource to conduct all of the duties required to maintain its current EPRR core standards level of compliance (74%). As AEO I will prioritise our available resource to maintain the statutory essential duties to risk assess, plan, respond and communicate to maintain services safely and respond to incidents – overseen by the Executive Management Team. We aim to mitigate the reduced capacity with the support of colleagues from across the Trust undertaking more direct EPRR work which would ordinarily be undertaken by the EPRR team.
In my role as Accountable Emergency Officer, I ask the Board to approve this statement of assurance.
Cover sheet for Emergency Preparedness, Resilience and Response (EPRR) Annual Report 2024-25
- Paper title: Emergency Preparedness, Resilience and Response (EPRR) Annual Report 2024-25
- Date of meeting: 31 July 2025
- Presented by: Joanna Forster Adams – Chief Operating Officer and Accountable Emergency Officer (AEO)
- Prepared by: Sam Grundy – Head of EPRR
This paper supports the Trust’s strategic objective/s (SO):
- SO1 – We deliver great care that is high quality and improves lives.
This paper relates to the Trust’s strategic risks (SR):
- SR1 – Quality including safety assurance processes
- SR4 – Financial sustainability
- SR5 – Adequate working and care environments
- SR6 – Digital technologies
- SR7 – Plan and deliver services that meet the health needs of the population we serve.
Executive summary
The attached document summarises the EPRR teams work over the year from 1 April 2023 to 30 March 2024.
The report covers the major pieces of work done in 2024-25, the increase in compliance against EPRR Core Standards in comparison with 2023-24, NHS Commander Training, Business Continuity and the main disruptive incidents of the year. This report was approved by the Finance and Performance Committee on 22 April 2025.
Do the recommendations in this paper have any impact upon the requirements of the protected groups identified by the Equality Act? No
Recommendation
The Board of Directors is asked to accept the 2024-2025 annual EPRR report, noting the breadth of work carried out during the year, the improvement in EPRR core standards compliance.
Emergency Preparedness, Resilience and Response (EPRR) Annual Report 2024-25
1 – Executive summary
The Trust, as an NHS funded organisation, is required to comply with NHS England’s Core Standards for EPRR. One of these standards requires that the Chief Executive Officer ensures that the Accountable Emergency Officer discharges their responsibilities to provide EPRR reports to the Board, no less than annually. This report meets this requirement and covers the year from 1 April 2024 to 31 March 2025 and was approved by the Finance and Performance Committee on 22 April 2025.
This report shows that in 2024-5 the Trust has increased its compliance with NHSE EPRR Core Standards. Significant work has been undertaken in the areas of Commander Training and Business Continuity. The team has responded to several incidents and events throughout the year.
2 – Report Regarding EPRR Activities in 2024-2025
2024 NHS England EPRR Core Standards
The Trust achieved 74% compliance with core standards in 2024. This is classed as non-compliant but represents a significant improvement over the 26% declared in 2023. The thresholds are:
| Score | Compliance level |
| 100% | Fully Compliant |
| 89%-99% | Substantially Compliant |
| 77%-88% | Partially Compliant |
| Below 76% | Non-Compliant |
Overall, the Trust positions was:
| Category | Compliant | Partially Compliant | Non-compliant |
| Self-assessment reviewed by the ICB | 43 | 15 | 0 |
2.1 – Statement of readiness
2024-2025 started positively with a full complement of staff at 3 WTE. Although the action plan from 2023-2024 EPRR assurance was significantly challenging given the extent of actions and their complexity.
In November 2024 the EPRR Officer started maternity leave mid November 2024 to late September 2025) and while some admin resource was found this did not mitigate the additional duties around EPRR plan areas that the EPRR officer was responsible for. Subsequently in Mid-March 2025 the Chief Operating Officer’s Personal Assistant has been providing support into the team to cover the remainder of the maternity leave. On 31 March 2025 the Resilience Lead and Corporate Business Manager retired from the Trust and his post was taken following interview by the EPRR Manager. To date the EPRR Manager post remains vacant. While this post remains unfilled a negative impact on Trust compliance with EPRR core standards is expected. Further details are provided in the Statement of Assurance.
- Overview of Readiness Activities in 2024-2025
In response to the 2024 EPRR core standards the EPRR team has:
- Business Continuity
The Trust’s maintenance of business continuity plans is showing improvement – many services while having plans are now updating these onto the most recent template. NHS England expect annual revision of all plans.
In 2024/25 Audit Yorkshire conducted an audit to gain assurance that the Business Continuity Management System in place is robust and that the Trust is compliant with the EPRR Business Continuity Core Standards 44-53. An opinion of Significant Assurance was provided for the new Business Continuity Management System (BCMS). The audit was primarily focused on the design of the BCMS where it was found that it was compliant with the Emergency Preparedness Resilience and Response (EPRR) Core Standards, NHSE Business Continuity Toolkit (BCT) and followed best practice. To improve the control environment one recommendation was made relating to enhancing the business continuity training available to appropriate staff. This will be taken forward by the EPRR team in the 2025 workplan.
2.5 – Chemical, Biological, Radiological and Nuclear (CBRN) and Hazardous Materials (HAZMAT)
Work has progressed to improve compliance against EPRR Core Standards for CBRN and HAZMAT. A full risk assessment and training needs analysis was completed in 2024. In 2025 the Trust will have its planning arrangements audited annually by the Yorkshire Ambulance Service HAZMAT/CBRN lead. The Trust will be collaborating with other Mental Health and Community Health providers across the North of England to design a consistent e-learning package for staff. This will ensure costs are minimised. Once training is completed the Trust HAZMAT & CBRN plan will be exercised.
2.6 – EPRR plans, Policies and Procedures
NHS England EPRR Core Standards requires plans and policies to be current (defined as being no more than one year old) and hence all EPRR documents are reviewed, where deemed non-compliant updated with NHS England recommendations and additional plans developed to meet any identified gaps.
Additionally, the EPRR team continue to develop local working instructions to cover processes most recently including recording of Health Commander training and EPRR governance. These are signed off in the EPRR Group.
- EPRR training
Formal training portfolios for Health Commanders at tactical and strategic level are now mandated for NHS organisations. Identification of training requirements and sourcing of some training has been problematic as has getting clarification about exact syllabus requirements from NHSE.
For the Trust approx. 60 staff are required to complete one of the three published portfolios (Those on executive on call – Strategic, those on the clinical manager on call – Tactical and EPRR mangers – EPRR specialist). Portfolios contain on average 12 separate requirements that need to be covered by attendance on courses or provision of written evidence of competence. Training must be undertaken on a repeated basis with some annual and three-yearly refresher courses required.
The EPRR team are assisting those with portfolio responsibilities by giving requisite training and providing updates to staff. The EPRR team has also provided a series of exercises to all tactical commanders within each care group to give them the opportunity to build their understanding and competence. This exercise has also been provided to some strategic commanders. The EPRR team provides the administration of this area of work and provides regular updates to the ICB on take up of training by commanders at all levels.
- Incidents
Industrial Action
Industrial action by medical staff continued until July 2024. As with 2023 the extent of action took up significant EPRR resources and meant other activities had to be postponed as the first half of 2024 progressed.
For all notified action the Trust instituted command and control arrangements centred on the Industrial Action Coordination group chaired by an executive director – normally the Chief Operating Officer. Generally, instances of action were effectively managed, and no adverse consequences occurred in any period of action.
In 2025 the EPRR team also took part in initial planning and reporting on the collective action by GPs. This work is now being led by the Head of Operations for Forensic Services and Head of Operations Community and Wellbeing with oversight from the Chief Operating Officer. To date impacts on Trust services have been minimal.
Civil Unrest
Following the tragic murder of three young girls in Southport in July 2024 waves of violent disorder occurred in other parts of the country with violence aimed at ethnic minority populations and asylum seekers. The level of violence, threat and intimidation was such that it directly affected the Trust’s ethnic minority workforce with some experiencing threatening behaviour and abuse while moving about in our communities or while in their homes.
The Trust raised the issue directly with the ICB and enabled a system wide consideration of risks and ways to mitigate threats to our staff. The Trust itself treated the situation as an ongoing incident implementing incident response arrangements to coordinate work on gathering information about possible threats and coordinate support and advice to staff groups.
The EPRR team linked with ICBs across the north of England recognising that, while Leeds thankfully did not see the violent rioting other cities and towns did, we had staff in these areas who needed information and support.
2.9 – Exercise and Testing
-
Business Continuity Tabletop Exercises
NHS England requirements specify that business continuity plans should be tested annually. This is a major undertaking given the Trust has around 90 separate business continuity plans. A number of exercises were run in 2023-2024 but as part of changes to business continuity arrangements services will be asked to run their own discussion exercises from 2025 onwards with the EPRR team providing larger exercises on a cyclical basis to service lines or to test interconnected business continuity plans.
Plans tested in 2024/25 saw all care services teams undertake a desktop exercise based on a mass casualty incident which tested elements of all business continuity plans within care services. Lessons identified in the exercises were recorded and are to be embedded into existing plans.
3 – Conclusion
2024-2025 was another busy year for the team. Ongoing industrial and collective action posed challenges on team resources to cover meetings, situational reporting, and liaison with all parts of the response. The requirements of delivering and administering the EPRR strategic and tactical commander portfolio training also proved challenging as did the embedding of a new Business Continuity Management System.
While the EPRR team increased to three staff from January 2024 enabling a more effective response this was tempered in March 2025 by the retirement of Andrew Jackson, the Resilience Lead and Corporate Business Manager. Capacity in the team is significantly reduced due to a pause in recruitment and cover of maternity leave that has created a significant reduction in expert/qualified capacity. This will be reviewed in Autumn 2025 following the conclusion of the Provider Alliance review in Leeds and exploration of how we could collaborate across West Yorkshire Provider Organisations on delivery against the EPRR requirements.
4 – Recommendation
The Board of Directors is asked to approve is asked to accept the 2024-2025 annual EPRR report, noting the breadth of work carried out during the year, the improvement in EPRR core standards compliance.
Andrew Jackson – Resilience Lead and Corporate Business Manager (Retired 28 March 2025)
Sam Grundy – Head of EPRR (Effective from 31/03/2025)
Date: 31 July 2025
Chair’s Report from the Quality Committee meeting on 12 June 2025
- Paper title: Chair’s Report from the Quality Committee meeting on 12 June 2025
- Date of meeting: 31 July 2025
- Presented by: Dr Frances Healey, Non-executive Director and Chair of the Quality Committee
- Prepared by: Kerry McMann, Head of Corporate Governance
This paper supports the Trust’s strategic objective/s (SO):
- SO1 – We deliver great care that is high quality and improves lives.
- SO3 – We use our resources to deliver effective and sustainable services.
This paper relates to the Trust’s strategic risks (SR):
- SR1 – Quality including safety assurance processes
- SR2 – Delivery of the Quality Strategic Plan
Committee details:
- Name of Committee: Quality Committee
- Date of Committee: 12 June 2025
- Chaired by: Dr Frances Healey, Non-executive Director
Alert – items to alert the Board to:
- No items to alert the Board to.
Advise – items to advise the Board on
- No items to alert the Board to.
Assure – items to provide assurance to the Board on
- The committee reviewed the BAF, paying particular attention to SR1 and SR2. It was assured that SR1 and SR2 were being adequately controlled and made some suggestions for inclusion at the BAFs next update.
- The committee received a report which outlined the Learning from Deaths data for quarter four of 2024/25 and an annual summary. It was assured on the work ongoing within the Trust to improve mortality reporting and recording and the learning across the organisation.
- The committee considered the Trust’s position against its 2024/25 organisational priorities at the end of quarter four and was assured as to the systems and processes in place for monitoring and supporting the delivery of each priority’s high-level milestones and underpinning tasks.
- The committee received a presentation which provided the highlights of the Older People’s Service’s Annual Quality Report, focusing on how the service had scored itself against the STEEEP dimensions of quality to enable the conditions for high quality care to flourish. Overall, the committee was assured that the service had good systems in place for understanding its quality issues and to drive improvements. The committee was also assured that the Executive Team had a clear understanding of the service’s strengths, weaknesses, challenges and blind spots and how issues were being managed.
- The committee received a presentation which provided the highlights of the Forensic Service’s Annual Quality Report, focusing on how the service line had scored itself against the Learning, Culture and Leadership (LCL) Framework. The presentation also outlined how the service line had scored itself against the STEEEP dimensions of quality to enable the conditions for high quality care to flourish. Overall, the committee was assured that the service line had good systems in place for understanding its quality issues and to drive improvements, and good knowledge of its strengths and weaknesses in relation to learning, culture and leadership. The committee was also assured that the Executive Team had a clear understanding of the service line’s strengths, weaknesses, challenges and blind spots and how issues were being managed.
- The committee received a report which provided an update on the development of a trustwide strategy on self-harm and suicide prevention. It acknowledged the work that had taken place in response to the NICE guidance on self-harm and supported the plan to develop a trustwide strategy, along with the development of a procedure and training for staff.
- The committee reviewed the NCISH Trust Safety Scorecard for 2025 which provided key indicators and benchmarking data designed to support quality improvement. It noted the 100% completion by the Trust of NCISH questionnaires, compared to a national rate of 91%, and agreed this was excellent practice that should be commended.
- The committee received and discussed the Restrictive Interventions Annual Report 2024/25. Dr Healey welcomed the reduction in the use of physical restraint compared to 2023/24 but acknowledged that quality committee had previously discussed levels of physical restraint used in 2023/24 were higher than in previous years, partly due to a small number of patients with exceptional needs. She suggested that the work undertaken around reducing physical restraint in nasogastric feeding could be shared with NHS England as a positive case study.
- The committee received and discussed a report which provided data on the number of incidents of patients being classed as absent without leave (AWOL), absconding or missing from inpatient services between 1 April 2024 and 31 March 2025 and outlined the work being undertaken within the Trust to manage these incidents. It was agreed that an annual report should be provided on the management and prevention of AWOL incidents, plus any harm that occurred as a result of the incidents. The committee asked for clarity as to the appropriate governance route for this report (formal action).
- The committee reviewed and discussed the results of the committee effectiveness questionnaire. It agreed that it remained effective and acknowledged that, although further developments were not required at the present time, it would continuously seek to improve its effectiveness.
Refer – Items to be referred to other Committees:
- Workforce Committee – The committee acknowledged that the Restrictive Interventions Annual Report referred to workforce challenges, including levels of vacancies, agency and bank use, as likely having contributed to the use of restrictive practices in some services, despite overall reductions between 2023/24 and 2024/25. It agreed to refer this to the Workforce Committee for further consideration of this issue.
Recommendation
The Board of Directors is asked to note the update provided.
Chair’s Report from the Quality Committee meeting on 10 July 2025
- Paper title: Chair’s Report from the Quality Committee meeting on 10 July 2025
- Date of meeting: 31 July 2025
- Presented by: Dr Frances Healey, Non-executive Director and Chair of the Quality Committee
- Prepared by: Kerry McMann, Head of Corporate Governance
This paper supports the Trust’s strategic objective/s (SO):
- SO1 – We deliver great care that is high quality and improves lives.
- SO3 – We use our resources to deliver effective and sustainable services.
This paper relates to the Trust’s strategic risks (SR):
- SR1 – Quality including safety assurance processes
- SR2 – Delivery of the Quality Strategic Plan
Committee details:
- Name of Committee: Quality Committee
- Date of Committee: 10 July 2025
- Chaired by: Dr Frances Healey, Non-executive Director
Alert – items to alert the Board to:
- No items to alert the Board to.
Advise – items to advise the Board on
- The committee received the Safeguarding Team’s Annual Report for 2024/25. It expressed concern at the findings from the domestic abuse, stalking, harassment and honour-based violence (DASH) It requested a report to outline the barriers identified to staff completing the DASH form and assurance on the work that will be undertaken to improve compliance in this area (formal action).
Assure – items to provide assurance to the Board on
- The committee reviewed an extract from the Board Assurance Framework (BAF) which detailed strategic risks one and two so that it could be mindful of its responsibilities to assure that these risks were being adequately controlled throughout the course of the meeting.
- The committee received the Annual Report of Infection Prevention and Control and Antimicrobial Stewardship for 2024/25 and the IPCBAF. It was assured on the activity of the IPC Team and thanked the team for its work during 2024/25. It was also assured that the Trust continued to follow all national infection, prevention and control guidance and that the Director of Infection, Prevention and Control had oversight of outbreak management within the Trust. The committee acknowledged the extensive activity and improvement work outlined within the report, which included:
- IPC policy and procedural documents being reviewed and updated to align with the National Infection Prevention and Control Manual.
- A significant reduction in airborne transmission outbreaks such as influenza and covid-19 compared to 2023/24.
- Overall antibiotic use remaining low within the Trust in comparison to acute trusts. Antimicrobial stewardship within the Trust optimised safe, appropriate, and economic use of antimicrobial agents. This has led to improved patient outcomes from infection while minimising negative consequences such as healthcare associated infections and the development of antimicrobial resistance.
- The committee reviewed two presentations which provided the highlights of the CONNECT Eating Disorder Service’s and the Community Rehabilitation Enhanced Support Team’s Annual Quality Reports, focusing on how the services had scored themselves against the Learning, Culture and Leadership (LCL) Framework and the STEEEP dimensions of quality to enable the conditions for high quality care to flourish.
- Overall, the committee was assured that the services had good systems in place for understanding their quality issues and to drive improvements, and good knowledge of their strengths and weaknesses in relation to learning, culture and leadership. The committee was also assured that the Executive Team had a clear understanding of the services’ strengths, weaknesses, challenges and blind spots and how issues were being managed.
- The committee received an update on the development of the quality dashboard and the work being undertaken against the Quality Strategic Plan. It was agreed that a report would be provided in October 2025 to outline the aligned measures that would be shared with the quality committee as part of the future quality dashboard (formal action).
- The committee received the Safeguarding Team’s Annual Report for 2024/25. It was assured that the Trust prioritised the safety of all children and adults at risk who are or whose parents or carers were in receipt of services. It was also assured that the Safeguarding Team supported the Trust in meeting its statutory requirements for Safeguarding. It acknowledged the extensive activity and improvement work outlined within the report, which included:
- Working with the Risk Assessment and Safety Planning Project Group to ensure routine enquiry was embedded within the Risk and Management Plan, which included providing guidance for staff on how to complete routine enquiry and providing lunch and learn sessions available to all Trust colleagues.
- The findings from the Voice of the Adult clinical re-audit, which sought to ascertain whether adults’ views and wishes in relation to safeguarding concerns were being sought by practitioners, documented, and addressed accordingly. Of the 50 safeguarding contact forms audited, 94% of cases showed that the adult’s views and wishes were sought by practitioners and recorded in the safeguarding contact form.
- The development of a training package to address how to make a good quality referral when requesting support from Adult Social Care and the delivery of this training to by the Interim Head of Safeguarding along with ICB colleagues to an audience of participants from across all services in Leeds.
Refer – Items to be referred to other Committees:
- Workforce Committee – Following the discussion on the challenges being faced around fit testing compliance, it was agreed that the Workforce Committee should consider whether bank shifts should be withheld until fit testing had been completed.
Recommendation
The Board of Directors is asked to note the update provided.
Cover sheet for LYPFT 2 Month Safer Staffing Review Report
- Paper title: LYPFT 2 Month Safer Staffing Review Report
- Date of meeting: 31 July 2025
- Presented by: Nichola Sanderson, Director of Nursing
- Prepared by: Alison Quarry, Deputy Director of Nursing
Miriam Blackburn, Head of Nursing
Jennifer Connelly, Professional Lead Nurse
Adele Sowden, E-Rostering Team Manager
This paper supports the Trust’s strategic objective/s (SO):
- SO1 – We deliver great care that is high quality and improves lives.
- SO2 – We provide a rewarding and supportive place to work.
- SO3 – We use our resources to deliver effective and sustainable services.
This paper relates to the Trust’s strategic risks (SR):
- SR1 – Quality including safety assurance processes
- SR2 – Culture and environment for the wellbeing of staff
Executive summary
This paper draws on the NHS National Quality Board (2016) reporting requirements to ensure that nursing and care staffing, capacity and capability is enabled to deliver high quality care and the best possible outcomes for patients whilst balancing quality and financial objectives and acknowledging the ongoing pressures experienced in relation to staffing and resource.
The paper contains a high-level overview of data and analysis to provide the Board of Directors and the public with information on the position of Leeds and York Partnership Trust wards staffing against safer staffing levels between 1st April to 31st May 2025 including unify data for March 2025.
This report details that 1 clinical shift during that period did not have a registered nurse and outlines the mitigations in place to ensure patient safety.
The paper draws focus to 4 clinical areas where there is either significant Registered Nurse and Health Support Worker vacancies or are using significantly higher numbers of staff above the planned establishment and provides data to demonstrate the impact through a series of quality indicators outlining any mitigation or workstreams to support the current workforce challenges. Not include embedded items anywhere in the cover sheet.
Do the recommendations in this paper have any impact upon the requirements of the protected groups identified by the Equality Act? No
Recommendation
The Board is asked to:
- Note the content of the report.
- Be assured that arrangements are in place to monitor, support and mitigate any impact of reduced staffing levels or skill mix in relation to patient safety.
Safer Staffing: Inpatient Services – March, April, and May 2025
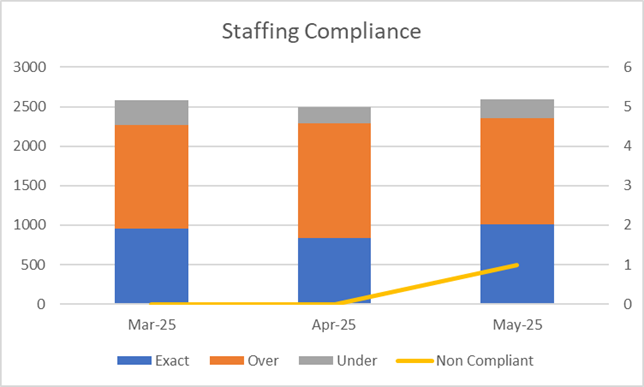
Number of Shifts
| Compliance | March | April | May |
| Exact | 960 | 838 | 1009 |
| Over Compliance | 1310 | 1454 | 1341 |
| Under Compliance | 310 | 206 | 241 |
| Non-Compliant | 0 | 0 | 1 |
Risks: Registered Nurse vacancies continue to be a major theme across the focussed areas highlighted by the Unify data (Appendix A).
Mitigating Factors:
Reduced Registered Nurse fill rates are being partially mitigated in many of our units by increasing Healthcare Support Worker (HSW) duties through temporary staffing to reach minimum staffing numbers. Ongoing improvements to the recruitment strategy and a multi-professional approach to a review of establishments, continues to be progressed.
Narrative on Data Extracts Regarding LYPFT Staffing Levels on x28 Wards during May 2025: This is the whole time equivalent (WTE) number of staffing posts the inpatient wards are funded for to deliver planned level of care and interventions within their speciality by shift.
Staffing Compliance: This tells us whether the wards met the planned numbers of staffing during a shift. The planned staffing numbers do not necessarily reflect the actual staffing need on any given duty as this may fluctuate dependent on current patient group and need.
Exact or Over Compliant shifts: The compliance data demonstrated an increase in the number of shifts which were staffed exactly as planned in May 2025. There was a decrease in the number staffed above the planned establishment of Registered Nurse and Health Support Worker duties during the month of May 2025. The largest proportion of clinical shifts are working over the planned establishment.
The staffing escalation and deployment protocol which was developed as part of the staffing escalation workstream is currently being embedded in practice across inpatient areas. The protocol will provide assurance that the correct steps for escalation of staffing shortfalls has occurred to support timely resolution, which in turn is anticipated to reduce reliance on temporary staffing. The work carried out aimed to understand developed cultures around different professions and roles on our inpatient wards. The group considered the cultural shift required to support and facilitate inpatient teams to use their workforce flexibly and effectively, in line with the Trust staff escalation protocol.
Under Compliant Shifts: There was a decrease in the number of clinical shifts that were working under the planned establishment in April and May 2025 in comparison to March 2025.
(Note this differs from the unify report in Appendix A which shows the total hours over the month rather than on a shift-by-shift basis).
Non-Compliant Shifts:
This metric represents the number of shifts where no Registered Nurses were on duty. On the 14th May at 2 Woodland Square due to sickness absence there was no Registered Nurse for the late shift. The Band 4 Nurse Associate was able to act as shift co-ordinator and administer medication which falls within their scope of practice with oversight from the Registered Nurse working at 3 Woodland Square.
MHOST
Four MHOST data collections have now been completed since the tool was reintroduced in LYPFT, with a further collection scheduled for September 2025. The MHOST tool is not applicable to the Learning Disability settings and therefore has not been used in Woodlands Square. Due to staff numbers and change in the leadership teams across our inpatient services, a small number of inpatient areas have required additional training on the MHOST tool and its application to practice.
This evidence-based tool provided the initial data to begin workforce planning; it is recommended that MHOST data alongside professional judgement and quality indicators is used to complete staffing establishment reviews. A minimum of two data collection periods are recommended prior to making changes to workforce establishment. Application of this evidence-based tool provides some quality assurance to this process. This data cannot be used in isolation and should always be triangulated with professional judgement and quality indicators.
All inpatient areas will begin preparing for the second establishment review which is due to commence in October 2025. The reviews will focus on identifying whether the current planned establishment across inpatient wards remains appropriate to deliver safe and effective care through the application of the triangulated approach, including MHOST data, quality outcomes and professional judgement. Following the completion of the first annual establishment review work was commenced to understand the use of observation and engagement and how this impacted on staffing numbers prior to any changes to establishments being made in those areas where the data suggested. This is referred to in more detail later in this report.
Service Area Updates
Sickness Absence
The chart below demonstrates the sickness rate (%) for each inpatient area in May 2025 and of those periods of sickness, what percentage is related to stress/mental health as reported on the E-Rostering system. Service lines have been reported together and provide an average across the wards.
Across the services, YCED, Mill Lodge and Woodlands Square have reported sickness absence levels below the Trust target of 5%. Stress/mental health sickness absence accounts for all absence related to stress/mental health and is not only work-related stress.
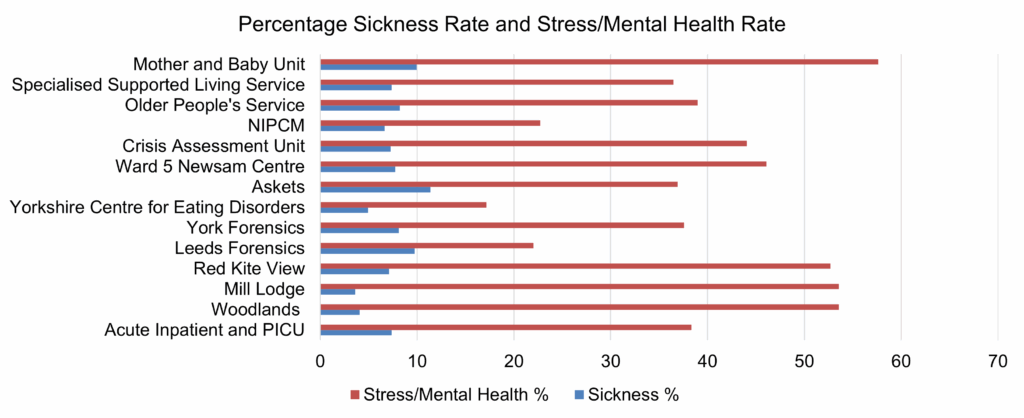
Vacancies
Below indicates the number of vacancies across each service as reported on ECHO in May 2025. This is across the multidisciplinary teams and not solely related to Registered Nurses and Health Support Workers, which are roles traditionally viewed in the safer staffing figures.
Although Registered Nurses and Health Support Workers are those reported in the establishment figures, it is important to recognise the range of roles within the multidisciplinary teams for providing safe and effective care in our ward environments and this is not captured in the unify data.

The chart below demonstrates the vacancy rates for Registered Nurses and Occupational Therapists (WTE) across services. This information is a snapshot and taken from the finance data using budgeted establishment for these roles and the vacancy information for May 2025. There has been successful recruitment of 33 preceptees into the inpatient wards which will see RN vacancies across many of the wards reduce into autumn and winter. Where vacancies remain, there will be on-going recruitment of RNs outside preceptorship, with a number of wards having recent successful recruitment of Band 5 RNs with a range of post registration experience.
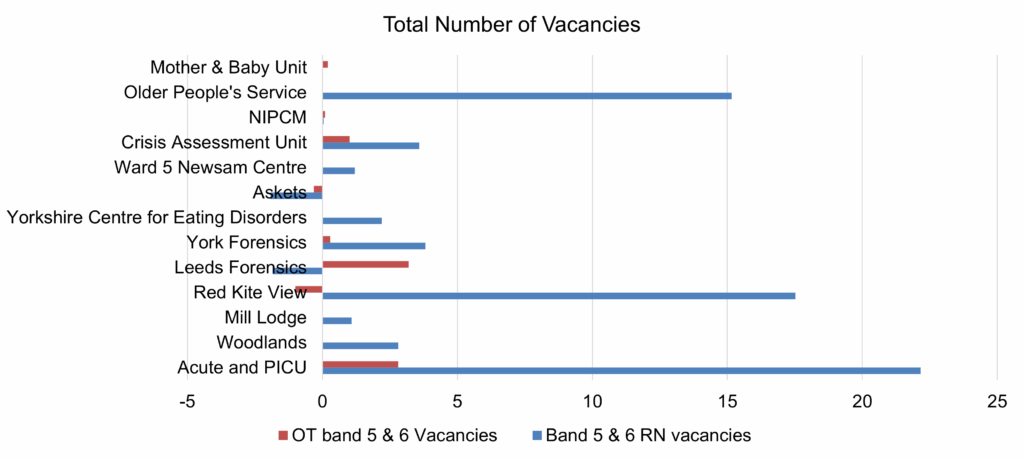
The chart below demonstrates the vacancy rates for Health Support Workers and Nursing Associates (WTE) across services. This information has been taken from the finance data using budgeted establishment for these roles and the vacancy information for May 2025. Some services such as NIPCM and Crisis Assessment Unit do not have Nursing Associates in their staffing establishment.

Due to the varied headcount of the services covered, the chart below has been included to show the vacancies for Registered Nurses and Health Support Workers by percentage.
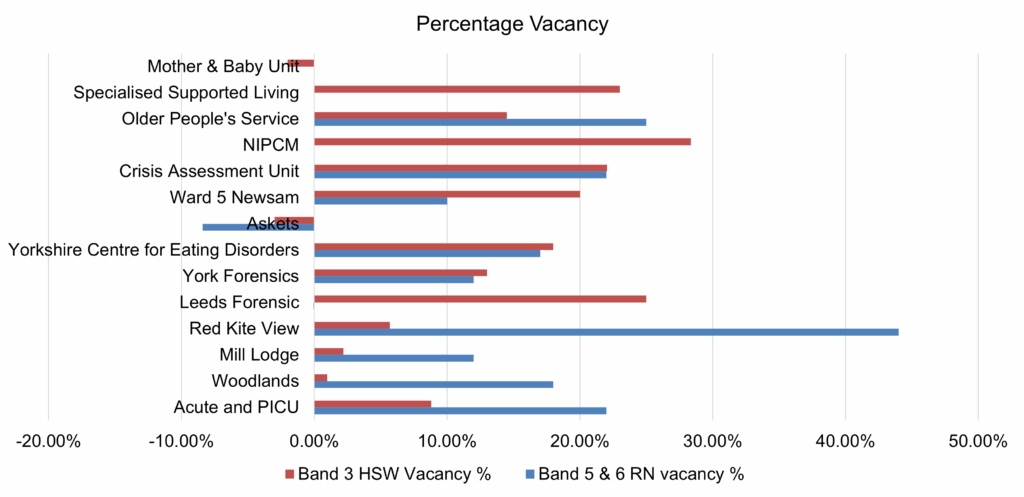
Acute Inpatient and PICU
The overall vacancies across the Acute Inpatient and PICU Service have increased slightly at 43 WTE (17%) in May 2025 with staff turnover at 4.92%. However, the number of Registered Nurse vacancies is predicted to fall in the coming months with Preceptee Nurses and successful applicants from a recent recruitment event commencing in post. A further recruitment event is also scheduled for the remainder of the Registered Nurse vacancies.
The Registered Nurse vacancies are also supported by Registered Nursing Associates; however, these roles are not currently captured in the unify data within their own role. Work is being carried out through the safer staffing forum to explore how these roles can be more effectively recorded on the system. The vacancy rate for Nursing Associate positions has recently reduced; four Trainee Nursing Associates have recently completed their training and commenced position as a Nursing Associate within the service. Nursing Associates play a valuable role in mental health inpatient settings by bridging the gap between Healthcare Assistants and Registered Nurses, providing a wider range of care, and supporting the focus of Registered Nurses on more complex duties.
The requirement for additional staffing above the planned establishment has been required within both the Female and Male Acute Wards. The Female Acute Wards have experienced the need to use enhanced levels of observation and engagement and escort status to support patient care, particularly to support service users who self-harm. This correlates with a higher number of incidents being reported in the Female Acute Wards during the data collection period, with the highest proportion of these being self-harm, violence, and aggression incidents. All staff continue to be supported to attend the Knowledge and Understanding Framework (KUF) training to ensure staff have the required skills to support the clinical presentation. The service has also recently recruited to the Consultant Psychologist position which has been vacant for some time, this role will provide specialised psychological expertise to enhance patient care, staff support, and service development.
The charts below demonstrate the supervision, appraisal and compulsory training rates for April and May 2025. Although the Acute Inpatient and PICU Service have not met the Trust target of 85% for both clinical supervision and appraisals, the service has consistently reached the target for mandatory training and compliance for Appraisals has continued to increase. Compliance for Appraisals has steadily increased over recent months with it reaching 77% in May 2025 in comparison to 56% in January 2025. Clinical supervision compliance increased to 62% in May 2025, however the overall compliance rate has been impacted by a falling rate of compliance in the PICU which has been impacted by sickness and other staffing challenges. This workforce data was recently discussed in the ward level and service line operational meetings with the aim of overcoming the challenges faced to achieving these targets and improving compliance. Clinical restorative supervision groups continue to be offered across all wards within Acute Inpatient and PICU Service.
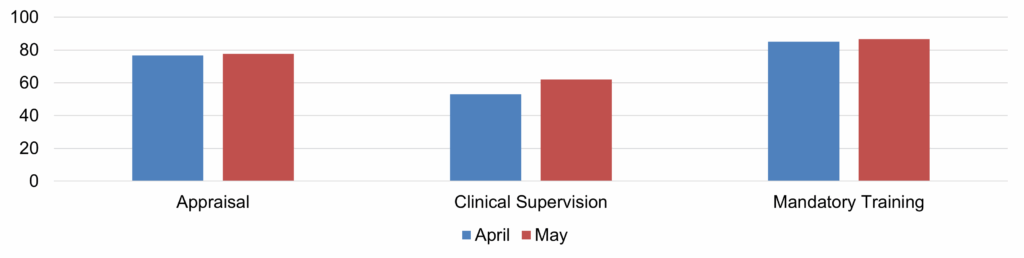
The table below demonstrates the number of incidents across the Acute Inpatients and PICU Service for the reporting period. The reduction in the total number of patient safety incidents reported in the previous two months report has been sustained. The highest number of patient safety incidents falls within either self-harm, violence, and aggression, this is consistent with previous months data.
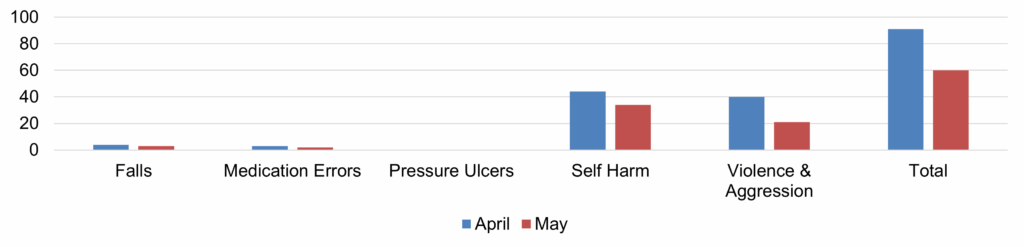
The Acute Inpatient and PICU Service received fifty Have Your Say responses in April and May 2025. Twenty-four responses reported care as “very good,” nine as “good,” six as “ok,” one recorded “don’t know” and nine reported as either “bad” or “very bad.” There were five complaints registered during the reporting period.
The fill rate monthly indicator (Unify) data demonstrates that the service maintained a minimum of 78% Registered Nurses during the data collection period and has achieved close to 100% for most clinical shifts. An increase in Registered Nurse sickness rate in PICU (28.7%) and Ward 4 Becklin (19.4%) alongside existing vacancies has impacted where the fill rate has not been met. This data does not reflect the total amount of care provided and the fill rate only includes those roles which are part of the planned establishment. Although we have on occasion seen less than 100% of Registered Nurses fill rate, it has not accounted for other roles such as Practice Development, Allied Health Professionals and Ward Manager. The fill rate data, although includes Nursing Associates, does not identify them as their own staff group and they are incorporated into the unregistered fill rate. Work is progressing through the Safer Staffing Steering Group to identify a system solution to resolve this issue.
The fill rate monthly indicator (Unify) data also demonstrates that the service have significantly exceeded the unregistered need above the planned establishment throughout the data period. A proportion of the increase of unregistered staff can be attributed to backfilling Registered Nurse duties with Healthcare Support Workers, however the high level of staffing has been consistent over a period of time and is being reviewed as part of the acute inpatient establishment review.
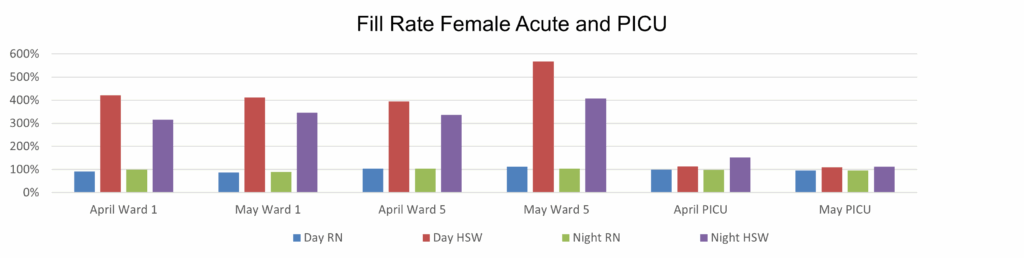
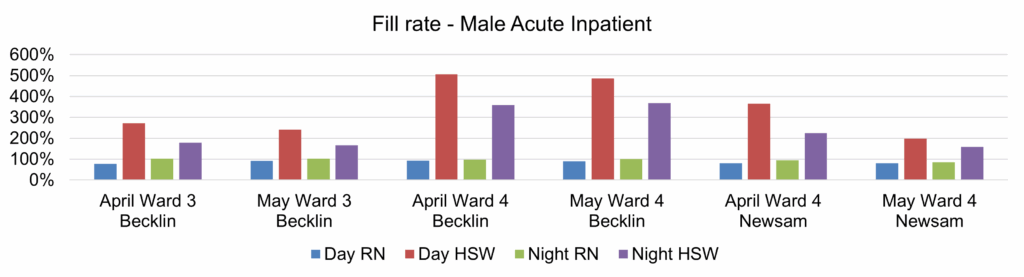
Older People’s Services
Since May 2024, there has been a significant reduction in Registered Nurse vacancies from 24.36 WTE (41.32%) to 15.16 WTE (25%) in this reporting period. This is a positive reduction through both standard recruitment processes and preceptee allocation. There is due to be a significant reduction in Registered Nurse vacancies over the summer and into autumn.
The service also has staff in Band 4 positions across the wards in both Nurse Associate and Assistant Practitioner roles supporting the service users as part of the establishment, which is not reflected in the vacancy data for Registered Nurses and Health Support Workers. The service continues to support colleagues to complete qualifications to become Nursing Associates, further building the workforce.
The team includes Allied Health Professions in the ward environment delivering profession specific interventions and providing care and support of the service users on the ward. There are currently no Occupational Therapy vacancies within the wards. The service has activity coordinators in post across the wards who support with therapeutic activity.
The below charts demonstrate the supervision, appraisal and compulsory training rates for April and May 2025. Although the Older’s People’s Service have not met the Trust target of 85% for both clinical supervision and appraisals, the service has consistently reached the target for mandatory training Maintaining good levels of appraisal, compulsory training and supervision can have a positive impact on patient care and staff wellbeing. Development work continues in these areas.
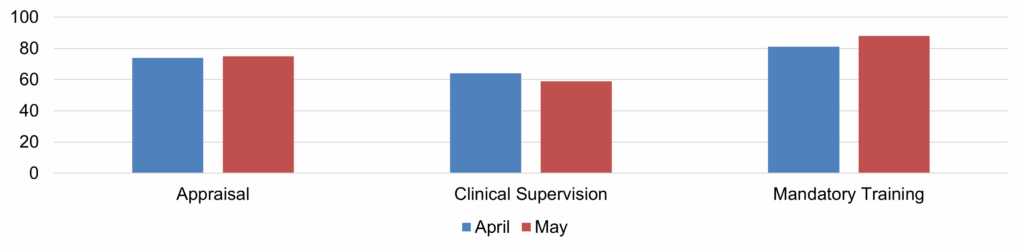
Below is the incident data for the service within the reporting period. There was a small overall reduction in these types of incidents between April and May, seeing fewer falls and an increase in medication error, which were spread across the wards and not concentrated in one area.
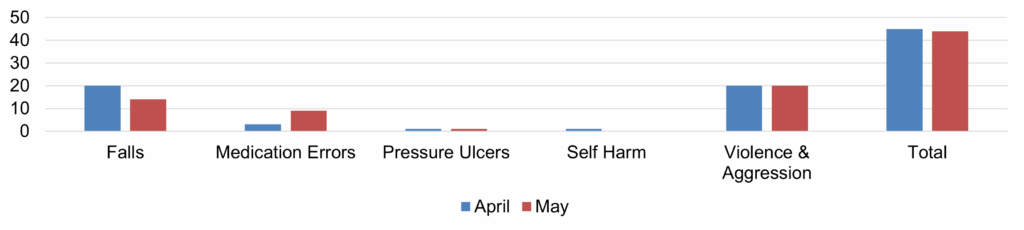
The fill rate monthly indicator (Unify) data demonstrates that the service maintained a minimum of 88% Registered Nurses during the data collection period and has achieved close to or above 100% for the majority of clinical shifts. This data does not reflect the total amount of care provided and the fill rate only includes those roles which are part of the planned establishment. The fill rate data, although includes Nursing Associates does not identify them as their own staff group. The unify data does not include the wider multidisciplinary team. Where figures are below the expected fill rate, such as on Ward 3, this does not account for the presence and care delivered by other professionals such as the Ward Manager, Allied Health Professionals, and the wider MDT.
The fill rate monthly indicator (Unify) data also demonstrates that three of the four wards have exceeded the unregistered need above the planned establishment throughout the data period. Increased staffing above the establishment can be for a range of reasons, one of those highlighted by the team at the Mount has been around supporting the physical health needs of service users during the reporting period.
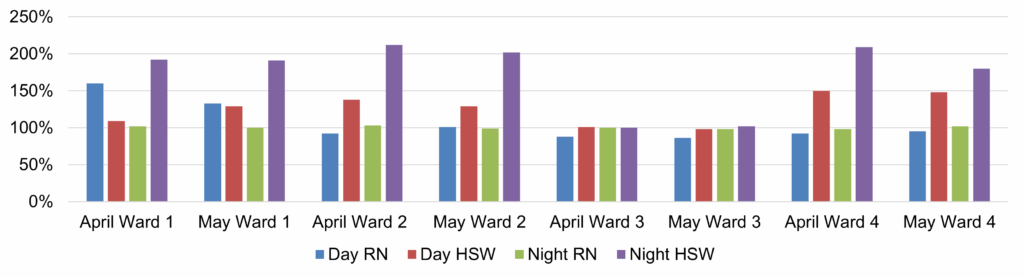
The Older Peoples Service received one complaint during the reporting period and fifteen responses to “Have Your Say.” The Have Your Say feedback reported that care was “very good” in 7 cases, “good” in 5 cases, “ok” in 2 and one stated “don’t know”.
Red Kite View (Skylark and Lapwing)
Since the last reporting period there has been a reduction in Registered Nurse vacancies by 2 WTEs. There are a number of Registered Nurses in the recruitment pipeline, including preceptees who will join Red Kite View in the coming months, further reducing the Registered Nurse vacancy figures across the two wards. Within Red Kite View there are Health Support Workers and Nursing Associate colleagues completing training to become Registered Nurses in the future. Red Kite View continues to support staff to complete Nursing Associate and the top up to a nursing route to build capacity within the service in the long term.
The Registered Nurse vacancies are supported by Nursing Associates who are not currently captured in the unify data as a separate role and are incorporated into the unregistered fill rate. The service also has additional Band 4 Health Support Workers, further increasing safer staffing numbers.
Red Kite View continues to have a high percentage of Registered Nurse vacancies across the two wards. However, there are a significant number and range of professionals who work within the multidisciplinary team who provide care to the young people within the service and ensure that there are adequate numbers of staff available each day with a range of skills and experience.
Following successful recruitment of Health Support Workers, the Band 3 Health Support Worker vacancies have fallen from 9.79 in the last reporting period, to 1.95 WTE. This has included colleagues who worked within our temporary staffing workforce taking up substantive roles in the service.
The service uses temporary staffing to support the wards where there may be vacancies or if increased staffing is required above the baseline establishment. The service has a number of both registered and non-registered temporary staff who work regularly in the service through block booking shifts supporting both the continuity of care and increasing the numbers of Registered Nurses on duty.
The below data demonstrates the current compliance figures for appraisal, clinical supervision, and mandatory training. Compulsory training figures remain consistently above the Trust target of 85% across both wards supporting staff to deliver safe care. The clinical supervision figures for Skylark reduced between April and May. The leadership team are maintaining oversight and supporting teams to access supervision through targeted work. It is understood that at times supervision is complete but not recording, impacting on the figures on ECHO. Skylark has a weekly reflective space and on monthly team core days, colleagues have access to reflective practice and care planning groups. The appraisal rate on Skylark had fallen below 70% in both April and May, to support ensuring that colleagues have a regular appraisal, the management supervision structure has been reviewed and discussed within the charge nurses time out day.
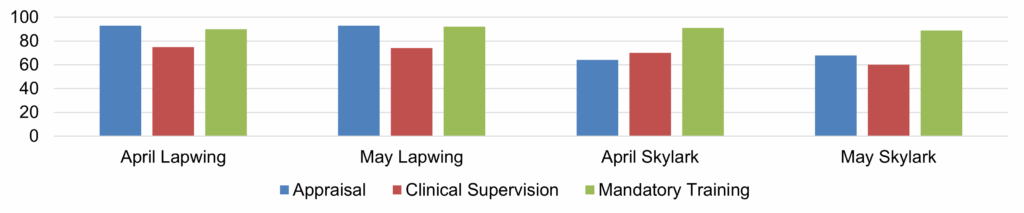
The graph below demonstrates the total number of patient safety incidents across Red Kite View that fall under the categories of falls, medication errors, pressure ulcers, self-harm and violence and aggression for the reporting period. There was an increase in self-harm between April and May 2025. March and April had seen lower numbers of self-harm incidents reported since June 2024 and the increase in May relates to a small number of service users.
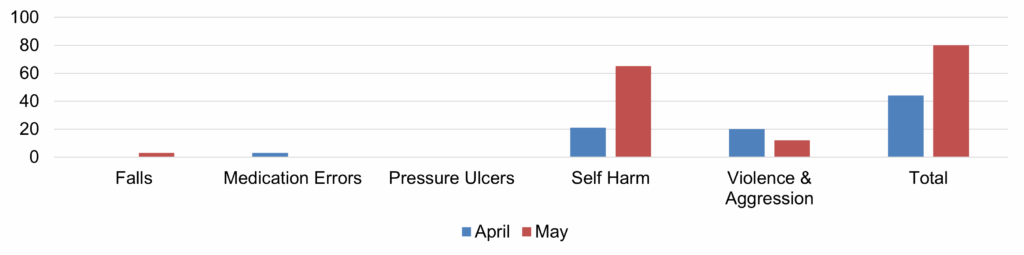
There was no Have Your Say feedback or complaints for Red Kite View in April or May this year.
The fill rate monthly indicator (Unify) data demonstrates that the service have maintained a minimum of 78% Registered Nurses on Lapwing during the data collection period and 83% on Skylark. The sickness rate for Registered Nurses during May was 9.9% on Lapwing and 16.2% on Skylark, both above the Trust target. There are a range of support offers available within the service to support staff well-being at work. Sickness absence along with Registered Nurse vacancies on the ward has impacted on the fill rate. Increased numbers of Health Support Workers have been used to backfill unfilled Registered Nurse posts where needed. Red Kite View work with a wide multidisciplinary team, bringing a range of skills to the team to support service users. This data does not reflect the total amount of care provided and the fill rate only includes those roles which are part of the planned establishment.
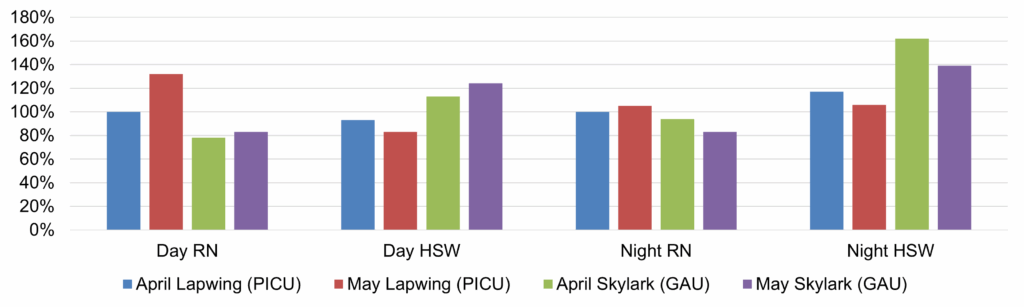
Specialised Supported Living Service
The Specialised Supported Living Service (SSLS) provides accommodation to individuals with learning disabilities and complex health needs at 16 locations across Leeds. The service is predominantly staffed with Support Workers (Band 3) or Senior Support Workers (Band 4). The service is funded by Adult Social Care for 250 WTE; 90% of this workforce is made up of either Senior or Support Workers, the remaining 10% being either Band 6 or 7 staff (registered and non-registered) who hold more of an operational focus and leadership role within the service. The current Support Worker vacancies are mitigated through a combination of substantive staff working additional bank shifts and temporary staffing.
The Service recently recruited 5 Apprentice Support Worker who have commenced position and have been a positive addition to the team. These development posts opened up recruitment to applicants who importantly have the right values but who do not necessarily have the required skills and competencies at this time. The apprenticeship option will support these applicants in achieving the skills and competencies to deliver safe and effective care.
Unfortunately, the last recruitment campaign for Band 3 Health Support Workers was unsuccessful, the successful candidates withdrew due to changes in government guidance on sponsorship. A further recruitment campaign is due to commence soon for both Band 3 Health Support Workers and Band 4 Senior Support Workers. Various recruitment initiatives are being coordinated within the service. The service has had further success in Bank to substantive Health Support Worker recruitment; this has enabled the recruitment of a cohort of experienced Health Support Workers.
The chart below demonstrates the clinical supervision, appraisal, and mandatory training for the SSLS across the reporting period. There has been a slight increase in compliance with Appraisals and Mandatory Training in comparison to the previous 2 months. Compliance for Clinical Supervision achieved 100% for May 2025. Turnover has remained significantly below target of 10% during the data collection period at 1.88%.
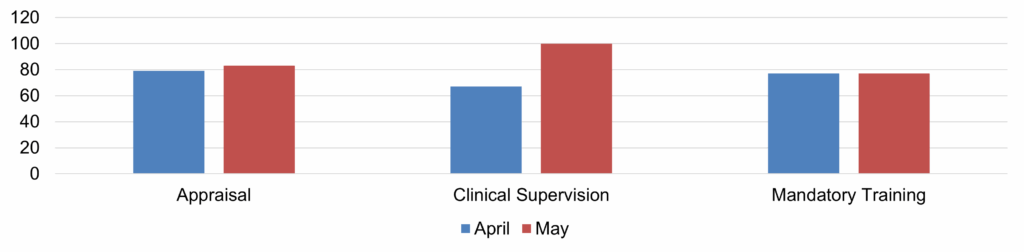
The below table demonstrates the number of patient safety incidents in the SSLS during the reporting period. This demonstrates a slight increase in the number of incidents over the 2-month period in comparison to the previous 2 months. The highest number of incidents in this service area fall under falls and violence and aggression incidents. The service recently commenced a focused piece of work looking at medication safety within the service, with a noted sustained reduction in medication related incidents over several months.
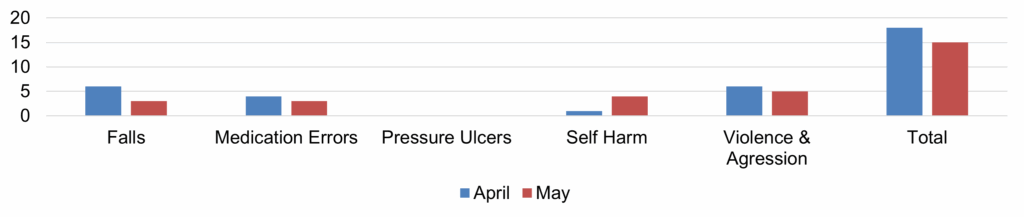
SSLS received no complaints during the data collection period and there were no open complaints to the service during this period. The service holds an annual Have Your Say event which offers various approaches to providing feedback. A detailed report is generated following these events and shared widely. The feedback is also discussed in the service line governance meeting to ensure learning and reflection on feedback.
Enhanced Therapeutic Observations and Care Programme (ETOC)
Observations and engagement are often used within mental health inpatient settings as an intervention to support and manage a person’s care, safety, and wellbeing. An increase in the use of therapeutic observations and engagement has become evident within our inpatient services over recent years particularly since the pandemic which has also been reflected nationally. Enhanced observations are often the reason that ward staffing is increased above the baseline establishment and additional staff are required on duty.
Over the next 12 months, LYPFT will be participating in a national programme focused on improving our approach to therapeutic observations and engagement within our inpatient services. The work aims to implement a set of best-practice principles that recognise enhanced observations as inherently restrictive practice and potentially harmful, despite their safety intentions. This will result in a full review of our current procedure and training package to incorporate the 14 key principles described within the associated guidance.
The programme has 5 aims set out by NHS England, which are:
- Person-centred approach to reducing harm and patient experience: Promoting a person- centred approach and training for staff to identify alternate plans of care to meet the patients needs.
- Enabling and supporting families and carers: Support reduced lengths of stay in hospital and providing patients, families, and carers with confidence that care is joined up and meets the patients needs.
- Effective education and training initiatives to support workforce utilisation: Provide appropriate training to staff, ensuring they have the right skills and competencies to provide effective enhanced therapeutic observations and care.
- Improving workforce efficiency and staff experience: Organisations being provided with tools to assess enhanced therapeutic observation and care requirements and manage staff resourcing.
- Reducing reliance on temporary staffing spend: Reducing reliance on temporary staffing through planning local workforce deployment models and developing escalation points and triggers.
This initiative will be overseen by the Positive and Safe Working Group and regular updates provided.
Summary
An overall improvement in relation to the workforce continues to be noted. However, a small number of services continue to experience some challenges in this area with a higher number of vacancies which are further compounded by sickness. However, positively a reduction in overall vacancies for inpatient areas is evident with this predicted to continue to improve over coming months following recruitment campaigns and Preceptee Nurses who will join inpatient areas. In several clinical areas, there has been the need for additional staffing above the planned establishment to deliver safe and effective care particularly to support service users requiring enhanced observations. Staffing pressures are currently mitigated through the combination of temporary staffing and substantive staff working additional duties.
The delivery of care through the multidisciplinary team and the professional specific roles which is not captured in the planned staffing establishment should be considered when reviewing the data. Workstreams commissioned through the Safer Staffing Forum continue to progress which are focused on a cultural shift moving away from viewing inpatient staffing in the traditional roles of Nurses and Health Support Workers and toward an integrated MDT approach to focus on improving the quality of care delivered to our service users. This work focused on developing a set of principles for clinical areas to use to effectively support this approach, these principles have recently been finalised and will be shared within clinical areas going forward. The recently developed staffing escalation and deployment protocol is currently being embedded across inpatient areas, which will further support the required cultural shift and in turn an anticipated reduction in the number of increased duties above planned establishment and increase in the quality of care delivered.
Recommendations:
The Board is asked to:
- Discuss and note the content of the report.
- Be assured of the arrangements in place to monitor, support and mitigate the impact of reduced staffing levels and skill mix in relation to quality and safety in inpatient setting.
Appendix A:
Safer Staffing: Inpatient Services March 25
Fill rate indicator return
Staffing: Nursing, Care Staff and AHPs
Allied health professionals refers only to Occupational therapists that are included in the ward establishment.
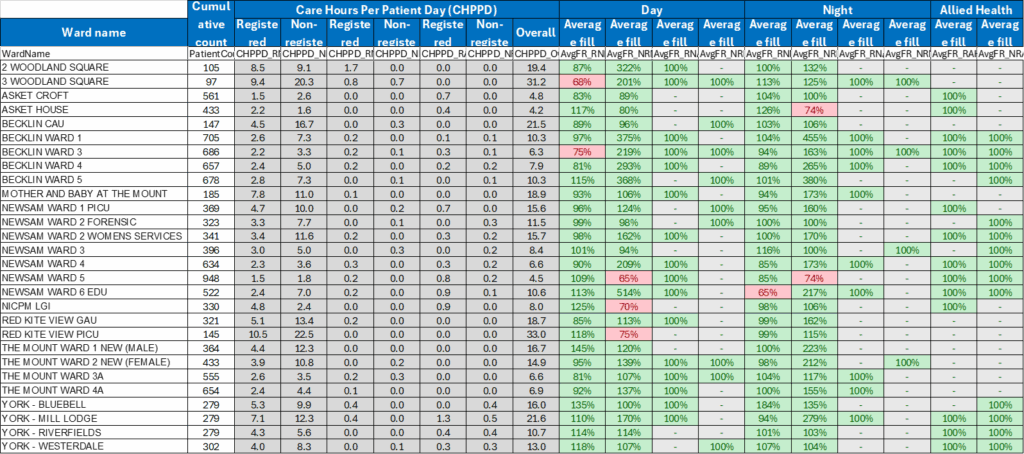
Safer Staffing: Inpatient Services April 25
Fill rate indicator return
Staffing: Nursing, Care Staff and AHPs

Safer Staffing: Inpatient Services May 25
Fill rate indicator return
Staffing: Nursing, Care Staff and AHPs
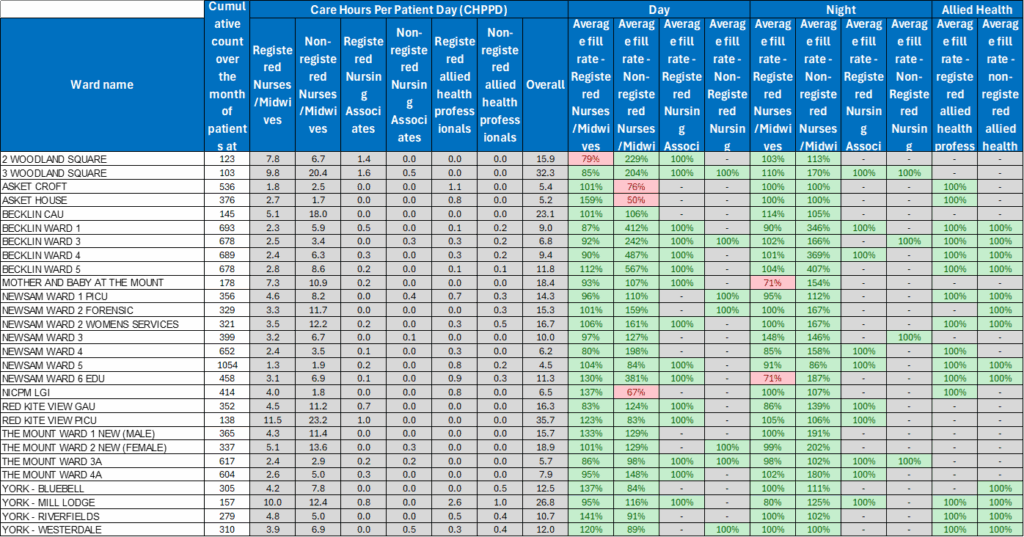
Appendix B
Have Your Say
The below pie chart shows the data for all inpatient areas who have received Have Your Say feedback during May 2025, 80% reported that their care was “good” or “very good” and 8% reported this as “bad” or “very bad”.
The below chart looks at all Have Your Say responses for inpatient services in LYPFT during May 2025. Repsonses were received for the Acute Inpatient Service and PICU, Mother and baby unit and Older People’s Service.

Cover sheet for Report from the Medical Director
- Paper title: Report from the Medical Director
- Date of meeting: 31 July 2025
- Presented by: Dr Chris Hosker, Medical Director and Directorate SLT
- Prepared by: Dr Chris Hosker, Medical Director and Directorate SLT
This paper supports the Trust’s strategic objective/s (SO):
- SO1 – We deliver great care that is high quality and improves lives.
- SO2 – We provide a rewarding and supportive place to work.
- SO3 – We use our resources to deliver effective and sustainable services.
This paper relates to the Trust’s strategic risks (SR):
- SR2 – Delivery of the Quality Strategic Plan
- SR3 – Culture and environment for the wellbeing of staff
- SR7 – Plan and deliver services that meet the health needs of the population we serve.
Executive summary
The purpose of this report is to inform the Board of Directors of the current state of the Medical Directorate and in doing so provide assurance that it is functioning in a way that promotes the success of the Trust, its patients, its staff and the wider public, while also managing any current risks that are positioned as potential barriers to that success.
The paper’s scope therefore covers the key functions that sit within the Medical Directorate and provides an update of key work within each one.
Do the recommendations in this paper have any impact upon the requirements of the protected groups identified by the Equality Act? No
Recommendation
The Board of Directors is asked to consider the information contained within the report and remain assured that the medical directorate is providing its key functions in a way that is in line with successfully achieving the Trust’s objectives.
Medical Director’s Report
1 – Executive Summary
The purpose of this report is to advise the Board of Directors of the status of the Medical Directorate and in doing so, provide assurance that it is functioning in a way that promotes the success of the Trust, its patients, its staff and the wider public, while also managing any current risks that are positioned as potential barriers to that success.
The paper’s scope therefore covers the key functions that sit within the Medical Directorate and provides an update of key work within each one.
2 – Directorate Overview
The Directorate continues to focus on core priorities from 2023-26 while also supporting the Trust’s 14 priority workstreams. Our pharmacy service has received much needed support from the wider organisation and continues to work towards sustained recovery of its functions and improvement in its culture and leadership.
Creation of class leading Clinical Leadership that enables our teams to be the ‘best at getting better’ in delivering outstanding, high quality services: “Best in Show”, Be a Beacon for other NHS Trusts.
3 – Core Directorate Functions
3.1 – Personnel and structure changes: Medical Professional Development Centre /Andrew Sims Centre (ASC)
The Andrew Sims Centre (ASC) provides Continued Professional Development (CPD) provision for mental health and learning disability professionals on behalf of Leeds and York Partnerships NHS Foundation Trust to internal staff and external organisations. It operates under a self-funding financial model, providing training courses in the North of England which has previously evidenced cost savings in travel and expenses costs for the medical study leave budget. Due to the current NHS financial pressures, there continues to be a noticeable impact on ASC bookings. ASC has tried to use various marketing strategies to boost income and encourage course bookings via email marketing and social media with little impact. The market has also as most medical CPD events are now on-line.
A review is currently underway to make a recommendation for the future strategic direction, sustainability for the service and a review of the business model. The main emphasis of the review is to integrate ASC into the Medical Directorate so as to provide not only medical CPD but, also a formal administrative function to the medical staffing work for Consultants, SAS and Trust doctors along with the work of managing the medical rotas (consultant and middle tier) at Red Kite View. This would mirror the highly effective administrative team in Medical Education (MEC) and the support provided for resident doctors.
During the review, there have been some staff changes. Our band 5 has resigned and is currently working notice. Our band 4 has submitted a request for a reduction in hours and our band 6 will be starting maternity leave in August. These staff changes will not impact on the current ASC planned work due to the reduction in the number of events the ASC have booked until the end of the calendar year which is being monitored. The income generated from the events will support salary costs. The outcomes of the review will be documented in the next board report.
The Head of Medical Development and Operations has pulled together the Medical administrative functions within the Directorate (MEC, ASC, Medical Directorate admin and Band 8a) so that there is meaningful data to be able to review following the staff survey results. We are delighted that we have scored highly on promise 1 and high overall in comparison to the Trust average. We have scored lower on promise 5, specifically on appraisal and career development which, will be embedded in monthly supervisions.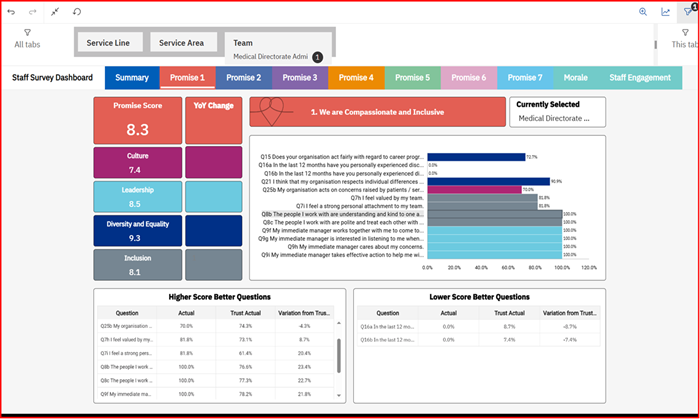
3.2 – Medical Education Centre (MEC)
Starting with the good news, Dr Jordan Williams, CT3, and Dr Charles Pope, ST5, have been awarded the core and higher resident doctor teaching prize respectively for their outstanding work supporting medical education with the organisation and delivery of teaching.
The Trust and the University of Leeds was successful in the bid for a second NIHR Academic Clinical Fellow (ACF) post which means from August 2025 the Trust has two NIHR ACF resident doctors in post. These posts are fully funded.
The Trust were also successful in a bid for a higher trainee in forensic psychiatry and the post is filled at Clifton ward under the supervision of Dr Jacobs from August 2025. This will boost the chances of successful consultant appointment in a hard to recruit area.
All the Trust’s core and higher training posts in psychiatry are fully recruited for August 2025.
Dr Charles Pope and Dr Sophia Kim have been carrying out a quality improvement project to ensure the Trust is compliant with the Safer Learning Environment Charter (SLEC) that NHSE Workforce, Training and Education have rolled out. Drs Pope and Kim will report their findings and any recommendations for change at the Trust Medical Education Committee (TMEC) in September 2025.
The MELM (Medical Education Leadership and Management Team) structure continues to work well. Dr Rajini Mulukutla has stepped down from her core trainee tutor role and has been replaced by Dr Mizrab Abbas. Dr Abbas will lead on FY3 recruitment, GP training and clinical attachés. From August 2025, Dr Ben Rutt, ST5, will undertake a leadership and management role in the MELM structure as part of his special interest time taking over the role from Dr Ayo Ilesanmi. Also from August 2025, Dr Liam Gilgar, consultant in addiction psychiatry will take over from Dr Guy Brookes as the addictions tutor.
A quality improvement project to improve the quality improvement pathway for resident doctors has taken place and is now complete. A leaflet and animation video guide to developing skills for improving quality improvement has been prepared and will be presented at the resident doctor inductions with effect from 6th August 2025. The leaflet and animation video will also be available for resident doctors to refer to at any time on Health ToolBox, the online repository app that is now used in medical education for all induction documents and useful information.
Current challenges are:
NHSE Workforce Training and Education continues to have significant staffing issues. They are now operating with a 16% WTE staff shortage plus 4.7% WTE staff sickness. Workstreams and core business continue to be prioritised however this adds workload pressures internally for medical education and PLDT as there is reduced support compared to previously.
The engagement process with the University of Leeds for consideration of Teaching Trust status is ongoing. The education working group last met on 17th June 2025 and the Trust teaching oversight group on 2nd June 2025.
Resident doctors are taking industrial action which will commence on the 27th July 2025 and continue for a 5 day period.
3.3 – Medical Professional Leadership
Medical staffing levels – vacancies, recruitment
We are pleased to update that since March, two substantive consultants have started in the Trust (both in West CMHT and both less than full time (LTFT)). The flexibility to advertise and recruit to LTFT posts has enabled the recruitment of these two high calibre consultants into the CMHT and the retention of a highly valued and very experienced Consultant through retire and return. There have been appointments of substantive consultants in Perinatal services, Ward 1 Becklin (two LTFT Consultants), Ward 4 Newsam, RKV and Rough Sleepers.
One Trust Locum consultant has started in Liaison service, with another currently going through pre-employment checks. There are also Trust locum consultant posts advertised in West ISS service and ward 3 Becklin.
There are currently a total of 18 agency doctors working at LYPFT. Of the 18 doctors, 14 are consultants with 7 doctors occupying consultant vacancies in adult CMHT posts.
Consultant vacancies: –
This table below lists the clinical services where agency doctors are filling vacancies. All have dates scheduled at consultant interview panels. Adverts for Trust locum consultants run alongside each vacancy providing the opportunity for potential candidates to apply for either permanent or fixed term positions, further supporting the work of reducing agency costs.
| Post | Reason for agency cover | Workforce planning to recruit to vacancy |
| Adult Acute W1B | Long term vacancy | 2 LTFT substantive consultants have been appointed to this post and due to commence in Q2. These appointments will release the current agency locum consultant from September 2025. |
| CAMHs (Leeds -RKV) | Consultant resigned | Substantive consultant starting in Q2 but one vacancy remains. |
| CAMHs (York – Mill Lodge) | Substantive consultant resigned | A higher trainee will be acting up into this post from August 2025 who is applying for the substantive post and would be eligible to start in Q3. |
| Eating Disorders | Long term vacancy | Difficult to recruit into post. Repeatedly advertised. Confirmed interest now from a potential applicant who will apply for the post in Q2 and could release the agency doctor in Q3. |
| Forensic (York) | Long term vacancy | Post has been difficult to recruit to and listed on regular AAC panels next panel in Q4. |
| LD | Long term vacancy | Listed on regular AAC panels, the next in Q2, there has been some interest from an applicant which could release the agency doctor by the end of Q3. |
| Perinatal | Internal move of substantive consultant to WAA CMHT | Substantive appointment made. Consultant to commence in post in Q2 |
| West ISS | Internal move of substantive consultant to Leeds forensic services | Higher trainee has acted up into the post which has now come to an end. The doctor is applying for the Trust locum consultant post and anticipated to start in post in Q2 which will allow release if agency locum by September. |
| CRISS CAU | Internal move of Trust locum consultant to West CMHT | Post been covered via agency locum, AAC panel taking place in Q2, there is a potential applicant which would release the agency doctor in Q3. |
| CMHT South | x1 resignation/notice (job share) | Fulltime post listed on AAC panel in Q2. Potential applicant has indicated they will be applying with potential to be in post by Dec 2025. |
| CMHT East | x1 retirement / 0.6 gap (clinical director’s clinical PAs) | Post listed on AAC panel in Q2 |
| CMHT West | x2 resignations | Posts all listed on AAC panel in Q2 |
Speciality and Associate Specialist (SAS) doctor vacancies
There are currently 2 agency SAS doctors, working in adult CMHT and in WISS. The recruitment and mitigation plan for each of the services are: –
| Post | Reason for agency cover | Workforce planning |
| West ISS | SAS doctor was on long-term sickness absence then retired. | Substantive SD recruited to start Oct 2025. |
| WAA CMHT | West – x2 | Both posts offered to and currently candidates going through pre-employment checks to start ASAP. |
Trust Doctors
The one agency Trust Doctor who is covering in adult acute services is leaving in August as post has been recruited to.
New Work
- Work with NOECPC is continuing involving a benchmarking exercise to assess how LYPFT compares with other NHS organisations in terms of agency rates. The aim is for Mental Health Trusts across the region to agree on rate cards.
- Work has taken place to align the agency fees for all agency locum consultants and agency locum specialty doctors to the national rate card. As of Q2 all agency fees for existing and future bookings will be aligned, resulting in cost savings.
- A training session for all medical line managers has been arranged to take place in Q3 covering sickness absence.
Specialty Doctors
These workstreams all provide an improved offer to our SAS workforce, increasing chances of retention in and recruitment to LYPFT:
- A paper outlining the pathway for progression from Specialty Dr to Specialist grade Dr has now been written and approved for use.
- In addition, a proposal for experienced and qualified SAS doctors to act up into consultant posts has also been produced. This also offers an alternative to agency locum consultant booking for future vacancies.
- The AC/Portfolio pathway is now up and running with 4 doctors working towards completion of the Portfolio route to become a consultant.
Higher trainees
Discussions continue to take place between all eligible Higher Trainees (HTs) and the Professional Lead who meets regularly and routinely with HTs rotating into the Trust to discuss career opportunities, providing information about consultant opportunities available to them in LYPFT. A system with medical education is in place to ensure all eligible HTs are contacted. We also regularly provide HTs across Yorkshire and the Humber a monthly updated recruitment flyer highlighting all the Trust’s consultant vacancies.
Job planning status update
There are a total of 136 consultants and SAS doctors – current compliance is stated below:
| Grade | Complete job plan | Not complete |
| Consultant | 93% | 7% |
| SAS | 94% | 6% |
We are working hard to achieve compliance of 95% however some of the doctors are new to the Trust and will have a formal job plan agreed within the first 3 months of being in post. A provisional job plan is used until then.
Between April 5th 2025 and April 5th 2026, services will move towards a new job planning process with joint meetings preceding individual meetings. The intention is for job plan objectives to better align with the service objectives and for the Head of Operations (or nominated manager) to be invited to participate in the meetings.
A new job planning policy has been written and is currently going through governance. An updated policy and the development of an oversight group were recommendations following the internal audit.
3.4 – Specialty Doctor and Associate Specialist (SAS) Advocate update
The following is a working summary of SAS Advocate (Dr Abhi Inglis) work since the last report submitted in March 2025.
The role continues to involve linking in with colleagues to check on well-being of the SAS group within the workplace. Individual support and guidance have been provided where required. The SAS Advocate and Tutor have streamlined this process for new SAS doctors by offering group meetings with both to address queries and concerns, as well as individual sessions. A page has also been set up on our Trustnet services as a forum for SAS doctors to share relevant information.
There has been ongoing liaison with the Local Negotiating Committee (LNC) and national SAS advocate group to gain and share pertinent information relating to the SAS group both locally and nationally in terms of developmental opportunities, sharing good practice and employment issues.
The role feeds into the Specialty Doctor and Specialist Committee (SASC) focusing on ensuring a forum for general discussion of any workplace concerns impacting health and wellbeing and providing peer support.
The SAS advocate is the organisational lead for annual SAS wellbeing days, and regularly surveys SAS colleagues within the Trust on wellbeing in the workplace. This is currently being undertaken and will influence the SAS the offering in the region. The well-being days have been reviewed and we will be linking these in with SASC meetings to encourage participation and networking.
The SAS development group was set up to discuss and address any issues around recruitment and retention of the SAS workforce and we continue to meet regularly. The ongoing lines of work include:
- Identifying areas in the trust where a Specialist Role would be beneficial. We have had some difficulty with this due to financial limitations and are endeavouring to address the issues across different teams.
- The Portfolio Pathway has successfully appointment posts and Dr S Stevens is supporting the candidates with this.
- The AC approval process has also allocated candidates and receives support from Dr S Stevens.
- Ensuring compliance with the BMA SAS Charter: we have a date set to discuss the implementation of the new charter and any changes needed in the trust to address these. This will also enable us to work towards our ‘SAS Seal of Approval’ – a project being implemented by NHS England across all trusts.
- Ongoing promotion of the mentoring and coaching offer to SAS doctors in LYPFT including recruitment and training of more SAS doctors as peer-mentors.
3.5 – Medical Continuing Professional Development (CPD) and the Andrew Sims Centre
The Andrew Sims Centre (ASC) continue to develop professional business relationships by collectively working with colleagues at LYPFT to co-organise events such as the ‘NHS Resolution: Case Investigator Training’ and ‘SAS Development Day’ that ran in June, and the upcoming ‘LYPFT: Annual General Meeting and Celebration Event’ scheduled to go ahead on 29th July.
ASC continue to build external relationships with Hospital Trusts and are co-organising a ‘Physical Update for Psychiatrists’ course for Nottinghamshire NHS Foundation Trust in September and a ‘Medical Education Conference’ for Humber Teaching NHS Trust in October.
Earlier this year, a review of ASC costs and charges took place along in-conjunction with the Trusts finance manager responsible for ASC. Since this review, ASC have used more cost-effective venues and transferred some courses to run virtually as this reduces expenditure pressures. ASC are in the process of investing in a Microsoft Teams Premium subscription, to use the webinar functionality for ASC courses.
From 1st April to 30th June 2025, ASC have organised 10 courses, of which 7 successfully went ahead. However, this means 3 were cancelled events due to low delegate bookings. The total income from April to June 2025 amounts to £33,691.00, while total expenditures have reached £40,011.00, resulting in a year-to-date loss of £6,320.00. However, this reflects an improvement of approximately £3,500 compared to the same period in 2024. The financial year end of 2024/2025 for the centre recorded a loss of -£45,425.00, an improvement compared to the forecast earlier in the financial year.
There has been a change in staffing costs since the last report because there is no longer a Band 5 working in the department. There will be further staffing cost changes, as the Band 6 will be going on maternity leave from the end of August and the Band 4 have reduced their hours from mid-September. These staffing alterations will lead to a reduction in salary expenses for the centre, as no replacements will be hired.
ASC continues to use various marketing strategies to boost income and encourage course bookings via email marketing and social media. The centre supports the administration of medical study leave for Consultant and SAS Doctors, working closely with the Director of CPD, and the Red Kite View middle tier rota for Medical Directorate.
4 – Responsible Officer
The Responsible Officer update report has been submitted as a separate paper.
5 – Clinical Leadership and Quality of Care
A Clinical Lead Development Day took place on the 4 of June 2025. The programme for the day was co-designed using feedback from Clinical Leads at the previous development session and monthly Clinical Lead Support Forum meetings.
It commenced with an Action Learning Set / Peer Group Coaching session, supported and facilitated by a member of the Trust Organisational Development Team. The afternoon session was separated into four workshop activities:
- Developing the Clinical Lead Induction Pack: For this part of the development day, the group was joined by the Trust Governance Lead Abby Boden, who co-facilitated a session on developing the Trust Governance section of the pack. In this session Clinical Leads were asked to reflect on the Trust Governance information, resources, and support that they wished they has received / needed when they started in the role as Clinical Lead and began their responsibilities in leading for good governance within their services. Ideas and feedback were discussed and debated and key learning points captured. The feedback and intelligence gained from this session were taken by Abby, who will be using the information to develop resources that will be available for use in both the Clinical Lead Induction Pack and within the wider organisation.
- Learning Needs Assessment: Feedback received from the previous development session requested an opportunity to explore formal learning opportunities within the development day. To be able to plan, organise and facilitate such learning opportunities, it was necessary to understand the current gaps and or needs for learning and development within the Clinical Lead community. Using a learning needs assessment framework that is based on learning needs of; new – acquiring new knowledge (learning something for the first time), more, expanding existing knowledge (expanding on / growing existing knowledge), apply, skills / knowledge to practical situations (putting learning into practice), solve –developing skills / knowledge to overcome a challenge (overcoming obstacles and challenges, perhaps through problem-solving or critical thinking), and change – new tech or process (adapting to new technologies or processes, like learning a new work method), the Clinical Leads were asked to work in small group to identify their learning needs and how they would like these needs to be met. The Johari Window concept was introduced to the group as a model for challenging and being curious about our learning needs. The information gained from the session is being analysed by the Clinical Directors and work will continue in the next development day (planned for September) to co-design how to take this forward.
- Building Sustainable Clinical Leadership: The problem and impact of sustainability of Clinical Leadership was introduced to the group. Group members were challenged to answer “who would replace you in your clinical service ..?”. Clinical leaders were encouraged to explore their role in intentionally leaning into this need and starting conversations within their services in relation to identifying those staff with a career interest in Clinical Leadership and holding conversations with them as to how they may develop skills and experience to enable them to grow toward the role. Discussions also took place as to how to create learning and development opportunities that would be valuable in providing those staff interested, with the lived experience they would need to apply for such roles in the future.
- Cost Improvement Process: Time was dedicated to discussing the Trust CIP work and the role of Clinical Leads within this process. The importance of working with service Heads of Operations in dyad partnership was highlighted and explored. Clinical Leads also shared examples of how they were engaging with their dyads and the outputs of some the work carried out.
The next Clinical Lead Development Day is planned for September 2025.
6 – Medicines Safety
The Pharmacy Service continues to address the remaining vacancies. Recruitment rates have significantly improved, and the remaining vacancies are yet to be advertised as they’re currently within pre-advertising processes.
The pharmacy service 1-year recovery plan ‘Getting to Good’ (outlined in the previous report to Board) has recently incorporated recommendations from the Pharmacy Listening Exercise undertaken last year. There are staff engagement sessions (to involve the wider team in the various work streams) being held in July to build on some of the work the senior team have been slowly progressing and establish further projects necessary to deliver the plan.
The Medicines Optimisation Group (MOG) and its subgroup the Medicines Safety Committee (MSC) continue to function in accordance with their ToRs, and a plan to tackle the backlog of medicines governance work is being overseen by the MOG.
7 – Clinical Information Management
E-Proms (Outcome Measures)
Significant progress has been made in advancing outcome measures, with a clear and collaborative structure now in place. The interconnection between the patient portal, electronic Patient-Reported Outcome Measures (e-PROMs), and the Electronic Patient Record (EPR) projects has been established and discussed both with Clinical Directors and at a recent meeting with Executive Directors. The e-PROMs component is progressing well, in line with the original project aims and the timeline submitted to the Project Management Office (Amanda Burgess). Constructive discussions have also taken place with another Trust (The Christie NHS Foundation Trust) that is further along in a similar initiative, providing valuable insights and comparative learning.
The outcome measures for Pilot 1 have now been identified, and work is underway to refine the associated processes in preparation for implementation. Additionally, with the support of Cath Sweeney, a broad understanding of outcome measures currently in use across the organisation has been established, providing a strong foundation for consistency and integration. The immediate next steps include finalising the administrative details required for Pilot 1, ensuring readiness for the anticipated launch of the patient portal pilot at the end of Q2.
8 – Research and Development
In 2025/2026:
- 46 participants recruited to studies
- 9 service areas contributed to recruitment
- 25 studies currently open
- 7 new studies opened
In the last quarter we opened FAST (blood biomarker trial) with Oxford Uni (Dr Ben Alderson is PI) – feeding into the national READOUT study to determine suitability of blood biomarker testing in advancing practice in relation to the Dementia diagnosis pathway for the NHS. We are using the facilities at Kippax for this study.
Two new Research Assistants have started in the team. Anna and Rachel are funded by the NIHR Research Delivery Network and will enable research recruitment across the Trust.
This quarter we closed FreshStart, a large talking therapy interventional study for those who present with repeated self-harm in A&E. We were the highest recruiting site and have been praised by the Research team at Leeds University for our contribution. It was a collaborative effort between the R&D department and the ALPS team. The study is now in follow–up.
We have signed a contract with AliveCor to the value of £320K to deliver research to validation the use of 6 Lead ECG’s in psychiatry. This will be a multicentre study lead by LYPFT which will directly contribute to NICE guidance. The research is led by Dr George Crowther.
COMIC have delivered another Research Ready Schools block of sessions to year 2 children as a result of receiving RRDN Strategic Funding. The 6 week programme introduces children to the importance of mental health research.
We have faced some challenges in relation to IG and IT. A paper to consider options around IG has now been created for consideration by the board. It has not proved possible to install 2 software options that could have enhanced our efficiency due to IG issues and other technical challenges. We continue to seek ways to improve efficiency with digital solutions.
9 – Improvement and Knowledge Service
Both the departmental Annual Service Quality Report and the monthly Improvement and Knowledge Activity Report are available on request.
This update provides a summary of how the Improvement Team is helping with the Trust’s 14 organisational priorities for 2025–26. It shows strengths, gaps, and chances to improve for further alignment. This update also reflects one specific activity where we have worked with other organisations—sharing our learning and learning from them, about the application of the Learning, Culture and Leadership framework.
Trust Priorities and Improvement Team Support
Summary Overview Table
The following table provides an overview of the Improvement Team’s involvement across the 14 priorities within the Trust. It categorises each area by the level of involvement—ranging from involved, light-touch or advisory, to no involvement and highlights key opportunities or considerations for further engagement. This summary aims to support prioritisation, identify areas where quality improvement (QI) methods could add value, and inform decisions about future resource allocation and collaboration.
| Trust Priority | Improvement Team Involvement | Level of Involvement: Involved, Light Touch/Advisory, Not involved | Opportunities or Notes |
| Delivery of our financial efficiency programme | Ideas exchange – joint lead with PMO | Light Touch/Advisory | Light-touch involvement. May benefit from formalised improvement support in cost productivity reviews. |
| Delivery of workforce efficiency programme | Involved with the Admin Digitalisation Group | Light Touch/Advisory | Opportunity to link with OD |
| Delivery of our inpatient quality transformation & improving patient flow programme | Active involvement – project coaching, oversight groups | Involved | Strong alignment with QI expertise. Continued support critical for sustainability. Would benefit from more QI input. Capacity to be reviewed. |
| Reducing mental health emergency department attendances and delays | Working with ALPS on pathways and relationship improvements | Light Touch/Advisory | Opportunity to develop full QI project focused on flow metrics and inter-team coordination. |
| Delivering a transformed community mental health service | Not involved | Not involved | Priority area for future engagement as transformation progresses. |
| Improving the quality of our children and young people’s mental health services | Actively supporting Safe Wards, Deaf CAMHS wait times | Light Touch/Advisory | Demonstrates improvement-led change in complex services. |
| Improving the quality of our perinatal services | Strategic input, relational coordination, metrics | Involved | A model of cross-boundary improvement. Potential learning site for other areas. |
| Implementing the Recommended Summary Plan for Emergency Care and Treatment. | Not involved | Not involved | May benefit from support in process redesign or implementation improvement methods. |
| Deliver our health equity priorities | Not directly involved, but team member is Health Equity Fellow | Light Touch/Advisory | Possibility of building a dedicated QI approach into equity projects. |
| Implement outcome measures across all care services | Linked to Quality Dashboard | Light Touch/Advisory | Working with two teams on improvement projects to implement outcome measures. |
| Implementation of quality and culture dashboards | Lead role in quality dashboard, civility work | Involved | Potential input to culture dashboard re LCL – attend Civility & Respect TFG |
| Develop and agree our future facilities management model across our Private Finance Initiative (PFI) sites | Not involved | Not involved | Unlikely priority for improvement unless linked to service experience or cost reduction. |
| Procure new electronic patient record system | Not involved | Not involved | Opportunity for improvement methodology during roll-out. |
| Delivery of key People Plan (workforce) priorities. | Supporting OD/HR on Pharmacy Culture Review | Light Touch/Advisory | Could be strengthened with broader workforce improvement projects |
High-Level Summary
71% of the trust priorities are directly supported or supported in a light touch/advisory capacity by the improvement team, broken down by:
- Directly supporting or contributing to 3/14 priorities (21%)
- Light Touch or advisory support in 7/14 (50%)
- No current involvement in 4/14 (29%)
Note that the support highlighted above for a priority could consist of more than one activity, in fact priority related activity is 45% of the total improvement work undertaken by the Improvement Team.
Summary Overview Table of all activity, including priorities
The team support a range of improvement related activities (including priorities) across the organisation as shown in the table below:
| Service Line | Improvement Projects | Other Activity | Total Activity | No. linked to priorities |
| Acute Care Services | 3 | 3 | 6 | 5 |
| Children & Young Peoples service | 1 | 2 | 3 | 3 |
| Community & Wellbeing | 2 | 0 | 2 | 1 |
| Connect, Rehab & Gender ID | 2 | 0 | 2 | 0 |
| Forensics | 0 | 0 | 0 | 0 |
| Learning Disabilities | 2 | 0 | 2 | 0 |
| Liaison MH & Perinatal Services | 3 | 0 | 3 | 1 |
| Older Peoples Service | 4 | 0 | 4 | 1 |
| Regional & Specialist Services | 2 | 1 | 3 | 0 |
| Corporate & other | 2 | 2 | 4 | 2 |
| Total | 21 | 8 | 29 | 13 |
Note that the improvement activity listed above excludes other Improvement Team activities like supporting the Annual Service Quality Report, Learning Culture Leadership framework and Relational Coordination facilitation.
Key Themes
- The Improvement Team is most impactful when engaged early and involved in planning.
- There is strong alignment between the Improvement Team and priorities related to inpatient quality, perinatal care, and quality dashboards.
- Opportunities exist to include improvement skills in all priorities, though this would need to be matched with the resources within the Improvement Team, which is currently at capacity.
Sharing and Learning Across Boundaries
During 2024, Leeds and York Partnership NHS Foundation Trust took part in a unique international collaboration to deepen our understanding and use of the Institute for Healthcare Improvement (IHI) Framework for Safe, Reliable, and Effective Care (renamed within LYPFT to Learning Culture and Leadership (LCL)). This framework gives a clear plan to support whole-system safety and reliability, focusing on building a comprehensive ‘system of safety’ rather than separate improvement efforts.
Together with Improvement Cymru (Wales) and Waterloo Regional Health Network (Canada), we formed a cross-border learning network. We met virtually every six weeks, and shared how each organisation had independently used and changed the IHI Framework to fit their national and local policy contexts, while remaining true to its main ideas. This collaboration allowed for useful sharing of experiences, resources, ways to measure progress, and real examples of how it was used.
 Our shared work was recognised internationally:
Our shared work was recognised internationally:
- A joint poster outlining our approach was accepted for presentation at the IHI National Forum in December 2024 (delivered by Grand River Hospital)
- The same poster was also showcased at the International Forum on Quality and Safety in Healthcare in May 2025 (delivered by Leeds and York Partnership NHS Foundation Trust)
Key learning from this work includes:
- The basic ideas of the IHI Framework are robust and can be successfully adapted to different policy and operational environments
- Regular collaboration enabled faster turning research into action
- The network provided a platform to co-create practical tools, improve how we use it locally, and learn from international peers
- This work shows we are serious about embedding safe, reliable, and effective care across the organisation and highlights the value of collaboration in making things better faster.
10 – Mental Health Legislation Compliance
Mental Health Legislation Training
We have reviewed the MHL training requirements for all staff in the trust to ensure that the right people are doing the right training. These adjustments have led to a short-term drop in compliance figures and additional training dates have been arranged to ensure that we meet the trust target again as soon as possible. We are continuing to monitor the passage of the MHA Bill through parliament and are involved in several regional and national groups in planning for these changes. We are currently considering which elements of the bill we can start to embed in training to ensure that we have a head start on the implementation, which will have a considerable impact on clinicians.
Mental Health Act Managers (MHAMs)
We are currently piloting a MHAMs paper review process for uncontested renewals and extensions, which reflects the process for some other trusts in our region. The purpose of the pilot is to assess whether we can reduce the workload of clinicians in relation to hearings, whilst ensuring that the rights of patients remain protected.
11 – Conclusion
This extensive report provides an overview of the major pieces of work being conducted within the medical directorate and the areas of work that required ongoing focus and support.
11 – Recommendation
The Board are asked to consider the information contained within this report on the key functions of the medical directorate and to be assured that the work being conducted is commensurate with the challenges being faced and in line with the wider Trust strategy
Dr Christian Hosker
Medical Director
July 2025
Cover sheet for Guardian of Safe-working Hours Q4 and Annual Report
- Paper title: Guardian of Safe Working Quarterly Report – Quarter 4: 1st January 2025 to 31st March 2025
- Date of meeting: 31 July 2025
- Presented by: Chris Hosker – Medical Director
- Prepared by: Rebecca Asquith – Guardian of Safe Working Hours
This paper supports the Trust’s strategic objective/s (SO):
- SO2 – We provide a rewarding and supportive place to work.
This paper relates to the Trust’s strategic risks (SR):
-
- SR1 – Quality including safety assurance processes
- SR3 – Culture and environment for the wellbeing of staff
- SR5 – Adequate working and care environments
Executive summary
The purpose of this report is to give assurance to the board that doctors in training are safely rostered and that their working hours are compliant with the terms and conditions of service (TCS) of the 2016 contract. Key points to note are:
- There have been 9 exception reports, including 3 breaches leading to a GOSW fine.
- There have been 0 patient safety issues recorded in this period.
- Resident Doctors Forum met on 17th January 2025 with continued review of ERs and rota gaps. Feedback was also received from Core and Higher Trainee Representatives.
Do the recommendations in this paper have any impact upon the requirements of the protected groups identified by the Equality Act? State below, ‘Yes’ or ‘No’.
If yes, please set out what action has been taken to address this in your paper.
Recommendation
The Board of Directors are asked:
- To agree that this report provides an assurance level for the systems in place to support the working arrangements of the 2016 Contract and TCS for the junior doctors working in the Trust and that they are meeting their objective of maintaining safe services.
- To provide constructive challenge where improvement could be identified within this system.
Guardian of Safe Working Annual Report (April 2024 to March 2025)
1. Executive Summary
On 1st February 2017 Leeds and York Partnership Foundation Trust (LYPFT) transitioned all doctors in training on to the 2016 Junior Doctor Contract. At this time, Dr Cashman was appointed as Guardian of Safe Working (GOSW), succeeded by Dr Alderson on 1st December 2019, and subsequently Dr Asquith on 1st June 2023.
There is a Trust strategic workforce plan in place to address recruitment and retention of staff. Both the Guardian of Safe Working and the Medical Education department (MEC) continue to work with our doctors in training and their clinical and educational supervisors to ensure patient safety and effective training.
Exception reporting is both welcomed and encouraged by the GOSW and MEC, to ensure any deviation from the contract terms and conditions is understood and actioned accordingly. There has been a total of 162 exception reports since the contract was implemented in February 2017. 23 of these are within the reference period of this report. There have been no reports raising concerns regarding patient safety in this period. There have been 4 breaches incurring fines, totalling £262.15, in this reporting period.
2. Introduction
The purpose of this report is to give assurance to the board that doctors in training are safely rostered and that their working hours are compliant with the Resident doctors contract 2016 and in accordance with Resident Doctors terms and conditions of service (TCS).
The report is for the period from 1st April 2024 to 31st March 2025.
It covers:
- staff vacancies and locum usage
- exception reports
- work schedule reviews
3. Background
The LYPFT Guardian of Safe Working (GOSW) was appointed in November 2016 and is responsible for ensuring compliance with the terms and conditions of the Resident Doctor Contract 2016. This is done through working with both the employed doctors and the organisation, with concerns raised both informally and formally through the mechanism of Exception Reporting, and also via a quarterly Resident Doctor Forum (RDF) for which the GOSW is chair. Details of exception reports for 2024-2025, as well as RDF feedback, are addressed later in this report
The current head count of all doctors in training working in LYPFT is 110. A summary table is included in appendix A. This total includes core trainees, higher trainees, foundation year doctors, and GP trainees. Less than full time trainees (LTFT) can be allocated to Trusts on a supernumerary basis i.e., additional to the agreed training scheme posts, which accounts for higher numbers of trainees than posts. It should also be noted that where there are vacant training places the Trust recruits junior grade doctors on temporary contracts. With the implementation of the 2016 contract these posts are called Trust doctors, and sometimes referred to as ‘FY3s’, but are not doctors in a training programme. These doctors are also employed under the resident doctors 2016 contract, as agreed with the Local Negotiating Committee.
LYPFT forms part of the Leeds and Wakefield Psychiatry core training scheme and acts as lead employer for trainees within LYPFT and Leeds Community Health Trust (LCH). Historically LYPFT also acted as lead employer for trainees being hosted within the scheme at South West Yorkshire Partnerships Foundation Trust (SWYPFT), however since August 2020 in SWYPFT now acts as lead employer for the trainees being posted within their organisation.
There are 45 established core training and 2 NIHR whole time equivalent posts funded via the medical tariff for Doctors in Training placed within LYPFT and LCR. In addition to these posts, there are 6 trust doctors (‘FY3s’) in service-funded posts to support service provision.
LYPFT is also the employer of psychiatry Higher Trainees (HT) allocated to the 34 established posts within the Trust across general adult psychiatry, psychotherapy, old age psychiatry, intellectual disability, and CAMHS. 2 CAMHS posts are based in York, with trainees allocated to these posts participating in the York locality rota, but continuing to be employed by LYPFT.
3. Background
Rotas for on call work within LYPFT and LCH core training are coordinated through LYPFT. This includes a Psychiatry Resident Shift (PRS) rota, staffed by the CT’s and FY2s. 4 doctors are resident on call on evenings and weekend days, with 3 further doctors working night shifts. There is also a non-resident middle tier on call rota which is staffed by the HTs, with two doctors working per 24 hour shift.
Leeds Teaching Hospitals Trust (LTHT) is the lead employer for the Foundation Training Scheme and holds responsibility for contractual requirements including exception reporting for these doctors. LYPFT is currently hosting 21 Foundation Trainees, including two FY1 Academic Clinical Fellows and six FY2s who participate in the LYPFT PRS rota. There is joint working between LYPFT and other local GOSWs when required.
4. – Vacancies and Rota Gaps
4.1 – Current Vacancies
In the absence of a trainee being allocated to a post, individual services are responsible for addressing gaps in daytime cover using a risk assessment approach. The options available to meet service needs are establishing specialty doctors posts, or booking of an agency locum if the need is short term and / or recruitment to specialty doctor post is unsuccessful. The CT vacancy at the end of March 2025 is zero as the vacant posts have been filled through the appointment of ‘FT3’ trust doctors. Such appointments have been funded through service budgets.
4.2 – Rota Gaps
In 2024/25 there have been a total of 414 rota gaps, 244 on the PRS rota (16% of all shifts) and 170 on the middle tier rota (23% of all shifts). The monthly breakdown of rota gaps has been provided in each of the quarterly reports and are included, along with reasons for gaps, in appendices B and C. Usual reasons for gaps include sickness, compassionate or other statutory leave, coming off the rota or leaving the trust, and gaps related to vacant posts or LTFT working.
174 shifts on the PRS rota were covered by internal locums. This equates to 71.3% of rota gaps which represents a decline from the year of 2023/2024 reporting period whereby 91.7% of rota gaps were covered internally. A total of 70 (29%) vacant PRS shifts were unfilled. Only 5 (3%) vacant middle tier shifts were unfilled. There has been no use of agency locums on either the PRS or middle tier rota.
4.3 – Cover for Rota Gaps
The medical education teams approach to providing cover for rota gaps is, in the first instance, to agree internal cover by doctors already working on the rota. This is known as an internal locum shift.
If the gap is still not covered, there are a number of doctors who have worked on the LYPFT rotas or are working in a medical post within the Trust that does not include an on-call commitment, who are approached. These would also be known as internal locum shifts.
If the shift remains uncovered, then the rota may be authorised to run on reduced staffing by the Director of Postgraduate Medical Education – Operational Lead. In this scenario the medical education team communicates this to the doctors of all grades on the rota, on-call senior manager and switchboard for the date affected to make them aware of the reduced cover. Doctors on the on-call rotas are informed of the possible need to ‘act down’ if there was a staffing crisis. The Director of Postgraduate Medical Education – Operational Lead has now ensured that in situation where a shift cannot be filled the Doctors who are working that shift are remunerated with an equal proportion of the internal locum fee that would have been spent were the shift to be filled.
There has been no use of external locums to cover rota gaps. It is recognised that such doctors are not often familiar with the trust or IT systems which limits effectiveness in providing out of hours cover. It is felt that utilising internal locum cover or running on an reduced rota or with acting down arrangements is most acceptable for patient safety. External locum cover would be considered if required in extenuating circumstances. There has been no use of external locum cover in this reporting period.
5. – Exception Reports
There have been 23 Exception Reports (ERs) in this reporting period. These are detailed in the quarterly reports and are provided in Appendix D. There have been no immediate safety concerns raised. There have been 4 ERs which have identified breaches for which issuing of a fine has been warranted as per the T+Cs.
The ER’s in this reporting period have mostly been related to difference in educational opportunities or difference in hours worked. Further detail as follows:
- Quarter 1: 8 exception reports received.
6 related to ‘difference in educational opportunities’ or ‘difference in support available’ as a result of rota vacancies on night shifts leading to the trainee allocated to attend ALPS (for the purpose of increasing emergency training experience) not being able to do so.
The remaining two ERs were both significantly outside of the contractual reporting periods. One ER related to missing the 5-10pm break on a non-resident middle tier shift. The second ER related to not being able to conclude a 24 hour non-resident shift at the expected time, due to needing to handover to daytime service, which led to the doctor working 4 hours beyond the end of their shift. Given the submission of the ERs significantly beyond the contractual requirements, a fine was not levied by the GOSW. Discussions were held between the resident doctor, Post Graduate Director of Medical Education – Ops Lead, the GOSW, and the clinical supervisor, to give trainee specific feedback. Additionally, further discussions have taken place between the GOSW, MEC, and PGDME to agree a process whereby if trainees are expecting they will not be able to take their breaks as contractually required during any on call shift and there are challenges in delegating or handing over the colleagues, this is escalated to the on call consultant in order to discuss and access any necessary supervision in relation to time management, prioritisation of tasks, and handover to appropriate colleagues. This will also be communicated by the GOSW at resident doctor inductions moving forwards and has been discussed at RDF.
- Quarter 2: 2 Exception Reports received
Both were in relation to loss of educational opportunities when the resident doctor allocated to ALPS was called back to support the PRS rota doctors due to increased volume of work load. On both occasions, the doctor was able to return to support the necessary work and then return to ALPS as intended.
- Quarter 3: 4 Exception reports received
Two were in relation to missed educational opportunities when resident doctor allocated to ALPS was called back to support the PRS rota due to volume of work load or rota gaps.
Two were in relation to overtime being worked. One of these was additional hour worked at the end of a normal working day which was compensated by TOIL. The second one related to additional hour worked at the end of an on call shift, breaching the maximum 13 hour shift duration stipulated by the T+Cs, resulting in a fine.
- Quarter 4: 9 Exception reports received
Four of these related to missed educational opportunities. Three of which related to inability of resident doctors to complete planned ALPS shifts due to acuity of workload on the PRS rota. Loss of such experience continues to be monitored by MEC and whereby there has been two or more lost opportunities for such experience, additional arrangements are made where possible. This has been the case for one doctor in this reporting period, whereby they were swapped into ALPS shifts to ensure opportunity to obtain such experience. One ER related to lost educational opportunity in core placement due to unexpected staff absence and no further action was deemed necessary following this.
Five ERs related to additional hours worked. One related to 1 hour and 15 mins worked by the resident doctor at the end of a normal working day to support with urgent physical health care of patients. TOIL was agreed. This was submitted as a second (duplicate) ER by the resident doctor due to access issues for the clinical supervisor which has since been resolved.
One ER related to 1 hour extra being worked at the end of a long day. This meant that 14 hours were worked, breaching the maximum 13 hour shift duration. As per the T+Cs the doctor was paid for one hours extra work at the enhanced rate and a GOSW fine was levied. It continues to be highlighted via MEC and RDF that doctors can utilise handover processes and seek supervision from seniors if required in order to avoid such breaches wherever possible.
One ER related to 15 minutes extra being worked at the end of a resident on call shift. Whilst there was no breach in the shift duration, the additional 15 minutes worked meant that the doctor did not receive 11 hours rest between consecutive shifts. TOIL was agreed with the doctor for the 15 minutes worked. As per the T+Cs a GOSW fine was levied for the breach in minimum rest requirements. It has been agreed via RDF with the resident doctor representatives that should such circumstances arise in the future, it can be agreed with colleagues on the shift (and senior supervision if felt necessary) for the doctor to start work slightly later to ensure adequate and necessary rest periods are achieved.
One ER related to 11 hours rest not being achieved between consecutive shifts due to the clock changes. The impact of the clock change has previously been discussed and agreed within the RDF that no action is required around this. However, considering the clock change impacts the necessary rest requirements and constitutes a breach, the GOSW deemed it appropriate to levy a fine as per the T+Cs and revisit this via RDF. Such discussions have now led to the agreement via RDF that during clock changes the doctors will stagger their start and finish times to ensure they each achieve minimum rest requirements. It is expected that this should avoid such breaches arising in the future.
6 – Work Schedules
A work schedule is a document that sets out the intended learning outcomes, mapped to the educational curriculum, the scheduled duties of the doctor, time for appropriate non-clinical activities, and the number and distribution of hours for which the doctor is contracted. Work scheduling allows both educational planning necessary for training programmes, as well as the ability to plan and deliver clinical services.
A generic work schedule issued by the employer forms the basis for a personalised work schedule, which is prepared by both the doctors in training and their clinical supervisors at the beginning of each placement. MEC communicate with the doctors to ensure these are understood and completed. Where forms are not returned by the deadline, then a reminder is sent from MEC and if this does not result in a return, then MEC inform the GOSW who contacts the trainee and their clinical supervisor to support where needed.
Where there are exception reports raised, or following request from the doctor or employer, a work schedule review can take place. This is a formal process by which changes to the work schedule may be suggested and / or agreed. No work schedule reviews have been completed in this reporting period.
I would note that whilst LYPFT do not hold responsibility for issuing of work schedules for Foundation Year doctors employed by LTHT, MEC have begun collecting evidence of ‘timetables’ being completed with the clinical supervisor so that we can be satisfied that doctors working within our trust are provided with the required information to support work scheduling with their lead-employer.
7 – Fines
There have been 4 Exception Reports which have identified breaches resulting in a financial penalty for the Trust. The total fine fund as of the end of this reporting period is £262.15 and sits within a GOSW cost centre. Spending from such funds will be agreed via the RDF.
8 – Resident Doctors Forum
The RDF has met on four occasions in 2024/2025. RDF was chaired by Dr Asquith throughout this period.
In addition to discussing rota gaps and exception reports as detailed above, resident doctors have used the forum to offer feedback via the resident doctor forums, the Resident Doctor Committee (RDC) and Higher Trainee Committee (HTC)
In 2024/2025 some of the key matters discussed included:
- Change of name from Junior Doctor Forum (JDF) to Resident Doctor Forum (RDF) in keeping with BMA recommended terminology.
- Requirement to utilise annual leave to permit locum shifts which is a return back to pre-pandemic practice and ensures no unintended impact upon loss of core placement experience by taking on additionally-paid locum work.
- Review of the SOP for booking overnight accommodation for the middle-tier non resident on call rota.
- Following discussions with MEC, resident doctors, and the BMA, it was agreed that trainees taking Fridays as their non-working day will be asked to work on call shifts that fall on this day. If unable to agree to this, a different non-working day will need to be considered. This is to ensure equity across all trainees.
- The JDC Terms of Reference and Wellbeing in Trainee Psychiatrist documents were approved.
- A request was made by GOSW for the Exception reporting details to be added to on-call rotas for ease and to encourage Exception Reporting.
9 – Issues Arising
9.1 – Engaging Resident Doctors
The GOSW has continued to attend induction to introduce the role to new starters in LYPFT. RDF has not been postponed or cancelled over this reporting period. All RDF meetings have had representation from both CT and HT grades. RDF has been held on Microsoft Teams throughout this reporting period in-line with the requests from the Resident Doctors to continue with use of this platform rather than a face to face meeting. The GOSW continues to highlight that informal discussions are welcomed whereby there may be uncertainty as to whether Exception Reporting is indicated, or for any other reason, and relevant contact details are provided at induction time to new starts, and re-circulated to existing resident doctors. The GOSW and MEC continually
support a culture of reporting variance from the work schedule or T+Cs.
9.2 – Recruitment
National recruitment in Core Psychiatry Training continues to improve. This is reflected locally in our CT recruitment.
LYPFT have a number of strategies in place aimed at increasing recruitment targeted at both medical students and Foundation Trainees. These include the ongoing engagement with undergraduate teaching through the University of Leeds and increased visibility throughout the Foundation Training Programme teaching sessions.
The Trust have a named Foundation Year tutor to enhance trainees experience within the speciality, as well as a designated teaching programme for the FYs placed within the Trust.
The CTs are also encouraged to participate in the medical student teaching programme by having protected time to deliver this to students from years 2 – 4. This provides a valuable experience for both CTs and medical students, and allows an opportunity for informal discussions also about the psychiatry training pathway. A notable strength of the core trainee programme is the support given to trainees in relation to passing membership exams through the Core Trainee Psychiatry Course held at Leeds University, with protected time to attend this throughout the training years.
10 – Summary
Whilst LYPFT receives relatively few ER’s comparative to other local and national trusts, these numbers are increasing. This likely represents both the awareness of the resident doctors to the T+Cs of their contract and the attentiveness to working to these, as well as the culture of encouraging and accepting exception reporting that has promoted by the GOSW and MEC.
Rota gaps continue to be a challenging issue. There are many reasons for rota gaps and MEC have worked extremely hard to minimise impact of rota gaps, with all filled gaps being covered by the internal locum pool of doctors and no reliance on external locums.
Given that there have been no patient safety concerns from ER it is clear that the rota patterns enable the resident doctors to work according to their contract in order to deliver safe patient care.
It should be noted that proposed changes to exception reporting processes as per the BMA + NHS Employers ‘Framework Agreement’ will be significant. Whilst further guidance is awaited, the proposed implementation date of the 12th September 2025 means that the GOSW, MEC, and the Medical Directorate are working closely to consider how to ensure the requirements of this agreement will be met. This has been challenging thus far due to the absence of follow up guidance that is specified as pending in the Framework Agreement itself, but progress is being made. Key points to be aware of are that the planned changes will automate payment / TOIL for exception reports made for extra work of less than 2 hours duration via a suggested HR process which in LYPFT will sit with the medical directorate. There will also be access restrictions to ER data or related information, to prevent detriment to reporting doctors. Data breaches will come with additional fines to the organisation. There will be requirements for access to ER systems (Allocate in LYPFT) within 7 days of starting. Whilst this is already achieved in LYPFT, there are other software requirements from Allocate that will be needed to best support the new processes and we await further updates from Allocate as to any planned system updates. It should be considered that the changes arising from the Framework Agreement could impact upon the number of exception reports received. Whilst it is possible there may not be a significant change, if there is underreporting of ERs within any organisation for fear of detriment to the reporting doctor, the new processes will support such ERs being completed confidentially and thus could lead to increased numbers, as well as increased costs to an organisation through both payment or TOIL.
Recommendations
The Board of Directors are asked:
- To agree that this report provides an assurance level for the systems in place to support the working arrangements of the 2016 TCS for the resident doctors working in the Trust and that they are meeting their objective of maintaining safe services
- To provide constructive challenge where improvement could be identified within this system
Dr Rebecca Asquith
GMC 7151560
Guardian of Safe Working Hours
Appendix A
| Grade of Dr | WTE posts within LYPFT | Current numbers (inc LTFT) |
| CT Psychiatry | 45 + 1 NIHR | 44 (inc 1 NIHR) |
| HT Psychiatry | 34 | 33 |
| GP Trainee | 5 (*Includes 2 Innovative GP – does not cover on-calls 50:50 split between GP & LYPFT) | 5 |
| FY Dr | 20 FY1 2 FY1 ACF 6 FY2 |
20 FY1 2 FY1 ACF 6 FY2 |
| Total | 112 | 110 |
On current numbers: Whilst the schemes have been full, current numbers are lower than WTE posts due to trainees more recently leaving the scheme.
Appendix B
Quarter 1 2024/2025
| Rota Gaps | April CT | April HT | May CT | May HT | June CT | June HT |
| Gaps | 11 | 13 | 24 | 15 | 17 | 16 |
| Internal Cover | 6 | 13 | 18 | 15 | 15 | 16 |
| Agency cover | 0 | 0 | 0 | 0 | 0 | 0 |
| Unfilled | 5 | 0 | 6 | 0 | 2 | 0 |
| Fill Rate | 54% | 100% | 75% | 100% | 88% | 100% |
Quarter 2 2024/2025
| Rota Gaps | July CT | July HT | August CT | August HT | September CT | September HT |
| Gaps | 24 | 22 | 13 | 14 | 12 | 9 |
| Internal Cover | 18 | 22 | 9 | 13 | 11 | 9 |
| Agency cover | 0 | 0 | 0 | 0 | 0 | 0 |
| Unfilled | 6 | 0 | 4 | 1 | 1 | 0 |
| Fill Rate | 75% | 100% | 69% | 92% | 91% | 100% |
Quarter 3 2024/2025
| Rota Gaps | October CT | October HT | November CT | November HT | December CT | December HT |
| Gaps | 18 | 9 | 17 | 11 | 24 | 15 |
| Internal Cover | 16 | 9 | 15 | 10 | 15 | 13 |
| Agency cover | 0 | 0 | 0 | 0 | 0 | 0 |
| Unfilled | 2 | 0 | 2 | 1 | 9 | 2 |
| Fill Rate | 89% | 100% | 88% | 91% | 62.5% | 87% |
Quarter 4 2024/2025
| Rota Gaps | January PRS | January Middle Tier | February PRS | February Middle Tier | March PRS | March Middle Tier |
| Gaps | 34 | 11 | 26 | 17 | 24 | 18 |
| Internal Cover | 22 | 11 | 14 | 17 | 15 | 17 |
| Agency cover | 0 | 0 | 0 | 0 | 0 | 0 |
| Unfilled | 12 | 0 | 12 | 0 | 9 | 1 |
| Fill Rate | 64.7% | 100% | 53.8% | 100% | 62.5% | 94.4% |
Appendix C
Reasons for rota gaps. Number of gaps per reason:
| Months and Year | PRS Rota | Middle Tier (HT) Rota |
| April – June 2024 | Sickness – 14 LTFT – 30 Vacant – 2 Off rota – 6 |
Left trust – 19 Off rota – 3 LTFT – 8 Sickness – 9 Vacant – 5 |
| July – September 2024 | Sickness – 26 LTFT – 8 Vacant – 6 Off rota – 7 Mat leave – 2 |
Left trust – 10 Vacant – 14 LTFT – 9 Sickness – 12 |
| October – December 2024 | Sickness – 22 LTFT – 16 Off rota – 11 Special absence – 5 Vacant shift – 5 |
Sickness – 10 Vacant – 10 Off rota – 11 LTFT – 4 |
| January – March 2025 | Sickness – 34 LTFT – 11 Off rota – 14 Special absence – 4 Vacant shift – 13 Mat / pat leave – 8 |
Sickness – 3 Vacant – 13 Left trust – 7 LTFT – 5 Off rota – 17 |
Appendix D
Exception Reports (ER) 24/25
| Reference period of report | 01/04/24 – 31/03/25 |
| Total number of exception reports received | 23 |
| Number relating to immediate patient safety issues | 0 |
| Number relating to hours of working | 9 |
| Number relating to pattern of work | 0 |
| Number relating to educational opportunities | 13 |
| Number relating to service support available to the doctor | 1 |
ER outcomes: resolutions
| ER outcomes: resolutions | Total |
| Total number of exceptions where TOIL was granted | 5 |
| Total number of overtime payments | 3 |
| Total number of work schedule reviews | 0 |
| Total number of reports resulting in no action | 15 |
| Total number of organisation changes | 0 |
| Compensation | 0 |
| Unresolved | 0 |
| Total number of resolutions | 23 |
| Total resolved exceptions | 23 |
Guardian of Safe Working Hours Report (Quarter 4: 1st January 2025 to 31st March 2025)
1 – Executive Summary
The purpose of this quarterly report is to give assurance to the board that doctors in training are safely rostered and that their working hours are compliant with the resident doctors contract 2016 and in accordance with resident doctors terms and conditions of service (TCS). The report includes the data from 01.01.2025 to 31.03.2025.
2 – Quarter 4 Overview
- Vacancies: There are a total of 45 Core Training posts and 2 NIHR posts. There are a total of 34 Higher Training posts. All schemes are full.
| Rota Gaps | January 2025 – PRS | January 2025 – Middle Tier | February 2025 – PRS | February 2025 – Middle Tier | March 2025 – PRS | March 2025 – Middle Tier |
| Gaps | 34 | 11 | 26 | 17 | 24 | 18 |
| Internal Cover | 22 | 11 | 14 | 17 | 15 | 17 |
| Agency cover | 0 | 0 | 0 | 0 | 0 | 0 |
| Unfilled | 12 | 0 | 12 | 0 | 9 | 1 |
| Fill Rate | 64.7% | 100% | 53.8% | 100% | 62.5% | 94.4% |
Comments:
- Rota gaps arise for various reasons including sickness, gaps arising from Less Than Full Time working patterns, rota gaps, and other leave including parental leave or special leave.
- The Psychiatry Resident Rota (1st tier) is covered by FY2 and CT doctors. The fill rate for gaps in this rota is less than has been the case in previous years. Of the shifts that were uncovered, 20 of these were night shifts, 5 were weekend long days, and 8 were evening shifts. The middle tier rota (2nd tier) is covered by Higher Trainee doctors and continues to have a high fill rate. The one shift that was unfilled was managed by use of the acting down processes.
Exception reports (ER):
There were 9 exception reports in total during the reporting period.
- Four of these related to missed educational opportunities. Three of which related to inability of resident doctors to complete planned ALPS shifts due to acuity of workload on the PRS rota. Loss of such experience continues to be monitored by MEC and whereby there has been two or more lost opportunities for such experience, additional arrangements are made where possible. This has been the case for one doctor in this reporting period, whereby they were swapped into ALPS shifts to ensure opportunity to obtain such experience. One ER related to lost educational opportunity in core placement due to unexpected staff absence and no further action was deemed necessary following this.
- Five ERs related to additional hours worked.
One related to 1 hour and 15 mins worked by the resident doctor at the end of a normal working day to support with urgent physical health care of patients. TOIL was agreed. This was submitted as a second (duplicate) ER by the resident doctor due to access issues for the clinical supervisor which has since been resolved.
One ER related to 1 hour extra being worked at the end of a long day. This meant that 14 hours were worked, breaching the maximum 13 hour shift duration. As per the T+Cs the doctor was paid for one hours extra work at the enhanced rate and a GOSW fine was levied. It continues to be highlighted via MEC and RDF that doctors can utilise handover processes and seek supervision from seniors if required in order to avoid such breaches wherever possible.
One ER related to 15 minutes extra being worked at the end of a resident on call shift. Whilst there was no breach in the shift duration, the additional 15 minutes worked meant that the doctor did not receive 11 hours rest between consecutive shifts. TOIL was agreed with the doctor for the 15 minutes worked. As per the T+Cs a GOSW fine was levied for the breach in minimum rest requirements. It has been agreed via RDF with the resident doctor representatives that should such circumstances arise in the future, it can be agreed with colleagues on the shift (and senior supervision if felt necessary) for the doctor to start work slightly later to ensure adequate and necessary rest periods are achieved.
One ER related to 11 hours rest not being achieved between consecutive shifts due to the clock changes. The impact of the clock change has previously been discussed and agreed within the RDF that no action is required around this. However, considering the clock change impacts the necessary rest requirements and constitutes a breach, the GOSW deemed it appropriate to levy a fine as per the T+Cs and revisit this via RDF. Such discussions have now led to the agreement via RDF that during clock changes the doctors will stagger their start and finish times to ensure they each achieve minimum rest requirements. It is expected that this should avoid such breaches arising in the future.
Fines:
- Three fines were levied in this reporting period as above. One for breach in the maximum shift duration, two in relation to not achieving minimum rest periods between shifts. These fines total £167.69 and comes from the service line in which the reporting doctor is based. In this case, this was the Eating Disorders Service.
- One fine of £94.46 was also levied in Quarter 3. The total fine fund as of the end of this reporting period is £262.15 and sits within a GOSW cost centre. Spending from such funds will be agreed via the RDF.
Patient Safety Issues:
- None
Resident Doctor Forum (RDF):
The meeting held during the Q4 reporting period took place on 17th January 2025:
- It was agreed to change the name of the JDF to RDF in keeping with terminology changes recommended by the BMA re ‘resident doctors’.
- Feedback from resident doctor representatives raised a query about use of trust taxis to return home from a non-resident shift. Advice regarding use of the on call hotel room (prebookable) or facilities at the Becklin Centre (if no hotel prebooking has been made) for rest was reiterated as use of trust taxis for this reason cannot be supported with viable alternatives already available.
- Work schedules continue to be collected by MEC to ensure compliance with this. Whilst LTHT hold responsibility for work scheduling as lead employer for foundation doctors, to satisfy LYPFT that such doctors are given the opportunity to agree a personalised work schedule, MEC are now collecting a ‘timetable’ from such doctors.
- Rota gaps were discussed and MEC advised that a ‘standby’ system has been implemented whereby doctors identify their ability to pick up rota gaps if required. This is mostly around gaps arising from sickness whereby there may be uncertainty as to if and when the doctor will be able to return to their shifts.
- Exception reports from the Q3 period were reviewed.
- The next RDF was scheduled for 25th April 2025.
3 – Conclusion
Exception Reporting has now been in place within the Trust since 2016 with the first ER being made in 2017. We continue to work with resident doctors and clinical supervisors to ensure that we are developing a culture where ERs are positively received and used as a mechanism to effect change. Examples of this includes the agreed process for MEC to oversee any missed educational opportunities related to ALPS and offer additional opportunities where required, and also more recent agreements via the RDF precipitated by ERs associated with breaches in the T+Cs. Through MEC colleagues, the RDF, and GOSW attendance at induction for new starters, we continue to support the position that doctors are encouraged to work according to the T+Cs for their own safe practice and the safe care of patients. GOSW fines have been levied in Quarters 3 and 4. Spending of such fine monies will be agreed through the RDF. There are anticipated changes to the Exception Reporting process from September 2025 as per the new ‘Framework Agreement’, however further guidance to support implementation of this is yet to be provided by the BMA and NHS Employers.
4 – Recommendations
The Board of Directors are asked:
- To agree that this reports provides an assurance level for the systems in place to support the working arrangements of the 2016 TCS for the resident doctors working in the Trust and that they are meeting their objective of maintaining safe services
- To provide constructive challenge where improvement could be identified within this system
Dr Rebecca Asquith
GMC 7151560
Guardian of Safe Working Hours
Cover sheet for Chair’s Report from the Workforce Committee meeting on 5 June 2025
- Paper title: Chair’s Report from the Workforce Committee meeting on 5 June 2025
- Date of meeting: 31 July 2025
- Presented by: Zoe Burns-Shore, Non-executive Director and Chair of the Workforce Committee
- Prepared by: Rose Cooper, Deputy Head of Corporate Governance
This paper supports the Trust’s strategic objective/s (SO):
- SO2 – We provide a rewarding and supportive place to work.
This paper relates to the Trust’s strategic risks (SR):
- SR3 – Culture and environment for the wellbeing of staff
Committee details:
- Name of Committee: Workforce Committee – Part A
- Date of Committee: 5 June 2025
- Chaired by: Zoe Burns-Shore, Non-executive Director
Alert – items to alert the Board to:
- No items to alert the Board to.
Advise – items to advise the Board on
The Committee received the People and Organisational Development POD Governance Group Chair’s Report and noted the advisory item in relation to Job Evaluation and the need for NHS organisations to correctly and robustly apply the NHS Job Evaluation Scheme to ensure consistency and local compliance. The Committee understood that boards needed to demonstrate ownership of local Job Evaluation and to be assured that it was being implemented correctly and noted that a future agenda item on this would come to the Workforce Committee ahead of the Board of Directors.
The Committee received a report which summarised the work to ensure the Trust provides high quality learning environments for all learners across the organisation. The Committee was made aware of an issue around the suitability of the Trust’s estate, noting that it was often a struggle to find adequate space to deliver face to face sessions, which was generally students’ preferred approach to learning. The Committee noted this challenge and the potential impact on the student experience and agreed to highlight this issue to the Board of Directors via the Chair’s Report, noting that there may be opportunities to collaborate with partners on learning space. The Committee also heard about a long-standing issue regarding wheelchair accessibility at some community sites which had been brought to the attention of the Practice Learning and Development and Medical Education teams as part of their efforts to support learners who were wheelchair users.
The Committee discussed clinical supervision compliance as part of the Workforce Performance Report, noting that compliance was consistently below target. The Committee understood the current issues regarding the recording of clinical supervision and noted the mitigations in place. The Committee heard that Audit Yorkshire had recently undertaken an audit of clinical supervision and agreed to wait until the recommendations had been completed and to monitor the impact on compliance. The Committee also noted that clinical supervision compliance was discussed at the Quality Committee.
Assure – items to provide assurance to the Board on
The Committee reviewed the Board Assurance Framework so that it could be mindful of its responsibility to assure that Strategic Risk (SR) 3 was being adequately controlled through the course of the meeting. The Committee was assured that SR3 was being adequately controlled; considered whether it was receiving assurance on any gaps through the reports it was already receiving; and agreed that it did not require any further assurance on the way in which SR3 was being managed.
The Committee asked if the associated cost savings of moving clinical agency staff onto the Bank could be demonstrated and heard that there was no real difference in the day rate between bank and agency staff and that agency staff working nights and weekends cost on average only £1 an hour more than bank staff. The Committee understood that the collaborative work on the agency cluster contract had helped to keep agency costs to a minimum. The Committee agreed to include this information in the Chair’s Report to the next Board of Directors’ meeting as an item for assurance.
The Committee received a “deep dive” into the data collected for consultant recruitment from April 2024 to April 2025 which was requested in response to the previous year’s Medical Workforce Race Equality Standard indicating that white British doctors were more likely to get shortlisted and selected for consultant posts compared to Black, Asian and Minority Ethnic (BAME) doctors. The Committee noted that although white British candidates had a higher success rate in terms of being appointed compared to BAME candidates, the process of shortlisting appeared to be equitable. The Committee highlighted the assurance provided in terms of the Trust being an equitable employer, noting that there were legitimate reasons for those who were not appointed.
Refer – Items to be referred to other Committees:
- No items to be referred to other Committees.
Recommendation
The Board of Directors is asked to note the update provided.
Cover sheet for Report from the Director of People and Organisational Development
- Paper title: Report from the Director of People and Organisational Development
- Date of meeting: 31 July 2025
- Presented by: Darren Skinner, Director of People and Organisational Development
- Prepared by: Andrew McNichol, Head of People Analytics and Temporary Staffing
This paper supports the Trust’s strategic objective/s (SO):
- SO2 – We provide a rewarding and supportive place to work.
- SO3 – We use our resources to deliver effective and sustainable services.
This paper relates to the Trust’s strategic risks (SR):
- SR1 – Quality including safety assurance processes
- SR3 – Culture and environment for the wellbeing of staff
- SR5 – Adequate working and care environments
- SR6 – Digital technologies
- SR7 – Plan and deliver services that meet the health needs of the population we serve.
Executive summary
The purpose of this report if to provide the board with an overview of the key workforce demographics linked to our people and highlight the plans in place to support performance in the context of the Trust People Plan.
Do the recommendations in this paper have any impact upon the requirements of the protected groups identified by the Equality Act? No.
Recommendation
The Board is asked to receive and note the report.
Report from the Director of People and Organisational Development
The purpose of this report if to provide the board with an overview of the key workforce demographics linked to our people and highlight the plans in place to support performance in the context of the Trust People Plan.
Summary of key points:
- The staffing distribution across the organisation reflects a continued high dependency on temporary staffing to meet the patient need. The agency element is being minimised through various workforce efficiency interventions but Bank working still plays a significant role in meeting the demand across all services. Bank workers are being used to backfill vacancy, absence and acuity/activity and this month’s report explores the distribution.
- The age and ethnicity profile of our workforce is broadly representative of the local population.
- The Trust sickness absence rate for this quarter is 5.73% This is an increase from 5.54% for the same period last year.
- The rolling 12-month sickness absence rate is 6.01% (Jul 25) and the Trust was one of the top 3 Trust in the region with the highest sickness rates based on the NHS Digital benchmarking data (Feb 25).
- The top five reasons for sickness absence over the last 12 months account for over 72% of all sickness within the Trust.
- PDR compliance has remained within tolerance of target 85% (+/- 5% of target) for 12 consecutive months. December reporting reflected some slippage against target, but July shows a growing recovery back to 83%.
- Clinical Supervision compliance continues to fluctuate between 70-80% With all but four services within 10% of target. The clinical supervision module expiration is 8 weeks so compliance can significantly fluctuate day to day.
- Compliance has been stable over the 13-month period averaging 86.6%. In July 2025 88.23% of staff have in-date mandatory training, above the 85% target.
Paper Author: Andrew McNichol (Head of People Analytics and Temporary Staffing)
Executive Sponsor: Darren Skinner (Director of People and Organisational Development
1.1 – Our People
Commitment: Deliver effective workforce planning processes which focus on recruitment and retention, new roles, skills mixing and future supply pathways to ensure a fit for purpose workforce for now and the future.
Resource Distribution and Staffing Fulfilment
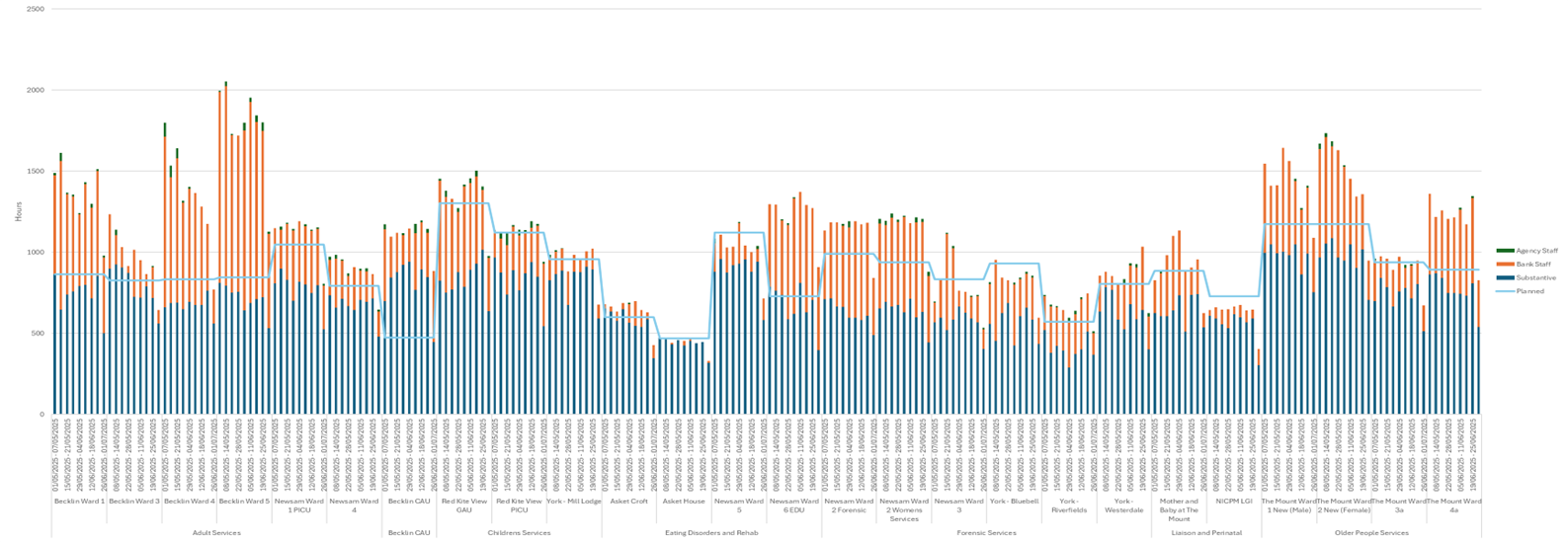
The chart above represents the unit fulfilment distribution for all inpatient services for Jan-Feb 25 by Week/Ward/Service (Blue – Substantive, Orange – Bank, Green – Agency). The scale is deliberately set to demonstrate the overall usage and temporary staffing dependency across the Inpatient Services. The planned hours represented by the blue line is the RN and HCA requirement for the ward and the bar columns represent the combined RN and HCA hours per 24 day.
The chart demonstrates the demand over and above the established budget that is being requested to support the additional staffing requirements. An establishment review is currently underway across all services to review the planned hours by unit. E.g. W5 Newsam’s planned establishment is currently incorrect on the roster and the ward is meeting with the rostering teams and Finance to address this anomaly.
Older Peoples Services
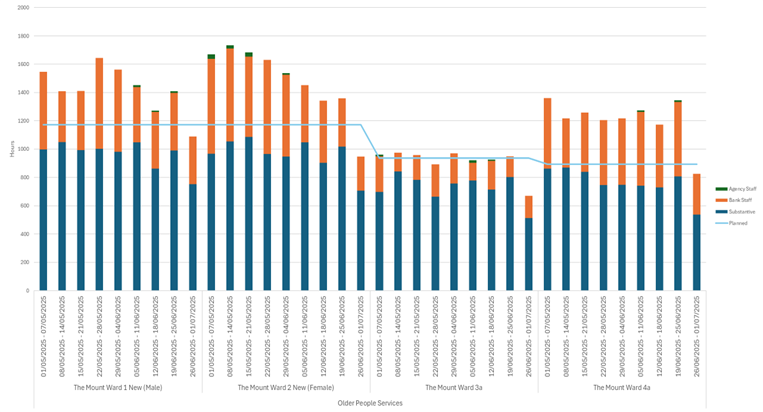
Adult Services

Forensic Services
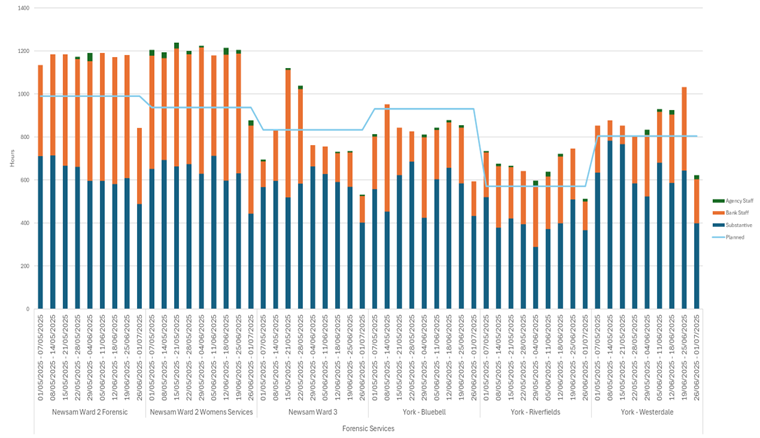
Children’s Services
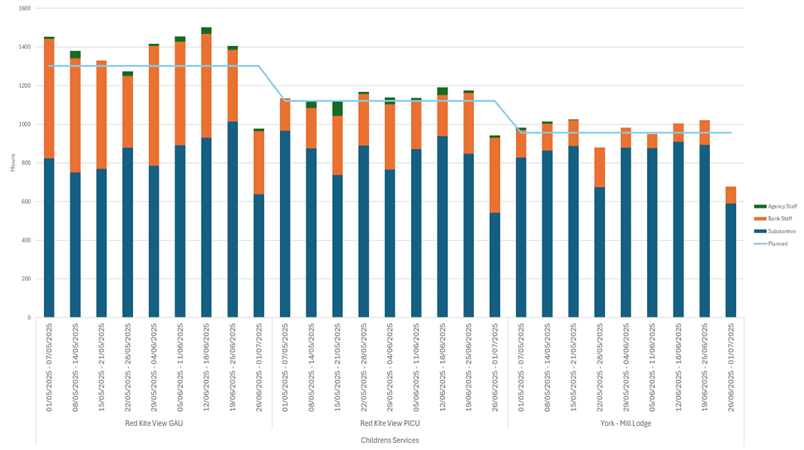
Eating Disorders and Rehabilitation
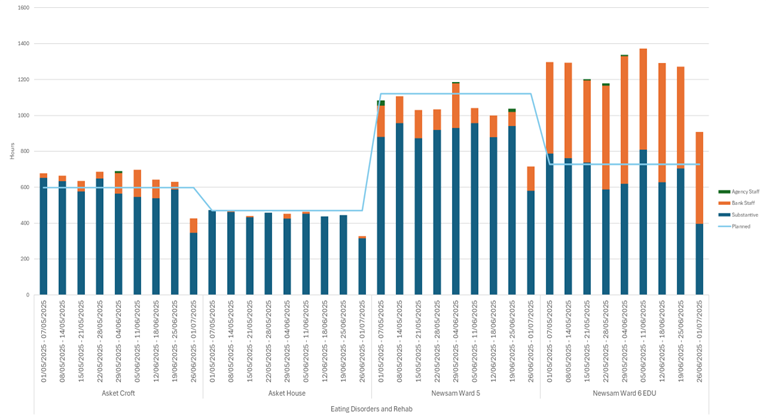
Liaison and Perinatal
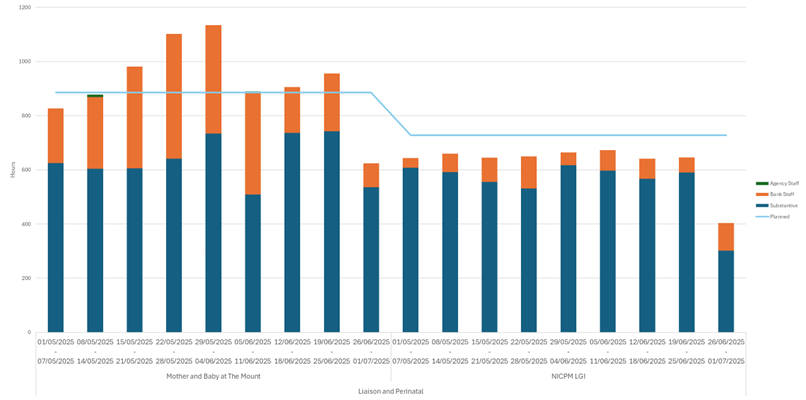
1.2 – Our People Profile
Our People – Substantive
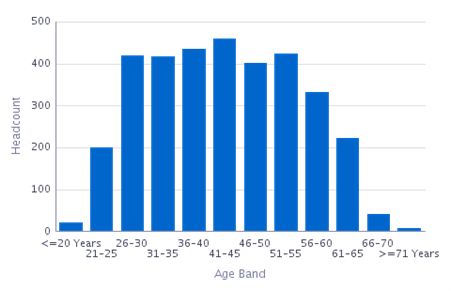
Our People – Bank
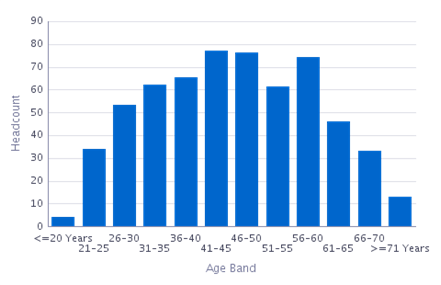
Ethnicity Profile (Substantive)

Ethnicity Profile (Bank)
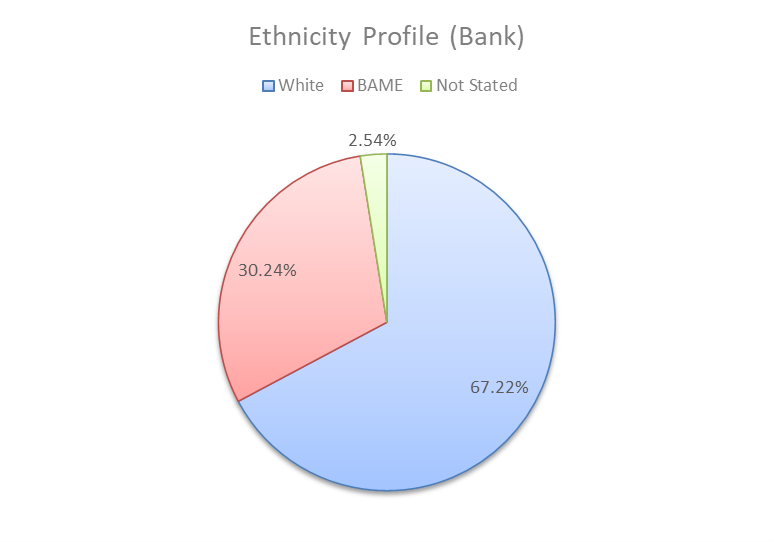
Disability Profile (Substantive)
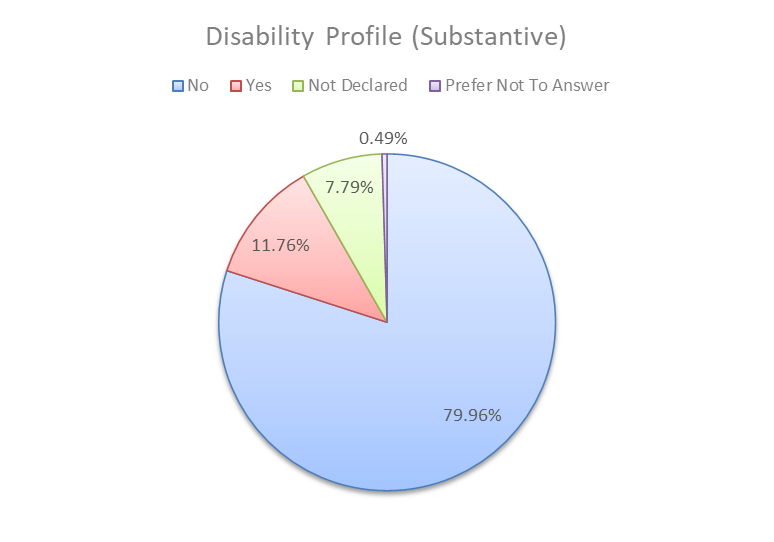
Disability Profile (Bank)
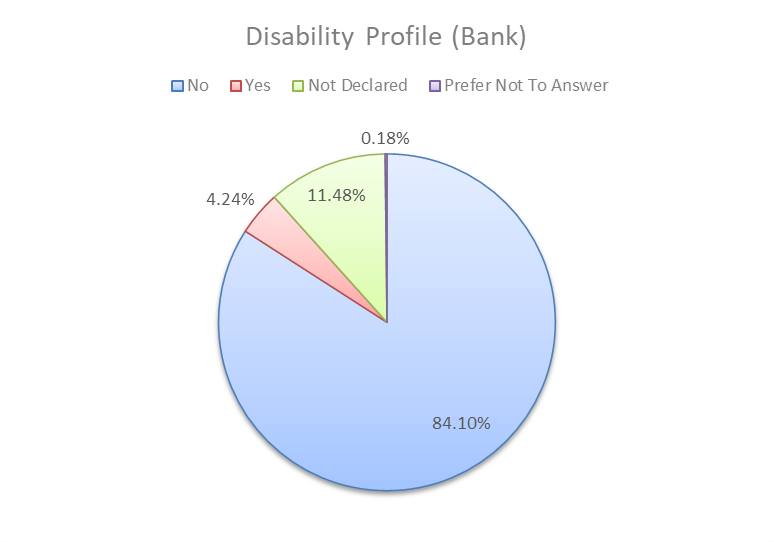
Gender Profile

Gender Pay Profile

1.3 – Our People Representation
Comparison of BME representation in workforce compared to census data of both Leeds and Yorkshire
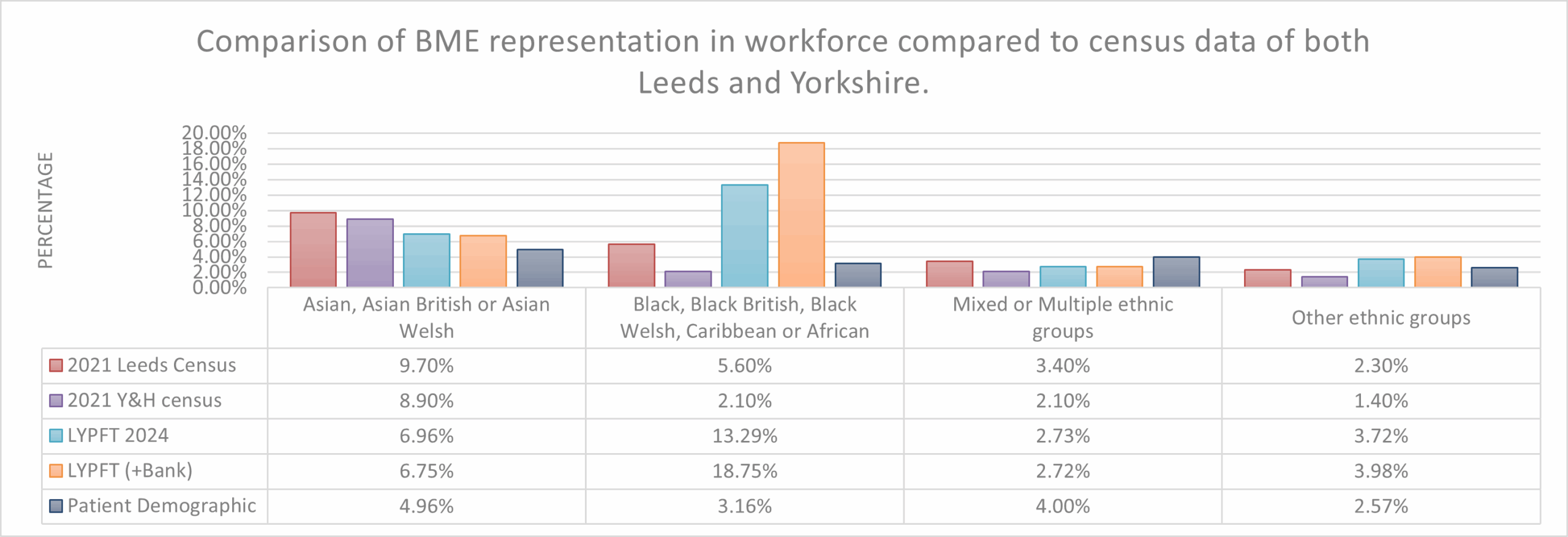
Ethnicity Pay Profile
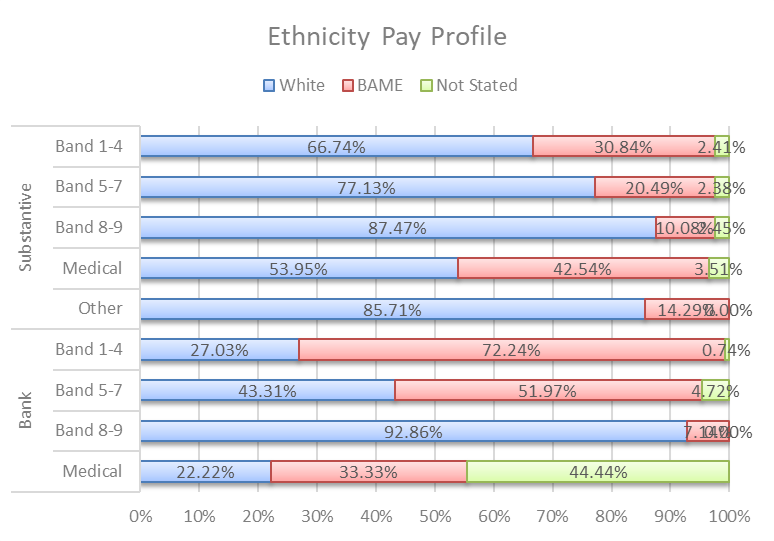
Key Points
- The age and ethnicity profile of our workforce is broadly representative of the local population even when considered against the patient ethnicity profile which reflects the impacts of health inequality of the broader Leeds and York census population.
Ethnicity:
- The Trust Asian representation is circa 2.7% lower than the ONS data for the city and 2% lower than the region.
Age:
- The Trust has a high proportion of employees who are aged between 35 and 64 (approximately 60%) and is slightly under-represented in the lower and higher age bandings. Point to note – The census data include all people up to twenty which distorts the percentage in the census when compared to the working age adults in LYPFT data.
Commitment: Improve the experience of those people with a protected characteristic as identified by the Equality Act.
People Plan Objectives for 2025:
- Embed the mediation support offer into business as usual processes by establishing a network of trained, supervised and effective mediators in-house, this will include the integration of early resolution training into the Manager 360 programme.
- Board members should demonstrate how organisational data and lived experience have been used to improve culture (March 2025)
- Evidence progress of implementation of the EDI NHS Improvement plan (by June 2025) and by October 2025 implement plan to widen recruitment opportunities within local communities.
- Develop and implement an improvement plan to eliminate pay gaps. Implement “Mend the Gap” review for medical staff and effective flexible working options. Analyse data to understand pay gaps by protected characteristics and develop an improvement plan.
- Through upskilling and increased awareness, influence the culture to support eliminating the conditions in which bullying, discrimination, harassment and physical violence at work occur. Refer to the EDI Improvement plan for deliverables.
- Work in partnership with community organisations to implement and embed the improvement plan for health inequalities
- To grow the reciprocal mentoring programme to be part of EDI objectives and identify a number from each service line.
- Review and implement employment practices and support for our Neurodiversity colleagues and their managers.
Comparison of Age representation in workforce compared to census data of both Leeds and Yorkshire
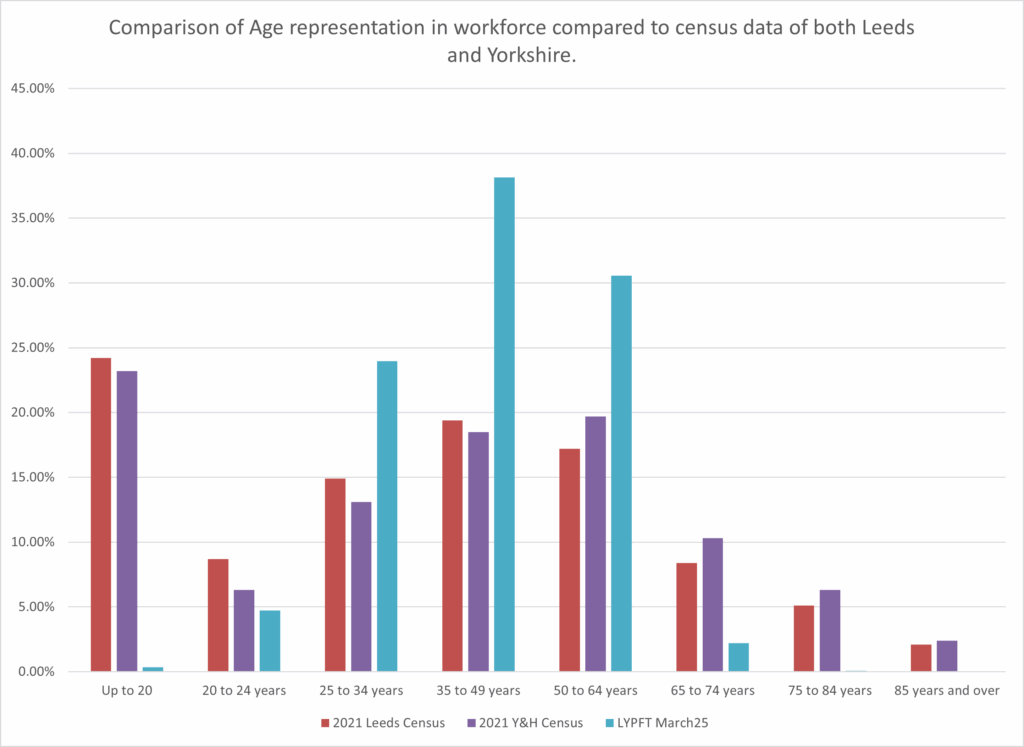
1.4 – Our People – Absence
| Absence FTE % | Absence Days | Absence FTE | Available FTE |
| 6.01% | 75,552 | 66,952.68 | 1,114,503.64 |
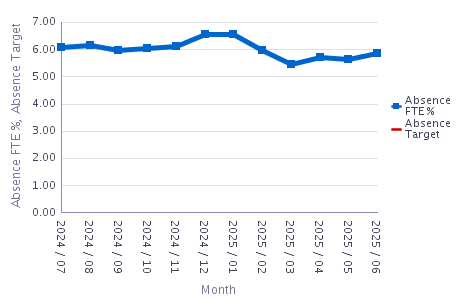
| Service Level | Absence Occurrences | LT Absence Occurrences | ST Absence Occurrences |
| Adult Acute Services | 1,104 | 112 | 992 |
| Care Services Other | 70 | 10 | 60 |
| Chief Operating Officer | 8 | 0 | 8 |
| Children and Young People’s Services | 525 | 33 | 492 |
| Community and Wellbeing Services | 452 | 64 | 388 |
| Corporate Services | 856 | 93 | 763 |
| Eating Disorders and Rehabilitation and Gender Services | 695 | 82 | 613 |
| Forensic Services | 602 | 52 | 550 |
| Learning Disability Services | 700 | 87 | 613 |
| Liaison and Perinatal Services | 446 | 36 | 410 |
| Older Peoples Services | 833 | 83 | 750 |
| Regional and Specialist Services | 303 | 38 | 265 |
| Resident Doctors Primary Care | 2 | 0 | 2 |
| WY MHLDA Programme Team | 1 | 0 | 1 |
| Grand Total | 6,607 | 691 | 5,916 |
Absence Long-Short Term
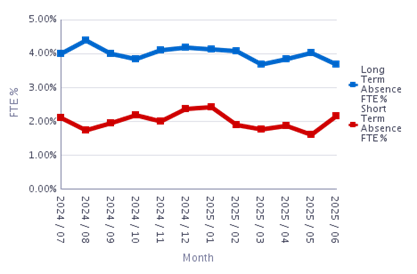
Absence by length

Regional NHS time lost to absence (Year to Feb 2025)

Ensure our people have equal access to and use a full range of well-being support – physical, psychological, financial, and social.
- Put in place a Standard Operating Procedure for reasonable workplace adjustments which includes targets and waiting times this needs to have support from Procurement, Informatics and Finance.
- Review the Partnership Agreement with Occupational Health
- Achieve Menopause Accreditation and aspire to be a leading Trust for Menopause awareness and support Develop a Menopause Policy and grow and develop the support network
Key Points
- The Trust sickness absence rate for this quarter is 5.73% This is an increase from 5.54% for the same period last year.
- The rolling 12-month sickness absence rate is 6.01% (Jul 25) and the Trust was one of the top 3 Trust in the region with the highest sickness rates based on the NHS Digital benchmarking data (Feb 25).
- The top five reasons for sickness absence over the last 12 months account for over 72% of all sicknesswithin the Trust.
| Service Level | Absence Occurrences | LT Absence Occurrences | ST Absence Occurrences |
| Adult Acute Services | 1,104 | 112 | 992 |
| Care Services Other | 70 | 10 | 60 |
| Chief Operating Officer | 8 | 0 | 8 |
| Children and Young People’s Services | 525 | 33 | 492 |
| Community and Wellbeing Services | 452 | 64 | 388 |
| Corporate Services | 856 | 93 | 763 |
| Eating Disorders and Rehabilitation and Gender Services | 695 | 82 | 613 |
| Forensic Services | 602 | 52 | 550 |
| Learning Disability Services | 700 | 87 | 613 |
| Liaison and Perinatal Services | 446 | 36 | 410 |
| Older Peoples Services | 833 | 83 | 750 |
| Regional and Specialist Services | 303 | 38 | 265 |
| Resident Doctors Primary Care | 2 | 0 | 2 |
| WY MHLDA Programme Team | 1 | 0 | 1 |
| Grand Total | 6,607 | 691 | 5,916 |
1.5 – Our People – Retention
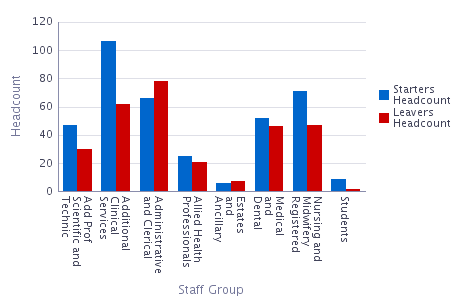
Turnover Rate (12m)
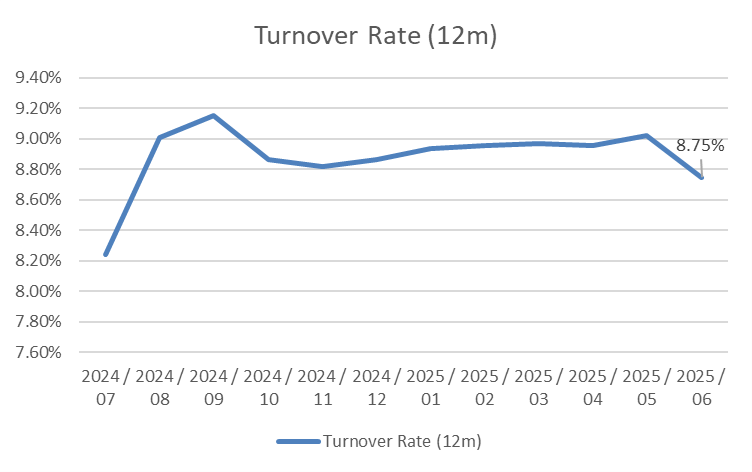
Starters / Leavers by Service Area

Leaver Destination

Leavers by Staff Group
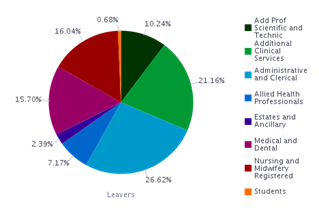
Leavers by Reason

Develop and implement an innovative approach to talent development, embedding the right culture and improving retention through delivery of our retention strategy.
- Pilot the new Succession Planning approach with EMT/SMT
- Launch the Stay Conversation approach.
Increase the opportunities for flexible working across the Trust, including flexible retirement options.
- Deliver the flexible working priorities including the revised procedure, manager training and comms plan.
1.6 Our People – Learning and Development
Performance Development Reviews

Compulsory Training
Clinical Supervision
| Requirement | Care Service | Number compliant | Number non-compliant | Total Headcount | Compliance status |
| Annual Appraisal | Adult Acute Services | 207 | 97 | 304 | 68% |
| Annual Appraisal | Care Services Other | 29 | 8 | 37 | 78% |
| Annual Appraisal | Chief Operating Officer | 5 | 1 | 6 | 83% |
| Annual Appraisal | Children and Young People’s Services | 116 | 28 | 144 | 81% |
| Annual Appraisal | Community and Wellbeing Services | 186 | 37 | 223 | 83% |
| Annual Appraisal | Corporate Services | 525 | 100 | 625 | 84% |
| Annual Appraisal | Eating Disorders and Rehabilitation and Gender Services | 215 | 25 | 240 | 90% |
| Annual Appraisal | Forensic Services | 181 | 19 | 200 | 91% |
| Annual Appraisal | Learning Disability Services | 299 | 32 | 331 | 90% |
| Annual Appraisal | Liaison and Perinatal Services | 161 | 35 | 196 | 82% |
| Annual Appraisal | Older Peoples Services | 265 | 59 | 324 | 82% |
| Annual Appraisal | Regional and Specialist Services | 133 | 18 | 151 | 88% |
| Annual Appraisal | Trust Board – Executive Directors | 4 | 1 | 5 | 80% |
| Annual Appraisal | Trust Board – Non-Executive Directors | 0 | 7 | 7 | 0% |
| Requirement | Care Service | Number compliant | Number non-compliant | Total Headcount | Compliance status |
| Clinical Supervision | Learning Disability Services | 106 | 14 | 120 | 88% |
| Clinical Supervision | Forensic Services | 159 | 26 | 185 | 86% |
| Clinical Supervision | Eating Disorders and Rehabilitation and Gender Services | 178 | 40 | 218 | 82% |
| Clinical Supervision | Regional and Specialist Services | 113 | 26 | 139 | 81% |
| Clinical Supervision | Liaison and Perinatal Services | 123 | 32 | 155 | 79% |
| Clinical Supervision | Care Services Other | 14 | 5 | 19 | 74% |
| Clinical Supervision | Children and Young People’s Services | 104 | 37 | 141 | 74% |
| Clinical Supervision | Older Peoples Services | 196 | 73 | 269 | 73% |
| Clinical Supervision | Community and Wellbeing Services | 103 | 61 | 164 | 63% |
| Clinical Supervision | Corporate Services | 3 | 2 | 5 | 60% |
| Clinical Supervision | Adult Acute Services | 170 | 117 | 287 | 59% |
| Care Service | Number compliant | Number non-compliant | Total Headcount | Compliance status |
| Overall | 1269 | 433 | 1702 | 75% |
Provide accessible and intuitive software solutions to support People and OD initiatives.
- Complete a tender exercise for a new employee relations case management system for HR.
- Assess the feasibility of AI applications in POD, conduct pilot programs in at least two areas, and implement AI solutions where efficiency gains exceed 20%.
- Implement a new SW form workflow
Key Points
PDR
- PDR compliance has remained within tolerance of target 85% for eighteen consecutive months.
- December reporting reflected some slippage against target, but July shows a growing recovery back to 83%.
Clinical Supervision
- Clinical Supervision compliance continues to fluctuate between 70-80% With all but four services within 10% of target. The clinical supervision module expiration is 8 weeks so compliance can significantly fluctuate day to day. Especially at year end with increased levels of annual leave.
Compulsory Training
Compliance has been stable over the 13-month period averaging 86.6%. In July 2025 88.23% of staff have in-date mandatory training, above the 85% target.
Culture Dashboard Update:
The Trust has introduced a new strategic objective for 2025, responsibility for which will sit in the POD Directorate. The objective is to develop a Culture Dashboard that uses key workforce demographics and indicators including data derived from our Staff Survey to demonstrate the Culture at LYPFT. Whilst the dashboard is still in its formative stages, it is envisaged that it will incorporate three domains linked to the People Plan:
Domain 1: Civility and Respect
Sub-groups – Staff Survey, Employee Relations, Compulsory Training compliance, Sickness Absence.
Domain 2: Equality Diversity and Inclusion
Sub-groups – Staff Survey, Workforce Race and Disability Equality Standards, Gender, Ethnicity and Disability pay gap data, demographic data analysis and comparators to national census and patient ethnicity data.
Domain 3: Leadership
Sub-groups – Staff Survey, Performance Development Review compliance, Manager 360 attendance, CPD adoption and Apprenticeship data.
The three domains will be introduced in phases over the coming year, and the stakeholder groups are being organised to inform a technical specification that will help the Informatics team plan the architecture and delivery schedule. It is important to note that the focus will remain on utilising existing, available data to start with and as the project progresses the listed sub-groups may change to incorporate new/different data as it becomes available.
Definition of Staff Groups
| Staff group | Acronym | Description |
| Add Prof Scientific and Technic | APS and T | All Qualified Technical Staff & Pharmacists – e.g. Optometrists, ODPs, General Technicians |
| Additional Clinical Services | ACS | All Unqualified Nursing Staff, Therapy Staff & Technical & Scientific Staff – e.g. Support Workers, Play Specialists, Physio Assistants |
| Administrative and Clerical | A and C | All Admin & Clerical Staff – e.g. Clerical staff, Managers, Senior Managers |
| Allied Health Professionals | AHP | All Qualified AHP Staff – e.g. Physios, Dieticians, Orthoptists |
| Estates and Ancillary | E and A | All Ancillary and Maintenance Staff – e.g. Domestics, Porters, Housekeepers, Joiners, Craftsman |
| Healthcare Scientists | HCS | All Scientific Staff – e.g. Biomedical Scientists, Scientists |
| Medical and Dental | M and D | All Medical Staff – e.g. Junior Doctors, Consultants |
| Nursing and Midwifery Registered | N and M | All Qualified Nursing Staff – e.g. Staff Nurse, Ward Manager, Health Visitors |
Definition of Other Terms
| Terms | Acronym | Description |
| Black and Minority Ethnic groups | BME | Term used to refer to members of non-white communities in the UK |
| Full Time Equivalent | FTE | The unit used to show the equivalence to a full-time member of staff. Sometime referred to as Whole Time Equivalent (WTE). E.g. a nurse working 30 hours per week would have an FTE of 0.80 |
| Key Performance Indicator | KPI | A type of measurement to evaluate success against a given target |
| Personal Development Review | PDR | Annual appraisal of staff performance and development |
Cover sheet for Chair’s Report from the Extraordinary Audit Committee meeting on 17 June 2025
- Paper title: Chair’s Report from the Extraordinary Audit Committee meeting on 17 June 2025
- Date of meeting: 31 July 2025
- Presented by: Martin Wright, Non-executive Director, and Chair of the Audit Committee
- Prepared by: Kieran Betts, Corporate Governance Officer
This paper supports the Trust’s strategic objective/s (SO):
- SO1 – We deliver great care that is high quality and improves lives.
- SO2 – We provide a rewarding and supportive place to work.
- SO3 – We use our resources to deliver effective and sustainable services.
This paper relates to the Trust’s strategic risks (SR):
- SR1 – Quality including safety assurance processes
- SR3 – Culture and environment for the wellbeing of staff
- SR4 – Financial sustainability
- SR5 – Adequate working and care environments
- SR7 – Plan and deliver services that meet the health needs of the population we serve.
Committee details:
- Name of Committee: Extraordinary Audit Committee
- Date of Committee: 17 June 2025
- Chaired by: Martin Wright, Non-executive Director
Alert – items to alert the Board to:
- No issues to which the Board needs to be alerted.
Advise – items to advise the Board on
- No issues to which the Board need to be advised.
Assure – items to provide assurance to the Board on
- The Committee received the Audited Annual Accounts 2024/25 and agreed to recommend that the Board adopt these accounts.
- The Committee received the ISA 260 Report and was assured that no significant control issues had been identified.
- The Committee agreed to recommend to the Board that the Chief Executive signs and returns the letter of representation to the external audit team.
- The Head of Internal Audit Opinion had been received and reported an overall position of significant assurance.
- The Committee received the Annual Governance Statement and agreed to recommend to the Board that the Chief Executive signs off the statement, subject to some agreed minor amendments.
- The Committee received the Annual Report 2024/2025 and was assured by the process to develop it and its content. It agreed that it should be adopted by the Board, subject to some agreed minor amendments.
- The Committee was assured the Trust was compliant with the Code of Governance and agreed to assure the Board that the “explain” elements of the code were included in the Annual Report.
Refer – Items to be referred to other Committees:
- No items were referred to other Board Committees.
Recommendation
The Board of Directors is asked to note the update provided.
Cover sheet for Chair’s Report from the Audit Committee meeting on 15 July 2025
- Paper title: Chair’s Report from the Audit Committee meeting on 15 July 2025
- Date of meeting: 31 July 2025
- Presented by: Martin Wright, Non-executive Director, and Chair of the Audit Committee
- Prepared by: Kieran Betts, Corporate Governance Officer
This paper supports the Trust’s strategic objective/s (SO):
- SO1 – We deliver great care that is high quality and improves lives.
- SO2 – We provide a rewarding and supportive place to work.
- SO3 – We use our resources to deliver effective and sustainable services.
This paper relates to the Trust’s strategic risks (SR):
- SR1 – Quality including safety assurance processes
- SR3 – Culture and environment for the wellbeing of staff
- SR4 – Financial sustainability
- SR5 – Adequate working and care environments
- SR7 – Plan and deliver services that meet the health needs of the population we serve.
Committee details:
- Name of Committee: Audit Committee
- Date of Committee: 15 July 2025
- Chaired by: Martin Wright, Non-executive Director
Alert – items to alert the Board to:
- No issues to which the Board needs to be alerted.
Advise – items to advise the Board on
- The “Integrated Governance and Risk Management Framework” internal audit report was received with a split assurance opinion, with the Board Assurance Framework elements receiving an opinion of significant assurance, and the Risk Management Framework elements receiving an overall opinion of limited assurance. The Committee was assured on the actions being taken to address the issues identified in the report and was reassured that all these actions were due to be completed in the timeline outlined in the report.
- The “Service Use Monies” internal audit report was received with an opinion of low assurance. The Committee was reassured that the issues which had been identified in the report were mostly known to the Trust. It was assured by the actions being taken to address the issues identified in the report and the progress of these actions and was reassured that all these actions were due to be completed in the timeline outlined by the report.
- The Committee received the updated Internal Audit Plan for 2025/26 and noted that due to ongoing work, Audit Yorkshire would contact the relevant Executive Director to check whether the following audits should remain on this plan or be deferred: Data Quality: Clinical Quality Dashboard, Mandatory and Statutory Training, and Minimising Self-Harm and Suicide. It additionally agreed to consult the Workforce Committee on whether the scope of the “Retention and Wellbeing” internal audit should be changed so that the Trust’s Bullying and Harassment arrangements were not assessed as part of this audit, but instead assessed in a separate audit on the 2026/27 plan.
- The Committee received the Health and Safety Annual Report for 2024/25. It commended the development of the report compared with previous iterations. It questioned some of the data presented in the report, such as incidents of violence and aggression involving staff and service users being presented separately and the recording of 6526 “Health and Safety Incidents” when historical Datix categorisation made this too ambiguous to separate or define accurately. It was agreed that additional caveats would be inserted into the report to provide additional clarity and transparency in this area prior to it being shared to the Board of Directors at its July 2025 meeting.
Assure – items to provide assurance to the Board on
- The Committee members met with Ms Helen Higgs and Mr Jonathan Hodgson in a private meeting ahead of the main meeting and were reassured that there were no items of concern from the internal audit team to escalate ahead of the meeting.
- The Committee received the Risk Management Annual Report and noted that the report demonstrated continued improvement within the risk management systems and processes.
- The Committee received the Internal Audit Progress Report and was assured that all of the audits on the 2024/25 internal audit plan had been completed and that good progress had been made on the delivery of the 2025/26 internal audit plan. It noted that seven internal audit report had been received since the Committee’s last meeting in April 2025 and that the results of these would be shared with the relevant Board Committee for that audit area. In addition to the Integrated Governance and Risk Management Framework and Service User Monies, these included:
- Time and Attendance Management – Significant Assurance.
- Patient Safety Incident Response Framework (PSIRF) – Significant Assurance
- Budgetary Controls: System Wide Review – Significant Assurance
- Procurement and Contract Management (Joint with LCH) – Advisory only.
- Data Security and Protection Toolkit – Moderate overall risk with medium confidence level of independent assessment.
- It was additionally noted that the Trust was ahead of its peers in implementing the PSIRF across the organisation and that this would be confirmed in a later thematic report.
- The Committee received and noted the contents of the Outstanding Audit Actions Report. It noted that a new extension process would be proposed at the July 2025 Executive Risk Management Group (ERMG) so that all extensions over six-months in length would require approval from the relevant Executive Director ahead of being proposed at ERMG. It also noted the importance of agreeing a challenging implementation timeframe which was proportional to the priority rating of the recommendation and sticking to this timeframe where possible.
- The Committee received the Local Counter Fraud Annual Report for 2024/25 and noted the contents. It was assured that the Counter Fraud Functional Standard had been submitted to the NHS Counter Fraud Authority on time and that the Trust was rated green in all 13 components.
- The Committee received and approved the Local Counter Fraud Annual Work Plan for 2025/26.
- The Committee received and noted the contents of the Local Counter Fraud Progress Report.
- The Committee received and was assured by the Health and Safety 2025/26 Quarter 1 Update Report.
- The Committee received the NHS Provider: Strategic Risk Benchmarking report from the external audit team and was assured that the Trust’s oversight of risks was in-line with other similar organisations.
- The Committee noted and was assured that there were no tender waivers or quotation waiver reports for the period of 1 April 2025 – 30 June 2025.
- The Committee received the Sponsorship, Hospitality, and Gift Registers and noted their contents. It noted that there were no sponsorships declared in the 2024/25 period and questioned whether as part of the medical revalidation process, relevant staff could be asked to confirm that they had no sponsorship, hospitality, or gifts to declare in the period.
- The Committee reviewed the responses to the Annual Committee Effectiveness and Committee Processes questionnaires. The Committee was assured based on this feedback that the Committee was working effectively in accordance with its terms of reference and to best practice as set out in the HFMA Audit Committee Handbook.
Refer – Items to be referred to other Committees:
- It was agreed that the Patient Safety Incident Response Framework internal audit report and the subsequently produced thematic report from Audit Yorkshire would be referred to the Quality Committee.
- It was agreed that the Time and Attendance Management internal audit report would be referred to the Workforce Committee.
- It was agreed that the Data Security and Protection Toolkit internal audit report and the subsequently produced thematic report from Audit Yorkshire would be referred to the September 2025 Finance and Performance Committee.
- It was agreed that the proposal to change the scope of the “Retention and Wellbeing” internal audit so that the Trust’s Bullying and Harassment arrangements were not assessed as part of this audit but instead assessed in a separate audit on the 2026/27 plan due to the planned rollout of the Trust’s Civility and Respect project would be referred to Workforce Committee.
Recommendation
The Board of Directors is asked to note the update provided.
Cover sheet for Board Assurance Framework (BAF) 2025/26
- Paper title: Board Assurance Framework 2025/26
- Date of meeting: 31 July 2025
- Presented by: Dr Sara Munro, Chief Executive
- Prepared by: Clare Edwards, Associate Director of Corporate Governance
This paper supports the Trust’s strategic objective/s (SO):
- SO1 – We deliver great care that is high quality and improves lives.
- SO2 – We provide a rewarding and supportive place to work.
- SO3 – We use our resources to deliver effective and sustainable services.
This paper relates to the Trust’s strategic risks (SR):
- SR1 – Quality including safety assurance processes
- SR2 – Delivery of the Quality Strategic Plan
- SR3 – Culture and environment for the wellbeing of staff
- SR4 – Financial sustainability
- SR5 – Adequate working and care environments
- SR6 – Digital technologies
- SR7 – Plan and deliver services that meet the health needs of the population we serve.
Executive summary
It is a requirement for all Trust Boards to ensure there is an effective process in place to identify, understand, address, and monitor risks. This includes the requirement to have a Board Assurance Framework that sets out the risks to the strategic plan by bringing together in a single place all the relevant information on the risks to the Board being able to deliver the organisation’s objectives.
All risks have been reviewed and updated to ensure that they are representative of the current position for strategic risks. This has included score, controls, actions and contributory risks.
There are no key points for escalation to the Board of Directors within this update.
Over the next quarter work will be undertaken to align the strategic risks to the Trust operational priorities to demonstrate clear lines of assurance and mitigation.
Do the recommendations in this paper have any impact upon the requirements of the protected groups identified by the Equality Act? Yes
If yes, please set out what action has been taken to address this in your paper.
This is detailed within the strategic risks, specifically strategic risks 1 and 7.
Recommendation
The Board is asked to:
- Receive the BAF and to be assured of the revie that has been undertaken to ensure that this accurately reflects the position as of July 2025, including risk scoring and mitigating actions.
Board Assurance Framework (BAF) 2025/26
1 – Executive Summary
It is a requirement for all Trust Boards to ensure there is an effective process in place to identify, understand, address, and monitor risks. This includes the requirement to have a Board Assurance Framework that sets out the risks to the strategic plan by bringing together in a single place all the relevant information on the risks to the Board being able to deliver the organisation’s objectives.
2 – Board Assurance Framework
2.1 – Strategic Objectives
This Board Assurance Framework is informed by Trust strategy and the related strategic objectives. These are:
- Through our Care Services: we deliver great care that is high quality and improves lives.
- For our People: we provide a rewarding and supportive place to work.
- Using our resources wisely: we deliver effective and sustainable services.
2.2 – The BAF
Overall responsibility for the BAF sits with the Chief Executive and this is administered by the Associate Director for Corporate Governance who has a co-ordinating role in respect of the information, and for ensuring the document moves through its governance pathway effectively and provides check and challenge to the content.
This BAF sets out the principal risks and how they could impact on the strategic goals.
2.3 – Risk Management
The Board Assurance Framework has seven strategic risks. Each strategic risk has an assigned lead Executive Director who has oversight of the detail within the risk ensure identified actions are appropriate and have correct timeframes.
Board Committees review the BAF at their meetings to ensure that the risks remain appropriate and that there is assurance that they are appropriately managed.
The Executive Risk Management Group has oversight of all Trust risks, with specific focus on the strategic risks and risks rated 15 or above. There is a clear escalation route to the Executive Management Team and the Trust Board for any identified risk or action required.
2.4 – Structure of the BAF Risk Report
This report helps to focus the Executive and Board of Directors on the principal risks to achieving the Trust’s strategic goals and in-year objectives and to seek assurance that adequate controls and actions are in place to manage the risks appropriately.
The BAF is structured and mapped against the three strategic objectives.
Each of the risk scores identifies how the score has been calculated with likelihood and consequence ratings. This is shown as ‘LX x CX’ in the main body of the BAF.
2.5 – Strategic Risk Detail Updates
Following a review of the current position in relation to the strategic risks, there are no key updates for the Board of Directors to be aware of. Following the review and approval of the risk appetite statement and position for each strategic risk, this will be included in this report moving forward.
BAF Dashboard
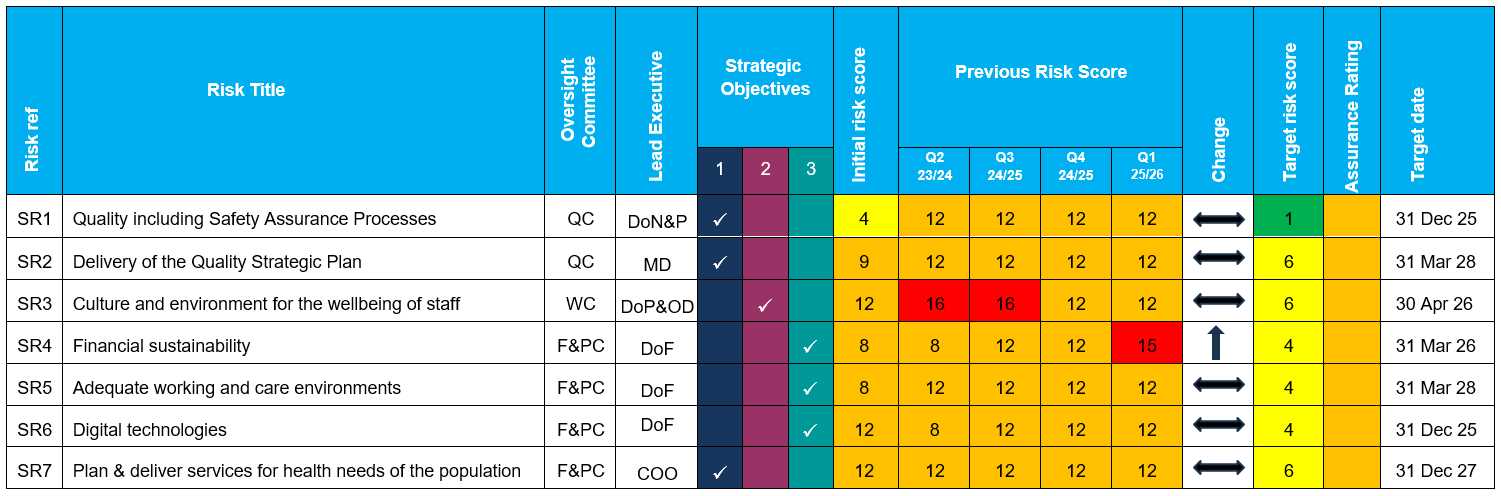
Strategic Risk Summary (as of Q1 2025/26) The organisation is currently monitoring seven strategic risks, each aligned with specific strategic objectives and overseen by relevant committees and executives. Below is a summary of each risk, its current status, and progress toward target scores: SR1 – Quality including Safety Assurance Processes Oversight: Quality Committee (QC) Lead: Director of Nursing and Patient Experience Current Risk Score: 12 (unchanged from previous quarters) Target Score: 1 Target Date: 31 Dec 2025 Assurance Rating: Q2 23/24 SR2 – Delivery of the Quality Strategic Plan Oversight: QC Lead: Medical Director Current Risk Score: 12 (stable) Target Score: 6 Target Date: 31 Mar 2028 Assurance Rating: Q2 23/24 SR3 – Culture and Environment for Staff Wellbeing Oversight: Workforce Committee (WC) Lead: Director of People and Organisational Development Current Risk Score: 12 (improved from 16) Target Score: 6 Target Date: 30 Apr 2026 Assurance Rating: Q3 24/25 SR4 – Financial Sustainability Oversight: Finance and Performance Committee (F&PC) Lead: Director of Finance Current Risk Score: 15 (increased from 12) Target Score: 4 Target Date: 31 Mar 2026 Assurance Rating: Q4 24/25 SR5 – Adequate Working and Care Environments Oversight: F&PC Lead: Director of Finance Current Risk Score: 12 (stable) Target Score: 4 Target Date: 31 Mar 2028 Assurance Rating: Q4 24/25 SR6 – Digital Technologies Oversight: F&PC Lead: Director of Finance Current Risk Score: 12 (increased from 8) Target Score: 4 Target Date: 31 Dec 2025 Assurance Rating: Q4 24/25 SR7 – Planning and Delivery of Services for Population Health Needs Oversight: F&PC Lead: Chief Operating Officer Current Risk Score: 12 (stable) Target Score: 6 Target Date: 31 Dec 2027 Assurance Rating: Q2 23/24
Strategic Risk 1
- BAF Risk SR1 – Risk 636: If there is a breakdown of quality including safety assurance processes, we risk not being able to maintain standards of safe practice, meeting population health needs and compliance with regulatory requirements.
- Strategic Objective: 1. Through our care services: We deliver great care that is high quality and improves lives
- Accountable Director: Executive Director of Nursing and Professions
- Oversight Committee: Quality Committee
- Risk Appetite: High / Open
- Initial Risk Score: 4 (L2xC2)
- Current Risk Score: 12 (L3x4C)
- Target Risk Score: 4 (L2xC2)
- Target Date: 31 December 2025
Controls in place
- Clinical governance structures in place at all tiers of the organisation to embed clinical governance.
- Process in place to review and learn from death supported by Learning from death policy and Learning from Incidents and Mortality
- Peer review process in place with oversight from CQC steering group
- Annual process in place for reporting on the controls in place in relation to risk to compliance incorporating the Annual Governance Statement Compliance
- Process for managing patient safety events supported by PSIRF policy and plan
- Structures and processes in place for staff to raise concerns and escalate issues supported by Whistle Blowing Procedure and Freedom to Speak Up Guardian
- Processes in place to seek and receive patient and carer feedback
- Risk management processes and policies in place to support the identification, management and reporting of incidents and risks
- Safer staffing group and establishment process
- Trust wide working group to implement the Risk Assessment and Management Plan (RAMP)
- Suicide prevention environment survey
- Culture of care programme
- Implementation of Sexual safety standards
- Systems (with supporting policies) in place relating to Safeguarding, physical health, Infection Prevention Control.
- Clinical Supervision training offer in place to support clinical practice.
Details of Assurance
- Assurance Rating: Partial
| Management / Service Level | Review Process / Oversight | Independent (external / internal audit) |
| – Escalation processes – Teir three clinical governance meetings supported by TOR and clinical governance framework. – Escalation mechanism in place from ward to board – Weekly LIMM meeting to review incidents (graded 3 and above) and deaths – Monthly Trust Incident Review Group with a focus on SI reports and overdue actions – Bi-monthly CQC oversight group with overview of peer reviews – Monthly safer staffing group with oversight of staffing levels and annual establishment review – Monthly positive safety group with overview of incidents of restraint – Monthly CLIP report shared with services giving an overview of incidents, complaints, PALS – E-rostering system in place – Monthly working group with overview of the implementation of the RAMP – Monthly suicide prevention environment group – Monthly sexual safety group meeting – Monthly falls and pressure ulcer group to review falls and pressure ulcer incidents (graded 3 and above) – Monthly safeguarding report shared with services giving overview of safeguarding training compliance and safeguarding referrals. |
– Clinical Governance Framework – Quarterly combined report reviewed by Quality Committee – 6-monthly Learning from Deaths report to Quality Committee – SI/PSII reports reviewed and signed off at Trust Incident Review Group – Quarterly safer staffing report to Quality Committee – Quarterly reducing restrictive practice report to Quality Committee – Quarterly sexual safety report to Quality Committee – Evaluation of the implementation of the RAMP to be reported through Quality Committee – Suicide prevention environment group summary supported to clinical environment group and escalated to ESG. – Nursing and Professions highlight report to quality committee – Falls and pressure ulcer group report to quality committee – Peer review reports shared via clinical governance structures – Monthly Executive risk management to review and discuss 15+ risk – Annual quality accounts – Annual Clinical Supervision Training report to Nursing and Professions’ Council. |
– Assurance report: complaints / PALS – Peer reviews: ICS level – Provider collaborative and ICB quality visit – Audit Yorkshire – internal audit programme & reports (list) – Healthwatch external visit – 2019 CQC inspection report, overall rating good – CQC MHA reviews – Significant assurance – sexual safety audit |
Gaps in assurance / controls:
- Development of suicide prevention plan and self-harm strategy
- Development of Clinical Governance dashboard
- Development of safer staffing SOP
- End of life care
Mitigating actions underway for controls and assurance:
| Action | Lead | Target Date | Progress |
| Establishment of end of life care steering group to develop clinical practice standards | Deputy Director for AHP’s, Social Workers | 31 March 2026 | Stakeholder and implementation group dates set which will have oversight of the risk until ReSPECT is implemented. |
| Development of a suicide prevention plan and Self-Harm Strategy | Head of Nursing | 31 December 2025 | Previous plans and current guidance being reviewed and PID being developed with support from Project Manager to guide strategy development and action plans. Engagement with citywide work ongoing to inform local plan. Working with neighbouring trusts to develop training. |
| Culture of Care Standards Transformation Programmes | Professional Lead for Nursing | 31 March 2026 | Launch event attended in May 2024. QI and coaching for pilot sites commenced in September 2024. Pilot sites currently implementing change ideas and collecting assurance data. Pilot sites due to come to an end in March 2026 and then a plan to roll out following this date. |
| Development of clinical governance dashboard in conjunction with the quality improvement team to support Tier 3 Clinical governance meetings. | Head of Clinical Governance | 30 January 2026 | Work in conjunction with quality improvement team to develop range of indicators that will inform services on the quality of care being delivered within services. To link with wider work on quality dashboard and annual service reports. Quality improvement at local governance meetings led by the Heads of Governance and Head of Digital for Nursing and Professions. This will be supported by a training package. |
| Development of a safer staffing SOP | Deputy Director of Nursing | 31 October 2025 | A SOP will be developed to support a standardised and consistent approach across inpatient services for the annual safer staffing establishment reviews with the staffing escalation procedure forming part of the document. |
Contributory risks at level 12 or above
| Risk ID | Description | Lead | Oversight Group | Risk Score |
| 973 | There are no agreed, trust wide, clinical practice standards in place that ensure consistency in regards to the access and storage of DNA CPR and ReSPECT documentation within inpatient areas. | Deputy Director for AHP’s, Social Workers | ReSPECT stakeholder group/4 in 1 meeting | 15 (L3xC5) |
Strategic Risk 2
- BAF Risk SR2 – Risk 829: There is a risk that we fail to make the improvements outlined in the Quality Strategic Plan and that this has an impact on how we understand and act on the care of those who use our services.
- Strategic Objective: 1. Through our care services: We deliver great care that is high quality and improves lives
- Accountable Director: Medical Director
- Oversight Committee: Quality Committee
- Risk Appetite: High / Open
- Initial Risk Score: 9 (L3xC3)
- Current Risk Score: 12 (L4xC3)
- Target Risk Score: 6 (L2xC3)
- Target Date: 31 March 2028
Controls in place
- Quality Strategic Plan
- Safe Effective Reliable Care Framework
- LYPFT LCL Framework
- Improvement Methodology
- STEEEP Framework
- Trustwide Clinical Governance structure
- Learning from Deaths process
Details of Assurance
- Assurance Rating: Partial
| Management / Service Level | Review Process / Oversight | Independent (external / internal audit) |
|
|
|
Gaps in assurance / controls:
- Multi-disciplinary support and service leadership group
- Development of culture of innovation and improvement
- Data access and availability
Mitigating actions underway for controls and assurance:
| Action | Lead | Target Date | Progress |
| Development of collective leadership | Director for Collaborative Working | 31 March 2026 | Collective leadership programme continues for 2025/26 |
| Building improvement capacity and capability programme | Deputy Director of Improvement | 31 March 2026 | This work has been hindered due to the vacancy freeze and CIPs within the organisation. Work has been undertaken to explore if improvement apprenticeships can be used to build both improvement capacity and capability. The first staff member to begin the improvement apprenticeship scheme starts soon and this will be used to evaluate the potential impact of this approach. |
| Creation of an integrated quality and culture dashboard | Deputy Director of Improvement | 31 December 2026 | The Quality Dashboard Development Plan 2025/26 – Focus on Working Age Adult Acute Care Services Pilot is underway with ACS pilot phase one implemented, initial feedback suggests teams require additional support to integrate data into day-to-day work. Discussions at executive and team/service level continue with progress made re pilot and understanding of alignment between organisation wide and team level metrics, with progress monitored via an agreed timeline. |
| The prioritisation of the setup, configuration and digital enablement of the Patient Portal solution to support eProms but also to include other functionalities | Chief Information Officer | 30 September 2025 | NetCall’s patient hub was procured to meet Trust objective 13 procure a system (patient portal) that will enable clinical outcomes to be embedded into clinical services. The initial deployment will focus on the collection of outcome measures by service users via the portal, with later phases deploying appointment reminders and clinical correspondence through the portal and NHS App integration. |
| Identifying all proms used across the organisation; establishing where proms are not used; supporting teams with effective use of proms; imbedding proms in clinical practice; interfacing with Patient Portal and EPR teams to ensure digital delivery and access to analysed results | Clinical Director | 31 March 2027 | Project plan and supporting documents completed and presented to Execs and CDs. Proms for Pilot 1 identified and forwarded for digitisation. Partnership with digital team to establish current measures used. Discussions with Execs and Chief Digital Information Officer regarding establishment of a Transformation Board ongoing. |
Contributory risks at level 12 or above
None
Strategic Risk 3
- BAF Risk SR3 – Risk 1109: There is a risk that we fail to deliver a culture and environment that recruits, retains, and attends to the wellbeing of staff to enable them to be their best and deliver quality services now and in the future.
- Strategic Objective: 2. For our people: We provide a rewarding and supporting place to work.
- Accountable Director: Director of People and Organisational Development
- Oversight Committee: Workforce Committee
- Risk Appetite: High / Open
- Initial Risk Score: 12 (L3xC4)
- Current Risk Score: 12 (L3xC4)
- Target Risk Score: 6 (L2xC3)
- Target Date: 30 April 2026
Controls in place
- Trust People Plan
- Trustwide Retention Plan
- Widening Participation Plan
- Apprenticeship Strategy
- Leadership and Management Programme
- Leadership Academy programmes
- Collective Leadership Programme
- International Recruitment programme
- Exit Interview process
- Performance Reporting Compliance
Details of Assurance
- Assurance Rating: Partial
| Management / Service Level | Review Process / Oversight | Independent (external / internal audit) |
|
|
|
Gaps in assurance / controls:
- Demographic challenges
- National staff supply issues
- Staff training
Mitigating actions underway for controls and assurance:
| Action | Lead | Target Date | Progress |
| Further upskilling for managers on workforce planning and how to develop new roles / skill mixing to support services and fill vacancies. | Acting Head of Resourcing | 31 December 2025 | Career development programme in place alongside the apprenticeship strategy to help upskill individuals. VMP panel in place to provide scrutiny to check and challenge vacancies. Workforce plan identifies new roles and opportunities for skill mixing. Begin to align the training provision with the national Leadership and Managerial Framework. |
| Pilot the Train the trainer programme for Cultural Inclusion training which will be targeted at teams/services to address issues around culture/equality/diversity and inclusion. | Head of Diversity & Inclusion | 1 October 2025 | Evaluation of programme underway. Findings will be used to share the programme going forward and how best to target teams and services. |
Contributory risks at level 12 or above
None
Strategic Risk 4
- BAF Risk SR4 – Risk 619: There is a risk that a lack of financial sustainability results in the destabilisation of the organisation and an inability to meet our objectives.
- Strategic Objective: 3. We deliver effective and sustainable services
- Accountable Director: Chief Financial Officer
- Oversight Committee: Finance and Performance Committee
- Risk Appetite: High / Open
- Initial Risk Score: 8 (L2xC4)
- Current Risk Score: 15 (L3xC5)
- Target Risk Score: 4 (L2xC2)
- Target Date: 31 March 2026
Controls in place
- Efficiency and Productivity Programme including Cost Improvement Programme
- Revenue and Capital Plan
- Standing Financial Instructions
- Organisational plans
- Tender and procurement policy / programme
- Out of Area Placement programme
- System partners working arrangements
- Financial modelling and forward forecasting
- External Audit
Details of Assurance
- Assurance Rating: Partial
| Management / Service Level | Review Process / Oversight | Independent (external / internal audit) |
| – Chief Financial Officer governance framework / structure – Efficiency Groups – Workforce and Agency Project Board / Inpatient Flow Group / Procurement Steering Group – Finance training – Finance skills development – Fraud awareness courses – Budget holder training |
– Board of Directors minutes – Finance and Performance Committee minutes – Provider Collaborative reports – Finance and Provider Collaborative meetings – Financial Planning Group – Tender review process – Executive Risk Management Group |
– Provider Collaborative Framework – signed risk and gain shares – Leeds Strategic Finance Executive Group – Audit Yorkshire incl. Head of Internal Audit Opinion – Annual Accounts – Capital Planning Forum – Audit Yorkshire – internal audit programme and reports – NHS England – performance metrics – PWC West Yorkshire Financial Improvement Support Audit |
Gaps in assurance / controls:
- No agreed plan for the recurrent budget £14.5m CIP
- SSL contact deficit
Mitigating actions underway for controls and assurance:
| Action | Lead | Target Date | Progress |
| Confirmed schemes detailing how the Trust will achieve the £14.5m recurrent budget CIP | Deputy Director of Finance | 30 September 2025 | Targets have currently been given to services and departments, schemes are being worked up |
| Re-negotiate the contract with LCC | Deputy Director of Finance | 31 March 2026 | The Trust is currently in the process of negotiating an inflationary uplift with LCC. |
Contributory risks at level 12 or above
| Ref | Description | Lead / Responsible Director | Oversight Group | Score |
| 650 | Protecting MHIS investment for MH services in this challenging Financial Environment | Deputy Director of Finance / Chief Financial Officer | Finance & Performance Committee | 12 (L4xC3) |
| 651 | Failure to achieve ongoing recurrent budget CIP requirements and demonstrate efficient and effective care will lead to a deterioration in the financial position. | Deputy Director of Finance / Chief Financial Officer | Finance & Performance Committee | 16 (L4xC4) |
| 731 | A continuation of agency spend at current levels could negatively impact the Trust in achieving its financial plan and hinder the system to meet its overall system agency cap | Deputy Director of Finance / Chief Financial Officer | Financial Planning Group | 12 (L3xC4) |
| 949 | Changes to the capital funding regime may impact on the ability to secure sufficient capital (CDEL) allocations to deliver our long-term capital planning objectives, including reprovision of PFI. Capital resources are allocated to each ICS to help address ICS priorities, there is a risk that LYPFT capital requests may not be prioritised in the context of the other ICS priorities. The operational methodology used for allocating capital resources between organisations may not benefit LYPFT and be lower than historic planned levels. The Health & Social Care bill introduced a requirement to manage within capital allocations, however there is a risk that other system partners do not. | Deputy Director of Finance / Chief Financial Officer | Financial Planning Group | 12 (L3xC4) |
| 1147 | Failure to re-negotiation of the SSL contract to ensure that is financially viable | Deputy Director of Finance / Chief Financial Officer | Finance & Performance Committee | 16 (L4xC4) |
| 1148 | Out of Area Placement expenditure increasing threatening the financial sustainability of the Trust | Deputy Director of Finance / Chief Financial Officer | Finance & Performance Committee | 16 (L4xC4) |
| 1149 | Impact of the growing gap between tariff uplift and Trust inflationary pressures | Deputy Director of Finance / Chief Financial Officer | Finance & Performance Committee | 15 (L5xC3) |
| 869 | Reliance on non-patient income e.g. Commercial & Interest Receivable | Deputy Director of Finance / Chief Financial Officer | Finance & Performance Committee | 16 (L4xC4) |
| 649 | The impact of financial risk share agreements linked to Provider Collaboratives | Deputy Director of Finance / Chief Financial Officer | Finance & Performance Committee | 12 (L3xC4) |
| 1323 | Failure to achieve the Trust expenditure run-rate reduction required to meet the Financial plan for the year | Deputy Director of Finance / Chief Financial Officer | Finance & Performance Committee | 16 (L4xC4) |
| 1324 | The risk that the Facilities management costs of the PFI properties will cost substantially more than the current budget post demise. | Deputy Director of Finance / Chief Financial Officer | Finance & Performance Committee | 12 (L4xC3) |
| 1325 | Risk that the EPR system cost substantially more than the current EPT system when it is renewed | Deputy Director of Finance / Chief Financial Officer | Finance & Performance Committee | 12 (L3xC4) |
| 1326 | Financial cost and impact of exiting the PFI | Deputy Director of Finance / Chief Financial Officer | Finance & Performance Committee | 12 (L3xC4) |
Strategic Risk 5
- BAF Risk SR5 – Risk 619: Due to an inability to provide adequate working and care environments we risk being unable to deliver safe and effective services.
- Strategic Objective: 3. We deliver effective and sustainable services
- Accountable Director: Chief Financial Officer
- Oversight Committee: Finance and Performance Committee
- Risk Appetite: High / Open
- Initial Risk Score: 8 (L2xC4)
- Current Risk Score: 12 (L3xC4)
- Target Risk Score: 4 (L2xC2)
- Target Date: 31 March 2028
Controls in place
- Security Management Policy
- Health and Safety Policy
- Technical Policies (Water, Asbestos, Fire Safety)
- Sustainability Plan (LYPFT Green Plan)
- Strategic Estates Plan
- Capital Project Planning and delivery
- PFI Governance Framework and overarching programme management to support work plans
- 2025 Commissioned 6 Facet Survey
- Compliance, Risk, Assurance, Governance group established locally
- Statutory Returns to NHSE (Premises Assurance Model, Patient Led Assessment of Care Environment, Estates Return Information Collection)
Details of Assurance
- Assurance Rating: Partial
| Management / Service Level | Review Process / Oversight | Independent (external / internal audit) |
| – Chief Financial Officer governance framework / structure – Operational site meetings – Escalation processes – Risk assessments – Compliance, Risk, Assurance and Governance Groups for Estates & Facilities |
– Finance & Performance Committee minutes – Estates Steering Group minutes – Clinical Environment Group minutes – Environment audit programme – PFI demise governance process – Chief Financial Officer reports – PFI BAU and operational contract management – Executive Risk Management Group |
– Audit Yorkshire – internal audit programme & reports – Independent Authorising Engineer / Independent Advisor Audits as per the requirements of Premises Assurance Model (PAM) – Patient Led Assessment of the Care Environment (PLACE) – Estates Return Information Collection (ERIC) |
Gaps in assurance / controls:
- Limited capital finance availability to address backlog maintenance (below condition B)
- Limited capital finance availability to fully support the care services aspirations
- Staffing pressures in relation to capacity, recruitment and retention, staffing competence etc short against required standards (HTM, HBN, National Standards Cleaning / Catering)
- Management and current ownership provision of our estate as a large proportion is managed and invested in by others i.e PFI and NHSPS.
Mitigating actions underway for controls and assurance:
| Action | Lead | Target Date | Progress |
| Extreme heating feasibility studies to be undertaken and costed and taken to CEG for discussion. | Deputy Director of Estates and Facilities | 30 September 2025 | Feasibility complete for Becklin Centre, ongoing at The Mount with reports due back at the start of August and presented to CEG then ESG by September. Reports for Becklin and The Mount complete – report to CEG / ESG required but previously agreed to defer due to other priorities. Note new Target Date ahead of Summer 25. New Sustainability Lead now appointed so we can proceed as priority. |
| Implementation of on-site staff safety alarm system using Capital Allocation via ESG, to address the issues in relation to the alarms. Supplemented with door lock adaptations and local SOPs. | Deputy Director of Estates and Facilities | 30 August 2025 | To be complete in June 2025 – project nearly complete. This will reduce the risk (116) of 12. Deferred to August from June due to final commissioning being linked to clinical SOP. |
| Health and Safety Audits to be completed on all the Trusts owned, leased and PFI Estate, on a periodic basis. | Head of Health and Safety | 31 March 2026 | This is a rolling programme to satisfy HSE requirements and to assure ourselves of our environment safety. 2024/25 schedules complete. 2025/26 underway. |
| Security Risk Assessments to be conducted on all the Trusts owned, leased and PFI Estate and to be completed on a periodic basis. | Trust Security Manager | 31 December 2026 | All buildings will be risk assessed across both physical and infrastructure security by the Trusts Security Team in accordance with the agreed schedule. This is a rolling programme; 2024 Risk Assessments are complete. 2026 next assessments are scheduled. |
| Updated 6 Facet Survey / Condition Survey to ascertain the condition and backlog requirement of the Trusts owned Estate. | Deputy Director of Estates and Facilities | 30 September 2025 | Previous review of existing 6F (completed in Feb 2022) now complete. This has prompted us to re-survey. Surveyors are currently on site assessing our estate (schedule to complete in June 2025) and outputs will link into capital planning and risk management. Capital backlog figures have been supplied (£2.8m) – reports have only been received in July so scrutiny required and added to capital planning. |
| PFI Joint Steering Group | Deputy Chief Executive / Chief Financial Officer Deputy Director of Estates and Facilities |
August 2028 | Quarterly meetings are maintained, and extraordinary meetings take place where required. Overseen by Exec level directors at respective organisations. Clear agenda with specific focus on business as usual, strategic projects and PFI Demise. This group now has oversight of PFI demise. |
| PFI LYPFT Concession Group | Deputy Chief Executive / Chief Financial Officer Deputy Director of Estates and Facilities |
August 2028 | Regular meetings are in place meeting every 2–3 months with a master overarching programme. Formal updates and reports provided for assurance or to seek appropriate support. The workplans are supported by legal reviews and under guidance from the NISTA (formerly known as IPA). |
| PFI Joint Demise Group | Deputy Chief Executive / Chief Financial Officer Deputy Director of Estates and Facilities |
August 2028 | Established in May 2024 under formal remit set out in Terms of References – a joint working group operationally managing crucial elements of the PFI Demise and reporting into the PFI Joint Steering Group. Key features include: Leases Expiry, Condition Survey, Documentation / Operating Manuals. Formal reporting and monitoring is provided to the Joint Steering Group as well as a Joint Demise Action Plan. |
| PFI LYPFT Monthly Contract / Performance Monitoring Meetings | Deputy Director of Estates and Facilities | August 2028 | Monthly meetings continue to progress with all parties including Mitie FM. Reports are provided to the PFI JSG and will be reviewed for effectiveness ahead of the PFI Demise and to ensure ‘Business as Usual’ assurance is provided in alignment to the Demise Plans. |
| Appraise the relevant sub-board committees on an annual basis for the outcomes of the PLACE and PAM outcomes | Deputy Director of Estates and Facilities | 31 October 2025 | F&P Committee have been appraised in 2025 on our statutory reporting across 2024 and have provided feedback for future reporting in 2025. |
| Green Steering Group | Deputy Director of Estates and Facilities | 31 December 2025 | Updated 2025 Green Plan has prompted the review of the previously known Sustainability Steering Group. The Group / ToRs, Membership and Action plan has been refreshed as the approach will now be organisationally wide as opposed to being delivered from just Estates and Facilities – there are 9 workstreams in alignment with Greener NHS. Heat decarbonisation plans have been produced to help inform route to net zero. |
Contributory risks at level 12 or above
| Ref | Description | Lead / Responsible Director | Oversight Group | Score |
| 1008 | The Trust is unable to meet the NHS Carbon Neutral requirements by 2040 and to implement a sustainable culture within the organisation | Deputy Director of Estates and Facilities / Chief Financial Officer | Estates Steering Group | 12 (L3xC4) |
| 1168 | No onsite alarm system at CMHT bases to ensure safety for staff and service users during clinical visits. Bases affected:- Aire Court, St Mary’s Hospital (Holly House), St Mary’s House – South Wing and North wing and Millfield House | Deputy Director of Estates and Facilities / Chief Financial Officer | Estates Steering Group / Clinical Environment Group | 12 (L4xC3) |
Strategic Risk 6
- BAF Risk SR6 – Risk 635: As a result of insecure, inadequate and poorly utilised digital technologies there is a risk the quality and continuity of services is compromised.
- Strategic Objective: 3. We deliver effective and sustainable services
- Accountable Director: Chief Financial Officer
- Oversight Committee: Finance and Performance Committee
- Risk Appetite: High / Open
- Initial Risk Score: 12 (L3xC4)
- Current Risk Score: 12 (L3xC4)
- Target Risk Score: 4 (L2xC2)
- Target Date: 31 December 2025
Controls in place
- Digital Strategy
- Cyber Security Policy
- IT Policy
- Data security and protection toolkit
- ICT infrastructure
Details of Assurance
- Assurance Rating: Partial
| Management / Service Level | Review Process / Oversight | Independent (external / internal audit) |
| – Chief Financial Officer governance framework / structure – Procurement processes incl. requisition approval – Junior Buyer / procurement team training – Category Codes (E Class) – Over £5k approval process – Digital Change Leads – ICT infrastructure – Phishing Exercise – Board level training |
– Board of Directors minutes – Finance & Performance Committee minutes – Digital Steering Group minutes – Procurement & ICT meeting minutes / action log – Information Governance Group – Cyber monitoring system – CareCerts process – Chief Financial Officer reports – Executive Risk Management Group |
– Audit Yorkshire – internal audit programme & reports – NHS Digital – National Cyber Operations Centre portal (returns process) – Penetration Testing – Phishing Exercise |
Gaps in assurance / controls:
- Culture, staff ability and aptitude
- Cyber attack awareness
Mitigating actions underway for controls and assurance:
| Action | Lead | Target Date | Progress |
| Work with staff through Digital Change Team to understand the barriers to using technology and provide the necessary help and support. | Chief Digital Information Officer | 26 December 2025 (ongoing process) | This is a continual process through our journey to continually deliver effective and efficient digital solutions and forms part of a continual improvement cycle.
Engagement through the digital change team continues to better understand barriers and to look at solutioning responses. Major review of CareDirector forms completed and workflows are currently being reviewed. Engagement planned to understand barriers across nonclinical areas. EPR Programme will also support this action as we evolve and mature through the programme startup Continued Engagement with Digital Leeds and ICB regarding support around digital literacy. |
| Continued Engagement with Digital Leeds and ICB regarding support around digital literacy. | Chief Digital Information Officer | 26 December 2025 (ongoing process) | Discussions taken place across the ICS and city footprint via CIO and digital leadership groups and meetings.
Local Authority have received funding for a digital exclusion lead to support identification and planning for new initiatives to support the addressing of this area. Engaged in discussions regarding support and sharing of knowledge and understanding however direct influence over shared ideas is small and programme being owned/delivered by the local Authority. Delay on further engagement due to changes across the system. to be raised and West Yorkshire CIO council. |
| Deliver cyber communications plan with target on delivering messages and examples of phishing relating to key annual milestones, religious festivals, significant holidays, return to school etc. | Head of Cyber and Networks | 26 December 2025 (ongoing process) | Schedule of themes determined. Comms completed and delivered against a number of themes, including broader awareness session to further support the most recent internal Phishing exercise.
Continual process and subject matters continue to evolve and flex with need. |
| Clinical and Care Service Engagement and involvement throughout EPR scoping, specification and procurement cycle to support views on functional requirements to support future uptake and adoption of a new EPR | Chief Digital Information Officer | 31 March 2025 (ongoing process) | High Level functional specification developed. Clinical directors engaged for initial review of high-level functional specification and a number of reviews with the wider clinician base completed.
Programme board set up and chaired by Medical Director. Outline Business Case developed and working through governance cycle. Approved by EPR programme board and planned for July Finance & Performance Committee and Trust Board. |
| Delivery of EPR functional requirements outside of CareDirector to support emerging need to support clinical pathways and mitigate potential areas of clinical risk and patient safety. | Chief Digital Information Officer | 31 December 2025 (ongoing process) | Review of complementary systems to support areas of development that CareDirector cannot deliver against.
Review of integration and interoperability to ensure ability to review and report on all data. OpenEHR environment created. ARCHETYPES under review to support application development for recording of observations |
| Usability reviews and NHS APP integration a fixed requirement for patient portal procurement and deployment | Chief Digital Information Officer | 31 December 2025 (ongoing process) | Patient portal review completed, business case approved, and solution procured.
Project board set up, technical installation complete and configuration underway. Technical configuration and testing underway. SMS and email functionality tested. Review of service requirements and scope of works for initial service pilot underway. NHS App integration dependant upon appointment management through portal, conversations ongoing with national team regarding questionnaire based app integration. |
Contributory risks at level 12 or above
| Ref | Description | Lead / Responsible Director | Oversight Group | Score |
| 105 | The danger of a cyber-attack to the Trust’s ICT infrastructure through malicious hacking or system virus infection. | Chief Digital Information Officer / Chief Financial Officer | Digital Steering Group | 12 (L3xC4) |
| 1223 | Advanced will not continue to make the same levels of investment in the growth of CareDirector v6. Going forward Advanced have committed to continue to maintain and support CareDirector v6 for the duration of customers current contract term, but the roadmap will be adjusted to only focus on essential maintenance activities and key legislative/security work. | Chief Digital Information Officer / Chief Financial Officer | Digital Steering Group | 16 (L4xC4) |
Strategic Risk 7
- BAF Risk SR7 – Risk 1111: There is a risk we fail to understand, plan and deliver services that meet the health needs of the population we serve.
- Strategic Objective: 1. Through our care services: We deliver great care that is high quality and improves lives.
- Accountable Director: Chief Operating Officer
- Oversight Committee: Finance and Performance Committee
- Risk Appetite: High / Open
- Initial Risk Score: 12 (L3xC4)
- Current Risk Score: 12 (L3xC4)
- Target Risk Score: 6 (L2xC3)
- Target Date: 31 December 2027
Controls in place
- Care service governance structure and framework in place to monitor and plan service delivery and development and report ward-to-board and board-to-ward
- Care Services Strategic Plan
- Annual operational planning and prioritisation process
- Trust’s People Plan
- Quality Strategic Plan
- Working in partnership with the ICB in relation to marginalised communities
- Partnership with other NHS organisations and community groups across our service delivery areas
- Work to look at inequalities in relation Restrictive Practices and their reduction
- Community Mental Health Transformation Programme
- Utilisation of population health information in the planning and design of services
- EHIA tool
- Out of Area Placement programme to ensure people are appropriately placed according to their need
- Business Continuity Plans
- Improving Health Equity Strategic Plan 2025-2029 and implementation plan
- PCREF Action Plan 2024-2027
- ‘Must do’ work on EDS, PCREF and Equality Act duties
- Care Services Performance Meeting and agreed reporting metrics
- Waiting List Management Process in place
- Business Continuity Management System in place
- Improving Health Equity Steering Group
Details of Assurance
- Assurance Rating: Partial
| Management / Service Level | Review Process / Oversight | Independent (external / internal audit) |
| – Chief Operating Officer governance structure and reporting framework – Care Services Strategic Plan implementation programme – Annual planning, monitoring and delivery framework – Business planning process – Update on delivery of the Trust’s People Plan – Update on delivery of the Quality Strategic Plan – Waiting times monitoring process – Protected characteristics monitoring – Workforce monitoring reports – Reduction in restrictive practice workstream – Monitoring of the ethnic mix of detained patients and those who access our service – Capacity and flow programme – EPRR monitoring compliance with Business Continuity management system |
– Assurance reports, discussion and actions relating to governance groups including: o Board of Directors o Finance and Performance Committee o Mental Health Legislation Committee o Workforce Committee o Quality Committee o Executive Risk Management Group o Care Services Development and Delivery Group o Care Services Performance Group o ICB MH Population Board – Chief Operating Officer reports – Annual Service Quality Reports – CSDDG Annual Report – WREN / DAWN Group |
– Audit Yorkshire – internal audit programme and reports – Contract meetings and monitoring – Provider Collaborative Framework – Community Mental Health Transformation Partnership Board |
Gaps in assurance / controls:
- Health Inequalities Strategy Implementation Plan
- Compliance with Business Continuity Management System
- Equality Impact Assessment Process
Mitigating actions underway for controls and assurance:
| Action | Lead | Target Date | Progress |
| Development of an Equality & Health Inequality Impact Assessment Process | Head of Health Equity | 31 October 2025 | New EHIA Policy, guidance and templates in development which will enable the Trust to proactively and positively consider how we can help improve health equity and actively work to tackle known inequalities. This is further enabling us to support and evidence the responsibility of LYPFT to reduce inequalities in access, experience and outcomes. |
| Compliance with the Business Continuity Management system | EPRR Lead | 31 May 2027 | Work is ongoing to ensure all relevant services have a business continuity plan and that these are regularly reviewed within relevant governance groups and evidence of this is provided to the EPRR Team. It is anticipated that all Care Services Teams will have a business continuity plan by the end of October 2025. All Corporate Services Teams will have a plan by May 2026 (Corporate Business Plans support the delivery of Care Services). |
| Care Services Strategic Plan appendices to be updated by service lines | Deputy Director for Service Development | 30 October 2025 | The update of the appendices will take place once the 10 Year Plan has been published and there has been consideration of the requirements of this Plan and its impact on our services. |
Contributory risks at level 12 or above
| Ref | Description | Lead / Responsible Director | Oversight Group | Score |
| 92 | The current level of demand for the gender service is greater than planned level of activity, resulting in a lengthy waiting list for assessment and treatment. In addition, due to the child and adolescent service closure, there are further increasing numbers of transfers from the child and adolescent services which is impacting upon waiting times to access the service for all. This presents a potential risk to service user mental and physical health, due to the inability to access care in a timely way. | Operational Manager for the Gender Service | Care Services Delivery and Development Group | 12 (L4xC3) |
| 1101 | West Yorkshire GPs are declining Connect blood requests for physical health monitoring under instruction from the West Yorks LMC that states eating disorder blood monitoring is not mandatory for GPs. Connect are not commissioned to provide phlebotomy services and do not have access to the necessary systems for requesting and monitoring bloods. This presents a potential risk to service user physical health, due to the inability to access care in a timely way. | CTM | Care Service Delivery and Development Group | 12 (L3xC4) |
| 1212 | Delayed service user transfer from LTHT to LYPFT inpatients. This has resulted in service users requiring mental health admission remaining in medical beds in LTHT for significant periods of time. There is a potential risk to service users due to not receiving timely and skilled mental health interventions. Additionally, there is a risk to other patients in LTHT and to staff. | CTM | Capacity and Flow Group | 12 (L3xC4) |
| 1213 | Increased risk of Leeds Service Users being inappropriate sent out of area for care and treatment because of reduced flow across our inpatient services. | Head of Operations | Capacity and Flow Group | 16 (L4xC4) |
| 1220 | Following the CMHT service moving to BAU from BCP status there are legacy issues which present a risk to the overall quality and performance delivery across CMHTs. There is a risk is that the CMHTs are under staffed across professional registered roles and unable to recruit to vacancies. | Head of Operations | Care Service Delivery and Development Group | 12 (L4xC3) |
| 1260 | The risk of new and emerging pandemics, as shown by COVID19, could have a devastating impact on society and a direct impact on how the Trust continues to provide services. | EPRR Lead | EPRRG | 12 (L3xC4) |
| 1263 | A supplier of a service that has been identified as critical to one of the Trust main service provision obligations or a key supporting service goes into administration or entirely closes, creating a service provision risk. | EPRR Lead | EPRRG | 12 (L3xC4) |
| 1270 | ADHD waiting list of 4,700 plus patients for diagnostic assessment, 100 minimum patients added to list each month, waiting time for new non-urgent assessments of 10 years minimum, likely far longer. This presents a potential risk to service user mental health, due to the inability to access care in a timely way. | Operational Manager | Care Service Delivery and Development Group | 12 (L4xC3) |
| 1271 | Patient waiting times for ADHD medication initiation presents a risk to patients due to a delay in medication commencing. | Operational Manager | Care Service Delivery and Development Group | 12 (L4xC3) |
| 1277 | Journey and DBT group work programmes with excessive wait times for first contact, assessments completed and treatment commencing. Current wait for groups minimum 6 months which presents a risk that service users cannot access the services they need. | Operational Manager | Care Service Delivery and Development Group | 12 (L4xC3) |
| 1289 | Physical health team are experiencing caseload and capacity issues and are unable to provide the level of service to meet service user need. | CTM | Care Service Delivery and Development Group | 12 (L4xC3) |
| 1306 | Lack of specialist addictions midwifery capacity due to vacancies with the risk service users cannot access the level of service required. | CTM | Care Service Delivery and Development Group | 12 (L4xC3) |
| 1310 | Backlog of referrals to be reviewed and processed in ME/CFS Service. Potential risk to patient care and treatment due to length of time taken to process referral and add to waiting lists. | Operational Manager | Care Service Delivery and Development Group | 12 (L4xC3) |
3 – Conclusion
The BAF demonstrates the key strategic risks for the organisation, and the controls and assurance have been updated to reflect the levels of assurance, with actions detailed on further work to be taken.
The document will be updated as per established governance and oversight processes, with links to the identified oversight committees.
4 – Recommendation
The Board is asked to:
- Receive the BAF and to be assured of the review that has been undertaken to ensure that this accurately reflects the position as of July 2025, including risk scoring and mitigating actions.
Clare Edwards
Associate Director for Corporate Governance and Board Secretary
21 July 2025
Cover sheet for Risk Appetite Statement
- Paper title: Risk Appetite Statement
- Date of meeting: 31 July 2025
- Presented by: Dr Sara Munro, Chief Executive
- Prepared by: Clare Edwards, Associate Director of Corporate Governance
This paper supports the Trust’s strategic objective/s (SO):
- SO1 – We deliver great care that is high quality and improves lives.
- SO2 – We provide a rewarding and supportive place to work.
- SO3 – We use our resources to deliver effective and sustainable services.
This paper relates to the Trust’s strategic risks (SR):
- SR1 – Quality including safety assurance processes
- SR2 – Delivery of the Quality Strategic Plan
- SR3 – Culture and environment for the wellbeing of staff
- SR4 – Financial sustainability
- SR5 – Adequate working and care environments
- SR6 – Digital technologies
- SR7 – Plan and deliver services that meet the health needs of the population we serve.
Executive summary
Risk appetite assists in understanding the degree of risk to which the Trust has deemed acceptable to tolerate. It is good practice to review the risk appetite on a regular basis, and to consider any internal or external changes that may affect the overall appetite.
Following an internal audit, there was a recommendation for the Trust to develop a risk appetite statement to support the Board Assurance Framework and the approach to risk.
The details of the Trust’s proposed risk appetite statement are set out in this document. The risk appetite categories are aligned to the Trust’s strategic risks on the Board Assurance Framework. Following approval of the risk appetite statement and position, this will be included in the Board Assurance Framework moving forward.
Do the recommendations in this paper have any impact upon the requirements of the protected groups identified by the Equality Act? No
Recommendation
The Board are asked to:
- review the contents of the risk statement
- approve each of the risk appetites
Risk Appetite Statement
1 – Executive summary
Risk appetite assists in understanding the degree of risk to which the Trust has deemed acceptable to tolerate. It is good practice to review the risk appetite on a regular basis, and to consider any internal or external changes that may affect the overall appetite.
Following an internal audit, there was a recommendation for the Trust to develop a risk appetite statement to support the Board Assurance Framework and the approach to risk. This paper sets out the proposed Trust position.
2 – Introduction
Risk appetite is defined as the amount of risk, on a broad level, that an organisation is willing to accept in the pursuit of its strategic objectives. The Trust has developed and documented its risk appetite statement to assist in understanding the degree of risk to which the Trust has deemed acceptable to tolerate.
The Trust recognises that its long-term sustainability depends upon the delivery of its strategic objectives and its relationships with individuals, colleagues, the public and partners. Our risk appetite should enable our ambition and managed risk taking needs to be a greater feature in more aspects of what we do so long as it does not have a negative impact on individuals or colleague safety.
The risk appetite categories are aligned to the Trust’s strategic goals, and cross referenced to the strategic risks on the Board Assurance Framework. The statement of risk appetite is dynamic and its drafting is an iterative process that reflects the challenging environment facing the Trust and the wider NHS.
3 – Use of the Trust risk appetite
It should be acknowledged that the statement of risk appetite is a broad one, which enables better internal control and does not offer definitive answers to any specific risk management issue. When assessing and managing risks, the risk appetite statement should be reviewed and considered to assist in determining an acceptable risk target score and the mitigating action required to achieve this.
No statement of risk appetite can cover every potential risk or outcome and there may be exceptions, which mean that the Trust has valid reasons for setting a level of tolerance outside of the scope of the statement of risk appetite. In this case, the rationale will be formally documented, and consideration will be given to incorporating changes as necessary in any future revision of the risk appetite statement.
4 – Risk Appetite Target Scores
The risk appetite is defined by the ‘Good Governance Institute risk appetite for NHS organisations’ matrix, which the Trust has adopted. This has been aligned to the Trust’s own risk assessment matrix as shown in the table below.
| Good Governance Institute matrix | Risk appetite level | Risk target score (range) |
| Avoid: Avoidance of risk and uncertainty is a key organisational objective | Zero | Nil |
| Minimal: (As little as reasonably possible) Preference for ultra-safe delivery options with low inherent risk and only for limited reward potential | Low | 1-3 |
| Cautious: Preference for safe delivery options that have a low degree of inherent risk and may only have a limited potential for reward. | Moderate | 4-6 |
| Open: Willing to consider all potential delivery options and choose, whilst also providing an acceptable level of reward (and VFM) | High | 8-12 |
| Seek: Eager to be innovative and to choose options offering potentially higher business rewards (despite greater inherent risk) | Extreme | 15-20 |
| Mature: Confident in setting high levels of risk appetite because controls, forward scanning and responsiveness systems are robust. | Extreme | 25 |
The proposed risk appetites for each strategic risk are shown in the table in appendix 1.
5 – Conclusion
The Trust acknowledges that it is operating in a time of national and system change with multiple stakeholders in decisions being made leading to potential risk. The organisation will manage clinical, financial, and business risks to deliver its objectives in a controlled manner.
6 – Recommendation
The Board of Directors are asked to:
- review the contents of the risk statement
- approve each of the risk appetites
Clare Edwards
Associate Director of Corporate Governance
16 July 2025
Appendix 1: Proposed Trust Risk Appetite
| Risk Appetite | Strategic Risk |
| Avoid | SR1: Quality including Safety Assurance Processes Delivering high quality services and care is core to the organisation’s aims, objectives and ambition, however the Trust will avoid risk which compromises the delivery of high quality and safe services, and jeopardises compliance with our statutory duties for quality and safety or meeting our regulatory compliance requirements. |
| Cautious | SR2: Delivery of the Quality Strategic Plan The Trust has a cautious risk appetite for the delivery of the Strategic plan and will consider new opportunities to deliver solutions to support the achievement of the key areas within the Plan. This includes a Patient Portal and Quality and Culture Dashboard, utilising technology to support the delivery of this, whilst considering any associated risks. |
| Cautious | SR3: Culture and environment for the wellbeing of staff The Trust has a cautious risk appetite to providing a rewarding and supportive place to train and work and recruiting and retaining the best staff. The Trust acknowledges the need to support staff through change management and innovative changes to our care delivery models therefore is open to risks associated with the implementation of new models of working, however will avoid risk compromising patient or staff safety. |
| Minimal | SR4: Financial sustainability Our appetite for financial risk is minimal. We continually aim to deliver our services within the budgets set out in our financial plans and will only consider accepting risks that may result in limited financial impacts or losses on the basis that there may be opportunities elsewhere within the Trust. We will ensure that all such financial responses deliver optimal value for money. |
| Open | SR5: Adequate working and care environments The Trust is open to delivering our vision to make the best use of our most modern and fit for purpose estate, in line with our Estates Strategy. This includes offering the most appropriate therapeutic environment for our service users, and ensuring efficiency and effectiveness of use for our workforce to deliver care. |
| Open | SR6: Digital technologies The Trust is open to ensuring secure and adequate digital technologies being utilised across the organisation. It recognises the importance of making the best use of data to inform and increase our understanding of our population to provide insight into the best way to provide care. The long-term Digital Plan aims to use innovative technology and intelligence to enable safer, inclusive and more effective care. We will avoid risks that increase our exposure to cyber-fraud or incidents. |
| Seek | SR7: Plan and deliver services for health needs of the population The Trust has an open risk appetite for collaboration with people and communities to ensure their experience influences equitable approaches, acknowledging that people who need help for their mental health, people with learning disabilities and those with neurodiversity conditions endure inequalities which affect their health and lives. We are committed to co-designing, co-producing and co-delivering proactive and integrated care and support through our care services. |
Escalation and Assurance Report
Report from: West Yorkshire MHLDA Collaborative Committees-in-Common
Date of the meeting: 23rd July 2025
Key discussion points and matters to be escalated from the discussion at the meeting:
Alert/Action:
- There remain concerns regarding where some of the functions undertaken by the MHLDA
collaborative on behalf of the ICB will sit in within the new system architecture. This
includes strategic commissioning roles (ie ND commissioning policy development),
statutory functions (eg LD Dynamic Support Register), system convening (eg MHLDA
networks and steering groups) and a range of other functions relating to the
performance/assurance relationship with NHSE, representation at national/regional forums
etc - The committee received an update on the West Yorkshire position against the NHSE mandate to ensure full coverage of Mental Health Support Teams. NHSE trajectory indicates 5 more teams are required in West Yorkshire this year, with Bradford and Leeds prioritised for further roll out.
- The ICB are no longer receiving funding separately/through Service Development Funding, the expectation being that MHSTs will be funded by the ICB, creating a cost pressure from new and existing teams (as they move towards full mobilisation in 2025 and 2026).
- NHSE have requested confirmation of West Yorkshire position by 31st July 2025.
Advise:
- The WY Neurodiversity programme is presenting the Neurodiversity commissioning policy to WY ICB Transformation committee in July for the final decision on whether formal public consultation is required. If agreed, consultation expected to begin early autumn.
- Trust Executive collaborative meeting planned for 30th July to identify opportunities for a shared West Yorkshire work programme across across Trusts.
- The committee agreed the importance of continuing to hold the committee in the coming months and to ensure that MHLDA system expertise and focus continues as part of the new ICB system architecture.
- The Complex Rehabilitation programme presented an update of the prior 24/5 objectives that included Community Rehabilitation Enhanced Support Team. Transfers to local services completed for most people with 3 final transfers in progress to Calderdale local services.
- New ICB commissioning focused objectives agreed for the Complex Rehabilitation programme: Objective 1. Develop a W Yorks approach to realising financial efficiencies, Objective 2. Develop an agreed W Yorks approach to Quality Assurance & Surveillance.
- Trusts are working to complete the NHSE Serious Mental Illness review of assertive and community mental health services, due to NHSE in September. Trusts have worked hard to implement all of the ‘low cost, no coast’ actions associated with the review; however, concerns raised around the increased resource required to meet NHSE standards in full across all West Yorkshire Mental Health Trusts given the variation in models and some places taking a Core/Enhanced approach. This is not just a challenge in West Yorkshire, but nationally with similar challenges echoed across the country.
Assure:
- Provider Trusts and West Yorkshire MHLDA Team working closely with ICB Core Team to feed into the future operating model. Trusts Execs attending workshops throughout August.
- The ICB joint committee for Yorkshire and Humber has supported the decision to enact the optional plus one of the NHSE Lead provider contract. The NHSE lead provider contract, any and all sub contracts will run until March 2027.
- West Yorkshire specialised commissioning hub has developed a standard operating policy for the patient safety incident response framework to support a consistent approach. This has been shared and has now been adopted nationally.
- There is work underway as part of the Secondary Care Pathways Programme, in partnership with the West Yorkshire Mental Health Police Forum to develop a shared work plan to support the implementation of Right Care Right Person and ensure that appropriate governance structures are in place.
Report completed by: Charlotte Whale, Programme Manager, Mental Health Delivery, West Yorkshire MHLDA
Date: 24th July 2025
Distribution: Chairs and Company Secretaries of Bradford District Care NHS Foundation Trust, Leeds Community Healthcare NHS Trust, Leeds and York Partnership NHS Foundation Trust, South West Yorkshire Partnership NHS Foundation Trust.
Return to agenda